Rajesh Kulkarni, Sagar Vartak, Naresh Sonkawade, Aarti Kinikar.
Department of Paediatrics, B.J. Government Medical College, Pune, Maharashtra, India.
ADDRESS FOR CORRESPONDENCE
Dr Rajesh Kulkarni, C1004, Triose Apartment, Pimple Saudagar, Pune 411027, India.
Email: docrajesh75@yahoo.com | | Abstract | | Electrical injuries frequently affect the cardiovascular system. Most of the patients have immediate devastating effects. Permanent myocardial injury or chronic cardiac disease following an electrocution is rare. We report a 10-year-old female with a history of electrocution who presented to us with dilated cardiomyopathy with severe left ventricular dysfunction. | | | | Keywords | | Electrocution, shock, dilated cardiomyopathy. | | | | Introduction | | Fatal electrical injuries or electrocutions are rare. Most of the injuries are accidental in nature, and happen when child handles any electrical equipment without proper precautions. Males are more affected than females.1 Deaths due to electrical injury are rare and occur in the setting of high voltage electrocutions. Following electrical injuries ventricular tachycardia, recurrent ventricular premature complexes, atrial fibrillation, supraventricular tachycardia and ST-T changes in the electrocardiogram (ECG) can occur.2 Electrical injury can produce myocardial damage, with ECG simulating myocardial infarction and high creatinine phosphokinase-MB (CK- MB) levels, which resolve in a few days.3 Myocardial damage can be secondary to direct thermal injury or ischemic injury due to arrythmias.4 Significant cardiac damage or dysfunction are rare in children and young adults in the setting of accidental electrical injuries at home.4 Most of the cardiac complications are seen in the acute phase. Delayed complications are rare.5 Here we report a rare delayed cardiac complication of an accidental electrical injury in a 10-year-old female. | | | | Case Report | A 10-year-old female presented to the pediatric casualty with complaints of progressively increasing breathlessness and vomiting for 15 days. There was no history of fever, cough, asthma, tuberculosis or heart disease. Child suffered from an accidental electrocution with 230 V for a few minutes 30 days ago. Following the episode, child was unconscious for a 20-30 minutes. She was taken to a nearby district hospital, where she was treated and discharged after 2 days. On presentation to us, she was afebrile, conscious and oriented. There were electrical burn marks on right hand and foot. She had a pulse rate of 150/min and respiratory rate of 40/min. She was hypotensive with a blood pressure of 80/40 mm Hg which was less than 5th centile for her age. Peripheral pulses were poor with cold peripheries and delayed capillary refill time. Pulse oximetry showed oxygen saturation of 84% at room air and arterial blood gas showed type 2 respiratory failure (pH 7.21, PaCO2 58 mm Hg, PaO2 60 mm Hg), She was intubated and started on mechanical ventilation. Serum potassium was 2.7 meq/l, and she was given potassium correction. Other investigations revealed hemoglobin 12.1 gm/dl, white cell count 6700 cells/cumm, platelets 350,000 cells/cumm, BUN 12 mg/dl, serum creatinine 0.9 mg/dl, ALT 36 IU/L, AST 32 IU/L, serum albumin 3.8 gm/dl and INR 1.1. ECG revealed sinus tachycardia with ST-T changes (figure 1). CPK-MB levels were normal (30 IU/L). Pro-BNP levels were elevated [1400 pg/ml (normal upto 100 pg/ml)] . Thyroid functions were normal (T3 79 ng/dl, T4 7.8 microgram/dl and TSH 2.45 microIU/ml). Blood and urine cultures were negative. Toxicology screen, anti-nuclear antibody, throat swab for streptococcal antigen and IgG for adenovirus, coxackie B virus, HIV Elisa, scrub typhus Elisa were negative. Serum calcium level and serum Vitamin D level were normal. 2D echocardiography (2D Echo) showed dilated left ventricle, severe left ventricular dysfunction with an ejection fraction of 30%, mild to moderate mitral regurgitation and mild tricuspid regurgitation. Chest radiograph showed cardiomegaly (cardiothoracic ratio of 0.7) (Figure 2). She was treated with intravenous fluids, milrinone infusion (0.75 mcg/kg/min), oral frusemide (2 mg/kg/day), enalapril (0.3 mg/kg/day) and aspirin (5 mg/kg/day) to which she responded in 8 days. She was discharged from hospital 13 days with ejection fraction of 45% on repeat 2D Echo.
Figure 1. ECG shows sinus tachycardia with non-specific ST-T changes.
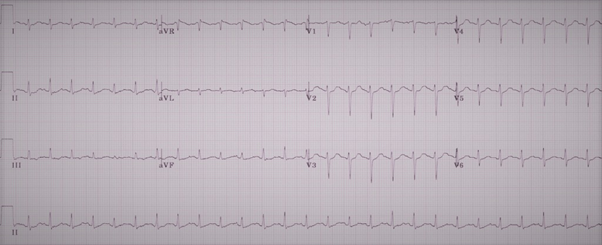
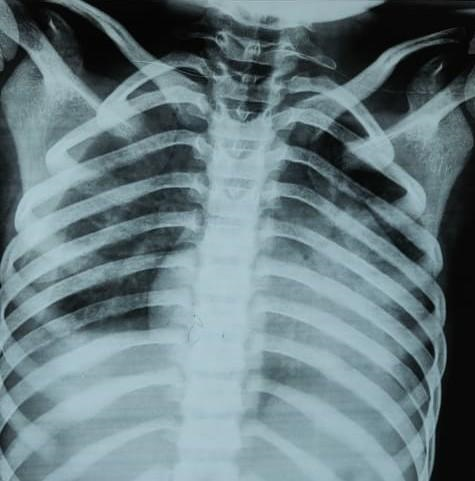
Figure 2. Chest radiograph showing cardiomegaly.
| | | | Discussion | Electrical injuries are common in children younger than 6 years of age.6 Home is the common place of majority of these incidents, mostly due to handling of faulty electrical appliances, wall sockets, extension cords or string light.6, The primary determinant of injury is the amount of current flowing through the body.7 Clinically, contact with a 120 V circuit carrying a 1 milliampere current is imperceptible to most persons, 3 mA leads to mild tingling, and 10 to 12 mA leads to pain. One hundred mA directed across the heart can cause ventricular fibrillation.7 In addition, the voltage, resistance, type of current (AC or DC), the current pathway, and duration of contact can all influence the extent of injury. Indian households have an electrical supply of 220-230 volts alternating at 50 hertz which is enough to cause burn injuries, cardiac arrythmias and myocardial damage.8
Arrhythmias are the most common cardiac manifestation after electrical injury occurring in about 15% of the cases and start within few hours after the event.9 Ventricular arrhythmias are the most fatal acute complications associated with AC electrical injuries while asystole is common in DC electrical injuries.9 Changes in the ST segment and T wave, as well as conduction disturbances, generally resolve without specific treatment. Damage to the myocardium is rare but can occur due to heat injury or myocardial contusion.9 Our patient had an AC electrical injury at home. She did not have any cardiac arrythmias. There was delayed presentation in the form of ventricular dysfunction with dilated cardiomyopathy secondary to the primary event. This was evident on the echocardiogram and supported by the laboratory investigations. Dilated cardiomyopathy has been reported previously with electrical injuries and may manifest clinically like cardiogenic shock or sudden cardiac arrest.8,9 In our patient, the temporal association between electrical injury and cardiomyopathy strongly suggest the electrical injury as the cause. Further, we reasonably ruled out other causes by history and relevant investigations. Our patient made good recovery with aggressive medical management of the cardiac dysfunction.
Treatment includes rapid initial assessment and trauma resuscitation in accordance with the pediatric advanced life support guidelines. Patients require intensive care and continuous monitoring of the vitals. ECG is useful to detect arrhythmias. Troponin-I levels and echocardiography can detect myocardial injury after electric shock.10 Beta- Blockers and angiotensin converting enzyme inhibitors can be beneficial.10
| | | | Conclusion | | Electrical injuries can have delayed cardiac complications. Early diagnosis and timely intervention are essential. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Celik A, Ergün O, Ozok G. Pediatric electrical injuries: a review of 38 consecutive patients. J Pediatr Surg. 2004;39:1233-1237. [CrossRef] [PubMed]
- Pilecky D, Vamos M, Bogyi P, Muk B, Stauder D, Racz H, et al. Risk of cardiac arrhythmias after electrical accident: a single-center study of 480 patients. Clin Res Cardiol. 2019;108:901-908. [CrossRef] [PubMed] [PMC free article]
- Waldmann V, Narayanan K, Combes N, Jost D, Jouven X, Marijon E. Electrical cardiac injuries: current concepts and management. Eur Heart J. 2018;39:1459-1465. [CrossRef] [PubMed]
- Haim A, Zucker N, Levitas A, Sofer S, Katz A, Zalzstein E. Cardiac manifestations following electrocution in children. Cardiol Young. 2008;18:458-460. [CrossRef] [PubMed]
- Zemaitis MR, Foris LA, Lopez RA, Huecker MR. Electrical Injuries. [Updated 2020 Dec 7] In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan- Available from: https://www.ncbi.nlm.nih.gov/books/NBK448087/
- Geddes LA, Baker LE. The specific resistance of biological material--a compendium of data for the biomedical engineer and physiologist. Med Biol Eng. 1967;5:271-293. [CrossRef] [PubMed]
- Kalra GS, Sharma A, Rolekar NG. Changing trends in electrical burn injury due to technology. Indian J Burns 2019;27:70-72. [CrossRef]
- Purdue GF, Hunt JL. Electrocardiographic monitoring after electrical injury: necessity or luxury. J Trauma. 1986;26:166-167. [CrossRef] [PubMed]
- Spies C, Trohman RG. Narrative review: Electrocution and life-threatening electrical injuries. Ann Intern Med. 2006;145:531-537. [CrossRef] [PubMed]
- Celebi A, Gulel O, Cicekcioglu H, Gokaslan S, Kututcularoglu G, Ulusoy V. Myocardial infarction after an electric shock: a rare complication. Cardiol J. 2009;16:362-364.
DOI: https://doi.org/10.7199/ped.oncall.2021.37
|
| Cite this article as: | | Kulkarni R, Vartak S, Sonkawade N, Kinikar A. Delayed Development of Dilated Cardiomyopathy in an Adolescent Following Electrocution. Pediatr Oncall J. 2021;18: 128-130. doi: 10.7199/ped.oncall.2021.37 |
|