Swati Kolpuru.
Pediatric GI Department, University of Maryland, USA.
ADDRESS FOR CORRESPONDENCE
Dr Swati Kolpuru, Pediatric GI Department, University of Maryland, USA.
Email: skgupta29@hotmail.com | History and background
Diarrhea is accountable for 25% of deaths in children under five in the world (3 million deaths per year or 8000 per day). Loss of intestinal fluid may lead to severe hypovolemia, shock, and death particularly in young children. Giving fluids to prevent or treat dehydration is called oral rehydration therapy (ORT).
ORT is the most essential and effective way of preventing these deaths. ORT, combined with guidance on appropriate feeding practices, is the main strategy recommended by the WHO Department of Child and Adolescent Health and Development (CAH) to achieve a reduction in diarrhea related mortality and malnutrition in children.
ORT was developed in the late 1960s by researchers in India and International Centre for Diarrheal Disease Research in Bangladesh, for the treatment of cholera. The Indo-Pakistani War of 1971 provoked a public health emergency in the refugee camps set up to house those fleeing the violence. With cholera spreading rapidly and death rates rising, the head of a medical centre in one of the camps instructed his staff to distribute Oral Rehydration Salts (ORS). It was a success, and over the next eight weeks, deaths fell to less than 1%. In 2002, Drs. Norbert Hirschhorn, Dilip Mahalanabis, David R. Nalin, and Nathaniel F. Pierce were awarded the first Pollin Prize for Pediatric Research, in recognition of their work in developing ORT.
In the 1980s nearly five million children under 5 years old died each year from diarrhea. In 2000 this figure had dropped to 1.8 million. Oral rehydration along with improved nutrition and sanitation is central to the package of measures that has helped ensure this fall in mortality.(1)
Early use of ORT at home in children with diarrhea decreases the number of outpatient visits and hospitalizations, and overall medical costs. Despite relatively high ORT access rates ORT use is inadequate2. These poor results could be a factor of diminished knowledge and inadequate numbers of trained staff. According to government studies, ORT use varies in India from 36-96.3%, but according to operational research by the National Institute of Cholera and Enteric Diseases, ORT use in the best health facilities is only 11-12%.
Pathophysiology of diarrhea
Oral rehydration therapy is widely considered to be the best method for combating the dehydration caused by diarrhea and/or vomiting.
In the past, diarrhea was considered to be caused by abnormal gastrointestinal motility. It is now clear, however, that most diarrheal conditions are due primarily to alterations of intestinal fluid and electrolyte transport and less to smooth muscle function. Infectious diarrhea occurs as a result of
- Toxigenic types, in which an toxin production is the major if not exclusive pathogenic mechanism.
- Invasive types, in which the organism penetrates the mucosal surface as the primary event, but enterotoxin may be produced as well.
PhysiologyPhysiology
On average, the luminal fluid load of the gut composed of oral intake and endogenous secretions is approximately 9 L per day.
Small intestine is very efficient in absorption and greater than 98% of fluid load (8.8 L per day) is absorbed. This efficiency is due to the presence of mucosal permeability to passive flux of water and electrolytes. Colon absorbs 1.8 L of fluid per day. Absorption in the colon occurs against high electrochemical gradients to make solid stool. Less than 0.2 L is excreted as stool.
Net intestinal secretion or absorption is the result of interaction of the effects of many different factors, including peptides, active amines, hormones, and neurotransmitters, that circulate in the blood or are released locally from mucosal epithelial cells, lamina propria cells, or enteric neurons. These factors can be classified as secretagogues or pro-absorptive agents, depending on the overall effect of the agent on intestinal cells.
Water transport appears to be largely a passive process that occurs through both paracellular and transcellular routes in the intestine, coupled with solute movement.
A variety of transport proteins are required for intestinal transport of water and electrolytes. Ion transporters can be grouped into three major classes: pumps, channels, and carriers. Pumps are energy driven and capable of transporting ions against large electrochemical gradients like Na+K+- ATPase.
Channels are ion selective and conductive like the Cystic fibrosis transmembrane regulator (CFTR).
Carrier transport proteins facilitate ion and nutrient transport across cell membranes.
Because this is not an active process, transport rate and direction are determined by the existing electrochemical gradients for the substrate.
Scientific basis for ORS (Figure 1)
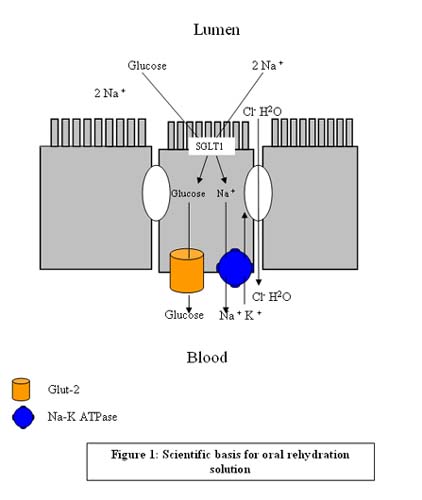
The intestinal brush-border membrane protein that plays a major part in the absorption of D-glucose from the diet is the Na+/glucose cotransporter (SGLT1). This transporter plays a major role in salt and water absorption, and provides the basis for ORT used to combat diarrhea.
Glucose is absorbed by a 2 stage process
- Active accumulation across the brush border membrane by SGLT1
- Downhill transport of glucose out of the enterocyte into the blood across the basolateral membrane by a facilitated glucose transporter (GLUT2).
The sodium gradient across the brush border is maintained by the basolateral Na+K+ pump; that is, the Na+ that enters the cell across the brush border long with sugar is pumped our across the basolateral membrane. The net result is that glucose and salt are absorbed.
The activation of SGLT1 has several other consequences. One involves the contraction of the perijunctional actin-myosin ring, which increases tight junctional permeability and facilitates paracellular transport of water and other small molecules. Activation of SGLT1 also appears to stimulate Na+ H+ pump activity, further enhancing Na+ absorptive capacity of the gut.(3)
In contrast with other Na+-absorptive pathways, glucose and amino acid stimulated Na+ absorption are not affected by enterotoxins such as cholera toxin and STa (heat-stable enterotoxin of E. coli). This property is the rationale for using sugar or amino acid based oral rehydration solutions (ORS) for the treatment of cholera and traveler's diarrhea.(4)
Rice-based electrolyte solutions also have been effective, because rice starch is rapidly converted to glucose by pancreatic amylase and brush border hydrolases.ORS has saved millions of lives and is highly cost-effective. Similarly, this is the basis for sports drinks, which essentially are sugar-based electrolyte solutions.
Desired composition of ors
The desired properties for ors as recommended by the World Health Organization (WHO) and UNICEF for global use include:
- Total osmolality between 200 to 310 mmol/L
- Equimolar concentrations of glucose and sodium
- Glucose concentration not in excess of 20 g/L (111 mmol/L)
- Sodium concentration between 60 to 90 meq/L
- Potassium concentration between 15 to 25 meq/L
- Citrate concentration between 8 to 12 mmol/L
- Chloride concentration between 50 to 80 meq/L
This ors formula can safely be used for all age groups and all etiologies of diarrhea. ors replaces the lost fluid and electrolytes and maintains fluid and electrolytes. Maximum uptake of water and electrolytes occurs when the ratio of carbohydrates to sodium in these solutions approaches one, but formulas range from ratios of 1:1 to 2:1.(5) Beverages with high sugar content (eg, fruit juices and soda) with a molar ratio of glucose in excess of sodium will increase diarrheal losses. The higher unabsorbed glucose load will increase the osmolality in the lumen, decreasing water absorption. Other fluids with excess sodium concentration compared with glucose (eg, chicken broth) also will increase diarrheal losses, as there is no organic solute for facilitated transport of sodium. Fluids with high sodium concentration also may result in hypernatremia. Potassium and chloride in the formula replace those lost in the stool of patients with diarrhea. Citrate, a base precursor, corrects acidosis and enhances the absorption of water and electrolyte. The ors formula has changed very little in the last decade except that sodium bicarbonate has been replaced by trisodium citrate, a more stable compound which allows for longer storage and cheaper packaging.(6)
Low osmolarity ors
Oral rehydration solutions have been improved since the early days: the formula was adjusted after a Cochrane Library systematic review in 2001 showed that a less concentrated solution had better outcomes.(7)
The need for unscheduled supplemental IV therapy in children given this solution was reduced by 33%. In a combined analysis of this study and studies with other reduced osmolarity ors solutions (osmolarity 210- 268 mOsm/l, sodium 50-75 mEq/l) stool output was also reduced by about 20% and the incidence of vomiting by about 30%. The 245 mOsm/l solution also appeared to be as safe and at least as effective as standard ors for use in children with cholera.
This new formula replaces the original ors, and is the only ors used globally by the WHO.(see Table 1)
Table 1: Composition of new ORS
| New ORS | grams/litre | % | New ORS | mmo/litre | | Sodium chloride | 2.6 | 12.683 | Sodium | 75 | | Glucose, anhydrous | 13.5 | 65.854 | Chloride | 65 | | Potassium chloride | 1.5 | 7.317 | Glucose, anhydrous | 75 | | Trisodium citrate, dihydrate | 2.9 | 14.146 | Potassium | 20 | | | | | Citrate | 10 | | Total | 20.5 | 100.00 | Total Osmolarity | 245 |
Rice based ors
Rice powder, being mostly starch, releases more than twice the amount of glucose when digested than is present in standard ors solution. This is enough glucose to support both the absorption of water and electrolytes in the ors solution and the reabsorption of a portion of the water and electrolytes secreted into the bowel as part of the diarrheal process. Protein in the rice powder may add to this effect through the release and absorption of amino acids. The osmotic activity of rice-ORS solution (about 220 mOsm/l) is lower than that of blood or other tissues (about 290 mOsm/l).
The results of the clinical trials performed to date indicate that the rate of stool loss is significantly reduced in patients with acute diarrhea given rice-ORS solution as compared with patients given glucose-ORS solution and it also reduces the duration of diarrhea.
Rice based ors is recommended in patients with cholera. Future studies are needed to assess the effect of rice based ors in children with acute, non-cholera diarrhea.
Role of ORT in clinical management
The recognition and treatment of dehydration are at the heart of case management of diarrheal disease. ORT is a simple, cheap, and effective treatment for diarrhea-related dehydration.
The general principles of case management include ORT and proper dietary management, with emphasis on appropriate, available, cost-effective methods of assessing and treating dehydration.
Principles of ORT treatment
- Adequate rehydration therapy using an appropriate ors
- Replacement of ongoing fluid losses from vomiting and diarrhea with ors
- Frequent feeding of appropriate foods as soon as dehydration is corrected.
ORT is recommended as first-line therapy for both mildly and moderately dehydrated children. ORT seems to be a preferred treatment option for patients with moderate dehydration from gastroenteritis.(8)
The 1st step in ORT is to weigh the patient and assess the degree of dehydration. ORT depends on the degree of dehydration. (See table2)
Table 2: ORT in the management of diarrhea
| No dehydration | Replace stool loses with ORS*
Continue age appropriate feeding | Mild dehydration
(3-5% volume loss) | Repletion phase - Hydration should be restored by administering ORT at a volume of 50 mL/kg over four hours. Additional ORS is given to replace ongoing loss of stool*. Reassessment of the patient's hydration status and replacement of ongoing losses should occur at least every two hours.
Maintenance phase - Once repletion is completed, feeding and fluids should be started. ORT is continued for ongoing diarrheal losses. | | Moderate dehydration(6-9% volume loss) | Repletion phase - Hydration should be restored by administering ORT at a volume of 100 mL/kg over four hours. Additional ORS is given to replace ongoing loss of stool*. At the end of each hour, the patient's hydration status and continuing stool and emesis losses should be calculated, with the total hourly loss added to the amount to be given over the next hour.
Maintenance phase - Once repletion is completed, feeding and fluids should be started. ORT is continued for ongoing diarrheal losses. | Severe dehydration
( 10 % or greater volume loss.) | Repletion phase - Emergent intravenous therapy with rapid infusion of 20 mL/kg of isotonic saline should be given. As the patient's clinical condition stabilizes and his/her level of consciousness returns to normal, therapy can be changed to ORT. A nasogastric tube can be used in patients who have a normal mental status but may be too weak to adequately drink the necessary volume of fluid. The intravenous line should remain in place until it is certain there is successful transition to ORT. ORT therapy is started at a volume of 100 mL/kg over four hours. Additional ORS is given to replace ongoing loss of stool*. At the end of each hour, the patient's hydration status and continuing stool and emesis losses should be calculated, with the total hourly loss added to the amount to be given over the next hour.
Maintenance phase - Once repletion is completed, feeding and fluids should be started. ORT is continued for ongoing diarrheal losses. | | * 1 mL of ORS should be administered for each gram of diarrheal stool or, 10 mL/kg of body weight of ORS should be administered for each watery or loose stool, and 2 mL/kg of body weight for each episode of emesis. |
Advantages of ORT
- Low cost
- Elimination of the need for IV line placement
- Treatment that can be done or continued at home.
- Safe and few side effects
Limitations of ORT use
- Altered mental status with concern for aspiration
- Abdominal ileus
- Underlying disorder that limits intestinal absorption of ORT (eg, short gut, carbohydrate malabsorption)
- Severe dehydration
- If stool output continues to be excessive, and ORT is unable to adequately rehydrate the child.
- If there is severe and persistent vomiting, and inadequate intake of ors, intravenous therapy is recommended.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Victora CG, Bryce J, Fontaine O, Monasch R. Reducing deaths from diarrhoea through oral rehydration therapy. Bull. World Health Organ. 2000;78(10):1246-55. [PubMed]
- Sarkar K, Sircar BK, Roy S, Deb BC, Biswas AB, Biswas R. Global review on ORT (oral rehydration therapy) programme with special reference to Indian scene. Indian J Public Health. 1990 Jan-Mar;34(1):48-53. [PubMed]
- Sarkar K, Sircar BK, Roy S, Deb BC, Biswas AB, Biswas R. Global review on ORT (oral rehydration therapy) programme with special reference to Indian scene. Indian J Public Health. 1990 Jan-Mar;34(1):48-53. [PubMed]
- Rao MC. Oral rehydration therapy: New explanations for an old remedy. Annu Rev Physiol 2004; 66:385. [CrossRef]
- Avery ME, Snyder J. Oral Therapy for Acute Diarrhea. New Engl J Med 1990. 323(13):891-4. [CrossRef]
- Lankinen KS , Bergstrom S, Makela PH, Peltomaa M. Health and Disease in Developing Countries, Macmillan 1994.
- Hahn S, Kim Y, Garner P. Reduced osmolarity oral rehydration solution for treating dehydration due to diarrhoea in children: systematic review. BMJ 2001:323;81-5. [CrossRef]
- Spandorfer PR, Alessandrini EA, Joffe MD, Localio R, Shaw KN. Oral versus intravenous rehydration of moderately dehydrated children: a randomized, controlled trial. Pediatrics. 2005;115:295-301. [CrossRef]
|
| Cite this article as: | | Kolpuru S. Oral Rehydration Therapy. Pediatr Oncall J. 2008;5: 121. |
|