Nibedita Mitra, G Kavitha, Madhuvanthi Rajendran, Prem Kumar, Nithin Siromony.
Department of Pediatrics, Southern Railway Head Quarter Hospital, Chennai, India.
ADDRESS FOR CORRESPONDENCE
Dr. Nibedita Mitra, B 142, Sunnyvale Apartment, 351 Kunnor High Road, Ayanavaram, Chennai-600023, India.
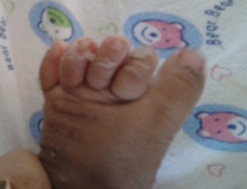
Email: nibeditamitra1@yahoo.co.in | Kawasaki Disease (KD) is difficult to diagnose in early infancy and can be missed due to its rarity and incomplete presentation. A five and half months old male infant presented with diarrhea and fever for four days. On admission, he was febrile (temperature 102 0F), irritable, had palmar and plantar erythema and maculopapular rash on the trunk. Infants with dengue fever were getting admitted in our ward with a similar presentation and a clinical diagnosis of dengue fever was considered for this child too. Initial investigations were inconclusive. Child continued to pass greenish stools, 8 to 10 times per day, with intermittent spikes of temperature (1020F to 1030F). Rash and palmar and plantar erythema decreased but the child developed perineal desquamation after admission and redness, dryness and cracking of the lips on the seventh day of fever. Repeat investigations on Day 11, revealed hemoglobin 8.3 gm/dl, platelet count of 11,03,000cell/cumm, white cell count 20,600 cells/cumm with a CRP 13.9 mg/dl and ESR was 80 mm in one hour. With the clinical symptoms of prolonged fever and rash, perineal desquamation and hyperaemia of the lips and supportive laboratory investigations of anemia, thrombocytosis, leucocytosis and raised CRP and ESR, a diagnosis of incomplete Kawasaki disease was considered. Echocardiogram demonstrated evidence of coronary artery dilatation with left anterior descending (LAD) coronary artery diameter 3.5mm (dilated) and right coronary artery diameter 1.5mm (within normal limits). Intravenous immunoglobulin at a dose of 2 gm/kg was given over a period of twelve hours, and aspirin was started at a dose of 80mg/kg/day. There was remarkable clinical improvement soon after completing the immunoglobulin infusion. aspirin was tapered to 5mg/kg after five days. Child developed periungal desquamation on fingers and toes on the sixteenth day of illness (Figure 1).
Figure 1: Periungal desquamation seen on the sixteenth day of illness
The proportion of KD patients younger than six months of age in relation to all KD patients reported is 11.2% in Japan and 7.7% in Korea. (1) Singh et al from India have reported that 3.6% of children with KD were below six months in their study. (2) Infants have substantially less extensive mucositis, pharyngitis, cervical lymphadenopathy and conjunctivitis. The most common findings were fever and rash. Infants had a high incidence of diarrhoea and irritability with a trend towards a more prolonged fever. (3) Relatively more children with incomplete presentation are in the extremes of age spectrum ≤ 1 year or ≥ 5 to 9 years. (4) The reported prevalence of incomplete presentation is 15 to 36.2% among patients with Kawasaki disease. More than three laboratory criteria of American Heart Association (AHA) guidelines support the diagnosis of incomplete Kawasaki Disease. (5) Mean time for coronary artery dilatation to develop is Day 10. Echocardiography, though important for diagnosis and follow-up, is inadequate as criteria for early treatment, and a normal echocardiogram should certainly not preclude treatment. (3) Long term management depends on the degree of coronary involvement. (5)
Thus, we conclude that Kawasaki Disease is rare in early infancy and can be easily missed due to its incomplete presentation. It should be considered in the differential diagnosis of infants with prolonged fever. All criteria for Kawasaki Disease may not be present at the same time and can appear in sequence. Continued surveillance and repeated revaluation of the child should be employed to detect any new clinical finding. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Yeom JS, Woo HO, Park JS, Park ES, Seo J-H, Youn H-S. Kawasaki Disease in infants. Korean J Pediatr 2013; 56(9): 377-382. [CrossRef] [PMC free article]
- Singh S, Agarwal S, Bhattad S, Gupta A, Suri D, Rawat A , et al. Kawasaki disease in infants below 6 months: a clinical conundrum. Int J Rheum Dis 2016. 2016 [Epub ahead of print] doi: 10.1111/1756-185X.12854. [CrossRef]
- Joffe A, Kabani A, Jadavji T. Atypical and complicated Kawasaki disease in infants – Do we need criteria? West J Med. 1995; 162: 322-327. [PMC free article]
- Yu JJ. Diagnosis of Incomplete Kawasaki Disease. Korean J Pediatr 2012;55(3):83-87. [CrossRef] [PMC free article]
- Newburger J, Takahashi M, Gerber M, Gewitz M, Tani L, Burns J et al. Diagnosis, Treatment and long-Term management of Kawasaki Disease. AHA Scientific Statement. Circulation. 2004; 110:2747-2771. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2017.27
|
| Cite this article as: | | Mitra N, Kavitha G, Rajendran M, Kumar P, Siromony N. Incomplete Kawasaki Disease in an infant with Diarrhea. Pediatr Oncall J. 2017;14: 73. doi: 10.7199/ped.oncall.2017.27 |
|