Mahesh D Shinde, Anilkumar M Khamkar, Pralhad D Pote, Pradeep B Suryawanshi.
Department of Pediatrics & Neonatology, Noble Hospital & Research Centre, Hadapsar, Pune, 411013, Maharashtra, India.
ADDRESS FOR CORRESPONDENCE
Department of Pediatrics and Neonatology, Noble Hospital and Research Center, Hadapsar, Pune, Maharashtra 411013, India
Email: maheshh248@gmail.com | | Abstract | | During this covid-19 pandemic, a few cases of vertical transmission of severe acute respiratory syndrome coronavirus-2 from mothers to the fetus have been documented. Anti-SARS CoV-2 antibodies mediated multisystem inflammatory response syndrome (MIS-C) is known phenomenon in children. With this case report, we aim to demonstrate the evidence of fetal inflammatory response syndrome (FIRS) associated with anti-SARS CoV-2 antibodies in a premature neonate presenting with respiratory distress, seizures and shock in initial hours of life. The infant was RTPCR negative for covid-19, but positive for anti-SARS CoV-2 antibodies with raised inflammatory markers, suggestive of systemic inflammatory response syndrome. A comprehensive workup for other infectious pathogens also came up negative. Baby received IvIg and steroids and recovered completely. We believe that this systemic inflammation occurred due to antenatal exposure to the covid-19 virus and that more such instances will emerge in future. | | | | Keywords | | Anti-SARS CoV-2 antibodies, FIRS, MIS-N | | | | Introduction | | In current times, COVID-19, caused by SARS-CoV-2, has been a global public health crisis. The disease severity is less in neonates and young children for certain reasons .1 But recent reports of multisystem inflammatory syndrome in children, MIS-C, have been described by Kathleen M et al and Shreepal J et al.2,3 The specific mechanism is unknown, although it is thought to be related to immunological dysregulation caused by SARS CoV2 infection.4 The disease manifests as persistent high grade fever and multisystem involvement with raised inflammatory markers and requiring PICU management]2. The disease simulates Kawasaki disease and cytokine storm as in adults. Majority of the children are positive for anti SARS CoV2 antibodies while less number of kids are RTPCR positive.2 Unlike MIS-C, where SARS-CoV-2 infection and multisystem inflammation occur in the same subject, a few case reports suggest neonatal multisystem inflammation occurs secondary to maternal SARS-CoV-2 infection.5,6 Here we report a case of a newborn with very high SARS CoV-2 antibodies titre and elevated inflammatory markers who presented as multi systemic inflammation also known as fetal inflammatory response syndrome within the first few hours of life. | | | | Case Report | A 26 years old primigravida went into spontaneous labour at 32 weeks of gestation and a male neonate (birth weight 1474 grams) was delivered by vaginal delivery in a private nursing home at Pune, Maharashtra, India. Baby cried immediately at birth and did not require resuscitation (APGAR score 8 at 1 minute, 10 at 5 minutes) but within 30 minutes developed grunting and respiratory distress. Baby was then shifted urgently in a tertiary care NICU at Pune, Maharashtra, India, under standard transportation protocol in neonatal ambulance. Baby was initially placed on CPAP with a PEEP of 6 and a FiO2 of 30 percent, but due to her increasing work of breathing, baby was intubated and given positive pressure ventilation. Initial ABG was showing pH of 7.29, pCO2 46, pO2 97, HCO3- 22.1, BE -4.5, lactate 1.5. As initial chest X-ray showed normal volume lungs and was not suggestive of respiratory distress syndrome hence surfactant was not given. Within 4 hours of life, the baby presented as poor perfusion (with prolonged CRT of 5 seconds, hypotension, tachycardia and cold extremities) and metabolic acidosis. Functional echocardiography showed mild LV dysfunction with LV ejection fraction of 40%. So baby was started on inotropic support after initial fluid resuscitation. Baby was lethargic and developed seizures within 6 hours of life, which were managed with phenobarbitone and levetiracetam. Neurosonography was done on second day of life which showed germinal matrix hemorrhage and parenchymal patchy haemorrhage. In view of deranged coagulation and drop in haemoglobin, baby received plasma and PCV transfusion. Sepsis screen and blood culture was sent and broad spectrum iv antibiotics were initiated as per unit protocol. CSF studies were normal. Both CSF and blood culture came negative so antibiotics were stopped after 48 hours of initiation.
Baby’s perfusion improved gradually over 48 hours hence inotropes were weaned. Functional ECHO done on day 7 and day 10 of life showed improvement in myocardial contractility with ejection fraction of 50 and 55 percent respectively without inotropes. Follow up neurosonography done at 7 day of life was normal. Baby was gradually weaned on ventilator and extubated at 72 hours of life. After which baby required non invasive respiratory support in the form of CPAP till day 8 and high flow till day 24 of life respectively. In the background of covid-19 pandemic, RTPCR for SARS CoV-2 as well as anti SARS CoV-2 antibodies were tested on day 1 of life. Although RTPCR was negative ( did only once), antibody titres were positive and very high, ( see table 1 ). Mother was asymptomatic before and after delivery. Maternal SARS CoV-2 RTPCR, which was done at the time of delivery as per nursing home protocol, was negative but she was also positive for anti SARS CoV-2 IgG antibodies ( titres 3; COI >1 = reactive ) like her baby for anti SARS CoV-2 antibodies which was ordered after positive titres in baby. Inflammatory markers were evaluated sequentially and found to be significantly elevated. Hence intravenous immunoglobulin was given in dose of 2 gm/kg. After ruling out sepsis, injection methyl prednisolone was started in a dose of 2 mg/kg/day and given for total 14 days. Ravindra Pawar, et al has used similar doses of injection methyl prednisolone.7 Despite the fact that D DIMER levels were substantially higher, because there was no clinical evidence of thrombotic problems and the coronaries were not dilated, injection low molecular heparin was not started. All inflammatory parameters slowly returned to normal values. At the time of discharge, the baby had no further convulsions, was maintaining saturation on room air, and was taking breast feeding nicely.
Table 1. Laboratory findings.
| Blood tests |
Normal values |
At birth |
DOL1 |
DOL3 |
DOL4 |
DOL7 |
DOL9 |
DOL10 |
| Hb (gm/dl) |
14.5-22.5 |
18.2 |
12.5 |
15.7 |
|
|
14 |
13.5 |
| PCV (%) |
48-69 |
53 |
38 |
47 |
|
|
43 |
44 |
| TLC (/cmm) |
9000-30000 |
8500 |
15500 |
8000 |
|
|
6400 |
5300 |
| PMNs (/cmm) |
54-62 |
53 |
52 |
56 |
|
|
38 |
58 |
| Lymphocytes (/cmm) |
25-33 |
42 |
44 |
40 |
|
|
52 |
36 |
| Platelets (/cmm) |
84000-478000 |
223000 |
179000 |
110000 |
|
|
309000 |
321000 |
| PT/INR(sec) |
14-21/1.11 |
|
20/1.9 |
|
|
14.5 / 1.4 |
|
|
| aPTT (sec) |
Upto 45 |
|
50 |
|
|
31.9 |
|
|
| Sr creatinine (mg/dl) |
0.6-1.2 |
|
1.18 |
|
|
|
|
|
| Sr Na+ (mEq/L) |
134-146 |
135 |
138 |
|
|
131 |
137 |
|
| Sr K+ (mEq/L) |
3-7 |
4.3 |
3.7 |
|
|
4 |
4.5 |
|
| Sr Cl- (mEq/L) |
97-110 |
109 |
107 |
|
|
110 |
110 |
|
| Sr Calcium (mmol/L) |
1.07-1.27 |
|
1.12 |
|
|
|
|
|
| Sr magnesium (mg/dl) |
1.2-2.6 |
|
3.1 |
|
|
|
|
|
| Phosphorus (mg/dl) |
4.8-8.2 |
|
7.56 |
|
|
|
|
|
| Anti SARS CoV2 antibodies (IgG) |
Non reactive(COI <1); Reactive (COI >1) |
|
57 |
|
|
|
|
|
| CRP (mg/L) |
Upto 6 |
|
17.21 |
|
2.38 |
6.29 |
12.14 |
2.15 |
| LDH (iU/L) |
250-450 |
|
2477 |
|
251 |
|
|
|
| Sr ferritin (ng/ml) |
15-150 |
|
1115 |
|
|
|
|
|
| IL-6 (pg/ml) |
0-7 |
|
72.21 |
|
18.7 |
|
|
|
| D-Dimer (ng/ml) |
<252 |
|
>1200 |
|
12000 |
6250 |
|
|
| Troponin T (pg/ml) |
<80 |
|
1062 |
|
114.8 |
113 |
|
|
| Alkaline phosphatase (u/L) |
145-420 |
|
|
|
|
887 |
|
|
| CSF proteins (mg/dl) |
10-120 |
|
135 |
|
|
|
|
|
| CSF glucose (mg/dl) |
60% of BSL |
|
21 (BSL 66) |
|
|
|
|
|
| CSF cells (PMNs/Lymphocytes) (/cmm) |
0-15 (0/15) |
|
1 (0/1) |
|
|
|
|
|
| CSF culture |
|
|
|
|
No growth |
|
|
|
| Blood culture |
|
|
|
|
No growth |
|
|
|
| RTPCR for covid-19 |
|
|
|
Negative sample was sent on day 1, didn’t repeat the test again |
|
|
|
|
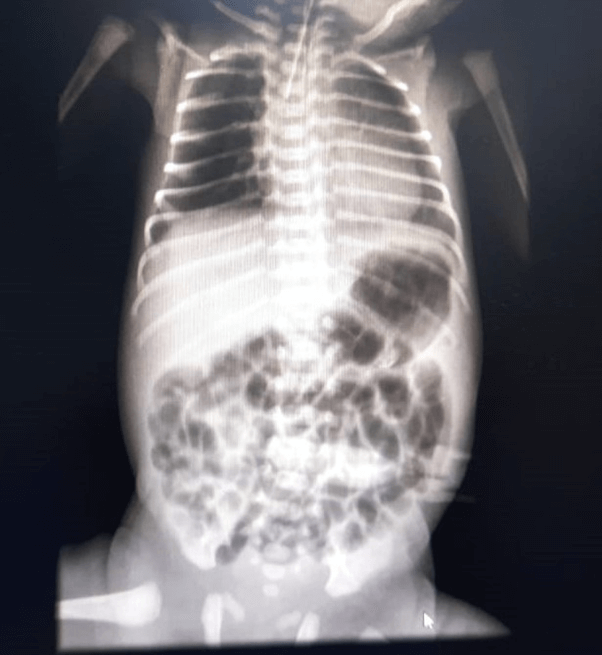
Figure 1. X-ray image, done at 1st hour of life immediately after stabilizing baby in NICU.
| | | | Discussion | We present this case report of a newborn presenting like multisystem inflammatory syndrome within initial few hours of life. The preterm newborn had respiratory failure, coagulopathy, seizures and cardiogenic shock. The common possible reasons for this multisystem involvement were investigated and ruled out. We attribute baby’s clinical worsening and very high inflammatory markers within first few hours of life to anti SARS CoV2 antibodies suggestive of antenatal exposure to SARS CoV-2. Similar findings were reported by Ravindra Pawar, et al7 and Saima Naz, et al.8 Fetus in utero deploys an inflammatory response to variety of infectious as well as non-infectious stimuli leading to fetal inflammatory response syndrome.9,10 Various reports have defined FIRS as elevated concentration of fetal interleukin-6.11 We label this presentation as fetal inflammatory response syndrome ( FIRS ) because all inflammatory markers, including IL-6, were considerably elevated in the newborn's blood samples taken in the first few hours of life ( cord blood samples were not available as the baby was delivered at another nursing home but was transported to NICU within 1 hour of life so we relate these blood samples to the cord blood samples ). Also, the neonate presented with the anti SARS CoV2 antibodies at birth itself meaning that the exposure to SARS CoV2 virus might have been in utero. These antibodies acted as the trigger for FIRS in this newborn. Older children, who present with MIS-C, have themselves exposed to SARS CoV2 virus a few weeks ago, but here in this case report, we assume that the newborn was exposed to the virus during fetal life itself. Similar findings were observed by Saima Naz, et al.8 The natural infection to mother, during pregnancy, may lead to development of protective antibodies in mother. These antibodies can cross placenta to provide passive immunity in the newborn. Besides this, secretory IgA in breast milk also offers protection for newborn.12 The vertical transmission of covid 19 infection is yet a topic of research but there are cases reported about vertical transmission of covid 19 from mother to fetus.6,8 We speculate that this vertical transmission may induce robust immune response in the fetus13 and immune dysregulation in the newborn may lead to similar picture like MIS C in older children].2,4 Also the response to intravenous immunoglobulin and methyl prednisolone supports the diagnosis of multisystem inflammatory syndrome in neonate.14 In this case report, the mother was tested for covid 19 by RTPCR test prior to delivery which came to be negative. The mother was not having any symptom suggestive of covid 19 neither she had received the vaccine ( as pregnant women were not eligible for vaccination as per guidelines in the prevailing time ). But she remembers one episode of upper respiratory infection 1 month before the delivery which was treated by general physician and which got relieved uneventfully, she was neither tested for covid 19 that time nor she remembers any contact with covid 19 patient. The lady presented in preterm unexpected labour, didn’t receive antenatal steroids and the neonate was delivered prematurely which could have been triggered because of fetal inflammatory response.15 X ray chest was not suggestive of respiratory distress syndrome and baby did not require surfactant. Blood culture was negative and there was no deterioration even after stopping of antibiotics rules out early onset sepsis. Perinatal history and postnatal lab parameters were not consistent with perinatal asphyxia. Functional echo ruled out hemodynamically significant patent ductus arteriosus (HsPDA).
The treatment for FIRS, triggered by anti SARS CoV2 antibodies, is primarily supportive along with IvIg and steroids6, this neonate received intravenous immunoglobulin and methyl prednisolone after ruling out sepsis and other possible causes of this clinical presentation. Baby responded well to this supportive and immune modulatory management. | | | | Conclusion | | We conclude that maternal history of SARS CoV2 infection or exposure during antenatal period is important as far as neonatal outcome is concerned. Vertical transmission of covid 19 infection from mother to fetus is possible and it may trigger FIRS in the newborn. In the background of this current covid 19 pandemic it is prudent to suspect SARS Cov-2 related FIRS in any neonate with rapid and unexplained worsening in early life. Although these types of cases are less in number at present, we may get to see increase in such cases as the time progresses. | | | Declarations :
Informed Consent Written informed consent was taken from the parents of the neonate.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Petra Zimmermann , Nigel Curtis. Why is COVID-19 less severe in children? A review of the proposed mechanisms underlying the age-related difference in severity of SARS-CoV-2 infections. Arch Dis Child 2020 Dec 1;archdischild-2020-320338 [CrossRef] [PubMed]
- Kathleen M. Matic, MD, FAAP. SARS-CoV-2 and Multisystem Inflammatory Syndrome In Children (MIS-C). Curr Probl Pediatr Adolesc Health Care. 2021 Apr;51(4):101000. [CrossRef] [PubMed] [PMC free article]
- Shreepal J, Supratim S, Srinivas L, Prashant B, Sumitra V, Soonu U, Laxmi S, Parmanand A, Tanuja K And Snehal K. Multisystem Inflammatory Syndrome in Children With COVID-19 in Mumbai, India. Indian Pediatr. 2020 Nov 15(57):1015-1019 [CrossRef] [PubMed] [PMC free article]
- Pui Y Lee, Craig D Platt, Sabrina Weeks, Rachael F Grace, George Maher, Kasey Gauthier, Sridevi Devana, Sally Vitali, Adrienne G Randolph, Douglas R McDonald, Raif S Geha, Janet Chou. Immune dysregulation and multisystem inflammatory syndrome in children (MIS-C) in individuals with haploinsufficiency of SOCS1. J Allergy Clin Immunol. 2020 Nov;146(5):1194-1200.e1. [CrossRef] [PubMed] [PMC free article]
- Lana A. Shaiba, Adnan Hadid, Khalid A. Altirkawi, Hind M. Bakheet , Aminah Mohammed Alherz, Shaik Asfaq Hussain, Badr H. Sobaih, Abdulrahman M. Alnemri, Rana Almaghrabi, Medina Ahmed, Maria A. Arafah, Abdullah Jarallah, Elham Essa Bukhari and Fahad A. Alzamil. Case Report: Neonatal Multi-System Inflammatory Syndrome Associated With SARS-CoV-2 Exposure in Two Cases From Saudi Arabia. Front Pediatr. 2021 May 13;9:652857. [CrossRef] [PubMed] [PMC free article]
- Sam Schoenmakers, Pauline Snijder, Robert M. Verdijk, Thijs Kuiken, Sylvia S. M. Kamphuis, Laurens P. Koopman, Thomas B. Krasemann, Melek Rousian, Michelle Broekhuizen, Eric A. P. Steegers, Marion P. G. Koopmans, Pieter L. A. Fraaij, and Irwin K. M. Reiss. Severe Acute Respiratory Syndrome Coronavirus 2 Placental Infection and Inflammation Leading to fetal Distress and Neonatal Multi-Organ Failure in an Asymptomatic Woman. J Pediatric Infect Dis Soc. 2021 May 28;10(5):556-561 [CrossRef] [PubMed] [PMC free article]
- Ravindra Pawar , Vijay Gavade , Nivedita Patil , Vijay Mali , Amol Girwalkar , Vyankatesh Tarkasband , Sanjog Loya , Amit Chavan , Narendra Nanivadekar , Rahul Shinde , Uday Patil and Satyan Lakshminrusimha. Neonatal Multisystem Inflammatory Syndrome (MIS-N) Associated with Prenatal Maternal SARS-CoV-2: A Case Series. Ravindra Pawar , Vijay Gavade , Nivedita Patil , Vijay Mali , Amol Girwalkar , Vyankatesh Tarkasband , Sanjog Loya , Amit Chavan , Narendra Nanivadekar , Rahul Shinde , Uday Patil and Satyan Lakshminrusimha. Children (Basel). 2021 Jul 2;8(7):572. [CrossRef] [PubMed] [PMC free article]
- Saima Naz, Tayyaba Rahat, and Farah Naz Memon Research, Development & Coordination Section, Pakistan Health Research Council, Islamabad, Pakistan. Vertical Transmission of SARS-CoV-2 from COVID-19 Infected Pregnant Women: A review on Intrauterine Transmission. Fetal Pediatr Pathol. 2021 Feb;40(1):80-92 [CrossRef] [PubMed]
- Eunjung Jung, Roberto Romero, Lami Yeo, Ramiro Diaz-Primera, Julio Marin-Concha, Robert Para, Ashley M. Lopez, Percy Pacora, Nardhy Gomez-Lopez, Bo Hyun Yoon, Chong Jai Kim, Stanley M. Berry, Chaur-Dong Hsu. The fetal inflammatory response syndrome: the origins of a concept, pathophysiology, diagnosis, and obstetrical implications. Semin Fetal Neonatal Med. 2020 Aug;25(4):101146. [CrossRef] [PubMed]
- Sreus A. G. Naidu , Roger A. Clemens , Peter Pressman , Mehreen Zaigham , Kamran Kadkhoda , Kelvin J. A. Davies, and A. Satyanarayan Naidu. COVID-19 during Pregnancy and Postpartum. J Diet Suppl 2020 Nov 8;1-28 [CrossRef]
- Eunjung Jung, Roberto Romero, Lami Yeo, Ramiro Diaz-Primera, Julio Marin-Concha, Robert Para, Ashley M. Lopez, Percy Pacora, Nardhy Gomez-Lopez, Bo Hyun Yoon, Chong Jai Kim, Stanley M. Berry, Chaur-Dong Hsu The fetal inflammatory response syndrome: the origins of a concept, pathophysiology, diagnosis, and obstetrical implications. Semin Fetal Neonatal Med. 2020 Aug;25(4):101146. [CrossRef] [PubMed]
- Ryan M. Pace, Janet E. Williams, Kirsi M. Järvinen, Mandy B. Belfort, Christina D. W. Pace, Kimberly A. Lackey, Alexandra C. Gogel, Phuong Nguyen-Contant, Preshetha Kanagaiah, Theresa Fitzgerald, Rita Ferri, Bridget Young, Casey Rosen-Carole, Nichole Diaz, Courtney L. Meehan, Beatrice Caffé, Mark Y. Sangster,David Topham, Mark A. McGuire, Antti Seppo, Michelle K. McGuirea Characterization of SARS-CoV-2 RNA, Antibodies, and Neutralizing Capacity in Milk Produced by Women with COVID-19. mBio. 2021 Feb 9;12(1):e03192-20. [CrossRef] [PubMed] [PMC free article]
- Alice Lu-Culligan, Arun R. Chavan, Pavithra Vijayakumar, Lina Irshaid, Edward M. Courchaine, Kristin M. Milano, Zhonghua Tang, Scott D. Pope, Eric Song, Chantal B.F. Vogels, William J. Lu-Culligan, Katherine H. Campbell, Arnau Casanovas-Massana, Santos Bermejo, Jessica M. Toothaker, Hannah J. Lee, Feimei Liu, Wade Schulz, John Fournier, M. Catherine Muenker, Adam J. Moore, Yale IMPACT Team, Liza Konnikova, Karla M. Neugebauer, Aaron Ring, Nathan D. Grubaugh, Albert I. Ko, Raffaella Morotti, Seth Guller, Harvey J. Kliman, Akiko Iwasaki and Shelli F. Farhadian Maternal respiratory SARS-CoV-2 infection in pregnancy is associated with a robust inflammatory response at the maternal-fetal interface. Med (N Y). 2021 May 14;2(5):591-610.e10. [CrossRef] [PubMed] [PMC free article]
- Clinical practice guideline, perinatal-neonatal management of covid-19 summary of recommendations Ver.3.0 | 16 June 2021. Report. National Neonatology Forum, India Federation of Obstetric & Gynaecological Societies of India Indian Academy of Pediatrics
- David A. Schwartz, MD, MS Hyg. An Analysis of 38 Pregnant Women With COVID-19, Their Newborn Infants, and Maternal-Fetal Transmission of SARS-CoV-2 Maternal Coronavirus Infections and Pregnancy Outcomes. Arch Pathol Lab Med. 2020 Jul 1;144(7):799-805. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2022.45
|
| Cite this article as: | | Shinde M D, Khamkar A M, Pote P D, Suryawanshi P B. Fetal Inflammatory Response Syndrome Associated With SARS-CoV-2 Exposure In Utero. Pediatr Oncall J. 2022;19: 127-130. doi: 10.7199/ped.oncall.2022.45 |
|