Shraddha Lohia1, Anilkumar M Khamkar2, Georgeena Elsa Jose3, P. D. Pote3.
1Pediatric Nephrologist, Noble Hospital and Research Center, Hadapsar, Pune, India,
2Academic Head NICU and Senior Consultant Neonatologist, Noble Hospital and Research Center, Hadapsar, Pune, India,
3Department Of Pediatrics, Noble Hospital and Research Center, Hadapsar, Pune, India.
ADDRESS FOR CORRESPONDENCE
Dr. Georgeena Elsa Jose, Junior Resident, Department of Pediatrics, Noble Hospital and Research Center, 153, Magarpatta City Road, Pune, India - 411013.
Email: egeorgeena@gmail.com | | Abstract | | Congenital nephrotic syndrome (CNS) is a rare and serious disease of infants, which is due to a genetic and or an infectious cause. First case is an 11-week old baby, a completely worked-up case which includes the tetrad of clinical manifestations (neurological, gastro-intestinal and renal), virological findings (positive CMV antibody and DNA PCR), histo-pathological findings and novel genetic mutation (c.712+1G>C) in NPHS 1 gene. On the contrary, the second case is an 8-week old baby with isolated renal involvement of CMV infection. CMV IgM was positive but CMV DNA polymerase chain reaction (PCR) was negative. Parents were unwilling to do a genetic work up. In the first case partial remission of renal symptoms were achieved with ganciclovir in four weeks, but she succumbed due to sepsis after being followed up for 730 days. The pediatrician of the second child skipped ganciclovir and gave four weeks steroid trial. Due to absence of remission, renal biopsy was done and tacrolimus was started. No recurrence of proteinuria was observed during the 14-month follow-up period. The need of anti-CMV therapy in isolated renal involvement of congenital CMV infection is questionable as the insult to the kidney has already occurred. It also highlights the dilemma perceived by a pediatrician, in starting anti-CMV therapy when CMV IgM antibodies are positive but CMV DNA PCR result is negative. This paper emphasizes the importance of performing a genetic test in every case of CNS to rule out any hereditary causes. | | | | Keywords | | Cytomegalovirus infection, Congenital Nephrotic Syndrome, NPHS 1, Novel mutation, Gancyclovir | | | Background
Nephrotic syndrome presenting within first three months of life is defined as congenital nephrotic syndrome (CNS). It can be caused by genetic defects in structural proteins that form the glomerular filtration barrier or secondary to infections like congenital syphilis, toxoplasmosis and cytomegalovirus infection (CMV) which disrupt the podocytes and/or the basement membrane.1 Till 2020, only four completely worked up CMV IgM positive CNS cases were reported globally signifying the low incidence of detection.2 We present the case of two infants with congenital CMV infection and nephrotic syndrome, one of whom one received anti-CMV therapy while the other did not and both of them experienced proteinuria remission. | | | | Case Report | Case 1
The first case was an 11-week-old female baby (ex 36 weeks gestational age, corrected age 7 weeks) who was referred to us with acute gastroenteritis and generalized tonic clonic seizures. Later the baby developed progressive generalized swelling of the body and decreased urine output for 2 days. The patient was the second child of non-consanguineous parents. The couple’s firstborn son is healthy. Pregnancy was complicated by moderate oligohydramnios and decreased fetal movements which led to emergency caesarean-section. Mother had no fever or rash during pregnancy. Birth weight was 2200 g (10th weight percentile). The weight of the placenta is not known but mother recollects it being almost as big as the baby. APGAR was 7 and 8 after 1 and 5 minutes, respectively. Immunizations, including pneumococcal conjugate vaccine -13 shots, were up to date.
At presentation, the baby was alert but irritable. She had microcephaly without any dysmorphic features. She had pallor, peri-orbital puffiness, marked genital edema and bilateral pitting pedal edema. There was no rash, jaundice, lymphadenopathy, petechiae, or ecchymoses. She had tachycardia (180 beats per minute) and tachypnea (62 per minute). The abdomen was distended with a palpably enlarged liver (3 cm below the right costal margin) and spleen (2 cm below left costal margin). Weight (with edema) was 3.7 kg (less than 3rd centile), length 50 cm (less than 3rd centile) and head circumference 35.5 cm (less than 3rd centile) as per WHO charts.
Case 2
The second case was an 8-week-old male baby (ex 36 weeks gestational age, corrected age 4 weeks) who presented with abdominal distension since birth, progressive in nature attained to the current size at presentation with engorged veins over the abdomen. The baby also had respiratory distress associated with it. This baby was the third child born out of 3rd degree consanguineous marriage, with previously two healthy children. In this case also the mother denied fever or rash during pregnancy and her urinalysis was normal. Child was born by normal vaginal delivery with an uneventful antenatal history. The birth weight was 2700 g and weight of the placenta was not known. APGAR was 8 and 9 after 1 and 5 minutes, respectively. Immunization was complete for respective age as per national immunization schedule.
On examination the baby was irritable with tachycardia (177 beats per minute) and tachypnoea (69 per minute). He had pallor, abdominal distension and bilateral pitting pedal edema without any icterus, lymphadenopathy, hyperpigmentation or rashes. Abdomen was distended with dilated veins over bilateral hypochondrium and epigastrium which were non-pulsatile. Weight (with edema) was 4.5 kg (between 3rd to 10th centile), length 52 cm (between 3rd to 10th centile) and head circumference 35 cm (3rd centile) as per WHO charts.
Investigations
Case 1
This baby was admitted in pediatric intensive care unit (P-ICU), with a provisional diagnosis of CNS with suspicion of spontaneous bacterial peritonitis. Laboratory findings showed severe hypoalbuminaemia, a high urinary protein dipstick level and hypercholesterolemia being consistent with nephrotic syndrome (shown in Table.1). The hemoglobin levels dropped from 9.4 gm% to 6.3 gm% in three days and peripheral blood smear was suggestive of microcytic hypochromic anemia with anisocytosis. Reticulocyte count, serum iron and ferritin levels were normal. Other secondary findings were low corrected calcium and sodium levels. Liver and renal and function parameters were within normal limits. Toxoplasmosis, rubella, cytomegalovirus and herpes virus complex (TORCH) antibody assessment showed CMV IgM positivity. The CMV polymerase chain reaction (PCR) of the blood sample was also positive showing 9542 copies/ml. Tests for other infections like hepatitis B and C were negative.
Table 1. Description of two infants with their clinical characteristics, histopathology report and or genetic work-up.
| Clinical Characteristics |
Case 1 |
Case 2 |
| Gender |
Female |
Male |
| Birth weight (kg) |
2.2 |
2.7 |
| Gestational Age (weeks) |
36 |
36 |
| Oligo/Polyhydraminos |
Oligohydraminos |
- |
| Consanguinity |
No consanguinity |
3rd degree consanguinity |
| History of previous fetal loss or sibling death from renal cause |
- |
- |
| Age of presentation to the tertiary care center (weeks) |
11 |
8 |
| Microcephaly |
Present |
Absent |
| Cardiac abnormalities |
- |
- |
| Hepato-splenomegaly |
Present |
Absent |
| Serum Albumin at the time of presentation (3-5 gm/dl) |
0.89 |
1.05 |
| Serum total cholesterol at the time of presentation (<170 mg/dl) |
211 |
300 |
| Serum Creatinine at the time of presentation (0.2-0.4 mg/dl) |
0.33 |
0.2 |
| Urine dipstick protein |
3+ |
3+ |
| TORCH screen, HIV, Hep B, Hep C |
All negative except CMV Ig M |
All negative except CMV Ig M |
| DNA PCR for CMV (Quantitative viral load) |
9542 copies/ml |
Negative |
| Genetic work up in the index child Gene (transcript) |
Homozygous mutation in intron 6 of NPHS1 c.172+ 1G>C (5' splice site) |
Not done |
| Method of genetic testing |
Sanger Sequencing |
Not done |
| Renal histopathology |
|
|
| Light microscopy |
Mesangio-proliferative glomerulopathy |
Mesangio-proliferative glomerulopathy |
| Direct immunofluorescence |
No significant glomerular immune deposits |
Trace mesangial IgM granular deposits |
| Electron microscopy |
Tubulo-reticular inclusions in glomerular endothelial cell cytoplasm |
Tubulo-reticular inclusions in glomerular endothelial cell cytoplasm |
| Magnetic Resonance Imaging Brain |
T2 weighted images showing white matter hyper-intensities in right frontal region |
Not done |
| Electroencephalogram |
Generalised epileptiform discharges |
Not done |
| Oto-acoustic emission tests |
Bilateral ear -Pass |
Bilateral ear -Pass |
| Fundus examination |
No evidence of CMV retinitis |
No evidence of CMV retinitis |
| Initial management in children |
|
|
| Albumin infusion |
Received |
Received |
| Angiotensin converting enzyme inhibitor |
Received |
Received |
| Antiviral agents |
Received (IV Gancyclovir and oral Valgancyclovir ) total for 28 days |
Not Received |
| Immunosuppresant medicines |
|
|
| Corticosteroids |
Received |
Received 4 weeks trial (no remission) |
| Tacrolimus |
Not Received |
Received |
| Response during presentation |
|
|
| Complete / Partial remission |
Partial remission |
Complete remission |
| Outcome |
Developed ESRD and died of sepsis after being followed up for 730 days |
At 14 months in remission |
|
TORCH - toxoplasmosis, rubella, cytomegalo virus and herpes virus screen; DNA PCR for CMV - DNA polymerase chain reaction test for cytomegalovirus infection; HIV - human immunodeficiency virus; Hep.B - Heaptitis B; Hep.C-Hepatitis C; ESRD- end stage renal disease
|
Ultrasonography of the abdomen showed normal-sized, hyperechoic kidneys with loss of cortico-medullary differentiation, moderate ascites and hepato-splenomegaly. Magnetic resonance imaging (MRI) of the brain showed white matter hyperintensities in right frontal region in the T2 weighted images indicative of CMV-associated central nervous system involvement. Electro-encephalogram showed generalized epileptiform discharges. Echocardiogram and oto-acoustic emission (OAE) test were normal. Ophthalmological examination revealed no evidence of CMV retinitis An ultrasound guided renal biopsy was performed after seven days of hospitalization (four days after starting ganciclovir), analyzing 32 glomeruli which showed a mesangio-proliferative glomerulopathy with no diffuse mesangial sclerosis (shown in Figure 1). Electron microscopy (EM) revealed occasional endothelial tubulo-reticular inclusions (shown in Figure 2). The genetic testing was done and showed a novel pathogenic homozygous 5’ splice site (c.712+1G>C) variant mutation in NPHS1 gene.
Figure 1. Light microscopy of the kidney biopsy specimen with periodic acid silver methenamine staining revealing glomeruli containing focal and segmental mild to moderate mesangial hyperplasia.
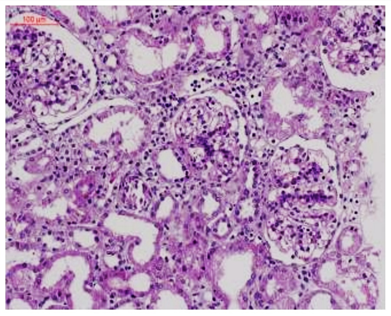
Figure 2. Electron microscopy of the kidney biopsy specimen showing diffuse effacement of the visceral epithelial foot processes were seen with no electron dense deposits. Tubulo-reticular inclusions identified in glomerular endothelial cell cytoplasm.

Case 2
This baby was admitted in P-ICU for further evaluation of congenital ascites and received supportive treatment for respiratory distress. In this case also the laboratory findings showed severe hypoalbuminaemia, a high urinary protein dipstick level with elevated total serum cholesterol levels and normal renal function tests (shown in Table.1). TORCH screening test showed CMV IgM positivity, but the DNA PCR for CMV in the blood sample was negative. Tests for other infections like hepatitis B and C were negative. Liver and thyroid function tests, OAE and echocardiography were normal. There was no evidence of CMV retinitis or central nervous system involvement.
An ultrasound guided renal biopsy was performed analyzing 53 glomeruli revealing mesangio-proliferative glomerulopathy, occasional foci of tubular atrophy and tubular microcalcinosis. Direct immune-fluorescence revealed trace mesangial granular IgM deposits and electron microscopy showed tubulo-reticular inclusions in glomerular endothelial cell cytoplasm indicating an infectious etiology. Due to financial constraints genetic work up was not done in this child.
Differential Diagnosis
The differential diagnosis of CNS includes diffuse mesangial sclerosis, congenital nephrotic syndrome of the Finnish type, Denys-Drash syndrome, Wilms tumor and Galloway-Mowat syndrome.
In both the cases, the clinical presentation, laboratory data and kidney biopsy findings, with or without genetic mutation, led us to conclude that CNS with congenital CMV was the diagnosis. Apparently when the genetic testing was done in the first case, a novel mutation was found in NPHS1 gene.
Treatment
The first case was given supportive treatment with 20% albumin and furosemide infusion, packed red cell transfusion, intravenous calcium gluconate, hypertonic saline, intravenous third-generation cephalosporins, phenobarbitone, enalapril and spironolactone. In view of CMV infection, intravenous ganciclovir (30 mg/kg/day) was initiated and was given for two weeks. Later switched over to oral valganciclovir (30 mg/kg/day) which was also administered for two weeks. It was given for a total of 28 days. During the ganciclovir treatment phase, neutropenia was monitored on a weekly basis. The second case was treated with 20% albumin and furosemide infusion, intravenous third-generation cephalosporins, enalapril and spironolactone. Treatment with ganciclovir was denied by parents. Subsequently the baby was administered prednisolone (by a local pediatrician), followed by tacrolimus in the event of non-response.
Outcome and follow-up
In the first case, CMV DNA became undetectable in plasma after 3 weeks of antiviral therapy and proteinuria improved against the presumptive clinical diagnosis of a genetic form of CNS. Six week prednisolone trial which started after the complete course of targeted anti-viral therapy, did not help and thus was stopped. Parents were unwilling for tacrolimus and for nephrectomy (medical/surgical). Angiotensin converting enzyme inhibitors helped to attain a state of partial remission. Tragically, at the age of 2 years she developed end stage renal disease and the patient succumbed to fulminant sepsis and death.
In the second case, baby received prednisolone trial for four weeks, to which the baby did not respond. Subsequently the baby was started on tacrolimus after renal biopsy which showed significant difference in proteinuria (urine protein-trace/+1). No recurrence of nephrotic range proteinuria was observed during the follow-up period of 14 months.
| | | | Discussion | The first case exhibits features of classical (Finnish-type) CNS due to a homozygous NPHS1 pathogenic variant, complicated by congenital CMV infection. The baby had microcephaly, hepato-splenomegaly and neurological involvement in the form of white matter hyper intensities in the right frontal lobe on T2 weighted images of MRI Brain. The histological findings were consistent with what has been described in CMV-related CNS by Chen et al, including mesangio-proliferative lesions, diffuse podocyte effacement and endothelial tubulo-reticular inclusions.3
First case was CMV IgM positive and CMV DNA PCR showed high titers. The baby was administered anti-CMV therapy for a total of four weeks and attained partial remission. While the second case showed an isolated renal involvement of CMV manifesting clinically as CNS, with similar histological features. Here CMV IgM was positive while CMV DNA PCR was negative. No anti-CMV therapy was administered and genetic studies were not done. There are no conclusive consensus whether anti-CMV therapy should be administered in cases of CMV associated renal involvement. However the literature portrays occasional studies including the study by Jacob etal and Chen etal, where anti-CMV therapy was instituted in CMV associated CNS.2,3
From India, Murugananth et al, describes the first case of isolated renal involvement of CMV infection in an infant who presented with reno-megaly, transient renal failure and renal biopsy with CMV inclusions.4 Similarly, our second case is also a sole renal manifestation of CMV infection. It is different from this above mentioned study, as the baby manifested in the form of nephrotic syndrome. To the best of our knowledge, this is the first reported case of CNS from India, which is an isolated renal manifestation of a congenital CMV infection. The mechanism of CMV-induced glomerular injury and podocytopathy is ill defined. However, some studies imply that tissue injury is caused directly by the virus, that the insult is mediated by the T-cell response and that the immune complex is formed as a result of the insult.5 This thinking raises the question of whether a targeted antiviral therapy is indeed necessary in the treatment of CMV-mediated kidney damage, a subject that is yet to be answered.
A novel homozygous 5’ splice site variation in intron 6 of the NPHS1 gene (c.712+1G>C) was noted in the first case. It was classified likely as a pathogenic variant based on the recommendations of American College of Medical Genetics. This mutation is not reported till date in the 1000G and ExAC databases. Such pathogenic variants in NPHS1 mutation cause classical Finnish type CNS.6 Few other novel mutations in NPHS1 gene was reported recently by Sinha et al in 2020 [7].
The first case illustrates a completely characterized case of CNS with concurrent CMV infection. Sinha et al describes that concomitant genetic mutations are present in significantly large number (23%) of the patients with CNS.7 Therefore, genetic diagnosis of the index case should be promoted considering the poor prognosis, large socioeconomic burden and the high recurrence rate in 25% of subsequent pregnancies due to the autosomal recessive inheritance pattern of CNS. It changes the management completely.
Another significant stumbling block is the complexity of variant interpretation and analysis. There is an obscurity in the genotype-phenotype correlation especially when there is a genetic heterogeneity and when genes have reduced penetrance.8 Getting genetic analysis done in each case gets the genetic pool or database to expand, hence contributing to revisit the existing knowledge and understanding of the genetic basis of many diseases. This would also help to modify the gene- disease scoring system and helps to upgrade clinically relevant gene findings. However our case had a homozygous pathogenic mutation easing the challenges in interpretation. The need of the hour is to percolate this awareness among the general pediatricians to promote genetic studies and also to offer services of clinical geneticists and syndromologists. This aids in better clinical diagnosis and management as they play a pivotal role in guiding the care of such children.
Learning points
• Nephrotic syndrome may be the sole manifestation of a CMV disease.
• The role of antivirals in treating a CNS case is questionable especially in cases of isolated renal involvement, as the insult to the kidney has already occurred.
• Genetic analysis is crucial to exclude hereditary CNS, signifying the importance of timely and complete diagnostic workup which includes the tetrad of clinical findings, virological work up, histo-pathological and molecular genetic studies.
| | | | Acknowledgement | | We would like to thank the parents for co-operating and for providing written consent for publishing this case report. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Wang JJ, Mao JH. The etiology of congenital nephrotic syndrome: current status and challenges. World J Pediatr. 2016; 12(2): 149- 58. [CrossRef] [PubMed]
- Jacob A, Habeeb SM, Herlitz L et al. A Case Report: CMV-Associated Congenital Nephrotic Syndrome. Front. Pediatr. 2020; 8:799 [CrossRef] [PubMed] [PMC free article]
- Chen Y, Zhang Y, Wang F, et al. Analysis of 14 Patients With Congenital Nephrotic Syndrome. Front Pediatr. 2019; 7:341. [CrossRef] [PubMed] [PMC free article]
- Murugananth S, Padmaraj R, Gopalakrishnan N et al. Isolated renal involvement of cytomegalovirus inclusion disease in an infant. Saudi J Kidney Dis Transpl. 2018;29(1):198-201. [CrossRef] [PubMed]
- Platt JL, Sibley RK, Michael AF. Interstitial nephritis associated with cytomegalovirus infection. Kidney Int. 1985; 28:550-2. [CrossRef] [PubMed]
- Kestila M, Lenkkeri U, Mannikko M, Lamerdin J, McCready P, Putaala H, et al. Positionally cloned gene for a novel glomerular protein-nephrin- is mutated in congenital nephrotic syndrome. Mol Cell. (1998) 1:575-82. [CrossRef]
- Sinha R, Vasudevan A, Agarwal I, Sethi SK, Saha A, Pradhan S etal. Congenital Nephrotic Syndrome in India in the Current Era: A Multicenter Case Series. Nephron. 2020;144 (1):21-29. [CrossRef] [PubMed]
- Jin YY, Feng BY, Mao JH. The status quo and challenges of genetic diagnosis in children with steroid-resistant nephrotic syndrome. World J Pediatr. 2018; 14(2):105-109. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2022.46
|
| Cite this article as: | | Lohia S, Khamkar A M, Jose G E, Pote P D. Is Cytomegalovirus a Partaker or a By-stander in Congenital Nephrotic Syndrome? : A novel mutation update.. Pediatr Oncall J. 2022;19: 122-126. doi: 10.7199/ped.oncall.2022.46 |
|