Shinas Nellicka, Abraham John, Vivin Abraham.
Department of Pediatrics, Medical Trust Hospital, Kochi, Kerala, India.
ADDRESS FOR CORRESPONDENCE
Dr. Shinas Nellicka, Senior Resident, Department of Pediatrics, Medical Trust Hospital, MG Road, Kochi, Kerala-681016, India.
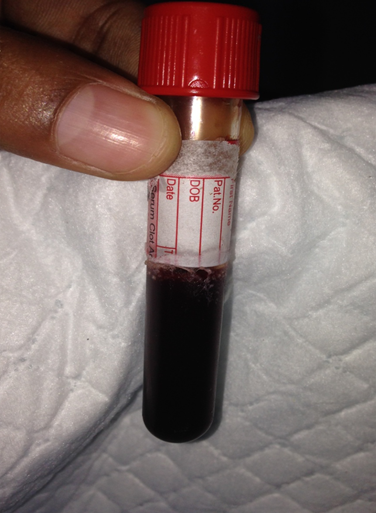
Email: shinas_156@hotmail.com | | Keywords | | Methemoglobinemia, Saturation Gap, Chocolate Colored Blood | | | A 1 year old female child born of non-consanguineous marriage presented with bluish discoloration of skin and mucosa since 6th months of life. Echocardiography done at 6th months of life was normal. Child had global developmental delay with a developmental quotient of 25%. She was the 3rd child born to G3P2L2 mother. Mother had history of intrauterine death at 6th months of first pregnancy. On examination, the child had central cyanosis and microcephaly. On Central nervous system examination, there was generalized hypertonia and brisk deep tendon reflexes. Other systems were normal. Pulse oximeter showed an oxygen saturation (So2) of 76% at room air which increased to 83% on administration of oxygen. Venous blood drawn was dark chocolate brown in colour (Figure 1). Chest x-ray and repeat echocardiography were normal. Arterial blood gas analysis revealed a pH of 7.35, pO2 252, So2 98%. The simultaneous pulse oximetry showed a saturation of 74%. MRI brain was normal. Methemoglobin levels were 24.7% by biochemical method. In view of global developmental delay, generalized hypertonia, saturation gap, dark colored venous blood and high methemoglobin levels a diagnosis of congenital methemoglobinemia type II was made. Child was started on high dose ascorbic acid following which cyanosis reduced clinically.
Figure 1: Chocolate brown colored blood
Methemoglobinemia is suspected when a patient presents with cyanosis and dyspnea that are unrelated to cardiopulmonary causes. Methemoglobin is the oxidized form of hemoglobin, which does not bind oxygen and increases the affinity of oxygen for the partially oxidized portion of hemoglobin. In normal circumstances only 1-2 % of the body’s hemoglobin exists as methemoglobin. (1) Increased levels of methemoglobin may be due to congenital absence of enzymes that normally reduce the ferrous ion or it may be acquired. A variety of drugs and toxins can lead to acquired methemoglobinemia. Type II congenital methemoglobinemia constitutes approximately 10% of all cases of congenital methemoglobinemia and usually causes death within the first few years of life. (2) The distinguishing features of type II is an unremitting, progressive, neurologic deterioration, characterized by mental retardation, microcephaly, opisthotonus, athetoid movements, and generalized hypertonia. (3) Signs and symptoms vary depending on the concentration levels of methemoglobin ranging from mild cyanosis to seizure, coma and death. Two very important clues in diagnosing this disorder include central cyanosis that does not improve with administration of supplemental oxygen and blood that appears darker than normal. (4) Another important pointer to the diagnosis of methemoglobinemia is the presence of a “saturation gap.” This occurs when there is a difference between the So2 that has been measured by means of pulse oximetry (the lower value) and the So2 that has been calculated by means of arterial blood-gas analysis. Typically, this saturation gap is greater than 5% in cases of methemoglobinemia. (5) Ascorbic acid in a dose of 200-500 mg/day is an effective treatment for congenital methemoglobinemia as it directly reduces methemoglobin, but the rate of the reaction is too slow. Inspite of these limited treatment congenital methemoglobinemia type 2 has poor prognosis. | | | | Contributor Statement | | NS: Case management and writing the manuscript; JA and AV: Case management and critical appraisal of the manuscript. All authors approved the final manuscript. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Trapp L, Will J. Acquired methemoglobinemia revisited. Dent Clin North Am. 2010; 54:665-75. [CrossRef]
- Hirono H. Lipids of myelin, white matter and gray matter in a case of generalized deficiency of cytochrome b5 reductase in congenital methemoglobinemia with mental retardation. Lipids 1980;15:272–275. [CrossRef]
- Worster-Drought C, White JC, Sargent F. Familial idiopathic methemoglobinemia associated with mental deficiency and neurologic abnormalities. Br Med J 1953;2:114–118. [CrossRef] [PMC free article]
- Rehman HU. Methemoglobinemia. Available from URL: http://www.emedicine.com/ped/topic1432.htm. Accessed on January 25 2016.
- Akhtar J, Johnson BD, Krezenlok EP. Mind the gap. J Emerg Med. 2007 August; 33(2): 131-2. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2017.19
|
| Cite this article as: | | Nellicka S, John A, Abraham V. CONGENITAL METHEMOGLOBINEMIA TYPE 2 - A RARE CASE REPORT. Pediatr Oncall J. 2017;14: 45-46. doi: 10.7199/ped.oncall.2017.19 |
|