Madalena Pereira de Sousa von Hafe Pérez1, Débora Valente Silva1, Georgeta Maria Costa Alves de Oliveira2.
1Pediatrics Department of Centro Hospitalar Universitário de São João, Oporto, Portugal,
2Pediatrics Department of Hospital Pedro Hispano, Oporto, Portugal.
ADDRESS FOR CORRESPONDENCE
Alameda Prof. Hernâni Monteiro, Porto, 4200-319 Oporto, Portugal.
Email: madalenavonhafe@gmail.com. | | Abstract | A 23-month-old healthy boy presented to the emergency department with a purpuric rash, fever and edema of the extremities. There were no recent vaccinations or drug intake. The skin showed round purpuric lesions dispersed. Complete blood count, inflammatory markers, plasma creatinine and urea levels, coagulation tests and urinalysis were normal.
Different differential diagnoses can be listed and different approaches should be considered depending on the diagnosis. Some of these require urgent medical attention and may be life-threatening.
This case reports a typical presentation of acute hemorrhagic edema in infancy, with very peculiar and detailed images of the skin that also show edema of the extremities. This case report aimed to explore this worrisome rash that has a benign course to alert pediatricians with different purpura diagnoses. The authors believe that the images presented are unique and might increase knowledge about the variety of cutaneous presentations of this under-recognized disease. | | | | Keywords | | Purpura, acute hemorrhagic edema, vasculitis. | | | | Case Report | A 23-month-old healthy boy, who had completed the National Vaccination Program and had no documented allergies, was brought to the emergency department with a purpuric rash that had developed over the past 24 hours. He also experienced swelling of both hands and feet. The day before, he had a fever of 38.3 °C, but at the time of admission, he had been without fever for 20 h. The patient did not report abdominal pain, diarrhea, vomiting or other symptoms. There were no recent vaccinations or medication intakes. The mother mentioned that the boy had an upper respiratory viral infection one week prior, which did not require medical attention.
Upon admission, the patient's vital signs were stable, with a temperature of 36.2°C, blood pressure within the 50th percentile range, respiratory rate of 22 breaths per minute and heart rate of 87 beats per minute. The patient appeared well and underwent a normal neurological examination. The skin exhibited dispersed round purpuric lesions in various areas, including the face and the left auricle (See Figures 1, 2, 3). Mild swelling was observed in the hands, ears and feet, without skin induration, joint swelling or tenderness. No other significant findings were noted during physical examination. Complete blood count, inflammatory markers, plasma creatinine and urea levels, coagulation tests and urinalysis yielded normal results.
During the stay in the emergency department, he remained without fever and was hemodynamically stable. He was discharged with a diagnosis of acute hemorrhagic edema of infancy (AHEI) and advised a follow-up appointment in the near future. Upon re-evaluation, the patient remained asymptomatic, apart from the presence of a purpuric rash. No new lesions appeared and the urinalysis and blood pressure remained normal. The rash completely resolved within two weeks.
Figure 1. Large, annular purpuric lesions on the leg.
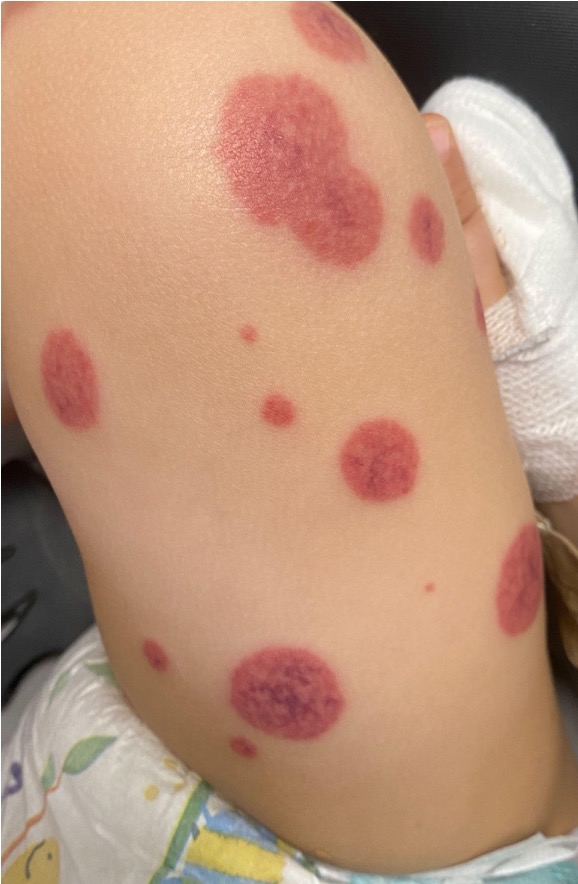
Figure 2. Large, annular, and target-shaped purpuric lesions on both legs and feet edema.
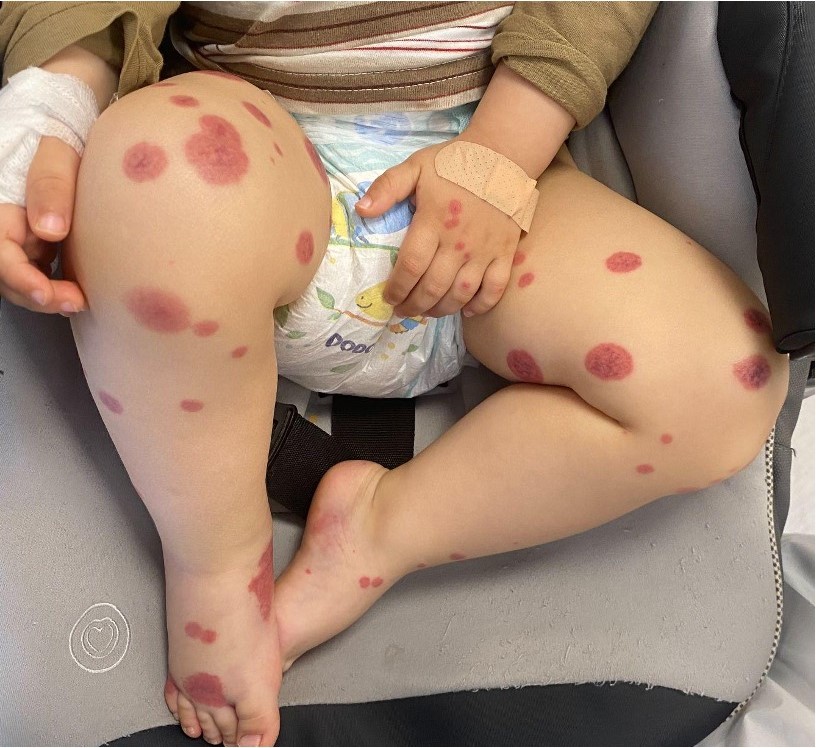
Figure 3. Ecchymosis and swelling of the left ear.
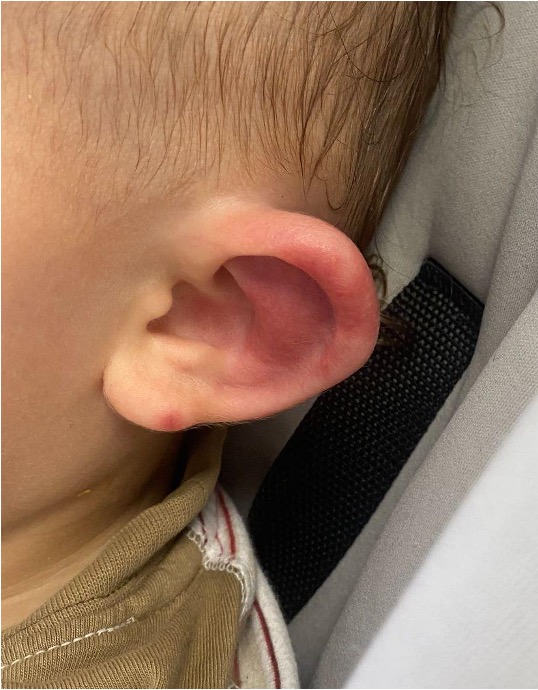
| | | | Discussion | AIHE, also known as Seidlmayer purpura, is a rare leukocytoclastic vasculitis that is associated with fever in pediatricians. Despite its acute onset, it follows a benign course, typically resolving spontaneously within approximately three weeks.1 This vasculitis affects predominantly males between the ages of 3 months and 2 years. The classic presentation includes fever; edema of the extremities; and large, annular or target-shaped palpable purpuric lesions, commonly involving the face, ears and extremities. Although patients typically have non-toxic appearance, clinical presentation often makes it challenging to differentiate AIHE from Henoch-Schönlein Purpura (HSP), with some authors considering AIHE as a cutaneous variant of HSP, although multiorgan involvement is less frequent in AIHE.2,3 AIHE tends to affect younger patients compared to HSP and the rash in AIHE is almost always present on the face and ears, while HSP predominantly affects gravity-dependent areas (legs and buttocks) and is smaller in size.3
Clinicians should consider other important differential diagnoses in cases of purpura with fever, such as purpura fulminans, meningococcemia, Sweet syndrome, erythema multiforme and other coagulopathies, owing to their severity and the need for urgent treatment. These conditions are often distinguished from AIHE by the toxic appearance of the patient and elevated serum inflammatory markers.4 Krause and colleagues have proposed clinical criteria for diagnosing AIHE, including age under 2 years, purpuric or ecchymotic target-like skin lesions with edema on the head and face, with or without mucosal involvement, absence of visceral involvement and spontaneous recovery within a few days or weeks.5
One of the most widely accepted pathophysiological explanations for AIHE is an immune complex hypersensitivity mechanism, as various viruses, bacteria, vaccines and drugs are frequent triggers.4 As seen in this case, the occurrence of a previous upper respiratory infection one week before. The most commonly implicated microorganisms include adenovirus, cytomegalovirus, herpes simplex virus, tuberculosis, streptococci and staphylococci.1 Similar to other vasculitides, extracutaneous involvement can occur in AIHE, although it is less frequent compared to HSP. Gastrointestinal and renal involvement are the most commonly affected organs.6
The diagnosis of AIHE is typically based on the clinical presentation, although blood samples are usually obtained. Although mild thrombocytosis or leukocytosis may occur, a complete blood count is often nonspecific. Inflammatory markers are typically within the normal range; although there may be a slight elevation in C-reactive protein and erythrocyte sedimentation rate.7 Hypocomplementemia affecting complement C4, complement C1q and complement CH50 may be present but is not necessary for the diagnosis.8 Skin biopsy is not required for diagnosis, but it may be necessary when the diagnosis is unclear. Histologically, AIHE is characterized by perivascular neutrophilic infiltration with fibrinoid necrosis. Skin biopsy can be useful in differentiating AIHE from HSP, as IgA deposits are frequent in the latter.6
The treatment of AIHE remains controversial and the use of steroids or other therapies does not alter the course of the disease. In fact, AIHE is a self-limiting condition and some authors suggest considering steroids when there is significant systemic involvement, similar to the approach taken in HSP.3 Recurrence of AIHE is rare; however, it is crucial to conduct regular follow-up until the rash has completely resolved and to exclude any potential visceral involvement. Monitoring the patient's progress ensures proper management and helps to rule out any complications that may arise during the disease.
| | | | Conclusion | | Although there are few case reports of AHEI in the literature, the authors of this study consider the presented images to be unique, contributing to a broader understanding of the diverse cutaneous presentations associated with this often under-recognized condition. It is crucial for pediatricians to develop the ability to recognize this self-limiting disease to prevent unnecessary procedures and therapies. By improving the awareness and knowledge of AHEI, healthcare professionals can provide more appropriate and efficient care to affected patients. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Fotis L, Nikorelou S, Lariou MS, Delis D, Stamoyannou L. Acute hemorrhagic edema of infancy: a frightening but benign disease. Clin Pediatr (Phila) 2012;51(4):391-3. DOI: 10.1177/0009922810396549. [CrossRef] [PubMed]
- Savino F, Lupica MM, Tarasco V, et al. Acute hemorrhagic edema of infancy: a troubling cutaneous presentation with a self-limiting course. Pediatr Dermatol 2013;30(6):e149-52. DOI: 10.1111/pde.12004. [CrossRef] [PubMed]
- Javidi Z, Maleki M, Mashayekhi V, Tayebi-Maybodi N, Nahidi Y. Acute hemorrhagic edema of infancy. Arch Iran Med 2008;11(1):103-6. (https://www.ncbi.nlm.nih.gov/pubmed/18154430).
- Roy KP, Madke B, Kar S, Yadav N. Acute Hemorrhagic Edema of Infancy. Indian J Dermatol 2015;60(6):624-5. DOI: 10.4103/0019-5154.169150. [CrossRef] [PubMed] [PMC free article]
- Krause I, Lazarov A, Rachmel A, et al. Acute haemorrhagic oedema of infancy, a benign variant of leucocytoclastic vasculitis. Acta Paediatr 1996;85(1):114-7. DOI: 10.1111/j.1651-2227.1996.tb13904.x. [CrossRef] [PubMed]
- Alhammadi AH, Adel A, Hendaus MA. Acute hemorrhagic edema of infancy: a worrisome presentation, but benign course. Clin Cosmet Investig Dermatol 2013;6:197-9. DOI: 10.2147/CCID.S51525. [CrossRef] [PubMed] [PMC free article]
- Arnold KA, Gao J, Stein SL. A review of cutaneous hypersensitivity reactions in infants: From common to concerning. Pediatr Dermatol 2019;36(3):274-282. DOI: 10.1111/pde.13827. [CrossRef] [PubMed] [PMC free article]
- Obeid M, Haley J, Crews J, Parhizgar R, Johnson L, Camp T. Acute hemorrhagic edema of infancy with abdominal pain and elevated transaminases. Pediatr Dermatol 2008;25(6):640-1. DOI: 10.1111/j.1525-1470.2008.00791.x. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2023.53
|
| Cite this article as: | | Pérez M P d S v H, Silva D V, Oliveira G M C A d. Acute onset of purpura and fever: A rare but benign etiology. Pediatr Oncall J. 2023;20: 146-148. doi: 10.7199/ped.oncall.2023.53 |
|