Jeannette Epée Ngoué1, Suzanne Sap Ngo Um1,2, Jocelyn Tony Nengom1,2, Isabelle Mekone Nkwele1,2, Hélène Kamo Doka3, Madeleine Onguene Ngambi1, Emilienne Epée1, Hubert Désiré Mbassi Awa1,2.
1Faculty of Medicine and Biomedical Sciences of the University of Yaoundé I, Cameroon,
2Mother and Child Centre of the Chantal Biya Foundation, Yaoundé, Cameroon,
3Faculty of Medicine and Biomedical Sciences University of Ngaoundéré, Cameroon.
ADDRESS FOR CORRESPONDENCE
Jeannette Epée Ngoué, Departement of Paediatrics, Faculty of Medicine and Biomedical Sciences of the University of Yaoundé I. Cameroon.
Email: jngoue@yahoo.com | | Abstract | Introduction: Neurological distress is life-threatening in most cases. Specific data on neurological pediatric emergencies in our environment are rare. We aim to describe the incidence and pattern of pediatric neurological emergencies.
Patients and method: This was a descriptive cross-sectional study conducted at the Mother and Child Center of the Chantal Biya Foundation in Yaounde. We collected data from the registers of emergency room admission during the year 2020. Any child aged 0 to 18 years who presented with neurological distress main complaint was included.
Results: A total of 5998 children were received in the emergency department during 2020, of which 640(10.1%) were for neurological distress, the average age was 46±6 months with extremes of 1 day and 18 years. The sex ratio was 1.2. The main neurological symptoms that motivated the need of emergency care were convulsions (77.8%), consciousness disorders (8.9%), and behavioural disorders (6.8%). The most frequent diseases were: severe malaria (32.0%), meningitis, and meningoencephalitis (30.8%). The main comorbidities were cerebral palsy (0.9%), sickle cell disease (2.19%), diabetes (0.5%) and hydrocephalus (0.5%).
Conclusion: This study clearly shows that neurological distress is a frequent reason for admission to the Mother and Child Center of the Chantal Biya Foundation emergency room. Their knowledge allows to anticipate and to improve the care offer. | | | | Keywords | | Neurological emergency, child, Mother and Child Center, emergency room | | | | Introduction | | Neuroemergencies are life-threatening situations in which, whatever the cause, common pathologic phenomena result in secondary brain lesions1. In children, there are many situations that can lead to neurological distress. The diseases encountered are very wide-ranging and are likely to result in significant morbidity and mortality. Data concerning the pattern of neurological distress in pediatric emergencies in our environment are scarce. Hence the interest of this study to determine the incidence and nosological framework of these disorders in pediatric emergencies. | | | | Methods & Materials | We conducted a descriptive cross-sectional study with a retrospective collection of data at the Mother and Child Center of the Chantal Biya Foundation (MCC/CBF), which is one of the oldest pediatric referral centre in Yaounde, capital of Cameroon where children are referred from even other cities of country. After obtaining administrative and ethical approvals, we examined the admission records. The sampling was consecutive.
We collected data on age, sex, place of residence, reason for consultation, diagnosis made, co-morbidities and destination after the emergency department. We included children aged 0 to 18 years who were received in the emergency room from January 1 to December 31, 2020, for a neurological disorder expressed as the main complain. The neurological disorders sought in the registry were plural. The disorders of consciousness were defined as a more or less complete abolition of the functions of the life of relationship ranging from simple confusion to coma.2 The convulsions corresponded to sudden and involuntary muscular contractions, related to the excitation of a more or less important group of neurons.2 Complaints described as feelings of numbness, tingling, electric shock, burning, a feeling of runoff or tightness, pain from touching an object and difficulty discerning hot from cold were listed as sensory disturbances. Balance disorders included vertigo defined as the feeling by which a person believes that he and herself and surrounding objects are in a circular or oscillating motion and may even fall due to loss of balance.3 Agitation defined as increased and maladaptive motor activity was classified as behavioral disturbance.3 We noted delirium when the child said or perceived things that were inconsistent with reality or the obvious.3
The reason for consultation corresponded to the main complaint declared by the carer. The diagnosis retained was the one that the consultant entered in the register after the consultation. Positive diagnoses were possible in the emergency room for malaria through the rapid diagnostic test, meningitis through cytological examination and Gram stain of cerebrospinal fluid and hypoglycaemia on the basis of a blood glucose strip.
The living quarters were classified in three groups according to the distance travelled to reach the MCC as a distance of less than 10 km, the outskirts for more than 10 km and outside the city for the other cities of the country.
The data were entered in the CSPro software version 23.0 and analyzed in the Epi Info 7.0 software. The results are presented as means and medians for the quantitative variables and as a percentage for the qualitative variables.
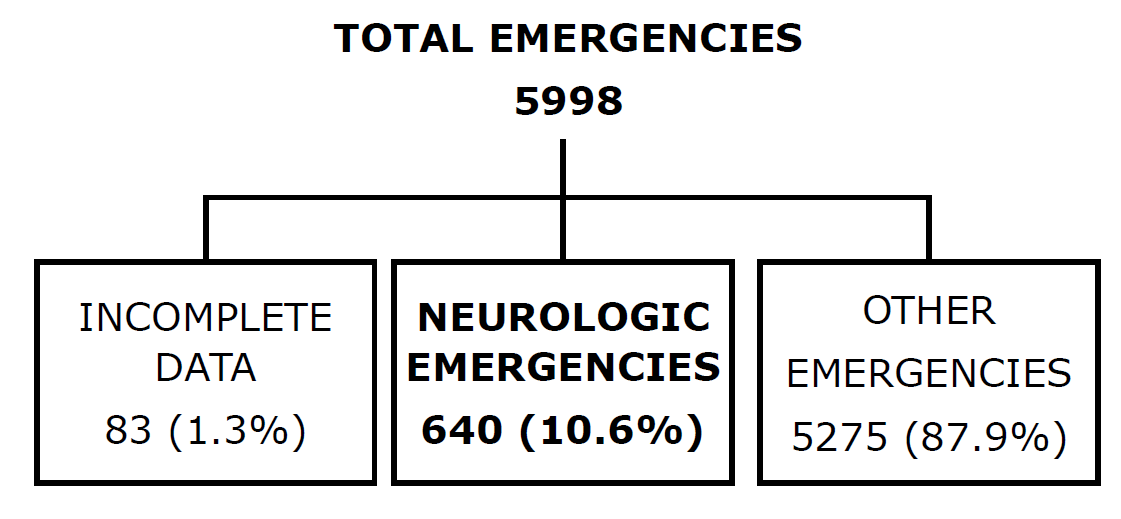
| | | | Results | Out of 5998 cases received in the emergency room during 2020, we acknowledged 640 cases of neurological distress, a frequency of 10.6% (Figure 1). The maximum neurological distress was recorded in August.
Figure 1. Incidence of neurological emergencies.
Almost half (46.4%) of the patients were from the outskirts of the city, the other half from the City center (46.1%), and a minority (7.5%) from other cities.
The average age of the children brought in for neurological distress was 46±6 months with extremes of 1 day and 18 years, the most represented age group being that of 24-60 months with 57.8%. We had a male predominance with a sex ratio equal to 1.2. (Table 1)
Table 1. Distribution of patients by age group and sex.
| Age (months) |
Female [n(%)] |
Male [n(%)] |
| [0-1] |
20 (6.9) |
17 (4.8) |
| [1-6] |
13 (4.5) |
20 (5.7) |
| [6-12] |
29 (10.1) |
36 (10.2) |
| [12-24] |
51 (17.7) |
71 (20.2) |
| [24-60] |
82 (28.5) |
103 (29.3) |
| [60-120] |
56 (19.4) |
70 (19.9) |
| [120-180] |
32 (11.1) |
26 (7.4) |
| [180-216] |
5 (1.7) |
8 (2.3) |
| Total |
288 (100.0) |
352 (100.0) |
Seizures led the way with 498 cases (77.8%). The age group most affected by seizures was 12-60 months (52.4%). They were associated with fever in 80% of cases. After the convulsions, consciousness disorders followed in 57 cases (8.9%) including coma (4.1%), drowsiness (4.8%). Behavioral disorders occurred in 39 cases (6.1%) marked by restlessness and abnormal movements. Tonal disturbances were noted in 11 cases (0.7%) (Table 2).
Table 2. Frequency of neurological emergencies symptoms.
| Symptoms |
Number of patients (n) |
Frequency (%) |
| Convulsive disorders |
Convulsion |
498 |
77.8 |
| Consciousness disorders |
Coma |
26 |
4.1 |
| drowsiness, confusion |
31 |
4.8 |
| Tone disturbances |
Tone disorder |
11 |
0.7 |
| Behavior disorders |
Agitation |
23 |
3.6 |
| Abnormal Movements |
16 |
2.5 |
| Balance disorders |
Dizzines |
1 |
0.2 |
| Loss of equilibrium |
1 |
0.2 |
| Motor deficit disorders |
Tétraparésis |
1 |
0.2 |
| Hémiparésis |
6 |
0.9 |
| Facial Paralysis |
1 |
0.2 |
| Sensory disorders |
Lost of sensivity |
1 |
0.2 |
| Others |
Pupillary abnormalities |
1 |
0.2 |
The diseases diagnosed were: severe malaria 205 cases (32%), meningitis and encephalitis 197 cases (30.8%), metabolic disorders 35 cases (5.5%), sepsis 29 cases (4.5% ) (Table 3).
Table 3. Frequency of primary diagnosis.
| Primary Diagnosis |
Number (n) |
Frequency (%) |
| Severe malaria |
205 |
32.0 |
| Méningitis et encéphalitis |
197 |
30.8 |
| Métabolic disorders |
35 |
5.5 |
| Epilepsy |
34 |
5.3 |
| Sepsis |
29 |
4.5 |
| Néonatal Infections |
25 |
3.9 |
| Fébrile seizures |
22 |
3.4 |
| Stroke |
11 |
1.7 |
| Traumatismes crâniens |
11 |
1.7 |
| Acute Flaccid Paralysis |
8 |
1.2 |
| Poisoning |
8 |
1.2 |
| Périnatal Asphyxia |
4 |
0.6 |
| Psychosomatic disorders |
4 |
0.6 |
| Functional gastrointestinal disorders |
4 |
0.6 |
| Brain tumors |
3 |
0.5 |
| Tétanus |
2 |
0.3 |
| Brain Abcess |
1 |
0.2 |
The most reported underlying pathologies were: cerebral palsy 6 cases (0.9%), sickle cell disease 14 cases (2.19%), diabetes 3 cases (0.5%), hydrocephalus 3 case (0.5%), malignant hemopathy 1 case (0.2%), nephrotic syndrome 1 case (0.2%).
Seven deaths (1.1%) were recorded on admission, the other 633 (98.9%) were admitted to different units of the center.
| | | | Discussion | The objective of this study was to determine the frequency of neurological emergencies as well as their profile. As the method used is limited to consulting the admission registers, we may find some limitations regarding the confirmation of the diagnosis mentioned. This does not affect the relevance of our results since studies have shown a diagnostic concordance of over 93%.4 In addition, certain data such as consultation time and treatment itinerary were not available as is customary in retrospective collections.
This study showed that neurological emergencies are frequent at CME/FCB. The symptoms are dominated by convulsions and disturbances of consciousness. The corresponding diseases are severe malaria and meningitis/encephalitis.
Neurological distress is frequent in MCC /CBF emergencies. We found a frequency of 10.6% which is close to that found in similar work by Penda in Cameroon and SO in Nigeria, which identified 11.0% and 11.1% respectively of neurological emergencies.5,6 They differ from those of Albertini et al in France who find 2.5% neurological emergencies in children.7
We observed a drastic drop in attendance in April and July, this is due to the covid19 pandemic and associated restrictions. This was also the case for "real" emergencies which unfortunately came too late. This fact was documented by Chelo et al, who in a recent study documented a drastic drop in hospitalizations coinciding with confinement in Cameroon and at the same time an increase in the number of deaths.8
More than half of the patients were from the outskirts of town probably because the MCC/CBF has forged a great reputation for decades given its central geographical position and the populations settled on the outskirts of the city still prefer to use it for emergency care. The low cost of services also contributes to increasing attendance in this center.
The predominance of the 0 to 5 year age group has also been noted in several studies.9 It testifies to the vulnerability of this group whose mortality remains high in Cameroon, with a rate of 80 per 1000 live births.10 Efforts remain to be made to reduce under-5 mortality to 25 per 1000 live births as formulated in the Development Goals by 2030. Seizures come first in most studies of paediatric emergencies like ours.7,11 In 2010, Nguefack et al, found that the majority of febrile seizures occured at the average age of two months, with a peak in frequency between 12 and 17 months. A relationship between age, degree of cerebral maturation and fever has been established: there is an age-related neuronal hyperexcitability induced by fever in an immature brain.12,13
Disorders of consciousness were frequent in our series. Another author, in a similar study finds convulsions and headaches in the lead.7 We did not have a significant proportion of headaches in our sample. This contrasts with the data of some authors.11 As self-medication has free rein in our environment, headaches are often calmed with first-level analgesics while waiting for an elective consultation. Likewise, we believe parents rush to the emergency room for perceived emergencies, since the headaches are not spectacular compared to the seizures or a motor or sensory deficit that would immediately worry them.
In terms of emergency room diagnoses, severe malaria, meningitis and sepsis came first. This result is not surprising because these infectious pathologies that are still dangerously rampant and fatal in our tropical environment. These data agree with those obtained in Nigeria by Fe et al in 2005 which revealed 32% of cases of cerebral malaria in pediatric emergencies, responsible for 17.8% of deaths. In the same study, the most common (82.2%) severity endpoint was seizures.14 Equally, Nzame in Gabon reported severe malaria as the most frequent paediatric emergency constituting 65.8% of all recorded emergencies.15
Regarding the outcome, in our series, apart from the deaths in the emergency room, all of our patients were hospitalized. This is the opposite of the SO’s series, where 37.7% were sent home while 7.7% died. This contrast could be explained by the high frequency of febrile convulsions, which was the second most common pathology in this study.16 Indeed, febrile convulsion in itself is not life-threatening if properly managed and after adequate observation and identification of underlying cause patient can be sent home with a consequent prescription.17
Our low death rate could be linked to the speed of the immediate responsible measures by taken experienced team. However, maximum number of deaths can subsequently occur in hospital wards. Ofovwe, in his study investigated the follow-up and found precisely 15.8% of deaths of children admitted for neurological diseases of which more than half (67.2%) occurred within 24 hours of admission9; as well as Tshimangani in Congo, whose cohort study during 12 months revealed an overall mortality of 21%.17
| | | | Conclusion | | This study clearly shows that neurological distress is a frequent reason for admission to the CME / FCB emergency room. More than one in ten children admitted to paediatric emergency departments present with a neurological emergency. Convulsions are the most frequent symptom. The aetiologies are dominated by infectious diseases. Their knowledge makes it possible to anticipate and improve the offer of care. Thus the ward should be equipped for the rapid management of convulsions. Malaria and meningitis prevention should be strengthened. | | | | Acknowledgement | | We thank the staff of the MCC/CBF for their support in this work. | | | | Authors Contribution | | SSN and JEN designed this work. JEN, JTN, IMN, and MON contributed for data collection and analysis, JEN and HKD wrote the draft manuscript. SSN, EE and HDM contributed in proofreading the manuscript. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Meyer G, Ducrocq S, Carli P. Pediatric neurologic emergencies. Curr. Opin. Crit. Care. 2001;7(2),81-87. doi:10.1097/00075198-200104000-00005 [CrossRef] [PubMed]
- Manuel MSD https://www.msdmanuals.com/fr/professional/Pédiatrie/troubles-neurologiques-chez-enfant consulted on 23th November 2021.
- Chabrol Brigitte. Neurologie pédiatrique. 3e édition. Paris: Éd. Lavoisier Médecine-sciences Flammarion, 2010. Print.
- De Gusmão CM, Guerriero RM, Bernson-Leung ME, et al. Functional neurological symptom disorders in a pediatric emergency room: diagnostic accuracy, features, and outcome. Pediatr Neurol. 2014;51(2):233-238. doi:10.1016/j.pediatrneurol.2014.04.009 [CrossRef] [PubMed]
- So I. Paediatric neurologic emergencies at the University of Nigeria Teaching Hospital, Enugu. West Afr J Med. 1997;16(2):80-4.
- Ida P., Mireille-Laurent E, Francine S, Lariale, M, Charlotte E , Bertrand, E. et al. Epidemiological Profile of Pediatric Vital Emergencies at Laquintinie Hospital of Douala, Cameroon. Open J. Pediatr. 2021;11(01):148-160. [CrossRef]
- Albertini F, Bresson V, Tardieu S, Milh M, Chabrol B. Pediatric emergency room visits for neurological conditions: Description and use of pediatric neurologist advice. Arch Pediatr . 2020;27(8):416-422 [CrossRef] [PubMed]
- Chelo D, Mekone I, Nguefack F, Mbassi HD, Enyama D, Nguefack S et al. Decrease in Hospitalizations and Increase in Deaths during the Covid-19 Epidemic in a Pediatric Hospital, Yaounde Cameroon and Prediction for the Coming Months. Fetal Pediatr. 2021;40(1):18-31 https://doi.org/10.1080/15513815.2020.1831664 [CrossRef] [PubMed]
- Ofovwe G, Ibadin M, Okunola P, Ofoegbu B. Pattern of emergency neurologic morbidities in children. J Natl Med Assoc. 2005;97(4):488
- Institut National de la Statistique (INS) and ICF. Enquête Démographique et de Santé du Cameroun 2018. Yaoundé, Cameroun et Rockville, Maryland, USA
- Personnic J, Titomanlio L, Auvin S, Dozières-Puyrave B. Neurological disorders encountered in a paediatric emergency department. Eur. J. Paediatr. Neurol.2021;32:86-92. [CrossRef] [PubMed]
- Nguefack S, Ngo Kana CA, Mah E, Kuate Tegueu C, Chiabi A, Fru F, et al. Clinical, etiological and therapeutic aspects of febrile convulsions. About 325 cases in Yaounde »[traduction]. Arch Pediatr, 2010;17(5):480-5 [CrossRef] [PubMed]
- Jensen A T, Sanchez R M. Why does the developing brain demonstrate heightened susceptibility to febrile and other provoked seizures? In: Febrile seizures. Academic Press 2002;153-68 [CrossRef]
- Fe L, Nwosu SU, Mafe AG, Egri-Okwaji MT. Pattern of cerebral malaria in children at the Lagos University Teaching Hospital. Niger. Postgrad. Med. J.2005;12(4):275-279 .
- Nzame Y, Ntsame S, Ndoutoume R, Gahouma D, Koko J. Épidémiologie des Urgences Pédiatriques de Nuit au Centre Hospitalier Universitaire de Libreville Health Sci. Dis. 2020 Apr;21(4):88-91
- JO Obi, NA Ejeheri, W Alakija. Childhood febrile seizures (Benin City experience). Ann Trop Paediatr. 1994;14(3):211-4. [CrossRef] [PubMed]
- Tshimangani T, Pongo J, Bodi Mabiala J, Yotebieng M, O'Brien NF. Pediatric Acute Severe Neurologic Illness and Injury in an Urban and a Rural Hospital in the Democratic Republic of the Congo. Am J Trop Med Hyg. 2018;98(5):1534-1540. doi:10.4269/ajtmh.17-0784 [CrossRef] [PubMed] [PMC free article]
DOI: https://doi.org/10.7199/ped.oncall.2022.47
|
| Cite this article as: | | Ngoué J E, Um S S N, Nengom J T, Nkwele I M, Doka H K, Ngambi M O, Epée E, Awa H D M. Incidence and pattern of neurologic emergencies in children at the mother and child center of the chantal biya foundation. Pediatr Oncall J. 2022;19: 114-117. doi: 10.7199/ped.oncall.2022.47 |
|