Ana Torres Rebelo1, Ana Isabel Martins2, Sara Rodrigues1, Josue Pereira3, Sónia Aires1.
1Pediatrics department, Centro Hospitalar de Entre o Douro e Vouga, Santa Maria Da Feira, Portugal,
2Pediatrics department, Centro Hospitalar e Universitário de Coimbra, Coimbra, Portugal,
3Pediatric Neurosurgeon, Department of Neurosurgery, Centro Hospitalar Universitário de São João CHUSJ e Faculdade de Medicina da Universidade do Porto FMUP, Porto, Portugal.
ADDRESS FOR CORRESPONDENCE
Ana Torres Rebelo, Rua Doutor José Bragança Tavares, 4580-123. Mouriz Paredes, Portugal
Email: anatorresrebelo@gmail.com | | Abstract | Arachnoid cysts (AC), extra-axial cerebrospinal fluid (CSF) collections of variable brain and spine location, are generally asymptomatic and detected incidentally on imaging. When large, or during expanding processes, may cause neurological signs and symptoms, mainly by intracranial hypertension (ICH). Cranial nerve deficits are rare presenting manifestations associated with AC.
An 8-year-old boy was observed at the emergency department with 3 months history of headache and double vision. On physical examination, a sixth cranial nerve palsy was identified. Computed tomography scan and magnetic resonance imaging detected a large arachnoid cyst in the left middle, posterior and anterior cranial fossa with brain compression and midline shift. Endoscopic fenestration of the arachnoid cyst to basal cisterns was performed with complete clinical recovery. | | | | Keywords | | Huge arachnoid cyst, Sixth cranial nerve palsy/Etiology, Diplopia/Etiology, Children, Endoscopic fenestration, Intracranial hypertension | | | | Case Report | A previously healthy 8-year-old boy, presented to the Emergency Department (ED), referred by the Ophthalmologist with headache (referred to the left frontal and temporal area) and diplopia for three months. Few days prior to his ED visit, the headache had been progressively worsening and he also referred nocturnal awakening. Additionally, he had been experiencing sporadic nausea and vomiting the week before; he lost four kilograms in two months. There was no history of recent trauma.
Of note, one year before admission, the patient was diagnosed with astigmatism and referenced to ophthalmology, changed glasses graduation twice, with persistent headache and diplopia. During his preoperative ophthalmology appointment, the patient was diagnosed with bilateral papilledema, which resulted in his transfer to the ED.
On physical examination, abduction of both eyes was deficient consistent with bilateral sixth cranial nerve palsy. The remaining neurological examination was unremarkable.
Cranial computed tomography (CT) scan revealed a large arachnoid cyst with mass effect and a concomitant chronic subdural hygroma on the left and he was referred to Paediatric Neurosurgery.
Magnetic Resonance Imaging (MRI) of the brain confirmed a left arachnoid cyst in the middle, posterior and anterior cranial fossa measuring 97x63 x84 mm with the mass effect on the left cerebral hemisphere and displacement of the midline structures, particularly in the frontotemporal region, with compression of the ventricular system and mesodiencephalic area. (Gallasi type 3 cyst, figure 1-2). Bone erosion of large sphenoid wing and parietal bone was also described.
Endoscopic fenestration of the arachnoid cyst to the basal pontine cisterns by a temporal burr hole was performed. Control imaging after this survival intervention revealed a decrease in the size and mass effect of both the cyst and subdural hygromas. At his two weeks follow-up external appointment he remains asymptomatic with normal ocular motility.
Figure 1 (a,b). Axial CT images of the temporal left arachnoid cyst seen along the frontal and temporal lobe with displacement of the ventricular system and midline structures to the right.
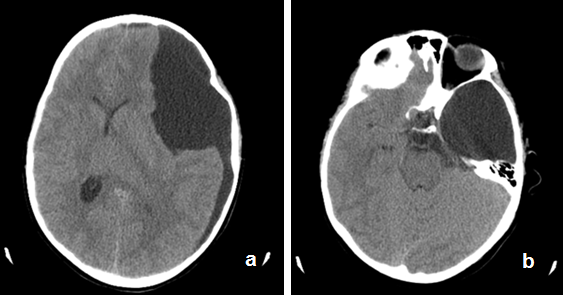
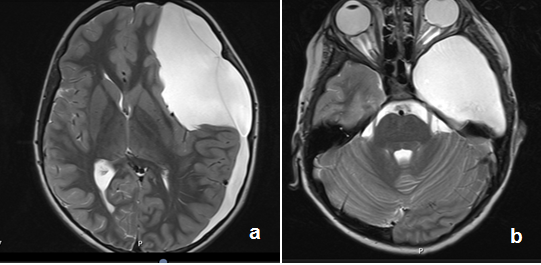
Figure 2 (a,b). Axial T2-weighted MRI images of the huge arachnoid cyst and associated homolateral parietal hygromas (a) protruding to the left prepontine cistern and nerves (b).
| | | | Discussion | Arachnoid cysts (AC) are congenital malformations accounting for approximately 1% of all intracranial mass lesions.1,2,3,4,5 The increasing use of imaging exams has led to more frequent diagnoses of AC.5 It is a benign lesion, composed of cerebral spinal fluid (CSF) within the arachnoid membrane. There is a prevalence of AC in males.5,6
The differential diagnosis of arachnoid cysts includes chronic subdural hygromas, dermoid cysts, infarcts, abscess and other cysts lesions.1
Arachnoid cysts are either primary (congenital) or secondary. Primary cysts arise from the splitting of the arachnoid membranes in intrauterine life, causing abnormal collections of CSF.2 Secondary cysts, less common, mostly occur after trauma, surgery, infection, or brain intracranial hemorrhage.4,7,8,9
In most cases, arachnoid cysts are congenital, but usually do not cause any symptoms and are found incidentally.3,10 Clinical presenting characteristics of AC depend on age, location, cyst volume and complication by other congenital abnormalities.9 If large, they can lead to neurovascular structures displacement and increased intracranial pressure (caused by expansion or secondary bleeding). Headaches are the most common symptom.4,7 AC may also be associated with other clinical presentations such as seizures, cranial deformities, obstructive hydrocephalus, cranial neuropathy, visual and hearing loss and endocrinopathies.1,2,5
Additionally, the cysts can rupture into the subdural space resulting in subdural hygromas (presence of CSF in the subdural space lined by fibrinous membranes) or even hematomas (blood containing spaces), with associated intracranial hypertension.5
Chronic compression by intracranial cystic lesion can led to nerve palsy and bone changes.2,12 In this case, abduction of both eyes was deficient, due to sixth nerve palsy. Review of literature confirms that arachnoid cysts are a rare cause of acquired sixth nerve palsy in children.12
AC can be formed everywhere on the cerebrospinal axis by widening spaces along the sheath of arachnoid membranes, but most lesions are in the middle cranial fossa (50-65%), half of which are in relation to the sylvian cistern.4,5,6
The Galassi classification categorizesmiddle fossa cysts into three types. Type I cysts are asymptomatic , present in the anterior middle cranial fossa. Type II cysts are larger and occasionally widening the Sylvian fissure and displacing the temporal lobe. Type III cysts occupy the entire middle cranial fossa, with extense opening of the Sylvian fissure and displacement of temporal, parietal and frontal lobes.4
Although AC are common intracranially, they may also appear in intradural spinal spaces.
Evaluation of AC, in pediatric cases, depends not only on clinical symptoms but also on imaging exams. Cranial MRI offer superior diagnostic and surveillance information compared with CT, by revealing the position of cysts as well as CSF characteristics and the relationship between cyst, arachnoid cisterns and brain tissue.9
Size does not correlate precisely with symptoms or the need for treatment.10 Treatment depends on whether the cysts are symptomatic or not. Despite the surgical risk associated, many authors agree that symptomatic AC should be operated.3,4
In patients with cysts discovered fortuitously or causing mild symptoms conservative management is the preferred approach.3
Surgical treatment includes craniotomy for partial or complete microsurgical cystectomy with large fenestration of the cyst wall to create a communication between the cyst and subarachnoid space within the basal cisterns; this communication port can be achieved also by portal trephine with minimal invasive neuroendoscopy, or with cyst peritoneal shunting (CPS).3 Some studies indicate that temporal uniportal endoscopic fenestration is a superior approach to treat temporal AC, with good efficacy and a lower risk of surgical complications. Endoscopic surgery avoids the risk of open surgery like the shunt disease associated with CPS.4
We report this case due to the unusual large size of the cyst associated with nonclassical clinical manifestations. Ophthalmological evaluation in children with intracranial cysts is mandatory to early screening of associated complications. Clinical surveillance with early recognition of warning signs and regular imaging of larger cysts are essential due to their greater propensity to ruptures in the subarachnoid space (causing hygromas or hemorrhage), occurring spontaneously or associated with cranial trauma.
Learning Points:
• Arachnoid cysts (AC) are fluid-filled malformations of the arachnoid tissue
• Acquired sixth nerve palsy may be a rare manifestation of AC
• Symptomatic arachnoid cysts should be treated surgically
• An early ophthalmological assessment, in children with intracranial cysts, seems to be indispensable to exclude papilledema and other associated complications
• Early brain imaging is mandatory in the presence of poorly understood ophthalmologic signs/symptoms, papillary edema, or ICH
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Mondal T, Kumar KJ, Anand R, Dubey NK, Sharma D. Large arachnoid cyst. Indian pediatrics. 1995;32(8):927-929. doi:10.1056/nejmicm1610483 [CrossRef] [PubMed]
- Rajesh A, Pelluru P. Enigmatic intracranial cyst causing diplopia and trigeminal neuralgia. Asian Journal of Neurosurgery. 2015;10(4):316. doi:10.4103/1793-5482.162717 [CrossRef] [PubMed] [PMC free article]
- Wild K von. Arachnoid cysts of the middle cranial fossa. Neurochirurgia. 1992;13(6):317-320. doi:10.3109/01658109309044580 [CrossRef]
- Mustansir F, Bashir S, Darbar A. Management of Arachnoid Cysts: A Comprehensive Review. Cureus. 2018;10(4). doi:10.7759/cureus.2458 [CrossRef] [PubMed] [PMC free article]
- Al-Holou WN, Yew AY, Boomsaad ZE, Garton HJL, Muraszko KM, Maher CO. Prevalence and natural history of arachnoid cysts in children: Clinical article. Journal of Neurosurgery: Pediatrics. 2010;5(6):578-585. doi:10.3171/2010.2.PEDS09464 [CrossRef] [PubMed]
- Mazurkiewicz-Beldzińska M, Dilling-Ostrowska E. Presentation of intracranial arachnoid cysts in children: Correlation between localization and clinical symptoms. Medical Science Monitor. 2002;8(6):462-466.
- Huang JH, Mei WZ, Chen Y, Chen JW, Lin ZX. Analysis on clinical characteristics of intracranial Arachnoid Cysts in 488 pediatric cases. International Journal of Clinical and Experimental Medicine. 2015;8(10):18343-18350.
- Eidlitz-Markus T, Zeharia A, Cohen YH, Konen O. Characteristics and management of arachnoid cyst in the pediatric headache clinic setting. Headache. 2014;54(10):1583-1590. doi:10.1111/head.12470 [CrossRef] [PubMed]
- Rezaee O, Ebrahimzadeh K, Maloumeh E, Jafari A, Shafizad M, Hallajnejad M. Prepontine arachnoid cyst presenting with headache and diplopia: A case report study. Surgical Neurology International. 2017;8(1). doi:10.4103/sni.sni_247_17 [CrossRef] [PubMed] [PMC free article]
DOI: https://doi.org/10.7199/ped.oncall.2023.5
|
| Cite this article as: | | Rebelo A T, Martins A I, Rodrigues S, Pereira J, Aires S. Huge Arachnoid Cyst Presented with Bilateral Sixth Cranial Nerve Palsy. Pediatr Oncall J. 2023;20: 17-19. doi: 10.7199/ped.oncall.2023.5 |
|