Agbere A D1, Koffi S1, Chiabi A2, Kouassi E K3, Assih D4.
1Paediatric Unit CHU-Tokoin, Lome, Togo,
2Yaounde Gynaecology-Obstetric and Paediatric Hospital, Yaounde, Cameroon,
3Division of Statistics,Studies and Research, Ministry of Health, Lome, Togo,
4Military Hospital, Lome, Togo.
ADDRESS FOR CORRESPONDENCE
A.D. Agbere, B.P. 20466, Lome, Togo.
Email: abdouagbere@yahoo.fr | | Abstract | Aim: To assess three key family practices concerning "appropriate home care", before implementation of community "Integrated Management of Childhood Illness" (C- IMCI) strategy in five Togolese health districts.
Methods: Done from the 29th March to 8th April 2004, simultaneously in these districts, our cross-sectional study comprised randomly 983 households, 506 caretakers and 733 under-five children. We studied mainly socio-demographic features and some family practices regarding home illness management through Epi-info and SPSS soft wares.
Results: 56.7% of the household heads were farmers, 53.6% illiterates, 47.6% aged between 30 and 49 years. A household comprised averagely seven people. The radio, gong and neighbours were the main ways of health information. In the previous two weeks, 20.6% of children suffered from fever (47% of sick children) and diarrhoea (19.9%). Caretakers managed them through self-treatment (50.3%) and health facility (35.8%). WHO/UNICEF/ORS (oral rehydration salts) (43.9%) and/or antibiotics (36.6%) were used for diarrhoea, and antimalarials (41.8%) and/or antibiotics (31.9%) for fever. 42.6% of caretakers consulted a health facility the day following onset of illness, 33.3% within one week. Only 12.3% of children had been fed more than usual with 47.2% by traditional force-feeding, and 39.7% had been given more appropriate liquids than usual. The most frequent accidents were falls (48.1%) and knife cuts (15.4%), and managed at home (47.1%), in the health facility (33.3%) and by traditional healers (19.6%).
Conclusion: Some milestones facing "appropriate home care", now available, will help follow up and evaluation of implementation of C-IMCI in the involved area. | | | | Keywords | | C-IMCI, appropriate home care, Togo. | | | | Introduction | Reducing under-five mortality rates in developing countries, one of the objectives of the "Integrated Management of Childhood Illness (IMCI)" strategy, needs more than health care services with competent personnel. Since families are the first caretakers of their children, success of this strategy can only be achieved with the support of these families and the community, so that health care at home should be favourable to the growth and development of these children. To face childhood disease, families should rightly react by appropriately seeking medical care, and by correctly administering the prescribed treatment. So, the family and community component of the IMCI strategy (C-IMCI) aims at developing, promoting and supporting family practices vital for the survival, growth and development of the child [1-4].
To follow-up and evaluate C-IMCI implementation in the five health districts it covers (East-Mono, Blitta, Sotouboua Tchaoudjo and Tchamba), the non-governmental organisation (NGO), PLAN Togo decided to study the key practices of C- IMCI [10-12] in these areas. Our study analysed three out of the five key family and community practices on "giving appropriate home care" which are: i)- Continue feeding and offer more fluids, including breast milk to children when they are sick ; ii)- Give sick children appropriate home treatment for infections and ensure that mothers should buy the drugs in the village pharmacy, and iii)- Take appropriate measures to prevent and treat wounds and accidents in children.
As soon as data analysis of the two remaining key practices of "giving appropriate homecare" is complete, both will be the subject of another publication : iv)- Prevent child abuse and neglect, and take appropriate measures whenever they occur, and v)- Ensure that men actively participate in health care of children and are implicated in the reproductive health of the family. | | | | Methods & Materials | The study was done in five PLAN Togo supported districts (East-Mono, Sotouboua, Tchaoudjo and Tchamba) which had a population of 553,000 inhabitants (11.2% of the Togolese population [10]) in 2003. We took as clusters, the sampling method in the five districts, which was previously used in the multiple indicators cluster survey (MICS)/UNICEF [11]. Out of 1000 households sampled, 983 effectively participated in the survey. The number of households surveyed in each district was proportional to the number of inhabitants. In each district, 33% of households were from urban areas and 67% rural. The number of households retained in each cluster and milieu was proportional to the size of the cluster, and sampling was random in each cluster.
After approval by the competent authorities, this cross-sectional study was done from 29th March to 8th April 2004, simultaneously in the five districts. It consisted of collecting data on the key practices of administration of appropriate health care at home to children less than five years. This was done with the use of questionnaires given to household heads and caretakers of children less than five years.
The data was analysed with the Epi info version 6.0 and Statistical Package for the Social Sciences (SPSS) version 11 softwares. Comparison of variables was done with the Chi-square (-2) test with the significance threshold of 5%.
CONCEPT-DEFINITION
Traditional force-feeding ("forced" feeding) is a procedure which consists of introducing forcefully food into the child's mouth, with the child laid on the extended hips of his/her seated mother, and with the child's head slightly more inclined backwards than the rest of the body. | | | | Results | Socio-demographic features
Out of 983 household heads surveyed, 64.3% were from the rural areas and 35.7% urban. About half had never attended school and about three quarters were men, with farming as their main profession (Table I). A household comprised averagely seven people ; 68.1% households disposed faeces in the bush exposing to faeces-borne diseases, which was aggravated by the anarchic disposal of household wastes and used waters. Nine out of ten caretakers were women, even progenitors, and more than half had never gone to school (Table II). The radio was the main source of getting information on health issues in 74 out of 251 urban households and 141 out of 632 rural ones; the gong the second source in respectively 46 out of 251 and 101 out of 632. Person-to-person communication, often associated with other traditional or modern media, had a key role in information circulation. Out of 733 under-five surveyed (Table III), 151 had been sick within the last two weeks preceding the survey. 50.6% of the sick children were 1-3 year old group and 20.2% less than one year.
Table I : Distribution (%) household heads according to sex, age, level of education, marital status and profession.
Indicators |
Districts |
Residence |
Total |
Blitta |
East-
Mono |
Sotou-
Boua |
Tcham-
ba |
Tchaou-
djo |
urban |
rural |
% |
n |
Sex |
Males |
71.1 |
76.3 |
71.4 |
80.0 |
70.8 |
68.7 |
75.5 |
73.0 |
718 |
Females |
28.9 |
23.7 |
28.6 |
20.0 |
29.2 |
31.3 |
24.5 |
27.0 |
265 |
| |
X 2 = 5.626 ; ddl = 4 ; p = 0.229. |
X 2 = 5.321 ; p=0.021 |
|
Age (years) |
15 - 19 |
- |
- |
1.2 |
0.7 |
1.8 |
0.6 |
1.1 |
0.9 |
9 |
20 - 24 |
3.2 |
1.5 |
4.1 |
2.1 |
5.1 |
4.8 |
2.8 |
3.6 |
35 |
25 - 29 |
4.7 |
7.4 |
6.2 |
3.6 |
8.3 |
6.0 |
6.5 |
6.3 |
62 |
30 - 34 |
15.3 |
8.1 |
12.9 |
6.4 |
10.8 |
14.0 |
9.7 |
11.2 |
110 |
35 - 39 |
15.8 |
5.9 |
11.2 |
6.4 |
12.3 |
12.3 |
10.3 |
11.0 |
108 |
40 - 44 |
11.6 |
15.6 |
12.4 |
11.4 |
14.1 |
11.7 |
13.8 |
13.0 |
128 |
45 - 49 |
11.1 |
17.8 |
15.8 |
10.0 |
9.0 |
13.4 |
11.9 |
12.4 |
122 |
50 - 54 |
8.4 |
15.6 |
9.5 |
12.1 |
8.7 |
10.3 |
10.3 |
10.3 |
101 |
55 - 59 |
10.0 |
5.2 |
5.0 |
10.7 |
6.9 |
7.4 |
7.3 |
7.3 |
72 |
= 60 |
16.8 |
18.5 |
20.3 |
25.0 |
13.7 |
17.1 |
18.8 |
18.2 |
179 |
unknown |
3.2 |
4.4 |
1.2 |
11.4 |
9.4 |
2.6 |
7.6 |
5.8 |
57 |
| |
X 2 = 87.525 ; p=0.000. |
X 2 = 19.267 ; p=0.037 |
|
Level of education |
None |
40.0 |
60.0 |
36.1 |
77.1 |
50.2 |
40.5 |
55.2 |
49.9 |
491 |
Primary |
37.9 |
27.4 |
36.1 |
15.7 |
23.1 |
27.6 |
29.3 |
28.7 |
282 |
Secondary |
21.6 |
11.1 |
26.6 |
7.1 |
23.5 |
28.5 |
15.0 |
19.8 |
195 |
Higher |
0.5 |
1.5 |
1.2 |
- |
3.2 |
3.4 |
0.5 |
1.5 |
15 |
| |
X 2 = 91.070 ; p = 0.000 |
X 2 = 43.485 ; p=0.000 |
|
Matrimonial status |
Unmarried |
6.8 |
1.5 |
2.5 |
1.4 |
5.8 |
5.7 |
3.0 |
4.0 |
39 |
Married
monogamous |
50.0 |
46.7 |
58.5 |
47.9 |
56.0 |
54.4 |
52.2 |
53.0 |
521 |
Married
polygamous |
26.3 |
32.6 |
29.5 |
41.4 |
25.6 |
25.9 |
32.1 |
29.9 |
294 |
Divorced/Staying apart |
6.3 |
5.9 |
5.0 |
1.4 |
2.9 |
3.7 |
4.6 |
4.3 |
42 |
widow |
10.5 |
13.3 |
4.6 |
7.9 |
9.7 |
10.3 |
8.1 |
8.9 |
87 |
| |
X 2 = 40.865 ; p = 0.001 |
X 2 = 8.855 ; p=0.065 |
|
Profession |
None |
4.2 |
5.2 |
9.5 |
10.0 |
6.9 |
8.0 |
6.8 |
7.2 |
71 |
Farming |
62.1 |
79.3 |
47.3 |
74.3 |
41.2 |
39.6 |
66.1 |
56.7 |
557 |
Trading |
10 |
7.4 |
20.3 |
6.4 |
16.6 |
15.9 |
12.2 |
13.5 |
133 |
Craftwork |
6.3 |
0.7 |
5.8 |
4.3 |
5.4 |
9.1 |
2.5 |
4.9 |
48 |
Private administration |
5.2 |
2.9 |
9.2 |
2.8 |
11.2 |
10.0 |
6.1 |
11.3 |
74 |
Public administration |
5.8 |
3.7 |
4.6 |
2.1 |
5.4 |
7.4 |
3.0 |
4.6 |
45 |
others |
6.3 |
0.7 |
3.3 |
0.1 |
12.3 |
10.0 |
3.2 |
5.6 |
55 |
| |
X 2 = 162.648 ; ddl = 32 ; p = 0.000 |
X 2 = 84. 302 ; p=0.000 |
|
|
Total (%)
(n) |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
- |
190 |
135 |
241 |
140 |
277 |
351 |
632 |
- |
983 |
Table II : Distribution(%) of caretakers according to sex, age, level of education, parental relationship, matrimonial status and profession
Indicators |
Districts |
Residence |
Total |
Blitta |
East-
Mono |
Sotou-
Boua |
Tcham-
ba |
Tchaou-
djo |
urban |
rural |
% |
n |
Sex |
Males |
10.3 |
16.7 |
3.4 |
0.0 |
6.4 |
7.9 |
6.0 |
6.5 |
33 |
Females |
89.7 |
83.3 |
96.6 |
100.0 |
93.6 |
92.1 |
94.0 |
93.5 |
473 |
| |
|
X 2 =0.566 ; p=0.452 |
|
Age (years) |
Less than 15 |
0.0 |
0.0 |
0.0 |
1.6 |
0.0 |
0.0 |
0.3 |
0.2 |
1 |
15 - 19 |
6.4 |
0.0 |
6.8 |
1.6 |
9.6 |
3.6 |
7.1 |
6.1 |
31 |
20 - 24 |
30.8 |
16.7 |
28.4 |
4.7 |
15.4 |
22.1 |
19.7 |
20.4 |
103 |
25 - 29 |
28.2 |
13.3 |
20.3 |
15.6 |
34.6 |
20.0 |
26.2 |
24.5 |
124 |
30 - 34 |
10.3 |
25.0 |
21.6 |
31.3 |
16.7 |
23.6 |
18.6 |
20.0 |
101 |
35 - 39 |
17.9 |
20.0 |
14.2 |
26.6 |
14.1 |
17.1 |
16.9 |
17.0 |
86 |
40 - 44 |
5.1 |
8.3 |
4.7 |
10.9 |
6.4 |
5.7 |
6.8 |
6.5 |
33 |
45 - 49 |
1.3 |
1.7 |
1.4 |
3.1 |
1.3 |
0.7 |
1.9 |
1.6 |
8 |
50 ans et plus |
0.0 |
15.0 |
2.7 |
4.7 |
1.9 |
7.1 |
2.5 |
3.8 |
19 |
|
|
X 2 =12.649 ; p=0.125 |
|
School attendance |
Yes |
69.2 |
26.7 |
62.2 |
15.6 |
40.4 |
44.3 |
47.3 |
46.4 |
235 |
No |
30.8 |
73.3 |
37.8 |
84.4 |
59.6 |
55.7 |
52.7 |
53.6 |
271 |
| |
X 2 =67.160 ; p = 0.000 |
X 2 =0.362 ; p=0.547 |
|
Level of education |
None |
30.8 |
73.3 |
37.8 |
84.4 |
59.6 |
55.7 |
52.7 |
53.6 |
271 |
Primary |
48.7 |
21.7 |
41.2 |
10.9 |
25.6 |
22.9 |
34.7 |
31.4 |
159 |
Secondary |
20.5 |
5.0 |
21.0 |
4.7 |
14.1 |
21.4 |
12.3 |
14.8 |
75 |
Higher |
0.0 |
0.0 |
0.0 |
0.0 |
0.7 |
0.0 |
0.3 |
0.2 |
1 |
|
X 2 =71.244 ; p = 0.000. |
X 2 =10.769; p = 0.013 |
|
Parental relationship with the child |
None |
0.0 |
0.0 |
0.7 |
0.0 |
0.0 |
0.0 |
0.3 |
0.2 |
1 |
Household |
1.3 |
0.0 |
1.4 |
3.1 |
1.9 |
0.7 |
1.9 |
1.6 |
8 |
Father/mother |
97.4 |
81.7 |
91.2 |
90.6 |
92.3 |
90.0 |
91.8 |
91.3 |
462 |
Grands-parents |
1.3 |
15.0 |
4.7 |
6.3 |
4.5 |
7.9 |
4.6 |
5.5 |
28 |
Other parents |
0.0 |
3.3 |
2.0 |
0.0 |
1.3 |
1.4 |
1.4 |
1.4 |
7 |
|
X 2 =22.367 ; p = 0.132. |
X 2 =3.230 ; p = 0.520
|
|
Total (%)
(n) |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
- |
78 |
60 |
148 |
64 |
156 |
140 |
366 |
- |
506 |
Table III : Distribution (%) of children according to sex, age, parental relationship with the household heads, level of education, and parent alive or not.
Indicators |
Districts |
Residence |
Total |
Blitta |
East-
Mono |
Sotou-
boua |
Tcham-
ba |
Tchaou-
djo |
urban |
rural |
% |
n |
Sex |
Males |
53.2 |
49.5 |
54.4 |
50.0 |
51.5 |
51.6 |
52.1 |
52.0 |
381 |
Females |
46.8 |
50.5 |
45.6 |
50.0 |
48.5 |
48.4 |
47.9 |
48.0 |
352 |
| |
X 2 = 0.903 ; p = 0.924 |
X 2 = 0.015 ; p=0.903 |
|
Age (months) |
Less than 12 |
26.6 |
34.7 |
21.1 |
22.2 |
29.9 |
23.9 |
28.1 |
27.0 |
198 |
12 - 23 |
22.3 |
17.9 |
23.9 |
15.6 |
23.0 |
20.2 |
22.0 |
21.6 |
158 |
24 - 35 |
23.4 |
18.9 |
18.9 |
20.0 |
19.7 |
21.8 |
19.3 |
19.9 |
146 |
36 - 59 |
27.7 |
28.4 |
36.1 |
42.2 |
27.4 |
34.0 |
30.6 |
31.5 |
231 |
| |
X 2 = 16.314 ; p = 0.177. |
X 2 =2.064 ; p= 0.559. |
|
Parental relationship with household head |
Father |
43.6 |
61.1 |
56.7 |
65.6 |
59.5 |
57.4 |
57.8 |
57.7 |
423 |
Mother |
14.9 |
14.7 |
16.7 |
22.2 |
29.2 |
17.6 |
22.9 |
21.6 |
158 |
Sister/ Brother |
10.6 |
2.1 |
- |
- |
0.4 |
1.6 |
1.8 |
1.8 |
13 |
Grands-parents |
26.6 |
21.1 |
21.7 |
10.0 |
9.1 |
20.2 |
14.7 |
16.1 |
118 |
Uncle/ Uncle |
2.1 |
1.1 |
3.3 |
1.1 |
1.5 |
2.1 |
1.8 |
1.9 |
14 |
Other parents |
- |
- |
1.7 |
1.1 |
0.4 |
1.1 |
0.6 |
0.7 |
5 |
others |
2.1 |
- |
- |
- |
- |
- |
0.4 |
0.3 |
2 |
| |
X 2 = 110.236 ; p = 0.000 |
X 2 =5.879 ;p=0.437 |
|
|
School attendance |
Yes |
1.1 |
- |
4.4 |
3.3 |
2.9 |
4.8 |
2.0 |
2.7 |
20 |
No |
1.1 |
1.1 |
1.1 |
2.2 |
1.1 |
1.1 |
1.3 |
1.2 |
9 |
Not at school age |
97.9 |
98.9 |
94.4 |
94.4 |
96.0 |
94.1 |
96.7 |
96.0 |
704 |
| |
X 2 = 6.663 ; p = 0.573 |
X 2 =4.078 ; p=0.130 |
|
Parents alive or not |
Both alive |
96.8 |
95.8 |
97.8 |
96.7 |
96.7 |
93.1 |
98.2 |
96.9 |
710 |
Father alive |
1.1 |
1.1 |
1.1 |
1.1 |
1.1 |
3.2 |
0.4 |
1.1 |
8 |
Mother alive |
2.1 |
3.2 |
0.6 |
2.2 |
2.2 |
3.2 |
1.5 |
1.9 |
14 |
Both dead |
- |
- |
0.6 |
- |
- |
0.5 |
- |
0.1 |
1 |
| |
X 2 = 5.788 ; p = 0.926 |
X 2 =15.663 ; p=0.001
|
|
Total (%)
(n) |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
100.0 |
- |
94 |
95 |
180 |
90 |
274 |
188 |
545 |
- |
733 |
Home management of diseases
The sick children had suffered from fever (47%), diarrhoea (19.9%), cough and/or respiratory difficulties (5.3%), ear pain (2%) and other problems (25.8%). They were mainly managed through self-treatment and health facility attendant (Fig. 1). Out of 41 children with diarrhoea, 18 took ORS/WHO/UNICEF and 15 received antibiotics bought from the market not in the village pharmacy. Within the day following onset of the illness, 55.6% of caretakers took their child to a health facility (Fig. 2). If 39.7% of caretakers gave sick children more fluids than usual, 63.8% fed them less frequently than usual during an illness (Fig. 3), while 41.3% of caretakers fed with appropriate foods which the child preferred, in order to incite appetite (Table IV).
The 51 cases of accidents and wounds, comprising mainly falls (48.1%) and knives cuts (15.8%), were managed at home (47.1%), in a health facility (33.3%) or by a traditional healer (19.6%). Concerning their prevention, the most cited approach, was close monitoring (Table V).
Figure 1 : Distribution (%) of sick children according to measures taken by caretakers (n = 151)
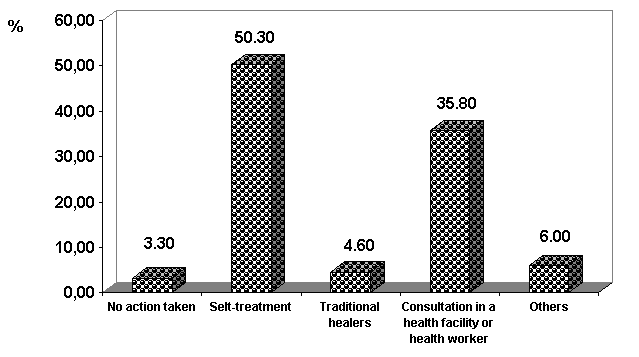
Figure 2 : Distribution (%) of sick children according to the time elapsed before being conducted to a health facility after onset of illness (n = 54)

Figure 3 : Distribution (%) of caretakers according to their declarations on manner of feeding the sick children and manner of offering them fluids (n= 506)
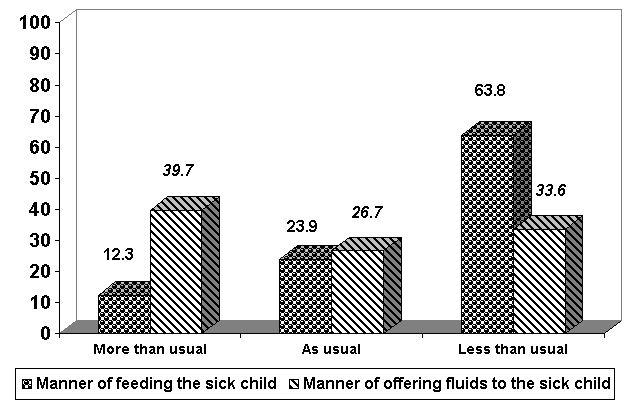
Table IV : Distribution (%) of way of encouraging feeding according to district, residence, sex and age of the sick children, age and level education of caretakers
Indicators |
Way of encouraging feeding |
Total |
Traditional force-feeding
|
Giving appropriate and
preferred foods |
Others |
% |
n |
District |
Blitta |
39.7 |
30.8 |
29.5 |
100.0 |
78 |
East-Mono |
56.7 |
40.0 |
03.3 |
100.0 |
60 |
Sotouboua |
59.5 |
37.8 |
02.7 |
100.0 |
148 |
Tchamba |
42.2 |
37.5 |
20.3 |
100.0 |
64 |
Tchaoudjo |
37.8 |
51.9 |
10.3 |
100.0 |
156 |
X 2 = 57.092 ; p = 0.000 |
Residence |
Urban |
41.4 |
45.0 |
13.6 |
100.0 |
140 |
Rural |
49.5 |
39.9 |
10.7 |
100.0 |
366 |
X 2 = 2.772 ; p = 0.250 |
Sex of child |
Males |
44.6 |
42.3 |
13.1 |
100.0 |
267 |
Females |
50.2 |
40.2 |
09.6 |
100.0 |
239 |
X 2 = 2,327 ; p = 0,312 |
Age (months) of the child |
0 - 3 |
39.6 |
37.7 |
22.6 |
100.0 |
53 |
4 - 6 |
56.8 |
32.4 |
10.8 |
100.0 |
37 |
7 - 9 |
56.0 |
32.0 |
12.0 |
100.0 |
25 |
10 - 11 |
57.9 |
31.6 |
10.5 |
100.0 |
19 |
12 - 17 |
48.4 |
37.5 |
14.1 |
100.0 |
64 |
18 - 23 |
50.0 |
36.4 |
13.6 |
100.0 |
44 |
24 - 29 |
57.6 |
37.9 |
04.5 |
100.0 |
66 |
30 - 35 |
50.0 |
33.3 |
16.7 |
100.0 |
36 |
36 - 59 |
38.9 |
53.1 |
08.0 |
100.0 |
162 |
X 2 = 26.402 ; p = 0.049 |
Age (years) of caretakers |
< 15 |
00.0 |
00.0 |
100.0 |
100.0 |
1 |
15 - 19 |
48.4 |
32.3 |
19.4 |
100.0 |
31 |
20 - 24 |
56.3 |
26.2 |
17.5 |
100.0 |
103 |
25 - 29 |
40.3 |
50.8 |
08.9 |
100.0 |
124 |
30 - 34 |
49.5 |
42.6 |
07.9 |
100.0 |
101 |
35 - 39 |
46.5 |
44.2 |
09.3 |
100.0 |
86 |
40 - 44 |
48.5 |
45.5 |
06.1 |
100.0 |
33 |
45 - 49 |
62.5 |
37.5 |
00.0 |
100.0 |
8 |
= 50 |
26.3 |
52.6 |
21.1 |
100.0 |
19 |
X 2 = 33.438 ; p = 0.006 |
Level of education |
None |
49.8 |
41.3 |
08.9 |
100.0 |
271 |
Primary |
45.9 |
42.8 |
11.3 |
100.0 |
159 |
Secondary |
40.0 |
38.7 |
21.3 |
100.0 |
75 |
Higher |
100.0 |
00.0 |
00.0 |
100.0 |
1 |
X 2 = 10.582 ; p = 0.102 |
Total (%) (n) |
47.2 |
41.3 |
11.5 |
100.0 |
- |
239 |
209 |
58 |
- |
506 |
Table V : Distribution (%) of measures taken by caretakers to prevent accidents in children according to district, residence, age and level education of caretakers
Indicators |
Measures taken to prevent accidents in children |
Total |
Monitoring children closely |
Preventing children from going out |
Keeping dangerous objects out of the reach of children |
Warning children |
Others |
% |
n |
Districts |
Blitta |
89.7 |
01.3 |
01.3 |
02.6 |
05.1 |
100.0 |
78 |
East-Mono |
91.7 |
00.0 |
03.3 |
01.7 |
03.3 |
100.0 |
60 |
Sotouboua |
69.6 |
14.9 |
01.4 |
02.7 |
11.5 |
100.0 |
148 |
Tchamba |
75.0 |
18.8 |
04.7 |
00.0 |
01.6 |
100.0 |
64 |
Tchaoudjo |
86.5 |
00.0 |
01.9 |
06.4 |
05.1 |
100.0 |
156 |
X 2 = 70.059 ; p = 0.000 |
Residence |
Urban |
85.0 |
09.3 |
02.1 |
00.7 |
02.9 |
100.0 |
140 |
rural |
79.8 |
06.0 |
02.2 |
04.4 |
07.7 |
100.0 |
366 |
X 2 = 9.621 ; p = 0.047 |
Age (years) |
= 15 |
100.0 |
00.0 |
00.0 |
00.0 |
00.0 |
100.0 |
1 |
15 - 19 |
74.2 |
06.5 |
03.2 |
03.2 |
12.9 |
100.0 |
31 |
20 - 24 |
81.6 |
05.8 |
00.0 |
02.9 |
09.7 |
100.0 |
103 |
25 - 29 |
81.5 |
07.3 |
02.4 |
04.8 |
04.0 |
100.0 |
124 |
30 - 34 |
82.2 |
06.9 |
04.0 |
03.0 |
04.0 |
100.0 |
101 |
35 - 39 |
77.9 |
10.5 |
03.5 |
03.5 |
04.7 |
100.0 |
86 |
40 - 44 |
93.9 |
00.0 |
00.0 |
00.0 |
06.1 |
100.0 |
33 |
45 - 49 |
100.0 |
00.0 |
00.0 |
00.0 |
00.0 |
100.0 |
8 |
= 50 |
68.4 |
10.5 |
00.0 |
05.3 |
15.8 |
100.0 |
19 |
X 2 =24.800 ; p = 0.814
|
Level of education |
None |
80.4 |
07.7 |
03.3 |
03.7 |
04.8 |
100.0 |
271 |
Primary |
81.8 |
06.9 |
01.3 |
03.1 |
06.9 |
100.0 |
159 |
Secondary |
82.7 |
04.0 |
00.0 |
02.7 |
10.6 |
100.0 |
75 |
Higher |
100.0 |
00.0 |
00.0 |
00.0 |
00.0 |
100.0 |
1 |
X 2 =11.580 ; p = 0.772
|
Total (%) (n) |
81.2 |
06.9 |
02.2 |
03.4 |
06.3 |
100.0 |
- |
411 |
35 |
11 |
17 |
32 |
- |
506 |
| | | | Discussion | Our data proved to be of good quality and reliable for analysis because of questionnaires elaborated upon local cultural factors, the high sample cover rate (98.3%), the survey training of the technical team , the proportion of under-five children estimated to be 12% in our study (against 13.7% for the whole country in 2000 [11]), while the average size of the households surveyed was 7 against 8 for the whole country in 1998 [12]. However, the cross-sectional studies are limited in time, and data might be difficult to interpret [13].
Household heads
Our results are similar to those of the Togo's Demographic and Health Survey [12] and MICS 2 [4], in which 76% of households were headed by men and more than half of the people above 15 years illiterate. The main economic activity of the surveyed people was farming (56.7%) as noted in Togo's Health and Nutrition Survey in rural areas (57.9%) [14].The low literacy rate coupled with low revenues might strongly influence individual behaviours towards hygiene and family health. Under-five children catered for by these illiterate people will thus be exposed to avoidable diseases. These factors could block behavioural change and practices on health, as they do not facilitate openness to innovations in practices in these social groups.
Caretakers
In our series, the predominance of women coupled with the fact that 9 out of 10 caretakers were progenitors, illustrates their awareness of healthcare, feeding and dressing for children. Contrarily, the high illiteracy rate in our population is a factor that does not favour hygiene, nutrition and family health.
Children
Only 2.7% of children attended school, against 4.6% in Burundi [15] and 9% in Togo in 2000 [11]. This low rate compared with the national rate could be explained by the scarcity of kindergartens in the PLAN covered areas, and the educational level of caretakers who might be ignorant of the importance of schooling of such children.
Health information means
The importance of the gong in the circulation and diffusion of health messages in towns, is understandable as most urban areas surveyed, still have many characteristics of rural life. In Kenya, Hamel MJ et al [16] found in 2002 that health workers (doctors, nurses, midwives and traditional birth attendants) were the main source of information in 94.1% households. Although less cited in our study, they remain the principal means of communicating health issues.
Treating the sick child
In the C-IMCI strategy, mothers are taught that appropriate home treatment of diarrhoea or any other illnesses requires that the sick child, firstly, be given more fluids and be fed more than usual [7-9]. About two out of three interviewed people, fed their sick children less than usually. These data are similar to those of MICS 2000 in Togo [11] which showed that 61% of sick children were fed less than usually. We noted that caretakers, whatever their ages, could have difficulties in sufficiently feeding the sick child. When children are sick, African mothers generally prepare special dishes and encourage them to actively feed without risky force-feeding. Since the 80's, studies showed that it was important to continue to feed the child with diarrhoea, to reduce not only its consequent nutritional disorders but also its duration [17]. It is also important to give more fluids to the sick child as to feed. In our series, 60.3% of sick children took fluids as usually or even less 64% in 2000 in Togo [11]. Thus, the need to reinforce education of the masses.
Attitude towards illness, is dominated by self-treatment at home, as largely observed : 47% of sick children in Kenya [16], 62 to 75% in Burkina Faso [18], 50.3% in our series. Self-treatment is the first action taken by parents towards a sick child, followed by attending a health facility. This high frequency of self-treatment might be explained by poverty of the people who do not always consult in the health facility because of lack of money, thus the need to promote and diffuse essential generic drugs in remote areas. According to many authors, fever/malaria remain the most frequent causes of morbidity, justifying the systematic administration of antimalarials in case of fever, followed by antipyretics and antibiotics and even drips at doses not in conformity with medical prescriptions [20-25]. Such a situation should incite governments and health personnel to organize campaigns to sensitize mothers or caretakers on the rational use of these drugs at home. Such drugs should be bought at the appropriate place (village pharmacy / drugstore) not from the roadside. Only a strong partnership between the health personnel and caregiver based on practical advice on diagnosis and treatment of some common diseases could considerably reduce infant mortality [20]. The fact is that drugs cure but, if misused, they could kill.
Elapsed time before taking a child to a health facility.
In our study, two out of three mothers reacted positively and rapidly when the child fell sick (that is, the following day after onset of illness). One third waited for more than one week before consulting. This situation should incite health personnel to increase communication activities for behavioural change in family health. Hamel M J et al [16] noted in their series that 51% of children taken for consultation arrived within two days of onset of illness while 34% received treatment at home and / or were taken to a health facility only within 24 hours, and only in the case of fever. The frequency of seeking consultation in a health facility in case of fever in a child, is estimated at 43% in Kenya [16] and 76% in Swaziland [26] whereas the frequency of home treatment was between 1% in Swaziland, and 83% in Togo [23].
Accidents and wounds in children
Accidents, whose amplitude is largely unknown [27], are the responsibility of the caregiver. Neglect and lack of vigilance are the main causes of these accidents suffered by under-five children. These children need to be well followed-up and parents should take all precautions to this effect. Actions taken in case of accidents show the importance attached to the home management of these children in our survey. Treating these accidents at home, should be completed at health facility level, for welfare of these children. Overall, close monitoring, more vigilance and availability of the parents, are key-measures taken to ensure the safety of these under-five children who are not yet aware of dangers [27]. | | | | Conclusion | The characteristics of the three studied key family and community practices need to be deepened about why people did not buy medicines in the village pharmacy and prefer those bought by the roadside. Besides, more studies have to be done on the prevention and negligence of children as well as on man involvement in the reproductive health. Until this is done, it is necessary to help the community effectively appropriate C-IMCI by:
-buying medicines in the village pharmacy not from the roadside,
-applying simple rules and recommendations from health personnel on IMCI in general, and
-mastering guidelines taught by that personnel for the management of health problems at home.
| | | | Acknowledgement | This study was supported by a grant from the Togolese office of the Non Governmental Organization PLAN (Plan Togo), and we are grateful for that. Our gratitude also goes to all the field investigators and the people interviewed, for their availability.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Talani P. Le guide de la medecine et de la sante au Congo. En avant pour la mise en "uvre de la strategie de prise en charge integree des maladies de l"enfant- Brazzaville : Ministere de la Sante, 2001 : 47.
- Lul Seged S. Integrated Management of childhood illness: a review of the Ethiopian experience and Prospects for child health. Ethiop Med J 2002; 40 (2): 187.
- Orne-Gliemann J, Perez F, Leroy V, Newell M-L, Dabis F. Une decennie de recherche sur la sante de l-enfant dans les pays en developpement. Cahiers Sante 2003,13 (2) : 69-75. [PubMed]
- Organisation Mondiale de la Sante, UNICEF. Rôle de la PCIME dans l-amelioration des pratiques familiales et communautaires en faveur de la sante et du developpement de l-enfant. PCIME Information 1999: 5.
- Organisation Mondiale de la sante, UNICEF. La prise en charge des maladies de l-enfant dans les pays en developpement : Justification d-une strategie integree. PCIME Information 1999 : 6.
- Organisation Mondiale de la Sante. Prise en charge integree des maladies de l-enfant (PCIME). Plan strategique pour 2000 - 2005. Harare : Regional Office for Africa, 2001:10.
- Murray J, Adeyi GN, Graeff J et al. Comportements-cles en sante maternelle et infantile: Importance des comportements des gardiens d-enfants pour l-elaboration de programmes communautaires de sante maternelle et infantile; Arlington : BASICS/USAID, 1997 : 14.
- Organisation Mondiale de la Sante. Vers de meilleures pratiques familiales et communautaires. Une composante de la strategie PCIME. Geneve : OMS, 1998:8.
- Hill Z, Kirkwood B, Edmond K. Family and community practices that promote child survival, growth and development : a review of the evidence. London : London School of Hygiene and Tropical Medecine, 2001: 106. [PubMed]
- Republique du Togo. Plan national de developpement sanitaire du Togo (2002 - 2006). Lome : Ministere de la Sante publique, 2002 : 64.
- UNICEF, Republique du Togo. Rapport de l-enquete sur les objectifs du sommet mondial pour les enfants (MICS II 2000). Lome : UNICEF, 2001 : 100.
- Kodjo A, Mboup G, Ouro-Gnao AM, Boukpessi B, Messan PA, Salami-Odjo R. Enquete demographique et de sante, Togo 1998. Calverton (Maryland, USA): Direction de la Statistique et Macro International Inc. 1999 : 287.
- Vaughan J, Morrow R - Enquete epidemiologique, Manuel d'epidemiologie pour la gestion de la sante au niveau du district, Geneve : OMS 1991,186 p.
- UNICEF, FAO, CRAN/OCCG, Republique Togolaise - Enquete nationale sur la nutrition et la sante au Togo en milieu rural. Ministere de l-Agriculture, de l-Elevage et de la Peche; Ministere de la Planification et du Developpement. Lome : Ministere de la Sante/UNICEF; 2000 : 188.
- UNICEF, Republique du Burundi - Rapport de l-enquete sur les objectifs du sommet mondial pour les enfants (MICS2 2000). Bujumbura : UNICEF; 2000 : 39.
- Hamel M J, Odhacha A, Roberts J M, Deming M S. Lutte antipaludique dans la district de Bungoma (Kenya) : enquete sur le traitement a domicile des enfants fievreux, l-utilisation des moustiquaires et les visites aux dispensaires de soins prenatals. Bull OMS 2002;6: 10.
- Victora CG, Bryce J, Fontaine O, Monasch R. Maladies diarrheiques : reduire la mortalite grace a la therapie par rehydratation orale. Bull OMS 2001; 4 : 122-31.
- Bob P. Prevention du paludisme a Ouagadougou. Focus (Ouaga) 2002;23 :2.
- Tarimo DS, Lwihula GK, Minjas JN, Bybjerg IC. Mothers- perceptions and knowledge on childhood malaria in the holendemic Kibaha district, Tanzania. Trop Med Int Health 2000;5: 179 - 84. [CrossRef]
- Kidane G, Morrow RH. Teaching mothers to provide home treatment of malaria in Tigray, Ethiopia : a randomised trial. Lancet 2000; 356: 550-5. [CrossRef]
- Lubanga RG, Norman S, Ewbank D, Karamagi C. Maternal diagnosis and treatment of children-s fever in an endemic malaria zone of Uganda: implications for the malaria control programme. Acta Trop 1997; 68 : 53 - 64. [CrossRef]
- Fawole OI, Onadeko MO. Knowledge and home management of malaria fever by mothers and caretakers of under five children. West Afr J Med 2001;20 : 152 - 7. [PubMed]
- Deming MS, Gayibor A, Murphy K, Jones TS, Karsa T - Home treatment of febrile children with antimalarial drugs in Togo. Bull World Health Organ 1989, 67(6): 695-700. [PMC free article]
- Dabis F, Breman JG, Roisin AJ, Haba F. Monitoring selective components of primary health care : methodology and community assessment of vaccination, diarrhoea malaria practices in Conakry (Guinea). ACSI-CCCD Team. Bull World Health Organ 1989; 67 : 675-84. [PMC free article]
- Slutsker L, Chitsulo L, Macheso A, Steketee RW. Treatment of malaria fever episodes among children in Malawi : results of a KAP survey. Trop Med and Parasitol 1994; 45 : 61-4. [PubMed]
- United States Agency for international development, Africa - Controlling malaria in Africa : progress and priorities. Atlanta, Georgia, Centers for disease control and prevention, Washington, D.C, : US Department of health and human services, 1994 (Regional project 698-0421).
- Deen JL, Vos T, Huttly SR, Tulloch J. Medical research council laboratories, Farafenini Field, the Gambia. Injuries and noncommunicable diseases: emerging health problems of children in developing countries. Bull World Health Organ. 1999; 77 : 518 - 24. [PMC free article]
|
| Cite this article as: | | D A A, S K, A C, K K E, D A. Household Community Management of the Sick Child in the Northern Part of Togo Before Implementation of the Community Component of the Integrated Management of Childhood Illness Strategy. Pediatr Oncall J. 2008;5: 145. |
|