Narendra Chaudhary, Sheetal Sharda.
Genetic and Metabolic Unit,Department of Pediatrics, Advanced Pediatrics Center, Post Graduate Institute of Medical Education and Research, Chandigarh, India.
ADDRESS FOR CORRESPONDENCE
Dr Sheetal Sharda, Assistant Professor, Genetic and Metabolic Unit, Department of Pediatrics, Advanced Pediatrics Center, Post Graduate Institute of Medical Education and Research, Chandigarh, India-160012.
Email: drnarendrapgi@rocketmail.com; sheetalsharda@hotmail.com | | Abstract | | Spondyloepiphyseal dysplasia as a sign of untreated congenital hypothyroidism is rare nowadays due to implementation of neonatal screening and increased awareness of pediatricians to detect hypothyroidism earlier. But neonatal screening is not routinely done in the developing countries. We report here a case of spondyloepiphyseal dysplasia due to untreated congenital hypothyroidism, which was not screened for hypothyroidism during neonatal life. Because of similar radiological findings, this patient was confused with the congenital spondyloepiphyseal dysplasia. Radiological findings of both entities are discussed. Being a treatable cause, hypothyroidism should always be considered as differential diagnosis of spondyloepiphyseal dysplasia, especially if the patient belongs to the developing world. | | | | Introduction | | A six year old girl was presented with progressive painful limp and referred to the Genetic Clinic with suspected congenital spondyloepiphyseal dysplasia. Radiography revealed bilateral epiphyseal dysgenesis of proximal end of femur with adaptive changes in acetabulam and vertebral changes. Previous medical records revealed that she was under treatment for congenital hypothyroidism since age of two years but was noncompliant and was a defaulter. Epiphyseal dysplasia as a sign of untreated hypothyroidism is described since early 1900's. Hypothyroidism must be considered as a differential diagnosis of spondylo-epiphyseal dysplasia, as the radiological findings can often be confused with the skeletal abnormalities seen in hereditary spondyloepiphyseal dysplasias. As clinical diagnosis of hypothyroidism is usually difficult before three years of age and appropriate treatment would lead to rapid normalization; high index of suspicion in such cases is emphasized and should not be confused with the osteodysplasias, which are not treatable. | | | | Case Report | A six year old girl was presented to the orthopedic outpatient department with chief complaint of progressive painful limp of about three months duration. There was no history of trauma, bone pain or fever. On suspicion of congenital spondyloepiphyseal dysplasia, she was referred to the Genetic Clinic. The girl was the second birth order of non-consanguineous marriage, delivered at full term by lower segment caesarian section (indication not known). The age of the mother was 24 years at the time of conception. The information about thyroid status during infancy was not available and the patient was not screened for hypothyroidism. There was history of delayed cry and she was kept in nursery for six days. There was a still birth prior to this child. The father had consulted a private physician at the local area at age of two years for global developmental delay. Review of previous records revealed that she was worked up for congenital hypothyroidism at that time. Her first thyroid profile showed TSH values > 100 IU/ml and free T4 was 1.34 pmol/L. Her 99mTc pertechnate thyroid scan was suggestive of sublingual thyroid gland. She was started on thyroxin replacement at a dose of 50 g/day. Her follow up thyroid profile showed TSH of 1.6 IU/ml and free T4 of 22.5 pmol/L. The child was then lost to follow up for next three years and was noncompliant as regard to medical therapy. On examination, height of the patient was 104 cm. (between 3rd -5th centile), weight was 14.4 kg (between 3rd -5th centile) & head circumference was 51 cm (normal). The patient kept her tongue protruded most of the times & had enamel involvement as well as dental caries. There was neither tenderness nor swelling in bones or joints. But leg length discrepancy was evident. The left leg was externally rotated and there was limitation of internal rotation and extension at hip joint. She was walking with waddling gait.
Repeat thyroid investigations revealed free T4=11.2 ng/ml; TSH=45.9 g/ml. Radiography showed irregular and deformed proximal femoral epiphysis suggestive of epiphyseal dysgenesis [figure 1A]. Neck-shaft angle was 1250 on left side and 1300 on right side (coxa vara). Acetabulum margins were irregular bilaterally. The left hip joint space was increased. Cortical thickening and narrowing of medullary canal is seen in tibia. There is narrowing of T12-L1 disc space and L1 is bullet-shaped and antero-posteriorly short (figure 1B). In view of clinical setting of congenital hypothyroidism, we kept first possibility of hypothyroidism induced skeletal dysplasia and treated accordingly.
Figure 1A. Radiological evidence of epiphyseal dysgenesis of the femoral head with acetabular changes.
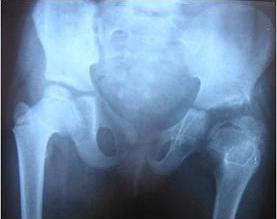
Figure 1B. X-ray spine showing changes [platyspondyly, bullet shaped vertebral bodies] due to untreated hypothyroidism.
![<b>Figure 1B. X-ray spine showing changes [platyspondyly, bullet shaped vertebral bodies] due to untreated hypothyroidism.</b>](/cgi_bin/caseimages/File_1_dysplasia2.JPG) | | | | Discussion | Epiphyseal ossification abnormalities occurring in childhood hypothyroidism began to appear in medical literature by 1909. Only those epiphyseal centers which would normally undergo ossification at the time of the hypothyroidism showed the dysgenesis [1]. Disappearance of epiphyseal dysgenesis was noted within a year or two after starting therapy [2]. Two case reports of spondyloepiphyseal dysplasia secondary to undiagnosed congenital hypothyroidism were found in literature [1, 3]. Both had ectopic thyroid in sublingual area.
Radiological findings: Epiphyseal dysgenesis is hallmark of long standing untreated hypothyroidism. This is due to irregular spotty and delayed ossification of epiphyseal centers which starts in numerous small foci, grows larger and coalesces to form a single centre of uneven density with irregular margins called 'cretinoid epiphyseal dysgenesis.' [5]. It is frequently seen in femoral head and humeral head but many epiphyseal centers may be affected [1]. In hip joint, coxa vara, coxa plana and coxa magna have been described [2]. Femur neck may be short and broad with reduction of neck shaft angle (coxa vara). Acetabulum margins may be irregular. Long bones may show narrowed medullary cavity with thickened cortex [5]. Spine may show platyspondyly, bullet shaped vertebral bodies, widened disc spaces and thoraco-lumbar kyphosis [3, 6]. Skull shows brachycephaly, periorbital sclerosis (lunette sign), enlarged sella (bowel shaped), wide open anterior fontanel and wormian bones [5]. Teeth may be malformed and susceptible to caries [4].
These radiological findings are difficult to differentiate from that of Legg-Calve-Perthes disease and hereditary forms of epiphyseal dysplasias. In Perthes disease, typical stages of avascular necrosis are found, usually unilateral but may be bilateral in 10-20% of cases [10]. Hereditary epiphyseal dysplasias are traditionally divided into two broad categories- spondyloepiphyseal dysplasia and multiple epiphyseal dysplasias. The later have little or no spinal change. Diagnosis is established on the basis of positive radiographic findings in absence of biochemical abnormalities [7].
Typical clinical signs of congenital hypothyroidism are usually present in older children, and clinical diagnosis is practically difficult before third year of life. To prevent mental retardation and skeletal changes, early diagnosis & treatment is very important. Due to neonatal screening and high index of suspicion, long-term untreated hypothyroidism is now rare. Ectopic thyroid is frequently demonstrable and this mild form of hypothyroidism is not always picked up by newborn TSH screening because of immaturity of hypothalamic pituitary thyroid axis [8]. Combined TSH & T4 screening is more sensitive but not found cost effective for routine use [9]. It is important therefore that clinicians to remain aware of hypothyroidism as a potential cause of illness despite normal screening. More importantly, neonatal screening is not routinely done in many developing countries, need of which is emphasized here. Our patient was oligosymptomatic who was suspected to have hypothyroidism based only on developmental delay at two years of age. But unfortunately she lost to follow up. Thus, besides mental deficiency, skeletal abnormalities may be an important cause of morbidity in children with hypothyroidism. The emphasis on good compliance can never be understated. | | | | Compliance with Ethical Standards | | Funding | | None | | | | Conflict of Interest | | None | | |
- Eberle AJ. Congenital hypothyroidism presenting as apparent spondyloepiphyseal dysplasia. Am J Med Genet. 1993; 47: 464-467. [CrossRef]
- Resnick D, Kransdorf MJ. Thyroid disorders. In: Bone and Joint Imaging, 3rd edition. Philadelphia, Elsevier Saunders, 2005: 597-602. [CrossRef]
- Huffmeier U, Tietze HU, Rauch A. Severe skeletal dysplasia caused by undiagnosed hypothyroidism. Eur J Med Genet. 2007; 50: 209-215. [CrossRef]
- Larsen PR et al. Hypothyroidism. In: William's Textbook of Endocrinology, 10th ed. Philadelphia, Saunders, 2003:423-447.
- Silverman FN, Kuhn JP. Bone Changes in Endocrinopathies. In: Caffey's Pediatric X-ray Diagnosis, 9th edition. Pennsylvania, Mosby Year Book, 1993; 2: 1927.
- Sutton D. Metabolic and Endocrine Disorders Affecting Bone. In: Textbook of Radiology and Imaging, 6th edition. New York, Churchill Livingstone, 1998; 1: 241.
- Grainger RG, Allison DJ. Skeletal Dysplasias and Malformation Syndromes. In: Diagnostic Radiology, 4th edition. London, Churchill Livingstone, 2001; 3: 1976.
- Wiedemann HR. Oligosymptomatic hypothyroidism presenting as apparent spondyloepiphyseal dysplasia. Am J Med Genet. 1994; 50: 385. [CrossRef]
- Buyukgebiz A. Newborn screening for congenital hypothyroidism. J Pediatr Endocrinol Metab. 2006; 19: 1291-1298. [CrossRef]
- Kulkarni GS. Dysplasias of Bone. In: Textbook of Orthopedics and Trauma, 2nd edition. New Delhi, JAYPEE, 2008; 4: 3430.
|
| Cite this article as: | | Chaudhary N, Sharda S. Congenital Hypothyroidism Induced Spondyloepiphyseal Dysplasia- A Case Report. Pediatr Oncall J. 2011;8: 10-12. |
|