Suba Guruprasad1, Mukesh Sanklecha2, Rama Yelikar3.
1Department of Pediatrics, Medeor Multispecialty Hospital, Manesar, Gurugram,
2Department of Pediatrics, Bombay Hospital Institute of Medical Sciences and Research, Marine Lines, Mumbai,
3Department of Neurology, Kokilaben Dhirubhai Ambani Hospital and Medical Research Centre..
ADDRESS FOR CORRESPONDENCE
Dr Suba Guruprasad, Department of Pediatrics, Medeor Multispecialty Hospital, Sector 5 IMT, Manesar, Gurugram- 122001, India.
Email: mail.suba.s@gmail.com | | Abstract | Aim: To compare the adverse effects of the three different bronchodilators in children with a wheeze.
Design: Randomised controlled double blind study
Setting: The study was conducted in the pediatric ward of a tertiary care institution in Mumbai, India. The study was conducted from December 2011 to October 2013.
Methods: Children aged one month to 18 years admitted to the pediatric ward with wheezing were included. Children needing intensive care units, those with co-existing renal or cardiac abnormalities, intolerance to the drugs or currently on medications that lower serum potassium levels or cause tachycardia, were excluded. Out of 130 eligible patients, 40 did not give consent. Remaining 90 were randomly allocated into 3 groups in the ratio of 1:1:1 by simple randomization using a random table provided by the statistician
Intervention: salbutamol, levosalbutamol and salbutamol + ipratropium bromide were administered to groups A, B and C respectively at intervals of twenty minutes for the first hour and then 6 hourly for the next 24 hrs. Heart rate, oxygen saturation, serum potassium levels and tremors at baseline, end of first hour and at twenty-four hours were compared in all the 3 groups.
Results: The average increase in heart rate at the end of the first hour was 11.1 + 7 beats/min in the group receiving salbutamol, 8.9 + 8 beats/min in patients receiving levosalbutamol and 8.4 + 6 beats/min in the salbutamol+ipratropium bromide group (p=0.07). At the end of 24 hours the group receiving salbutamol had an average increase in heat rate of 9.8 + 5 beats/min., 8.2 + 9 beats/min in the levosalbutamol group and 7.6 + 5 beats/min in the group receiving the combination (p=0.08). The mean baseline oxygen saturation percent were 97.7 + 1.08, 97.7 + 1.09 and 97.4 + 1.3 for the groups receiving salbutamol, levosalbutamol and salbutamol+ipratropium bromide respectively. The mean fall in the oxygen saturation in the three groups at the end of the first hour was 1.8 +1.1, 1.5+0.7 and 1.4+0.6 in the salbutamol, levosalbutmaol and salbutamol+ipratropium groups respectively (p=0.4). At the end of 24 hours the fall in saturations were 1.2 + 1.2, 0.9 + 1.1, 1.1+0.8 in the three groups respectively ( p=0.3). Fall in serum potassium levels was 0.08 + 0.5 in the group receiving salbutamol, 0.1 + 0.5 in the levosalbutamol group and 0.06 + 0.3 in the group receiving salbutamol with ipratropium bromide (p=0.4). Tremors were noted in 30% (9/30) of patients receiving only salbutamol.
Conclusion: The only adverse outcome that was significantly associated with salbutamol in our study was that of tremors. Considering the benign nature of this effect, and easy reversibility on stoppage of the drug switching to the more expensive levosalbutamol solely for this adverse effect is not justified and counseling parents regarding this potential adverse effect may be sufficient.
| | | | Keywords | | Salbutmol, levosalbutamol, ipratropium bromide, adverse effects, tachycardia | | | | Introduction | Acute asthma is a potentially life threatening emergency that is estimated to cause 250,000 deaths annually worldwide.1 All guidelines recommend the use of short acting beta-2 agonist as the first line therapy for children presenting with acute exacerbation.2 salbutamol is a racemic mixture of the (S) and (R) stereoisomers. The (R) isomer is the therapeutically active component responsible for the bronchodilator activity, while the (S) isomer, which was till recently thought to be an inert component, is now believed to be responsible for the adverse effects associated with salbutamol.3 levosalbutamol is a pure (R) isomer and is claimed to be free of the detrimental side effects associated with salbutamol.4 This claim however is not consistently supported in literature. There are conflicting opinions, worldwide, on whether there are sufficient benefits to justify the 5-10 times higher price tag.5 Guidelines recommend addition of ipratropium to the therapy in moderate to severe asthma in children not responding to first line short-acting beta 2 agonist nebulization.6 However, in practice, often the combination is used at the outset when a child presents to the emergency room. The combination of ipratropium bromide and salbutamol, which was earlier used widely, has now been entirely withdrawn from the market and replaced by a substantially more expensive combination with levosalbutamol.
In this study we aim to see the differences in the occurrence of clinically important adverse effects associated with these drugs and to establish if these differences justify choosing the more expensive alternatives.
Setting:
The study was conducted in a tertiary care center from December 2011 to October 2013. All children from one month to 18 years of age admitted to the pediatric ward with wheezing were included. Children admitted to intensive care units, those with co-existing renal or cardiac abnormalities, known intolerance to the drugs or currently on medications known to lower serum potassium levels or cause tachycardia like oral beta 2 agonists and diuretics, were excluded.
Study design:
This randomized, double-blinded, parallel-group study was designed to determine the safety and efficacy of levosalbutamol in comparison with salbutamol and salbutamol + ipratropium bromide. Sample size estimation for this study was done using a PS (Power and Sample Size) Software Version 2.1.31 (Vanderbilt,Canada) considering the mean changes in heart rate as the key parameter from other studies in literature.7,8 A sample size of 90 was required to detect differences between study medications with 95% power to show equivalence at a significance level of 5%. Ethical approval was taken from the institutional ethics committee (reference no.-BHMIS/6140). The trial was retrospectively registered with the clinical trial registry of India (CTRI/2017/11/010335). The drugs needed for the study were pre-packed and sealed prior to the recruitment of study participants, and labeled as A, B and C respectively. Neither the treating physician nor the patients were aware of the contents. Packet A contained salbutamol 2.5mg vials, packet B contained levosalbutamol 1.25 mg vials and packet C contained salbutamol + ipratropium bromide (2.5mg and 250 mcg respectively). Eligible patients were recruited as and when they presented in the outpatient department or the emergency room and were allocated to one of the three groups by a chit system. Written informed consent (and assent, where applicable) was obtained. Group A received salbutamol 0.15 mg/kg/dose (minimum dose of 2.5 mg), Group B was given levosalbutamol 0.075 mg/kg/dose (minimum dose of 1.25 mg) and Group C received salbutamol + ipratropium bromide (0.15mg/kg/dose of salbutamol + 250mcg of ipratropium bromide) which were administered by a nursing staff not involved in the study. Drugs were administered at intervals of twenty minutes for the first hour and then 6 hourly for the next 24 hours. Outcomes were measured at baseline, at first hour and at twenty-four hours.
Heart rate and oxygen saturation was monitored using a portable hand held pulse oximeter with a pediatric probe at baseline, at end of 1 hour and at end of 24 hours. Serum potassium levels were analyzed by biochemical methods at baseline and at end of 24 hours and tremors as reported by the parent or confirmed on clinical examination.
Statistical Analysis
Demographic characteristics were calculated by simple proportions. The mean values at the end of different time points within a group were compared using the Wilcoxon Signed Rank Test. Comparison of parameters between the three study groups was done using Kruskal-Wallis One Way Analysis of Variance on Ranks test. A P value less than 0.05 was considered significant.
| | | | Results | Among 130 patients who were eligible, 40 did not consent to participate in the study. All ninety patients enrolled in the study completed the study protocol (Figure 1). Patient demographic characteristics were similar among treatment groups (Table 1). The mean baseline oxygen saturation percent were 97.7+1.08%, 97.7+1.09% and 97.4+1.3% for the groups receiving salbutamol, levosalbutamol and salbutamol+ipratropium bromide respectively. Serum potassium levels at admission were 4.4+0.5 meq/L, 4.2+0.5 meq/L and 4.3+0.5 meq/L in the groups receiving salbutamol, levosalbutamol and combination therapy respectively. The changes in heart rate, oxygen saturation, serum potassium at the end of 1 hour and at the end of 24 hours in all the 3 groups is depicted in table 2. Tremors were observed in 9 out of 30 participants (30%) in the group receiving salbutamol.
Figure 1. CONSORT diagram depicting the enrollment of study participants into the three study groups
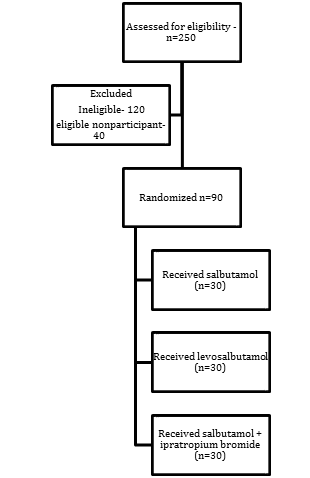
Table 1. Baseline characteristics of the study groups.
| Demographic feature |
Salbutamol |
Levosalbutamol |
Salbutamol with ipratropium bromide |
p-value |
| Age (mean) |
5.5+4.3 |
6.5+4.5 |
7.0+4.7 |
0.32 |
| Males (%) |
20 (70%) |
17 (56%) |
17 (56%) |
0.47 |
| Females (%) |
10 (30%) |
13 (43%) |
13 (43%) |
0.47 |
Table 2. Comparison of the outcome between the study groups.
Drugs ->
Outcome |
Salbutamol |
Levosalbutamol |
Salbutamol + ipratropium bromide |
p-value |
| Mean increase in heart rate 1st hour (beats/min) |
11.7+7 |
8.9+8 |
8.4+6 |
0.07 |
| Mean increase in heart rate at the end of 24 hours (beats/min) |
9.8+5 |
8.2+9 |
7.6+5 |
0.08 |
| Decrease in oxygen saturation at end of 1st hour (%) |
1.8+1.1 |
1.5+0.7 |
1.4+0.6 |
0.5 |
| Decrease in oxygen saturation at end of 24 hour (%) |
1.2+1.2 |
0.9+1.1 |
1.1+0.8 |
0.3 |
| Fall in serum potassium levels (24 hours) |
0.08+0.5 |
0.1+0.5 |
0.06+0.3 |
0.4 |
| | | | Discussion | The superiority of levosalbutamol over salbutamol in the management of children with acute asthma remains a controversy. Effect on heart rate, one of the clinically significant adverse effects anticipated with the use of salbutamol, was similar in all the three study groups at the end of the first hour and at 24 hours. Fall in oxygen saturation, although statistically significant in all three groups, did not lead to clinically significant hypoxia. This finding may be of relevance in cases where the baseline oxygen saturation is low and it may be prudent to use oxygen while nebulizing with any of the three drugs studied here. There were no significant changes in serum potassium levels associated with the use of any of the three drugs. The only adverse outcome that was significantly associated with salbutamol in our study was that of tremors. Considering the benign nature of this effect, and easy reversibility on stoppage of the drug switching to the more expensive levosalbutamol solely for this adverse effect is not justified and counseling parents regarding this potential adverse effect may be sufficient.
A literature review by Browoski et al compared seven randomized controlled trials and concluded that there were no significant differences in the efficacy, adverse effects and hospital admissions of levosalbutamol and salbutamol. They also found no evidence of a greater increase in heart rate with salbutamol compared to levosalbutamol.9 A systematic review in 2013, considered seven trials with 1625 participants. The pooled results failed to demonstrate superiority of levosalbutamol over salbutamol for respiratory rate, oxygen saturation, change in FEV1, side effects profile and duration of emergency department care. levosalbutamol was superior to salbutamol in decreasing hospital admission rate. However, this was contributed solely by one trial and the benefit was not evident after excluding this trial from the meta-analysis.10
Comparison of the effects of racemic salbutamol versus its combination with ipratropium bromide has shown no difference in the occurrence of side effects. A study comparing levosalbutamol with a combination of salbutamol and ipratropium bromide demonstrated efficacy and symptom profiles of nebulized levosalbutamol 1.25 mg comparable to nebulized salbutamol 5.0 mg combined with ipratropium bromide 0.25 mg. The study concluded that “the more expensive levosalbutamol did not shorten length of stay, reduce number of nebulized treatments, improve peak flow measurements, reduce symptomatic complications, or reduce unplanned return visits for asthma management when compared to combination therapy”.11
Asthma is a condition that needs long-term therapy and entails several other expenses. Considering the expense already associated with treatment, efforts must be made to rein in costs at every step. In the absence definite evidence of levosalbutamol’s superiority, the basis to recommend levosalbutamol over salbutamol is tenuous and financial considerations must be made when choosing one over the other.
Our study had certain limitations. A larger sample would improve the power of the study and our study is limited by it small sample size. Also, effect of fever on the parameters studied was not taken into consideration and may have acted as a confounding factor.
| | | | Compliance with Ethical Standards | | Funding | | Bombay Hospital Trust | | | | Conflict of Interest None | | |
- Masoli M, Fabian D, Holt S, Beasley R. The global burden of asthma: executive summary of the GINA Dissemination Committee report. Allergy. 2004;59:469-78. [CrossRef] [PubMed]
- Reddel HK, Bateman ED, Becker A, Boulet L-P, Cruz AA, Drazen JM, et al. A summary of the new GINA strategy: a roadmap to asthma control. Eur Respir J. 2015;46:622–39. [CrossRef] [PubMed] [PMC free article]
- Kercsmar CM, McDowell KM. Love it or lev it: levalbuterol for severe acute asthma--for now, leave it. J Pediatr. 2009;155:162–4. [CrossRef] [PubMed]
- Method for treating asthma using optically pure R(-) albuterol [Internet]. 1996 [cited 2016 Feb 1]. Available from: https://www.google.com/patents/US5547994
- Hendeles L, Hartzema A. Levalbuterol is not more cost-effective than albuterol for COPD. Chest. 2003;124:1176. [CrossRef]
- POCKET GUIDE FOR ASTHMA MANAGEMENT AND PREVENTION A Pocket Guide for Health Professionals Updated 2018 (for Adults and Children Older than 5 Years) BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION [Internet]. 2018 [cited 2019 Mar 10]. Available from: www.ginasthma.org.
- Punj A, Prakash A, Bhasin A. Levosalbutamol vs racemic salbutamol in the treatment of acute exacerbation of asthma. Indian J Pediatr. 2009;76:1131–5. [CrossRef] [PubMed]
- Gawchik SM, Saccar CL, Noonan M, Reasner DS, DeGraw SS. The safety and efficacy of nebulized levalbuterol compared with racemic albuterol and placebo in the treatment of asthma in pediatric patients. J Allergy Clin Immunol. 1999;103:615–21. [CrossRef]
- Browoski J MC. Nebulized albuterol versus levalbuterol in pediatric and adult patients : A review. Formulary (Cleveland, Ohio). 2009; 44(4):108-118
- Jat KR, Khairwa A. Levalbuterol versus albuterol for acute asthma: a systematic review and meta-analysis. Pulm Pharmacol Ther. 2013;26:239–48. [CrossRef] [PubMed]
- Ralston ME, Euwema MS, Knecht KR, Ziolkowski TJ, Coakley TA, Cline SM. Comparison of levalbuterol and racemic albuterol combined with ipratropium bromide in acute pediatric asthma: a randomized controlled trial. J Emerg Med. 2005;29:29–35. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2019.15
|
| Cite this article as: | | Guruprasad S, Sanklecha M, Yelikar R. Adverse Effects of Bronchodilators Used In Childhood Asthma - A Randomized Control Trial. Pediatr Oncall J. 2019;16: 45-48. doi: 10.7199/ped.oncall.2019.15 |
|