Alexandra Martins1, Benedita Aguiar1, Ana Ferreira1, Joana Rodrigues1, Rosa Cardoso2, Denise Schmitt1, Margarida Azevedo1.
1Department of Pediatrics, Centro Hospitalar Entre o Douro e Vouga,
2Department of Radiology, Centro Hospitalar Entre o Douro e Vouga.
ADDRESS FOR CORRESPONDENCE
Alexandra Martins, Rua da Gandara, 36, Francelos, 4405-917, Gulpilhares, VNGaia.
Email: lmartins.alexandra@gmail.com | | Keywords | | Subcutaneous Fat Necrosis, hypocalcemia, preterm, sepsis | | | A male preterm was delivered at 33 gestational weeks after premature membrane rupture with placental abruption. A cesarean section was performed due to acute fetal distress. Birth weight was 2425 g. There was no need for resuscitation. He had transient tachypnea and supplemental oxygen was needed for 48 hours. Hypocalcemia was diagnosed on day seven of life (minimum serum calcium 6.3 mg/dL) that was treated with oral supplementation until day 16 of life. Afterwards serum calcium levels were always normal. On day 12, inflammatory signs appeared on the anterior surface of the right leg and ankle, with pain during manipulation. Within 24 hours, the preterm presented with signs of sepsis in form of fever, poor perfusion and aggravation of the inflammatory signs on his leg. C-reactive protein (CRP) and procalcitonin were elevated. He was treated with flucloxacillin, cefotaxime and gentamicin along with inotropes. Blood culture grew Enterobacter cloacae. Ultrasound (USG) of the ankle excluded intra-articular compromise. On day 16 a painful induration in his right leg was noticeable, although the inflammatory signs were improved (Figure 1). An x-ray showed subcutaneous calcification areas (Figure 2), seen by USG, confirming the diagnosis of SFN. Analytic inflammatory markers were always negative from the day 20 onwards, with improvement of the inflammatory signs. The newborn was discharged on day 34. He was reassessed at age of one month and 13 days of life. There was induration on the leg, with no inflammatory signs and no pain at manipulation. At age of six months, both the examination and laboratory results were normal, including calcium levels.
Figure 1. Erythematous subcutaneous nodules on day 16 of life.
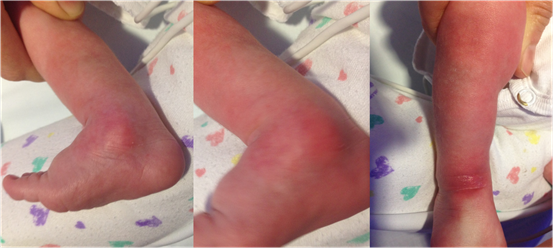
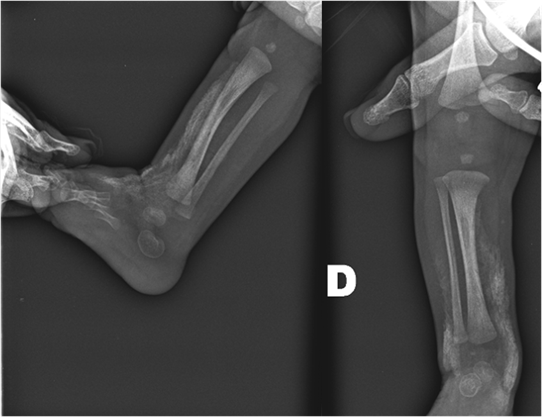
Figure 2. Right lower limb radiograph showing extensive linear and nodular subcutaneous calcifications.
Subcutaneous fat necrosis (SFN) is a rare clinical entity, which affects mostly term and post-term newborns and can lead to hypercalcemia.1,2 SFN is a rare type of panniculitis, occurring within the first weeks of life. The diagnosis is clinical, but x-ray and USG play an important role.3 The etiology of SFN is still unclear but some predisposing factors have been identified: perinatal hypoxia, hypothermia, meconium aspiration, Rh incompatibility, trauma and sepsis.1 Our patient had several risk factors such as mild neonatal hypoxia and sepsis. The main differential diagnosis is sclerema neonatorum (SN), which affects typically severely ill newborns, begins in the lower limbs and has a poor prognosis.4 Although SFN is a benign, self-limited disease, several alterations may occur, namely hypercalcemia. In our patient, calcium levels were initially low and remained normal afterwards – this may be related to the prematurity. Despite normal levels in an initial phase, calcium levels must be monitored afterwards, since hypercalcemia may be delayed for 6 months after the onset of the skin lesions.5 Although self-limiting, SFN is a condition important to be diagnosed to identify potential complications and avoid unnecessary investigations and treatments. It is important for the neonatologist and radiologist, to be aware of this disease, so that it can be promptly identified. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Mitra S, Dove J, Somisetty SK. Subcutaneous fat necrosis in newborn-an unusual case and review of literature. Eur J Pediatr. 2011;170:1107–10. [CrossRef] [PubMed]
- Shumer DE, Thaker V, Taylor GA, Wassner AJ. Severe hypercalcaemia due to subcutaneous fat necrosis: presentation, management and complications. Arch Dis Child Fetal Neonatal Ed. 2014;99:F419-21. [CrossRef] [PubMed] [PMC free article]
- Onyiriuka AN, Utomi TE. Hypocalcemia Associated with Subcutaneous Fat Necrosis of the Newborn: Case Report and Literature Review. Oman Med J. 2017;32:518–21. [CrossRef] [PubMed] [PMC free article]
- Tran JT, Sheth AP. Complications of subcutaneous fat necrosis of the newborn: a case report and review of the literature. Pediatr Dermatol. 2003;20:257–61. [CrossRef]
- Lara LG, Villa AV, Rivas MMO, Capella MS, Prada F, Ensenat MAG. Subcutaneous Fat Necrosis of the Newborn: Report of Five Cases. Pediatr Neonatol. 2017;58:85–8. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2019.10
|
| Cite this article as: | | Martins A, Aguiar B, Ferreira A, Rodrigues J, Cardoso R, Schmitt D, Azevedo M. Subcutaneous Fat Necrosis in a Preterm Newborn - An Atypical Case. Pediatr Oncall J. 2019;16: 23-24. doi: 10.7199/ped.oncall.2019.10 |
|