Types of Burns
Burns are divided into 3 different types:
First degree or superficial burns:
It is commonly seen with a sunburn. It is usually red and blanches (becomes white) on pressure. It occurs due to damage to the top (epidermis) layer of the skin only. It heals by itself in 3-6 days and generally does not require hospitalization.
Partial thickness burns or second degree burn:
It involves the entire epidermis and some portion of the dermis. They are of two types:
- Superficial partial-thickness burns: They are painful and associated with blisters. They heal within 3 weeks without any visible scars. There may be some pigment changes.
- Deep partial-thickness burns: They are dry and white in colour. They may cause scarring and take longer to heal. Skin grafting is usually required for healing.
Full thickness burns:
They involve the entire epidermis and dermis. They are dry and leathery in appearance. They cause scarring and require immediate skin grafting and the use of compression garments.
Burns
Burns are death and necrosis of a tissue due to heat. Burns may occur due to dry heat, (in the form of fire) wet heat (in the form of scalds), or electrical burns.
Burns - Pathophysiology
Heat damages the cells of the skin releasing chemicals that stimulate the nerves and cause pain. A burn heals when a new layer of skin grows in from the edges of the burn. However, if the burn is very large or very deep, bacteria may invade and cause infection. Also, due to the evaporation of fluids from the open wound, the patients may get dehydrated. Hence, the two major short term complications of burns are infection and dehydration. In the long term, in the healing process, the wound may start shrinking or becoming smaller leading to contractures. If contracted tissue is present in the limbs, this may lead to a loss of normal motion and can also cause a distorted appearance due to the pulling of the surrounding healthy tissue. In a burn patient, sensations of hot, cold, wetness, dryness, touch, and pain may change even permanently. A patient post-burn will not be able to sweat properly due to the damaged sweat glands. Hence, appropriate clothing as per the season is required (cotton in summer and warm clothing in winter),
Skin color is determined by the melanin and carotene pigments in the epidermis. Melanin protects the skin from sunburns. After a burn, the burnt skin may not be able to produce melanin, hence leading to sunburns. Also, the skin may become lighter(depigmented or hypopigmented) or darker (hyperpigmented) as compared to the normal skin.
Wallace Rule of 9: The surface area of the body involved in burns is generally estimated by using the Wallace Rule of 9. The following is the distribution of the surface areas:[1]
For adults
Head and neck- 9%
Thorax- 9% for front and 9% for back of chest
Abdomen- 9% for front and 9% for back of abdomen
Upper limbs- 9% for each
Lower limbs- 9% for front and 9% for back of each
External genitalia- 1%
The following diagram summarises the distribution[1]
[Reference : Essentials of Forensic Medicine by NK Reddy
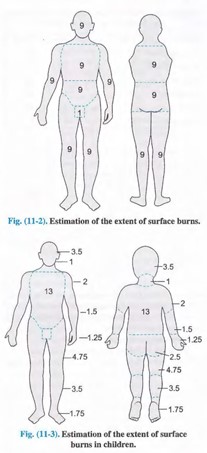 ]
]
Complications of burns
Burns can cause the following major complications
- Septic shock - It is the most common cause of mortality in burn patients. Burn patients are at increased risk of infections due to exposed skin surfaces.[2]
- GI ulcers - Stress ulcers are common post burns and hence proper prophylaxis must be given.[2]
- Acute Kidney Injury - AKI is seen commonly with patients who have severe burns leading to increased fluid losses.Acute Renal failure can also occur as a consequence.[2][3]
- Post burn contractures - They are fairly common, limiting patient’s day-to-day activities and usage of the particular limb.[4]
- Pancreatitis - Though not a common complication, pancreatitis has been reported in burn patients.[5]
Treatment
First degree or superficial burns heal naturally. Deep second degree and full-thickness burns require skin grafting for rapid healing and minimum scarring and generally require hospital care. In addition, supportive therapy like fluids, blood infusion, and pain medication is required. In some patients, the burn may lead to intolerable and excruciating pain for which even lV morphine may be required. For first degree burns and open wounds, topical creams like silver sulfadiazine and bacitracin may be applied. Often dressings may be applied.
Treatment of Skin Discoloration that Occurs with Healing
UV protection is required for 12-18 months post-burn and these patients should apply sunscreen lotion while going out in the sun. Camouflage cosmetics to cover the burns can be used. Hair coloring products can be used 6 weeks after healing is completed. Permanent products can be used 3 months after healing.
Skin Grafting
Skin grafting consists of excision or removal of burnt devitalized tissue and removal of healthy skin from a donor site to cover the cleaned burnt area. An instrument (dermatome) gently shaves a piece of skin about 1/100 of an inch thick from the healthy skin and that skin is grafted over the burnt area. Skin can also be used from dead people (cadavers).To help the graft become secure, the area of the graft is immobilized for at least 5 days and after that, normal daily activity is started. Skin grafting is usually done under anesthesia.
There are other types of artificial skin grafts available which can temporarily cover the wounds:
- Xenograft or Heterograft: Skin is taken from animals
- Collagen
Meshing is a process by which the donor skin is enlarged to cover a large burnt area when there is not enough healthy skin available. The disadvantage is that it is a less durable graft and leads to more scarring. However, it helps allow the blood and body fluids to drain under the graft and thus prevents graft loss and it also allows the donor skin to cover a greater burnt area.
Grafts are held in place with surgical staples or stitches. Once the graft becomes stable (usually within 4-5 days), the staple/stitches are removed.
Other required care[2] -
- Gastrointestinal - Stress ulcers in the GI tract may occur after a burn, and thus stress-ulcer prophylaxis may be given.
- Renal - Acute Kidney Injury is a very common finding in severe burn patients. This can be managed by Renal Replacement Therapy.
- Infectious - Burn patients are more susceptible to septic shock, hence proper antibiotic prophylaxis must be given. Septic shock is the most common cause of mortality in burn patients.
- Nutritional - Owing to severe nutritional losses due to burns, the patients are to be provided with adequate nutrition, which may be via enteral or parenteral route.
- Palliative - Palliative care is to be provided in the form of physiotherapy and occupational therapy to help the patients lead a near-normal life.
What Happens to the Donor Site from where the Skin Is Removed?
Although the skin taken from the donor site is very thin, it can cause scarring and pigmentary changes at the donor site.
How Does Exercise Help A Burn Patient?
Exercise helps the body heal better. It helps a burn patient to regain independence. They may also help prevent contractures.
How Do You Prevent Contractures?
Contractures usually occur due to the extension of burns over a joint limiting movement. Skin tightness may be the first sign of contracture and anti-contracture positioning may be required for 24 hours a day. Exercises to stretch or elongate the skin are recommended. Sometimes, surgical procedures like the release of the band area (z-plasty) may be required. Before surgery, casting of the limb may be required, as a constant stretch is applied by the cast to elongate the skin.
How Do You Prevent Ugly Scars (hypertrophic Scars) From Developing?
Compression garments are worn over the burnt area. Compression can also be given by splints, orthoses, and casts. Compression garments help heal the burn with minimum amount of scarring by pressing and flattening the scars. Compression is given for 22-23 hours a day. It is required until almost 12-18 months post- burn or till the burn completely heals (matures).
1. Essentials of Forensic Medicine by NK Reddy
2. Britton GW, Wiggins AR, Halgas BJ, Cancio LC, Chung KK. Critical Care of the Burn Patient. Surg Clin North Am. 2023 Jun;103(3):415-426. doi: 10.1016/j.suc.2023.01.005. Epub 2023 Apr 4. PMID: 37149378.
3. Palma SA, Metnitz PG, Kamolz LP, Frey M, Druml W. Akutes Nierenversagen bei Brandverletzten - Ursachen, Konsequenzen und Vermeidungstrategien [Acute renale failure in burns - causes, consequences and avoidance strategies]. Anasthesiol Intensivmed Notfallmed Schmerzther. 2011 Jan;46(1):12-9. German. doi: 10.1055/s-0030-1270554. Epub 2011 Jan 17. PMID: 21243549.
4. Brown M, Chung KC. Postburn Contractures of the Hand. Hand Clin. 2017 May;33(2):317-331. doi: 10.1016/j.hcl.2016.12.005. Epub 2017 Mar 1. PMID: 28363298.
5. Ryan CM, Sheridan RL, Schoenfeld DA, Warshaw AL, Tompkins RG. Postburn pancreatitis. Ann Surg. 1995 Aug;222(2):163-70. doi: 10.1097/00000658-199508000-00008. PMID: 7543741; PMCID: PMC1234774.