Amar Taksande, V Gouthami, Sumanta Padhi, Kinjal Bakshi.
Department of Pediatric Cardiology, Innova Children Heart Hospital And Research Centre, Hyderabad, India.
ADDRESS FOR CORRESPONDENCE
Dr. Amar Taksande, Innova Children Heart Hospital And Research Centre, White House, Tarnaka, Hyderabad, A.P. 500017, India.
Email: amar_bharti2000@yahoo.co.uk | | Keywords | | Aortopulmonary window, Congenital heart disease, Infant | | | A 3 month old male infant, weighing 4.6kg was referred for the assessment of a heart murmur. History of breathlessness, noisy breathing since last 2 months and not feeding well since last 3 days was present. He was a full-term delivery born by emergency caesarean section for non progression of labour. On physical examination, heart rate was 130/min, respiratory rate was 48/min, blood pressure was 106/62 mmHg and oxygen saturation was 92%. There was no respiratory distress. All the peripheral pulses were well felt. On auscultation, first and second heart sounds were present with P2 louder than A2. Third heart sound was present. Ejection systolic murmur was best heard in the upper left parasternal area. On investigation, complete blood cell count showed hemoglobin of 9.3gm%, hematocrit of 30%, white cell count of 10,000/cumm, and platelet count of 3.8lakhs/cumm. Chest X-ray revealed an enlarged cardiac silhouette (CT>0.55) and increased pulmonary vasculature. Electrocardiography (EKG) showed sinus rhythm, normal QRS axis with biventricular hypertrophy. Echocardiography (fig1) showed large (13mm) distal aorto-pulmonary window involving the right pulmonary artery origin with bidirectional shunt with hyperkinetic pulmonary hypertension. There was mild tricuspid regurgitation with moderate pulmonary regurgitation (gradient=56mmHg). Left atrium and left ventricle was dilated. Subsequently, surgical closure of AP window was done. Post operative echo revealed no residual flow, normal left pulmonary artery & right pulmonary artery with good biventricular function. On follow-up after two month, child is doing well.
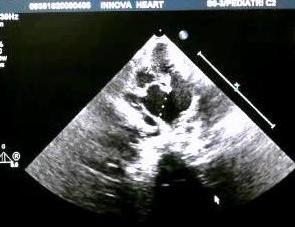
Figure 1: Echocardiography shows the large aorto-pulmonary window.
An Aortopulmonary window (APW) is usually wide, causing important symptoms in the first weeks or months of life, which result from the significant left-to-right shunt (1,2). In 1936, Abbot reported that the APW is a rare congenital cardiac anomaly accounting for about 0.1% of all cardiac defects in an autopsy study. This anomaly exists causing a communication between the ascending aorta (AA) and the pulmonary artery (PA) with normal separation of the aortic and pulmonary valves, which resulted from faulty embryogenesis of septation of the aortopulmonary trunk. John Elliotson first described it in 1830 and Gross performed the first successful surgery in 1948 (3,4). APW is classified into three types according to proximal, distal or total defects as per Mori's classification (5,6). Hemodynamic abnormalities of AP window mimic a large Ventricular Septal Defect (VSD) or Patent Ductus Arteriosus (PDA) with pulmonary hypertension. The heart murmur of this anomaly is often mistaken for the murmur of a high VSD, because although a continuous murmur may be present in patients with APW, more often there is only a systolic murmur that is generally heard along the upper left sternal border. Congestive heart failure (CHF) and pulmonary hypertension appear usually during early infancy. The clinical diagnosis of APW, although difficult to make, should be considered in any patient with congestive heart failure and low weight gain. EKG and chest X-ray are nonspecific, the echocardiogram is very important for diagnosing the APW (7,8). Garver et al. found that noninvasive imaging with echocardiography and/or MRI adequately defined the anatomical defects before surgery (9). Transcatheter closure of APW should be considered when anatomy is favorable in terms of location and size of the defect, in the absence of associated anomalies. In our case, the aorto pulmonary window was distal and large size, which was not possible to close by device. Hence, surgical closure of the APW was done. The Rashkind double umbrella device, the Amplatzer duct occluder, the Amplatzer septal occluder, muscular VSD occluder, and perimembranous VSD occluder have all been used to close small (type I) defects (10-12). Surgery is indicated as soon as the diagnosis is established, regardless of the patient's age when Eisemenger syndrome does not exist. The choice of the surgical technique is based upon the type and size of the AP window. The aorta and pulmonary artery may be divided, and the defects in the walls may be closed primarily or with patch material. Alternatively, the aorta or pulmonary artery may be opened and the defect patched using autologous, homologous, xenograft, or synthetic material. The prognosis of the patient with APW is excellent if surgical correction is performed early in life, before irreversible pulmonary vascular changes occur. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Moore P, Brooks MM, Heymann MA. Patent ductus arteriosus and aortopulmonary window. In: Allen HD, Shaddy RE, Drisccoll DJ, Feltes TF (eds): Moss and Adams' Heart Disease in Infants, Children, and Adolescents, Including the Fetus and Young Adult (7th ed.). Baltimore: Willians & Wilkins, 2008: 697-699.
- Fyler DC. Aortopulmonary window. In: Fyler DC, (ed): Nadas' Pedriatic Cardiology. Philadelphia: Hanley & Belfus, 1992: 693-695.
- Elliotson J. Case of malformation of the pulmonary artery and aorta. Lancet. 1830; 1: 247-251.
- Gross RE. Surgical closure of an aortic septal defect. Circulation. 1952; 5: 858-863. [CrossRef] [PubMed]
- Richardson JV, Doty DB, Rossi NP, Ehrenhaft JL. The spectrum of anomalies of aortopulmonary septation. J Thorac Cardiovasc Surg. 1979;78: 21-27. [PubMed]
- Mori K, Ando M, Takao A, Ishikawa S, Imai Y. Distal type of aortopulmonary window. Report of 4 cases. Br Heart J. 1978; 40: 681-689. [CrossRef] [PubMed] [PMC free article]
- Snider RA, Serwer AG, Ritter BS. Echocardiography in Pediatric Heart Disease, 2ª ed. Mosby, 1997; 292-293.
- Pieroni DR, Gingell RL, Roland JM, Chung CY, Broda JJ, Subramanian S. Two-dimensional echocardiographic recognition and surgical management of aortopulmonary septal defect in the premature infant. Thorac Cardiovasc Surg 1982; 30: 180-183. [CrossRef] [PubMed]
- Garver KA, Hernandez RJ, Vermilion RP, Martin Goble M. Images in cardiovascular medicine. Correlative imaging of aortopulmonary window: demonstration with echocardiography, angiography, and MRI. Circulation. 1997; 96: 1036-1037. [CrossRef] [PubMed]
- Naik GD, Chandra VS, Shenoy A, Isaac BC, Shetty GG, Padmakumar P, Jayranganath M.. Transcatheter closure of aortopulmonary window using Amplatzer device. Catheter Cardiovasc Interv. 2003; 59: 402-405. [CrossRef] [PubMed]
- Stamato T, Benson LN, Smallhorn JF, Freedom RM. Transcatheter closure of an aortopulmonary window with a modified double umbrella occluder system. Cathet Cardiovasc Diagn. 1995; 35: 165-167. [CrossRef] [PubMed]
- Richens T, Wilson N. Amplatzer device closure of a residual aortopulmonary window. Catheter Cardiovasc Interv 2000; 50: 431- 433. [CrossRef]
|
| Cite this article as: | | Taksande A, Gouthami V, Padhi S, Bakshi K. Aorto Pulmonary Window in Infant. Pediatr Oncall J. 2010;7: 50-51. |
|