|
Genital Lesions in a Teenager
Sofia Reis1, Paulo Morais2.
1Department of Pediatrics, Tondela-Viseu Hospital Center, Viseu, Portugal,
2Department of Dermatology, Tondela-Viseu Hospital Center, Viseu, Portugal.
ADDRESS FOR CORRESPONDENCE
Sofia Reis, Department of Pediatrics, Av. Rei D. Duarte, 3504-509 Viseu, Portugal.
Email: reis.carlasofia@gmail.com
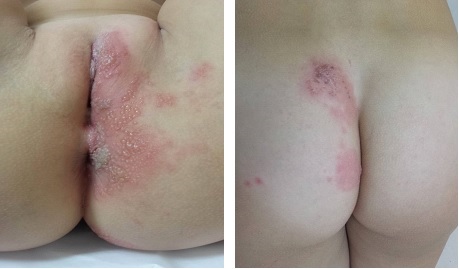
Figure 1: Grouped herpetiform vesides located in the left labium majus, perineum and homolateral buttock.
|
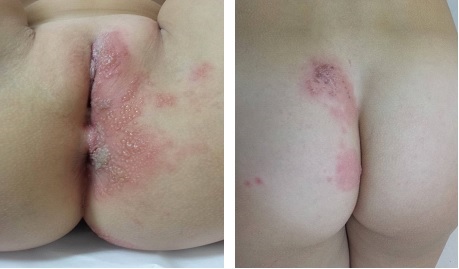
Figure 1: Grouped herpetiform vesides located in the left labium majus, perineum and homolateral buttock.
|
What is the diagnosis?
Based on the diagnostic hypotheses of shingles or HSV infection with zosteriform distribution, she was treated with acyclovir and paracetamol, gabapentin and prednisolone. However polymerase chain reaction (PCR) for VZV in the exudate was positive while that for HSV-1 and 2 were negative.
Herpes zoster (HZ), also known as shingles, corresponds to VZV reactivation in persons with previous history of chickenpox. (1,2) Its incidence increases with age and is uncommon under the age of 15 years. (1) It is associated with primary infection in utero, immunosuppression (especially cellular immunity) and/or aging. The lesions are, characteristically, unilateral and distributed in a dermatome. (1,2) Although the diagnosis of childhood HZ can usually be made clinically, differentiating it from zosteriform HSV infection may be difficult. In those cases, direct fluorescent antibody staining and PCR method (as performed in our patient) can precisely identify the virus in skin lesion specimens. (3)
The first line of therapy for uncomplicated HZ in immunocompetent children is oral acyclovir (20 mg/kg/dose, maximum 800 mg/dose, four times a day for 5 to 7 days), while intravenous acyclovir (10 mg/kg or 500 mg/sqm, three times a day for 7 to 10 days) is the treatment of choice for immunocompromised children. (1,4) Systemic acyclovir therapy accelerates the healing of skin lesions and the resolution of acute neuritis, and decreases the risk of post-herpetic neuralgia. Due to severe pain, functional impairment and rapid extension of the lesions, our patient was admitted to the pediatric ward and was treated with intravenous acyclovir (10 mg/kg, every 8 hours), gabapentin (15 mg/kg/day, given in three divided doses) and paracetamol (15 mg/kg/dose, every 8 hours) for 7 days, and prednisolone for 3 days (1 mg/kg/day). |
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
|
- La Russa PS, Marin M. Varicella-zoster virus. In: Kliegman RM, Stanton BF, St Geme JW III, Schor NF, editors. Nelson Textbook of Pediatrics. 20th ed. Philadelphia, PA: Elsevier. 2016: 1579-86.
- Gabutti G, Franchi M, Maniscalco L, Stefanati A. Varicella-zoster virus: pathogenesis, incidence patterns and vaccination programs. Minerva Pediatr. 2016;68(3):213-25. [PubMed]
- Nikkels AF, Nikkels-Tassoudji N, Piérard GE. Revisiting childhood herpes zoster. Pediatr Dermatol. 2004;21(1):18-23. [CrossRef] [PubMed]
- Leung AK, Robson WL, Leong AG. Herpes Zoster in Childhood. J Pediatr Health Care. 2006;20:300-3. [CrossRef] [PubMed]
|
|
DOI: https://doi.org/10.7199/ped.oncall.2017.43 |
| |
Cite this article as:
Reis S, Morais P. Genital Lesions in a Teenager. Pediatr Oncall J. 2017;14: 75. doi: 10.7199/ped.oncall.2017.43
|