Kei Wong, Gunjan Tiyyagura, Melissa L Langhan.
Department of Pediatrics, Section of Pediatric Emergency Medicine, Yale University School of Medicine, Connecticut, USA.
ADDRESS FOR CORRESPONDENCE
Kei Wong M.D, Department of Pediatrics, Section of Pediatric Emergency Medicine, Yale University School of Medicine, 100 York Street (Suite 1F) New Haven, Connecticut, USA.
Email: Kei.Wong@yale.edu | | Abstract | | The sleeping arrangements of young children may depend on factors such as socioeconomic limitations and cultural beliefs. Approximately 3,700 infants die annually in the United States from sudden unexpected infant deaths (SUID), including sudden infant death syndrome (SIDS), accidental suffocation and less frequently reported, strangulation of the neck because of hair tourniquet syndrome when a young child co-sleeps with family members who have long hair. This case report describes a 13-month old male who was brought to the pediatric emergency department after he was found entangled with his mother’s hair around his neck. The mother was awoken by her son’s movement, struggling to breathe in bed. Given the unusual nature of the event, presentation of the child with diffuse facial petechiae and circumferential ligature mark that extended around his neck, the child was admitted to the general pediatric ward for observation and further investigation of possible non-accidental trauma. To the best of our knowledge, only two previous case reports of such strangulation from human hair were reported within the last 2 decades. The aim of this case report is to increase physician and parental awareness of the potential danger in accidental strangulation during co-sleeping, and promote safe sleep environments. | | | | Keywords | | Hair tourniquet syndrome, near strangulation, co-sleeping, accidental strangulation, sleep-related deaths. | | | | Introduction | | It has become increasingly important to address causes of sleep-related infant death. Approximately 3,700 infants die annually in the United States from sudden unexpected infant deaths (SUID), including sudden infant death syndrome (SIDS), ill-defined deaths, and accidental suffocation and strangulation in sleep.1 The number of infant deaths initially decreased in the 1990s after a national safe sleep campaign but has plateaued in recent years.1,2 Although rare, hair tourniquet syndrome has been recognized since the 17th century.3,4 Hair tourniquet syndrome is often considered in the medical evaluation of the irritable or crying infant, with the majority of cases involving digits and external genitalia.3,4,5 Less frequently reported is strangulation of the neck as a result of hair tourniquet syndrome when a young child co-sleeps with family members who have long hair.5,6,7,8,9 To prevent such injury, our case highlights the importance of parental education on risk factors associated with co-sleeping, and our role as pediatricians to promote safe sleeping environment during anticipatory guidance. | | | | Case Report | A 13-month old male was brought to the pediatric emergency department (ED) after he was found entangled with his mother’s hair around his neck. The mother was awoken by her son’s movement, struggling to breathe in bed. By the time the father returned to the bedroom with scissors, the mother had freed the child. At this point, the child was lethargic and developed a facial rash. Prehospital personnel noted that the child had no respiratory compromise and returned back to his baseline mental status prior to arrival to ED. On presentation, the child was quiet, consolable when he cried, and in no apparent distress. Vital signs were normal for age with pulse oximetry of 100% on room air. On examination, the child had diffuse facial petechiae without subconjunctival hemorrhage, and a linear circumferential ligature mark that extended around his neck (Figure 1). The remainder of his examination, diagnostic imaging (computed tomography (CT) of the head, CT angiogram of the neck, and chest x-ray) and laboratory work up (complete blood count and comprehensive metabolic panel with lipase) were unremarkable. Given the unusual nature of the event, the child was admitted to the general pediatric ward for observation and investigation of possible non-accidental trauma.
Hospital Course: Based on concern of inflicted strangulation, patient underwent a skeletal survey to rule out occult fractures and MRI of the neck under anesthesia to rule out cervical ligamentous and spinal injuries. He was evaluated by child abuse specialists who concluded that, while unusual, mom’s hair causing a tourniquet around the patient’s neck while co-sleeping was a plausible explanation. The mother’s hair reached to the mid-point of her back. No other risk factors were noted in the social history. The child remained well, was subsequently cleared from his cervical collar, and discharged home the next day following negative skeletal survey to rule out occult fractures and MRI findings. His final discharge diagnosis was accidental strangulation from hair tourniquet syndrome.
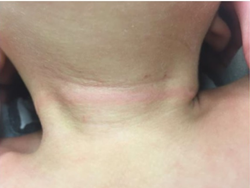
Figure 1. Erythematous linear circumferential ligature mark extended around the neck from hair tourniquet.
| | | | Discussion | Classically, hair tourniquet syndrome involves a single human hair or fine thread producing a tourniquet effect on an appendage.3,4 When not promptly recognized and immediately removed, this syndrome may result in necrosis of the affected appendage from impedance of lymphatic drainage, followed by arterial inflow obstruction.5 A physical property of human hair is that it stretches when wet and shrinks when dry, which is hypothesized to be a contributing factor.4,5 Hair tourniquets are found most commonly in children younger than 6 months of age. This coincides with postnatal telogen effuvium, or hair shedding.6 To the best of our knowledge, only two previous case reports of such strangulation from human hair were reported within the last 2 decades.5,7 The first case report by Kinley et al of a 27-month-old boy who suffered from an accidental strangulation by the mothers “unbraided waist length hair” as a result of co-sleeping with the mother.10 While the clinical aspects of hair tourniquet syndrome are well-described, the debate continues whether it is abusive or accidental in origin. Rare cases of hair tourniquets as a form of child abuse have been described in the setting of a caregiver creating a genital tourniquet to prevent nocturnal enuresis. Such cases are incredibly rare, while unintentional hair tourniquets are relatively more common.11,12
A policy statement released by American Academy of Pediatrics (AAP) on “SIDS and Other Sleep-related Deaths: Update 2016 Recommendations of Safe Sleeping Environment” calls for a safe sleep environment, including room-sharing without bed-sharing, to reduce the risk of sleep-related infant deaths.2,13 The report also includes new evidence that addresses the use of bedside and in-bed sleepers and adds additional recommendations on how to create a safe sleep environment.2,14
The sleeping arrangements of infants and children may depend upon multiple factors including socioeconomic limitations and cultural beliefs.5,13,14 The AAP recommends that providers have open and non-judgmental conversations with families about their sleep practices to promote a safe sleeping environment.2 | | | | Authors Contribution | | All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work. | | | | Financial Disclosure | | All authors have no financial relationships relevant to this article to disclose. | | | | Compliance with Ethical Standards | | Funding | | No funding was secured for this study | | | | Conflict of Interest | | All authors have no conflicts of interest to disclose. | | |
- Task Force on Sudden Infant Death Syndrome. SIDS and other sleep-related infant deaths: Updated 2016 recommendations for a safe infant sleeping environment. Pediatrics. 2016 Oct 27:e20162938.
- Mitchell EA, Thompson JM. Co-sleeping increases the risk of SIDS, but sleeping in the parents' bedroom lowers it. Sudden infant death syndrome: New trends in the nineties. Oslo, Norway: Scandinavian University Press; 1995.
- Hussin P, Mawardi M, Masran MS, Ganaisan P. Hair tourniquet syndrome: revisited. Il Giornale di chirurgia. 2015 Sep;36(5):219. [PubMed]
- Sivathasan N, Vijayarajan L. Hair-thread tourniquet syndrome: a case report and literature review. Case reports in medicine. 2012 Oct 15;2012.
- Chegwidden HJ, Poirier MP. Near strangulation as a result of hair tourniquet syndrome. Clinical pediatrics. 2005 May;44(4):359-61. [CrossRef] [PubMed]
- Templet TA, Rholdon RD. Assessment, Treatment, and Prevention Strategies for Hair-Thread Tourniquet Syndrome in Infants. Nursing for women's health. 2016 Aug 1;20(4):421-5. [CrossRef] [PubMed]
- Milkovich SM, Owens J, Stool D, Chen X, Beran M. Accidental childhood strangulation by human hair. International journal of pediatric otorhinolaryngology. 2005 Dec 31;69(12):1621-8. [CrossRef] [PubMed]
- Lim, N. The Courier Mail. Toddler 'strangled' in sleep. 17 June 2015[online] Available at: http://www.couriermail.com.au/questnews/southeast/toddler-strangled-with-sisters-hair-while-cosleeping-mothers-warning-goes-viral/news-story [Accessed 10 Oct. 2017].
- Ruszkiewicz AR, Lee KA, Landgren AJ. Homicidal strangulation by victim's own hair presenting as natural death. The American journal of forensic medicine and pathology. 1994 Dec 1;15(4):340-3.Kindley, A.D. and Todd, R.M., 1978. Accidental strangulation by mother's hair. The Lancet, 311(8063), p.565. [CrossRef]
- Claudet I, Pasian N, Debuisson C, Salanne S, Rekhroukh H. Tourniquet syndrome: interest of a systematic analysis of families' social conditions to detect neglect situations. Child abuse & neglect. 2009 Sep 30;33(9):569-72. [CrossRef] [PubMed]
- Klusmann A, Lenard HG. Tourniquet syndrome—accident or abuse?. European journal of pediatrics. 2004 Aug 1;163(8):495-8. [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Sudden Unexpected Infant Death and Sudden Infant Death Syndrome. https://www.cdc.gov/sids/data.htm. Accessed September 15, 2017.
- Moon RY, Hauck FR. SIDS Risk: It's More Than Just the Sleep Environment. Pediatrics. 2015 Dec 2:peds-2015.
- Bamber AR, Kiho L, Upton S, Orchard M, Sebire NJ. Social and behavioural factors in Non-suspicious unexpected death in infancy; experience from metropolitan police project indigo investigation. BMC pediatrics. 2016 Jan 12;16(1):6. [CrossRef] [PubMed] [PMC free article]
DOI: https://doi.org/10.7199/ped.oncall.2019.2
|
| Cite this article as: | | Wong K, Langhan M L, Tiyyagura G. Accidental Strangulation: A Rare but Potential Risk of Co-Sleeping. Pediatr Oncall J. 2019;16: 21-22. doi: 10.7199/ped.oncall.2019.2 |
|