|
All that Blisters is not Herpes
Pavitra Viswanathan, Sahana Devadas.
Department of Pediatrics, Bangalore Medical College and Research Institute, Bangalore, India.
ADDRESS FOR CORRESPONDENCE
Dr Pavitra Viswanathan, S1, Pinewood Golflinks, S.R.layout, Murugeshpalya, Bangalore-560001, India.
Email: drpavitraviswanathan@gmail.com
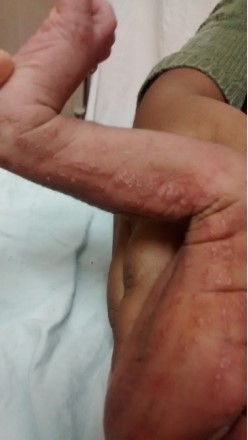
Figure 1: Day 5- Blistering lesions

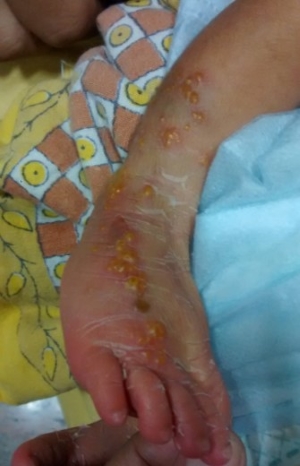
Figure 2: Day 7- Verrucous lesions
|
Figure 1: Day 5- Blistering lesions
|
What is the diagnosis?
Incontinentia pigmenti {IP}. It is a rare, X- dominantly inherited neurocutaneous syndrome with birth prevalence of approximately 1 in 143,000. The female to male ratio is 20:1. Bardach originally described the condition in twin sisters in 1925. Incontinentia pigmenti is due to a mutation in the NF- kappa B essential modulator {NEMO}, inhibitor kappa kinase {IKK}-gamma gene. {1} The disorder primarily affects the tissues and organs derived from ectoderm or neuroectoderm and represents a type of ectodermal dysplasia. {2} The skin lesions usually present in four stages: I-vesiculobullous lesions on the limbs, scalp and frequently on trunk, II-verrucous streaks , III-reticulated hyperpigmentation, IV- Linear hypopigmented band lacking hair and sweating. {3,4} It is imperative to consider IP in the differential diagnosis of vesicular lesions in newborn since the prognosis and outcome is significantly different from that of the common disorders with vesiculobullous skin manifestations. Retinal changes are: peripheral avascular zone, tortuous and irregular vessels, aneurysmal-like dilatation and neovascular changes. Non-retinal associations include microphthalmos, ptosis, strabismus, cataracts, conjunctival and iris changes of pigmentation. {3} IP patients can show various central nervous system manifestations {ulegyria, acute destructive encephalopathy, hemorrhagic necrosis, brain edema, and encephalitis with hemorrhagic necrosis}. {2,3} Skeletal abnormalities include spina bifida, hemivertebrae, accessory ribs, and syndactyly. {3} Delayed dentition, pegged teeth, and abnormal crown formation are also seen. {5} Treatment remains symptomatic and supportive. Recent reports indicate some success in treating early skin lesions with corticosteroids and topical tacrolimus. Spastic disorders, pyramidal disease, club foot, scoliosis, and other features need specific treatment for each alteration, such as physiotherapy, specific surgery for scoliosis or other orthopedic problems and antiepileptic drugs substances for epilepsy. {4}
Contributor Statement: Both authors were involved in the management of the case, literature survey and drafting of the document.
Financial Disclosure: None
Conflict of interest: None |
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
|
- Jones KL, Jones MC, Campo MD. Hamartoses, incontinentia pigmenti syndrome. In: Smith's Recognizable patterns of Human malformation. 7th edn. Elsevier Health Sciences. 2013:654 [PMC free article]
- Maingay-de Groof F, Lequin MH, Roofthooft DW, Oranje AP, de Coo IF, Bok LA, et al. Extensive cerebral infarction in the newborn due to incontinentia pigmenti. Eur J Paediatr Neurol 2008; 12: 284-9. [CrossRef] [PubMed]
- Pascual Castroviejo I, Ruggieri M, Incontinentia pigmenti. In: Ruggieri M, Pascual Castroviejo I, Di Rocco C. Neurocutaneous Disorders, Phakomatoses and Hamartoneoplastic Syndromes. Springer. Germany. 2008: 393-404 [CrossRef]
- Emre S, Firat Y, Güngör S, Firat AK, Karincaoglu Y. Incontinentia pigmenti: a case report and literature review. Turk J Pediatr. 2009 Mar-Apr; 51(2):190-4 [PubMed]
- Kitakawa D, Fontes PC, Magalhães FA, Almeida JD, Cabral LA. Incontinentia pigmenti presenting as hypodontia in a 3-year-old girl: a case report. J Med Case Rep. 2009; 3:116. [CrossRef] [PubMed] [PMC free article]
|
|
DOI: https://doi.org/10.7199/ped.oncall.2016.15 |
| |
Cite this article as:
Viswanathan P, Devadas S. All that Blisters is not Herpes. Pediatr Oncall J. 2016;13: 53. doi: 10.7199/ped.oncall.2016.15
|