Beatrice Ezenwa, Patricia Akintan, Iretiola Fajolu, Jejelola Ladele, Chinyere Ezeaka.
Neonatology unit,Department of Pediatrics, Lagos University Teaching Hospital, Lagos, Nigeria.
ADDRESS FOR CORRESPONDENCE
Beatrice Ezenwa. Neonatology unit, Department of Pediatrics, Lagos University Teaching Hospital, Lagos, Nigeria.
Email: beatriceezenwa@yahoo.com | | Abstract | Respiratory distress syndrome (RDS) is a common health problem especially in preterm newborns. In Nigeria, prematurity accounts for about 25% of neonatal mortality and RDS have been identified as the major cause of these deaths. The major problem in RDS is immaturity of the lungs with deficiency of surfactant. Surfactant reduces surface tension in the alveoli, thereby preventing collapse of the lungs during expiration. Bubble continuous positive airway pressure (bCPAP) is a low cost intervention that delivers continuous distending pressure on alveoli thus preventing collapse during expiration.
Objective: To describe the experience in the use of bubble CPAP in the neonatal unit of Lagos University Teaching Hospital (LUTH) and to determine the outcome and efficacy of improvised bCPAP in the management of babies with respiratory distress syndrome.
Study design: Retrospective observational study
Subjects: Inborn preterm infants (gestation 25 to 34 weeks) admitted to the Neonatal Intensive Care unit (NICU) and managed for respiratory distress and with chest X- ray findings of RDS.
Intervention: Improvised bCPAP
Results: Forty-two subjects who were diagnosed with RDS were recruited into the study. Oxygen saturation was monitored in all babies and there were significant differences in mean oxygen saturations pre- and post-CPAP commencement from a mean of 82.93±4.07 to 94.±1.11 (p=0.02). Thirty-two babies were successfully weaned off CPAP with overall CPAP success rate of 76.2%. There were ten RDS specific mortality with case fatality rate of 23.8% during the study period. The mean birth weight of survivors were higher (1435.4g) compared to those who died (963.4g), p<0.05. Babies that died had lower mean gestational age (27.8 weeks) than those that did not (30.3 weeks) though this was not statistically significant (p >0.05).
Conclusion: Improvised bCPAP is a simple and cost effective intervention that can be used in resource limited settings to treat RDS in preterm babies and reduce morbidity and mortality due to surfactant deficiency. | | | | Introduction | Respiratory distress syndrome (RDS) is a common health problem in newborns, especially preterm very low birth weight (VLBW) and extremely low birth weight babies (ELBW).(1-3) In Nigeria, prematurity accounts for about 25% of neonatal mortalities (2) and RDS has been identified as the major cause of these deaths.(1)
The major problem in RDS, previously called Hyaline membrane disease, is a deficiency of surfactant. Surfactant is a complex substance of lipids, proteins and glycoproteins produced by the Type II pneumocytes. This production starts from 22 weeks gestation and is fully developed by 34 weeks gestation. Surfactant reduces surface tension in the alveoli, thereby preventing collapse of the lungs during expiration. Without adequate amounts of surfactant, the air-spaces collapse and are very difficult to expand leading to very high mortalities in affected babies.
Over the years, several interventions had been used to treat RDS and to reduce mortality resulting from it. In developed countries, respiratory support is provided with mechanical ventilation or continuous positive airway pressure (CPAP) with administration of surfactant. (3) Each intervention is however not without risks, merits and demerits. Mechanical ventilation is very costly and usually out of reach of most hospitals in developing countries. On the other hand, CPAP and especially bubble CPAP is a less expensive and affordable means of treating RDS in affected babies. Bubble CPAP (bCPAP) is a low cost intervention that delivers continuous distending pressure on alveoli keeping them from collapsing during expiration. (4) CPAP delivered by under-water seal causes vibrations of the chest due to gas flow under water (bubbles), and these vibrations simulate wave forms produced by high frequency ventilations. (4) There have been several documentations of proven efficacy of variously locally improvised bCPAP in resource poor countries. (3, 5) Improvised bCPAP has been documented by several researchers as a less expensive and efficacious method of respiratory support most suitable for babies with RDS in resource constrained neonatal units in developing countries. (3, 7)
This study aimed to describe efficacy of improvised bubble CPAP in the management of RDS | | | | Methodology | The study was a retrospective review of case notes of babies delivered in the labour ward of the Lagos University Teaching Hospital (LUTH), Nigeria and admitted into the inborn unit of the Neonatal Intensive Care Unit (NICU) of the hospital between January and June 2015. Improvised bubble CPAP had been in use in the unit for more than 1 year before the commencement of this study.
All newborn babies admitted into the NICU of LUTH and treated for respiratory distress at birth or shortly after birth, and whose shake tests results showed intermediate or high risk for RDS or with chest X-ray (CXR) suggestive of RDS were recruited. Babies with obvious congenital anomalies were excluded. Ethical approval was obtained from the institution’s ethics committee.
As per unit protocol, bCPAP is commenced soon after birth for at risk babies like the very preterm babies <33 weeks gestation or as soon as respiratory distress is observed. Due to unavailability of the expensive conventional bCPAP, our center uses improvised, locally constructed bCPAP to deliver CPAP to babies requiring it. The improvised bCPAP system costs approximately one thousand Nigerian naira, (≈USD 4.00), to set up. This cost effective improvised bCPAP system consisted of readily available materials in our locality viz: a neonatal nasal prong with tubing, an oxygen source and a calibrated plastic bottle. (Fig 1) The tube was cut on one side of the prong; the free end served as the expiratory limb. The other end was tied firmly and glued to prevent air leaks. The second tubing on the other side of the prong served as the inspiratory limb.
Fig 1: Equipment for bCPAP

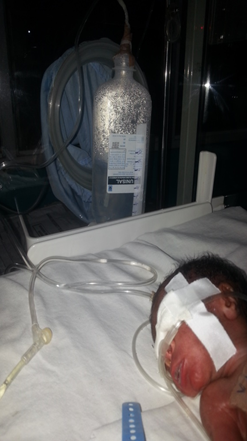
The inspiratory limb is connected to the humidified oxygen source while the expiratory limb is inserted into the plastic bottle. Prior to this, the paper tape was secured to the bottle and used to calibrate it. The bottle when filled with distilled water up to 5cm-8cm mark produces CPAP level of 5-8cm H2O. The expiratory limb is passed through the straw to keep it straight and it is ensured that the tube did not touch the bottom of the bottle. The oxygen flow meter is set at 5-8L/min and the nasal prongs are blocked to test for bubbling before connecting it to the baby. (Fig 2)
Fig 2: Baby on bCPAP
Relevant data extracted from mother’s case notes included: maternal age, parity, mode of delivery, multiple births and the use of ante-natal steroids. The variables collected from baby’s case notes included: sex of baby, gestational ages in weeks (calculated from the maternal last menstrual period, first trimester ultrasound or Modified Ballard score), birth weights, 5th minute Apgar score, CXR findings, shake test results, surfactant use, age at commencement of CPAP and duration of CPAP. Other clinical data recorded were respiratory rate, temperature, heart rate, oxygen saturations pre- and post-CPAP, presence of CPAP complications like CPAP belly, intraventricular hemorrhage and outcome for the babies. Bubble CPAP was considered successful under the following circumstances: respiratory distress improved with minimal or no retractions, respiratory rate was 30-60cpm/min and saturation improved.
Statistical analysis: Data was presented using descriptive statistics. Student’s t-test was used to compare numerical variables. Multivariate analysis was used to identify significant associations between categorical variables. Discrete data was compared by Chi-square or Fisher exact test and p value <0.05 was considered significant.
| | | | Results | A total of 183 neonates were admitted into the inborn NICU of LUTH during the study period, out of which 88 were preterm babies. Of the preterm babies, 42 subjects who were diagnosed with RDS and met all the inclusion criteria were recruited into the study.
All the subjects had primary diagnosis of RDS with CXR findings in keeping with RDS. The maternal characteristics and the base line characteristics of the study subjects are shown in Tables I and II respectively.
Table I: Maternal characteristics of study subjects
| PARAMETERS |
n (%) |
| Maternal age (years) |
|
| 20-25 |
5(11.9) |
| 26-30 |
14(33.3) |
| 31-35 |
16(38.1) |
| 36-40 |
7(16.7) |
| Antenatal steroids |
|
| Received |
28(66.7) |
| Not Received |
14(33.3) |
| Mode of delivery |
|
| Caesarean section |
34(80.1) |
| Vaginal Delivery |
8(19.0) |
| No of babies delivered |
|
| Singletons |
27(64.3) |
| Twins |
12(28.6) |
| Triplets |
3(7.1) |
Table II: Baseline characteristics of study subjects
| PARAMETERS |
n (%) |
| Gestational ages (weeks) |
|
| <= 28 |
20(47.6) |
| 28-32 |
15(35.7) |
| 33-34 |
7(16.7) |
| Gender |
|
| Male |
16(38.1) |
| Female |
26(61.9) |
| Birth weight |
|
| <1000g |
14(33.3) |
| 1000 – 1499 |
15(35.7) |
| 1500- 2500 |
13(31) |
| 5 minutes APGARS |
|
| 0-4 |
3(7.1) |
| 5-7 |
12(28.6) |
| 8-10 |
27(64.3) |
The mean birth weight of subjects was 1256g±410.25g. As per protocol, all babies’ ≤33 weeks were commenced on bCPAP from the delivery room. Only 2 babies received surfactant administration (INSURE protocol) with median age at administration of 3.5 hours.
Oxygen saturation was monitored in all babies and the mean oxygen saturation pre- and post-CPAP were recorded. There were significant differences in mean oxygen saturations pre-CPAP (82.93±4.07) and post-CPAP (94.00±1.11) commencement (p= 0.02). The mean duration of bCPAP was 5±3.3days.
Outcome: Thirty-two babies were successfully weaned off CPAP with overall CPAP success rate of 76.2%. There were 16 (38.1%) mortalities during the study period. Ten (62.5%) of the deaths were RDS specific mortality with case fatality rate of 23.8%. Severe perinatal asphyxia had a mortality rate of 18.75% (3 children) while sepsis, necrotising enterocolitis and intraventricular haemorrhage were attributed to another 18.75% of the mortalities.
The mean birth weight of survivors were higher (1435.4g) compared to those who died (963.4g), with a p-value of <0.05. Babies that died had lower mean gestational age (27.8 weeks) than those that did not (30.3 weeks) though this was not statistically significant (p >0.05). Babies whose mothers did not receive antenatal steroids also recorded more significant mortality (8 deaths out of 14 babies) compared to 8 deaths out of 28 babies of mothers who received (p=0.001). | | | | Discussion | Improvised bCPAP has recently become the treatment of choice for respiratory distress syndrome in resource limited settings. (3,5) Its attraction has been the low cost as it can be constructed from locally available materials, (5,7) its potential to reduce need for invasive ventilation (3) and its efficiency in keeping the alveoli distended with minimal risks for lung injury and bronchopulmonary dysplasia (BPD). (8-10) Globally, there has been a trend toward use of CPAP in the management of RDS in the newborn with well documented benefits. (3-6,9,10) Different devices can be used to deliver CPAP; these include the conventional ventilators, variable-flow infant CPAP and the bubble CPAP. (7) With the improvised bCPAP used at our centre, we had a high success rate which is comparable to what other studies in developed countries achieved on CPAP. (11,12) This may be attributable to the early commencement of bCPAP at delivery. Also most of the mothers received antenatal steroid (66.7%) which has been associated with improvement in lung maturity (13) with decrease in severity of RDS in preterm babies. (14) It is probable that the use of prenatal steroids in majority of the subjects (66%) could have contributed to the success of the CPAP in our subjects. Further prospective studies are currently ongoing to help elucidate this relationship.
Audu et al (5) in Abuja demonstrated immediate clinical improvement in oxygen saturation using customized bCPAP. Malik et al (15) noted a rapid rise in SPO2 to >85% when CPAP was commenced and this was sustained by survivors. The findings in the current study showed similar trend with a mean increase in SPO2 post commencement of CPAP from 82.9% to 94%.
Only 2 of our participants had surfactant administration as the others could not procure it due to its exorbitant price in Nigeria. Of the 2 babies that received surfactant, only one survived. Mortality in babies with RDS after administration of surfactant has also been documented in the studies by Rodriguez (16) and Rojas-Reye et al. (17) The baby that died in our study met the criteria for failed CPAP (despite surfactant administration) and would probably have benefitted from mechanical ventilation if it were available. Though surfactant therapy improves cardiorespiratory stability and oxygenation in babies with RDS, the need for respiratory support following its administration is well documented. (3,8-10,16-19) Where there is unavailability or failure of CPAP, mechanical ventilation becomes the choice of respiratory support as it offers quick normalization and maintenance of blood gases and acid-base balance. But it has the drawback that it can cause more barotrauma, air-leak syndromes and chronic lung injuries as well as being very expensive and unaffordable in most resource poor settings. (3,8-10,19)
The case fatality rate of 23.8% in the present study though high, was lower than the findings by other studies that reported RDS as accounting for more than half of their mortalities. The study also recorded mortality from other complications which are common in preterm babies such as intraventricular haemorrhage, necrotising enterocolitis, perinatal asphyxia and neonatal sepsis. Considering that nearly half (47.6%) of the cohort of neonates studied were products of ≤28 week gestation, severe RDS and its complications were expected. Babies that died during the study period had lower mean gestational age of 27.8 weeks and mean birth weight of 963.4g. Management of these very small babies is quite challenging and require dedication, use of newer, cost-effective and improved facilities to bring mortality to the barest minimum.
The positive results obtained in this study demonstrates that simple interventions can go a long way in reducing neonatal mortality rate; this can be cascaded down to other doctors and health care providers that care for these neonates through training and retraining of these personnel. This should include training on the assembly and use of bCPAP with anticipatory management of the complications that these delicate preterms are prone to. This would further reduce morbidity and mortality from RDS. It is however also important to continue research into how to improve the effectiveness and ensure safety of this improvised bCPAP to ensure that these babies benefit optimally from it and prevent or reduce complications. | | | | Conclusion | | Improvised bCPAP is a simple and cost effective intervention that can be used in resource limited settings to treat RDS in preterm babies and reduce morbidity and mortality due to surfactant deficiency. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Kamath B d, Maclure E M, Goldenberg R L, Job A L. Neonatal Mortality from respiratory Distress Syndrome: Lessons for low resource countries. Pediatrics 2011; 127(6): 1139-1146. [CrossRef] [PubMed]
- Federal Ministry of health. Saving newborn lives in Nigeria: Newborn health in the context of the integrated Maternal, Newborn and Child Health Strategy. 2nd edition. Abuja: Federal Ministry of Health, Save the Children, Jhpiego; 2011:26.
- Kawaza K, Machen HE, Brown J, Mwanza Z, Iniguez S, et al. (2014) Efficacy of a Low-Cost Bubble CPAP System in Treatment of Respiratory Distress in a Neonatal Ward in Malawi. PLoS ONE 9(1): e86327. doi:10.1371/journal.pone.0086327. [CrossRef]
- Urs PS, Khan F, Maiya PP. Bubble CPAP- A primary Respiratory support for respiratory distress syndrome in newborns. Indian Pediatr 2009; 46: 409 – 411. [PubMed]
- Audu LI, Otuneye AT, Mairami AB, Mukhtar MY. Improvised bubble continuous positive airway pressure (BCPAP) device at the National Hospital Abuja gives immediate improvement in respiratory rate and oxygenation in neonates with respiratory distress. Niger J Pead 2015; 46 (1) 12-16.
- Lanieta K, Joseph K, Josaia D, Samantha C, Trevor D. An evaluation of bubble-CPAP in a neonatal unit in a developing country: effective respiratory support that can be applied by nurses. J Trop Pediatr 2006; 52: 249-253. [CrossRef] [PubMed]
- Audu LI, Otuneye AT, Mukhtar MY, Mairami AB, Mshelia LJ, Garu M. Customized bubble continuous airway pressure device at the National Hospital Abuja for the treatment of respiratory distress syndrome (RDS). Niger J Paediatr 2013; 40(3)275-277.
- Narendran V, Donovav EF, Hoath SB, Akinbi HT, Steichen JJ, Jobe AH. Early bubble CPAP and outcomes in ELBW preterm infants. Journal of Perinatology (2003) 23, 195–199. [CrossRef] [PubMed]
- Lundstrom KE, Griesen G. Early treatment with nasal-CPAP. Acta Paediatr Scand 1993; 82:856. [CrossRef]
- Kamper J, Wulff K, Larsen C, Lindequist S. Early treatment with nasal continuous positive airway pressure in very low-birth weight infants. Acta Paediatr Scand 1993; 82:193–7. [CrossRef]
- Sahni R. Bubble CPAP: Can we predict success or failure? Indian Pediatr 2010; 47:139-143. [CrossRef]
- Ammari A, Suri M, Milisavljevic V, Sahni R, Bateman D, Sanocka U, et al. Variables associated with early failure of nasal CPAP in very low birth weight infants. J Pediatr 2005; 147: 341–347. [CrossRef] [PubMed]
- Roberts D, Dalziel S. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev 2006; CD004454. [CrossRef]
- Liggins GC, Howie RN. A controlled trial of antepartum glucocorticoid treatment for prevention of the respiratory distress syndrome in premature infants. Pediatrics 1972; 50:515. [PubMed]
- Malik R K, Gupta R K. A two year experience I Continuous Positive Airway Pressure Ventilation using nasal prongs and pulse oximetry MJAFI 2003;59:36-39.
- Rodriguez R. Management of respiratory distress syndrome: an update. Respir Care. 2003; 48(3):279 –286. [PubMed]
- Rojas-Reyes MX, Morley CJ, Soll R. Prophylactic versus selective use of surfactant in preventing morbidity and mortality in preterm infants. Cochrane Database Syst Rev. 2012;3(3):CD000510. [CrossRef]
- Yu V. surfactant replacement: Review article. Indian Paediatr 1998; 35: 1081-1096. [PubMed]
- Canadian Pediatric Society. Recommendations for neonatal surfactant therapy. Paediatrics & Child Health. 2005; 10(2):109-116. [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2016.11
|
| Cite this article as: | | Ezenwa B, Akintan P, Fajolu I, Ladele J, Ezeaka C. Bubble CPAP in the Management of Respiratory Distress Syndrome in Resource Constrained Settings: The Luth Experience. Pediatr Oncall J. 2016;13: 9-12. doi: 10.7199/ped.oncall.2016.11 |
|