Karam Chand, Hukum Singh, Vikas Gupta.
Dept. of Neurosurgery, VMMC & Safdarjung Hospital, New Delhi - 29, India.
ADDRESS FOR CORRESPONDENCE
Dr. Karam Chand, Head, Dept of Neurosurgery, VMMC & Safdarjung Hospital , New Delhi - 29. India.
Email: sharmakchand@rediffmail.com | | Abstract | | An 18 months old child, presented with growing skull fracture. CT scan brain with 3D reconstruction showed Leptomeningeal cyst with skull defect. There was a large associated Parafalcine CSF collection on the side of herniating brain; the child was managed accordingly with good outcome. | | | | Introduction | | Cranio-cerebral erosion or growing skull fracture is a rare complication of skull fracture seen in infancy and early childhood. It is characterized by progressive enlargement of diastatic fracture line, along with collection of CSF and herniated brain matter below the scalp. This collection has also been termed as Lepto-meningeal cyst. Diagnostic modalities include X-Ray skull, CT scan brain along with 3-D reconstruction of skull to visualize the entire cranial defect and MRI brain to evaluate the extent of parenchymal injury. Therapeutic measures include surgical exploration of cyst with delineation of dural margins below the defect and duraplasty along with cranioplasty of the skull defect. | | | | Case Report | An 18 months old child was brought in with the history of fall 6 months back. He presented to us with the complaint of progressively enlarging swelling over left parietal region after the trauma. There was no history of any vomiting, seizures or any discharge from ear or nose. The patient was conscious and crying, with no focal neurological deficit. He had soft, cystic non-tender left parietal scalp swelling with visible brain pulsations. X-Ray skull showed wide left parietal bone defect. NCCT scan brain along with 3D reconstruction was done, which showed large left parietal skull defect measuring about 10cm x 4cm (Figure-1). There was a large CSF collection associated with herniation of brain matter through the skull defect, below the scalp, leading to a large cystic scalp swelling. There was an associated large left parafalcine CSF collection (Figure-2 and Figure-3).
Figure 1: NCCT scan brain with 3D reconstruction showing large left parietal skull defect measuring about 10cm x 4cm
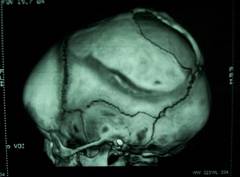
Figure 2: Herniation of brain matter through the skull defect, below the scalp, leading to a large cystic scalp swelling with associated large left parafalcine CSF collection in coronal section.
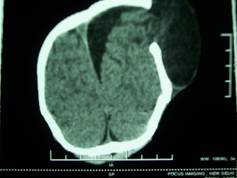
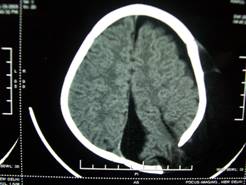
Figure 3: Herniation of brain matter through the skull defect, below the scalp, leading to a large cystic scalp swelling with associated large left parafalcine CSF collection in axial section.
Patient was operated for the above-mentioned pathology. Surgical exploration of cystic swelling was done, CSF collection was drained and herniated brain matter was excised. Craniotomy surrounding the skull defect was done and dural margins were defined. Duraplasty was done using pericranial graft and bone defect was closed with split calvarial graft. Child recovered well with no neurological deficit. | | | | Discussion | Growing skull fractures usually occur after head trauma in the first three years of life (particularly in infancy) and almost never after 8 yrs of life. Incidence reported is only 0.05 to 0.1% of skull fractures in childhood [1, 2]. During this stage, the brain volume is increasing rapidly which is in part responsible for their development. Though the development of growing skull fractures after diastatic fractures is multifactorial but the predominant factor in their causation is the presence of lacerated dura mater. The pulsatile force of the brain during its maximum growth causes cerebral or subarachnoid herniation through the lacerated dura, which causes the fracture in the thin skull to enlarge. This interposition of tissue prevents osteoblasts from migrating, inhibiting fracture healing. The resorption of the adjacent bone by the continuous pressure from tissue herniation through the bone gap adds to the progression of the fracture line.
The brain extrusion may be present shortly after diastatic linear fracture in neonates and young infants [3] resulting in focal dilatation of the lateral ventricle near the growing fracture. This focal dilatation is reversible and may normalize after surgical repair [4]. Because cranial defects never increase if the underlying dura is intact and also craniotomy performed without watertight closure of dura does not cause a growing fracture. Therefore, for growing fractures to develop a dural laceration is a must with a fracture line.
Another risk factor is severity of underlying trauma. A linear fracture associated with hemorrhagic contusion of subjacent brain suggests a trauma significant enough to cause dural laceration. The brain at the growing fracture site shows a cerebromeningeal cicatrix formation. Cystic changes at the growing fracture site may be because of cystic encephalomalacia. Post-traumatic aneurysms and subdural hematomas have also been reported to accompany growing skull fractures [6, 7]. Though most patients show damage to underlying brain, this finding is not a prerequisite for the development of growing skull fractures [8]. Parafalcine CSF collection as in our case is rare.
These skull fractures after reaching maximum extent will cease to grow and remain stable through out adulthood [2, 5]. A depressed fracture usually does not become a growing fracture [9] but a linear fracture extending from a depressed one can become one [10]. A fracture with a diastasis of > 4mm may be considered at risk of developing a growing skull fracture [3, 11, 12]. But a post-traumatic diastasis of a cranial suture is an unusual site for a growing fracture.
These fractures commonly present as a progressive, often pulsatile, scalp mass that appears sometime after head trauma sustained during infancy. Also related are seizures, hemiparesis, psychomotor retardation, but an asymptomatic palpable mass may be the sole sign. The usual site is the parietal region. A growing fracture at the skull base may present with ocular proptosis or CSF rhinorrhea or otorrhea.
A plain radiograph may show a fracture line that crosses a coronal or lambdoid suture but it is usually limited to a parietal bone [13]. On CT, a hypodense lesion is seen near the fracture site. Intracranial hypodense area may be an encephalomalacia, arachnoid loculation or cortical atrophy. Owing to the risk of neurological deterioration and development of seizure disorder surgical correction of growing fractures is recommended.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Des champs GT Jr, Blumenthal BI. Radiologic seminar CCXLIX : Growing skull fractures of childhood. J Miss state Med Assoc 1988; 29:16-17. [PubMed]
- Ramamurthi B, Kalanaraman S. Rationale for surgery in growing fractures of skull. J. Neurosurg 1970; 32:427-430. [CrossRef] [PubMed]
- Thompson JB, Mason TH, Haines GL, Cassidy RJ. Surgical management of diastatic linear fractures in infants. J Neurosurg 1973; 39:493-497. [CrossRef] [PubMed]
- Scarfo GB, Mariottini A, Tomaccini D, Palma L. Growing skull fractures : progressive evolution of brain damage and effectiveness of surgical treatment. Childs Nerv Syst 1989; 5:163-167. [CrossRef] [PubMed]
- Rahimizadeh. A growing skull fracture in the elderly. Neurosurgery 1986; 19:675-676. [CrossRef] [PubMed]
- Buckinghum MJ, Crone KR, Ball WS, et al. Traumatic intracranial aneurysms in childhood : Two cases and review of literature. Neurosurgery 1988; 22:398-408. [CrossRef]
- Locatelli D, Messina AL , Bonfanti N, et al. Growing fractures : an unusual complication of head injuries in paediatric patients. Neurehirurgia (Stuttg.) 1989; 32:101-104. [CrossRef]
- Lende RA, Erickson TC, Growing skull fractures. J Neurosurg 1961; 18:479-489. [CrossRef] [PubMed]
- Arsenic C, Ciurea AV. Clinicotherapeutic aspects in growing skull fractures. A review of literature. Childs Brain 1981; 8:161-172.
- Lye RH, Occleshaw JV, Dutton J. Growing fractures of skull and the role of CT. Case report. J Neurosurg 1981; 55:470-472. [CrossRef] [PubMed]
- Gruber FH, Post traumatic leptomeningeal cysts. Am J Roentgenology 1969; 105:305-307. [CrossRef]
- Traveras JM, Ransohoff J. Leptomeningeal cysts of brain following trauma with erosion of skull : a study of seven cases treated by surgery. Neurosurg 1953; 10:233-243. [CrossRef] [PubMed]
- Kingsley D, Till K, Hoase R. Growing fractures of skull. J Neurosurg psychiatry 1978; 41:312-318. [CrossRef]
|
| Cite this article as: | | Chand K, Singh H, Gupta V. CRANIO-CEREBRAL EROSION WITH PARAFALCINE CSF COLLECTION: A CASE REPORT. Pediatr Oncall J. 2006;3: 50-51. |
|