Dr Ira Shah.
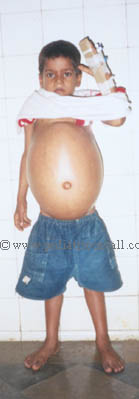
Medical Sciences Department, Pediatric Oncall, Mumbai, India. | | Case Report | A 7 years old male child presented with gradually increasing abdominal distension since 2 ½ months and breathlessness since 15 days. On examination, he had a tense ascitis. His weight was 15 kg and height was 105 cms suggestive of chronic malnutrition. There was no edema, icterus and hepatomegaly. Ascitic tap was milky and microscopy showed no cells with proteins of 1.08 gm%. Ascitic fluid chylomicrons was positive and ether test was positive. Peritoneal biopsy showed occasional mesothelial cells with plenty of lymphocytes and no malignant cells suggestive of tuberculous etiology. His Mantoux test was positive 14 x 14 mm. USG Abdomen did not show any IVC obstruction. CT abdomen was not suggestive of mesenteric cyst or thoracic duct damage. Thus a diagnosis of tuberculous peritonitis was made and the child was started on 4 drug AKT and steroids. At start of therapy, his abdominal girth was 68.5 cms, which decreased to 62 cms after 2 months of therapy, and ascitis completely disappeared after 4 months of therapy.
 | | | | Discussion | Chylous ascitis - It is defined as presence of milky, turbid or creamy ascitic fluid due to presence of increased triglyceride (fat) content of>1000 mg/dl either due to presence of intestinal or thoracic lymph. The common causes are congenital anomaly of lymphatics, obstruction of thoracic duct within its abdominal portion due to trauma, tumor, large lymph nodes and rupture of major lymphatic channel. The other causes are tuberculosis, filariasis, nephrotic syndrome, cirrhosis, rheumatoid arthritis and other serositis. When the patient is fasting, the milky color will fade and the fluid looks like a transudate with predominance of lymphocytes.
In patients with chronic peritonitis and persistent ascitis, the fluid color may be milky due to degeneration of inflammatory products (leukocytes/tumor cell) and may be confused with chylous fluid. However it can be distinguished from chylous ascitis by doing the ether test. When a drop of ether is added to the turbid ascitic fluid, the top layer clears in chylous fluid whereas it does not in a pseudochylous fluid.
Treatment of chylous ascitis consists of dietary management and therapeutic paracentesis. A low fat diet containing medium chain triglycerides with high protein diet is advocated. (MCT are directly absorbed in the portal circulation). Treatment may be required for several months for effective medical management. A surgical abdominal exploration may be required to detect the site of the leak.
Tuberculous ascitis may occur with few constitutional symptoms despite extensive involvement of the peritoneum. Radiographic evidence of pulmonary lesions is such cases are minimal. Direct smear of ascitic fluid may not show acid-fast bacillus. The best diagnostic methods are culture of the fluid and histopathological reading of biopsy of the peritoneum. Treatment consists of anti tuberculous drugs with surgery being reserved for cases with enteritis leading to bowel obstruction, perforation, fistula or a mass that does not resolve with drug therapy. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- IAP Textbook of Pediatrics - A. Parthasarthy, 2nd edition, Jaypee Brothers Medical Publishers (P) Ltd., New Delhi, 2002, pg - 457-458. 2. Ackerman's Surgical Pathology - Vol.II, Juan Rosai - 8th edition, Mosby Year Book Inc., St. Louis, 1996, pg - 2136.
|
| Cite this article as: | | Shah I. CHYLOUS ASCITIS. Pediatr Oncall J. 2004;1. |
|