Dipankar Sarkar1, Shruti Sarkar1, Ashutosh S Mangalgiri2, Gagan Thakur3, Vijaya Beohar1.
1Department of Pediatrics, Peoples College of Medical Science & Research Center, Bhopal, India,
2Department of Anatomy, Peoples College of Medical Science & Research Center, Bhopal, India,
3Department of Oral and Maxillofacial Surgery, Peoples College of Medical Science & Research Center, Bhopal, India.
ADDRESS FOR CORRESPONDENCE
Dr. Dipankar Sarkar, Assistant Professor, Department of Pediatrics, Peoples College of Medical Science & Research Center, Bypass Road, Bhopal ,MP 462037. India.
Email: dipankarshruti@gmail.com | | Abstract | | Ludwig's angina is a rapidly spreading cellulitis of the floor of the mouth characterized by firm induration and elevation of the tongue. The cellulitis may spread and cause life-threatening complication by obstructing the airway. Several other complications have been reported secondary to the progress of cellulitis in different anatomical plains. We describe a case of a two year old girl with Ludwig's angina who developed left-sided marginal mandibular nerve palsy. This complication has never been reported before. | | | | Keywords | | Marginal mandibular nerve palsy, Ludwig's angina, complication | | | | Introduction | | Ludwig's angina is a potentially life-threatening infection of submandibular space characterized by hardness of floor of mouth (1). It presents most often with fever, neck mass or swelling and has a varying degree of systemic toxemic symptoms. The spreading cellulitis may cause complications like life-threatening obstruction of airway. Cellulitis may progress in different anatomical spaces extending to the lateral pharyngeal space, retropharyngeal space and may even descend to the mediastinum. We present here a case report of a two year old child with Ludwig's angina who had an unusual complication of paresis of marginal mandibular branch of facial nerve. | | | | Case Report | A two year old female child presented with fever for last 4 days along with swelling of the lower part of the face which was progressively increasing in size. She had mild cough and occasional vomiting. She was not taking any oral feeds and was quite irritable. She was the only child of her parents. She was born by normal delivery and her immediate neonatal period was uneventful. She was vaccinated with BCG, opv, DPT and mmr. Her development was normal and she did not have any significant illness before. On examination she was irritable, febrile and had pallor. She had a brawny, indurated and markedly tender significant swelling in the submandibular region extending both sides up to the parotid region. The floor of the mouth was raised. There was no pharyngeal or tonsillar inflammation. There were multiple enlarged lymph nodes in the neck region. She also had palsy of the left lower part of the face as her angle of mouth was getting deviated to the right side while crying indicating involvement of left marginal mandibular nerve, a branch of cervicofacial division of facial nerve (Figure 1). A clinical diagnosis of Ludwig's Angina was made.
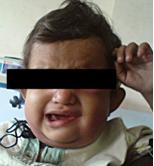
Figure 1: Illustration showing swelling in the submandibular region with deviation of angle of mouth towards right side.
On complete blood examination, hemoglobin was 9.2 g/dl and total WBC count was elevated to 13600/cu mm with predominant leucocytosis. CRP was positive and her random blood sugar was normal. An ultrasound of neck showed soft tissue swelling of the neck region with diffuse enlargement of submental lymph nodes along with diffuse bulkiness of parotid glands. No necrotic focus was seen. She was treated with IV ampicillin, cloxacillin, amikacin, dexamethasone, maintenance IV fluids, oral anti-inflammatory and analgesics. Over next 2 days, the fever was less but the swelling, tenderness and the left lower facial paresis persisted. She was unable to eat or drink and continued to be on IV fluids along with IV antibiotics and analgesic. After two days she was operated by maxillofacial surgeons and 25cc pus was drained from bilateral submandibular space and submental space and through & through communication between spaces was achieved by dissection. Corrugated rubber drains were placed and secured in place with the help of silk suture to achieve continuous drainage. Irrigation was done every day and dressing was placed. The pus culture did not show any growth. The child became afebrile within next 24 hours and the paresis of left lower part of the face improved. She had a gradual recovery over next 3-4 days and she was discharged home after 5 days with oral antibiotics. The paresis resolved completely before discharge. | | | | Discussion | Ludwig's angina is a rapidly progressing cellulitis involving the submandibular neck space. It is characterized by brawny induration of the submental region and floor of mouth, bearing the potential for rapid airway obstruction. It was formally described by von Ludwig in 1836, and criteria for diagnosis were developed by Grodinsky in 1939 (2). Patients with Ludwig's angina classically present with progressive bilateral submandibular and submental neck swelling, firm induration of the floor of the mouth, and edematous posterior and superior displacement of the tongue. The systemic symptoms generally are fever, chills, malaise, dehydration from decreased oral intake, and a generalized toxic ill-appearance. Other symptoms may include tongue and throat pain, dysphagia, trismus, dysphonia, and drooling (3) Infants less than 9 months old most often present with a neck mass or swelling, lymphadenopathy, fever, rhinorrhea, poor oral intake, and cough (4).
The cellulitis rapidly involves sublingual space with subsequent expansion of the floor of the mouth. This results in displacement of both the oral tongue superiorly and the base of the tongue posteriorly, producing a potentially life-threatening obstruction of the airway at the level of the oral cavity and oropharynx (3). Various complications may arise secondary to progress of the cellulitis in different anatomical plains. Those include mediastinitis and mediastinal abscess formation, subphrenic abscess formation (5), pneumothorax(6), pericardial or pleural effusion, necrotizing fasciitis, jugular venous thrombosis, rupture of the innominate artery (7), empyema (8), and mandibular or cervical osteomyelitis (9). Besides these complications, a generalized sepsis syndrome (10, 11) or aspiration pneumonia (7) also have been reported. But unilateral palsy of any branch of facial nerve secondary to Ludwig's angina has never been reported before in literature. This complication can also be explained on anatomical basis (1,12). Kissig et al (2006) described clinical findings from 35 cases of paralysis of distinct branches of facial nerve and out of those marginal branch of mandibular nerve was involved in 21 cases. The various causes described were iatrogenic, tumour, trauma, congenital, idiopathic and inflammation (13). In this particular case, the complication could have arisen due to involvement of the marginal mandibular nerve secondary to the inflammatory process. This particular complication of paresis of marginal mandibular branch of facial nerve secondary to Ludwig's angina has never been reported before. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Hollinshed WH. Anatomy for Surgeons, The Head & Neck, A Hober Harper Book, USA, 1958;1: 282-339.
- Spitalnic SJ, Sucov A. Ludwig's angina: case report and review. J Emerg Med. 1995; 13: 499-503. [CrossRef]
- Lin HW, O'Neill A, Cunningham MJ. Ludwig's angina in the pediatric population. : Clin Pediatr (Phila). 2009; 48: 583-587. [CrossRef]
- Cmejrek RC, Coticchia JM, Arnold JE. Presentation, diagnosis, and management of deep-neck abscesses in infants. Arch Otolaryngol Head Neck Surg. 2002; 128: 1361-1364. [CrossRef]
- Bounds GA. Subphrenic and mediastinal abscess formation: a complication of Ludwig's angina. Br J Oral Maxillofac Surg. 1985; 23: 313-321. [CrossRef]
- Barsamian JG, Scheffer RB. Spontaneous pneumothorax: an unusual occurrence in a patient with Ludwig's angina. J Oral Maxillofac Surg. 1987; 45: 161-168. [CrossRef]
- Ruiz CC, R.-Labajo AD, Vilas IY, Paniagua J. Thoracic complications of deeply situated serious neck infections. J Craniomaxillofacial Surg, 1993; 21:76-81. [CrossRef]
- Van der Brempt X, Derue G, Severin F, Colin L, Gilbeau JP, Heller F. Ludwig's angina and mediastinitis due to Streptococcus milleri: usefulness of computed tomography. Eur Respir J. 1990; 3: 728-731. [PubMed]
- Megran DW, Scheifele DW, Chow AW. Odontogenic infections. Pediatr Infect Dis. 1984; 3: 257-265. [CrossRef]
- Gridley J, Franaszek J. Ludwig's angina and pneumococcal sepsis. J Emerg Med. 1986; 4: 201-204. [CrossRef]
- Quinn P, Guernsey LH. The presentation and complications of odontogenic septic shock. Report of a case. Oral Surg Oral Med Oral Pathol. 1985; 59: 336-339. [CrossRef]
- Standring S. Gray's Anatomy Ch 29, Face & Scalp, 39th edn Elsevier, Churchill Livingstone, Edinburgh, 2005: 497-517.
- Kissig B, Zierz S. Isolated pareses of the terminal branches of the facial nerve: clinical findings, etiology and differential diagnosis. Fortschr Neurol Psychiatr. 2006; 74: 371-376. [CrossRef]
|
| Cite this article as: | | Sarkar D, Sarkar S, Mangalgiri A S, Thakur G, Beohar V. Marginal Mandibular Nerve Palsy as an Unusual Complication in Ludwigs Angina. Pediatr Oncall J. 2010;7: 11-13. |
|