|
Complex regional pain syndrome in the pediatric emergency
Joana Rita da Silva Gonçalves, Catarina Rocha de Albuquerque, Ana Sofia Ferreira Lança, Paula Alexandra Simão Nunes.
Pediatric Department, Hospital de São Francisco Xavier, Centro Hospitalar de Lisboa Ocidental, Lisbon, Portugal.
ADDRESS FOR CORRESPONDENCE
Dr. Joana Goncalves, Estrada Forte do Alto Duque, 1449-005, Lisboa, Portugal.
Email: joanarsgoncalves@gmail.com
Adolescent, Chronic pain, Complex regional pain syndrome, Trauma
A 17-year-old girl presented to the emergency department with two weeks of severe pain and swelling of the right foot and ankle. Of her previous medical history, anxiety disorder was of notice. Two months back she had an acute right ankle sprain. For which she was observed at the emergency room, ankle radiography was performed showing no abnormalities and RICE (rest, ice, compression, elevation) therapy was recommended. After this minor trauma and despite RICE therapy, there was a progressive worsening of the symptoms. She complained of load-dependent pain and swelling of the right foot and ankle, that progressed into permanent allodynia, hyperalgesia (9 points in numeric pain rating scale), change of skin colour and temperature of that region which was now blueish and cold respectively. She could not bear weight on the affected leg. On physical examination she presented with oedema, cyanosis and lower temperature of the right foot and ankle, associated with tenderness on palpation, decreased and painful range of motion in the affected joint (Figure 1). Hyperalgesia and allodynia were also present. This raised concerns regarding a possible vascular complication but Homan´s sign was negative, pulses were palpable and a doppler ultrasound was performed, ruling out that possibility. No other abnormalities were present on physical examination, including trophic changes, motor disturbances, or neurological deficits. Radiography of her foot and ankle was performed showing signs suggestive of osteopenia of the right heel (Figure 2).
Figure 1. Patient’s right foot and ankle presenting with cyanosis and oedema, in contrast with normal left foot.
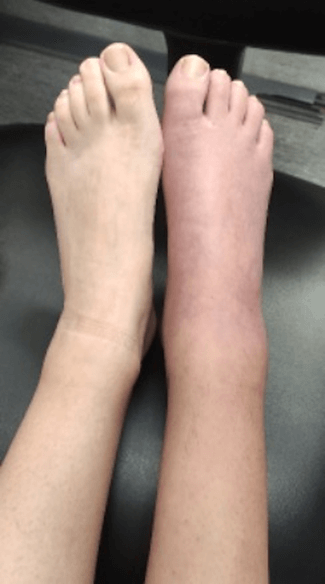
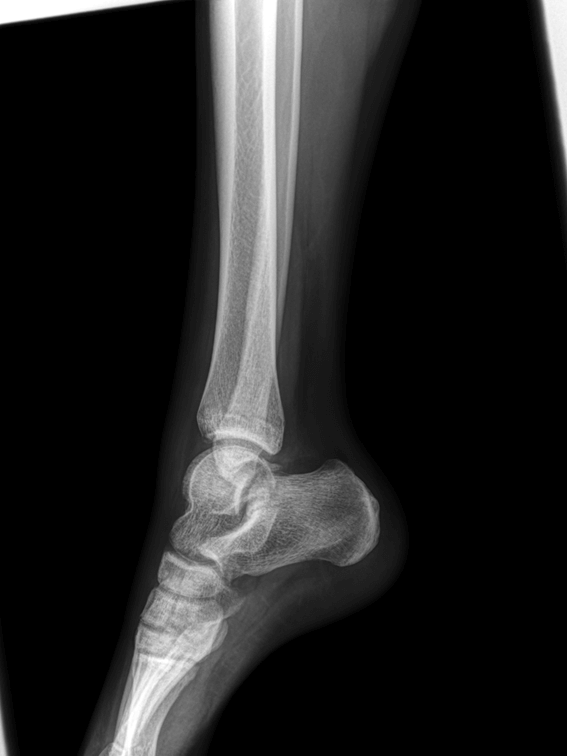
Figure 2. Radiography showing signs suggestive of osteopenia of the right heel.
|
Figure 1. Patient’s right foot and ankle presenting with cyanosis and oedema, in contrast with normal left foot
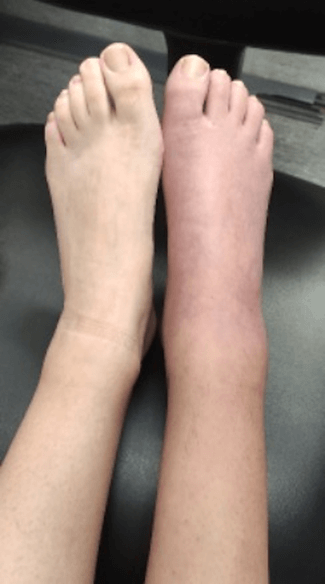
|
What is the diagnosis?
After a thorough anamnesis and physical examination excluding another diagnosis and in the face of a stimuli-induced chronic peripheral pain of a distal extremity, disproportionate to the actual incident trauma, concurrent with autonomic and motor disturbances, complex regional pain syndrome type I was diagnosed according to Budapest clinical diagnostic criteria. The osteopenia was attributed to the long period of immobilization.
She started intensive physical therapy and pregabalin was initiated at a dose of 150 mg twice a day for pain control. Active surveillance was continued at the outpatient clinic. The pain, monitored with a numeric pain rating scale, progressively reduced and so did the other signs and symptoms. Within 3 months there was a complete resolution of all symptoms.
Complex regional pain syndrome (CRPS) is a chronic painful condition affecting one part of the body usually of a distal extremity. More frequently is stimuli-induced, usually after minor trauma but it can also be spontaneous. The pain is characteristically disproportionate to the severity of the injury. Two subtypes are described: CRPS type 1, without nerve injury and CRPS type 2 associated with nerve injury. In the paediatric population, CRPS type 1 is more frequent. Teenage girls are the most affected group mostly of white ethnicity and the mean age at diagnosis is around 12 years of age.1,2
The pathophysiology is not fully understood. However, multiple peripherical and central mechanism seems to be involved that includes: microvascular disease related to ischemic reperfusion injury and activation of both classic and neurogenic inflammation contributing to local inflammatory signs and symptoms; upregulation of sympathetic nervous system and nociceptive sensitization through activation of adrenergic receptor leading to higher sensitivity to circulating catecholamines and increasing response to pain and nociceptive fibres that amplifies the pain. There are some contributing factors to the persistence of pain namely altered somatosensory representation, genetic polymorphisms, psychosocial aspects, stress and anxiety, particularly in the paediatric population.1,3,5
Regarding treatment, a multidisciplinary approach is suggested, which includes intensive physical therapy daily for at least 4 weeks combined with occupational and cognitive-behavioural therapy to develop strategies of coping with pain and desensitization. In selected patients, adjuvant pharmacological interventions with paracetamol, non-steroid anti-inflammatory drugs, antidepressants (amitriptyline) and anticonvulsants (gabapentin) are suitable for pain control in the acute setting, in order to facilitate physical therapy.1, 3,6,7,8 It is expected that with appropriate treatment most of the children will have full resolution of the symptoms within 6 months of treatment. Nevertheless, relapses can occur mainly in the first months after therapy.1
We aim to raise the clinician’s awareness of this syndrome, as prompt diagnosis and initiation of physical therapy along with pharmacological intervention can lead to a faster resolution of symptoms, as was observed in our case. |
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
|
- Weissmann R, Uziel Y. Pediatric complex regional pain syndrome: A review. Pediatric Rheumatology; 14. Epub ahead of print April 29, 2016. DOI: 10.1186/s12969-016-0090-8. [CrossRef] [PubMed] [PMC free article]
- Katholi BR, Daghstani SS, Banez GA, et al. Noninvasive treatments for pediatric complex regional pain syndrome: A focused review. PM and R 2014; 6: 926-933. [CrossRef] [PubMed]
- Bruehl S. Complex regional pain syndrome. BMJ (Online); 351. Epub ahead of print July 29, 2015. DOI: 10.1136/bmj.h2730. [CrossRef] [PubMed]
- Eldufani J, Elahmer N, Blaise G. A medical mystery of complex regional pain syndrome. Heliyon; 6. Epub ahead of print February 1, 2020. DOI: 10.1016/j.heliyon.2020.e03329. [CrossRef] [PubMed] [PMC free article]
- Harris EJ, Schimka KE, Carlson RM. Complex Regional Pain Syndrome of the Pediatric Lower Extremity A Retrospective Review.
- Mesaroli G, Ruskin D, Campbell F, et al. Clinical Features of Pediatric Complex Regional Pain Syndrome: A 5-Year Retrospective Chart Review. Clinical Journal of Pain 2019; 35: 933-940. [CrossRef] [PubMed]
- Lascombes P, Mamie C. Complex regional pain syndrome type I in children: What is new? Orthopaedics and Traumatology: Surgery and Research 2017; 103: S135-S142. [CrossRef] [PubMed]
- Vescio A, Testa G, Culmone A, et al. Treatment of complex regional pain syndrome in children and adolescents: A structured literature scoping review. Children; 7. Epub ahead of print November 1, 2020. DOI: 10.3390/children7110245. [CrossRef] [PubMed] [PMC free article]
|
|
DOI: https://doi.org/10.7199/ped.oncall.2024.1 |
| |
Cite this article as:
Gonçalves J R d S, Albuquerque C R d, Lança A S F, Nunes P A S. Complex regional pain syndrome in the pediatric emergency. Pediatr Oncall J. 2024;21: 39-40. doi: 10.7199/ped.oncall.2024.1
|