Cavigelli-Brunner Anna1, Bauersfeld Urs1, Waldeck Guenter2, Balmer Christian1.
1Division of Cardiology, University Children's Hospital, Zurich, switzerland,
2General practitioner, Zurich, switzerland.
ADDRESS FOR CORRESPONDENCE
Cavigelli-Brunner Anna, Division of Pediatric Cardiology, University Children's Hospital Zurich, Steinwiesstrasse 75CH 8032 Zurich, Switzerland.
Email: anna.cavigelli@kispi.uzh.ch | | Abstract | | Supraventricular tachycardias (SVTs) are not rare in the paediatric age group, clinical presentations may vary and recognizing the diagnosis can be challenging. Nowadays most of the patients with SVTs can be cured by radiofrequency catheter ablation (RFA) of the accessory pathway or the focus of the tachycardia. In this report we describe a patient, who has been suffering from neuro-psychiatric symptoms for years until the cause, recurrent episodes of supraventricular tachycardia, was revealed. At the age of four years, the boy started to be hyperactive and showed poor concentration. Symptoms persisted despite various therapies. At the age of ten years, exercise tolerance decreased and a fast heart rate was noticed during "pulse diagnostic" in view of hyperactivity therapy. A 12 lead ECG showed a supraventricular tachycardia with 160 bpm. Echocardiography revealed a left ventricular dimension at the upper normal limit and a moderately impaired contractility. A treatment with amiodarone was initiated and the mean heart rate was reduced although no definitive termination of the tachycardia was achieved. Cardiac function normalised within five days. The intracardiac electrophysiologic study confirmed an atrioventricular reentrant mechanism on the basis of a left-sided accessory pathway, which was successfully ablated. | | | | Introduction | Attention deficit and hyperactivity disorder (ADHD) is characterized by inattention, hyperactivity, distractibility and impulsiveness lasting over at least 6 months. Symptoms usually start at the age of three to four years [1]. The prevalence of an ADHD is up to 9.5-11% depending on the diagnostic tests and criteria [2]. In children with poor school performance, restlessness and inattention there is a low threshold for this diagnosis.
Supraventricular tachycardias (SVTs) are frequent in children with an overall incidence of 0.1-0.4%. In 95%, the underlying mechanism is an atrioventricular re-entrant circuit via an accessory pathway [3]. Symptoms of recurrent intermittent SVTs are unspecific and may mimic ADHD. The taking of an accurate history from the patient himself can be difficult depending on the age of the child. Clinical diagnosis however is easy if the patient is seen during a tachycardic episode as illustrated by the following case report. | | | | Case Report | A ten years old boy suffered from hyperactivity and poor concentration since the age of four years. In the last months, his school achievement and sports performance decreased. A medical doctor providing alternative medicine was consulted for pulse diagnostics in view of a therapy of the ADHD. He noted a very fast heart rate and the patient was referred to the hospital. On examination, the boy was restless but compensated; his heart rate was elevated at 160bpm. The clinical examination was uneventful, but the 12 lead ECG showed a supraventricular tachycardia with narrow QRS complexes. P waves could be seen before each QRS complex with long RP and short PR intervals, typical for atrioventricular re-entrant tachycardias (Figure 1).
Figure 1: 24 hour Holter monitoring showed most of the time a supraventricular tachycardia, with short spontaneous sequences in sinus rhythm
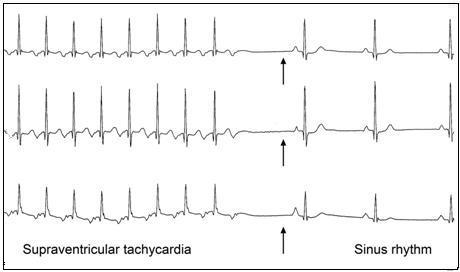
The size of the left ventricle was at the upper limit of normal and systolic function was moderately impaired with an ejection fraction of 40% (normal > 55%) as shown by echocardiography. The tachycardia was incessant and converted intermittently to sinus rhythm for a few seconds. The 12 lead ECG during sinus rhythm was normal (arrow). Administration of intravenous amiodarone did not result in permanent termination of the tachycardia but the episodes of the tachycardia became shorter which allowed the cardiac function to improve within five days. Electrophysiological examination two weeks later revealed a left-sided accessory pathway. The tachycardia was successfully terminated by radiofrequency ablation of the accessory pathway. The patient's personality returned to normal. His school performance improved dramatically and he remained free of symptoms without any medication. | | | | Discussion | ADHD is frequent in the pediatric age group. Diagnosis is established by clinical judgement based on comprehensive clinical evaluation and assessment considering the typical symptoms [1].
SVTs are not unusual in children, but clinical presentation may vary [4]. Older children often complain about the characteristic palpitations, heart stumble or funny heartbeat. Especially in younger patients, atypical and unspecific symptoms such as pain in the head, throat, or chest, dizziness, anxiety, paleness, sleep disturbances, restlessness and hyperactivity may appear. At first sight, it may not be evident that these symptoms refer to a tachycardia. Even in adults, a SVT can be elusive. Lessmeier et al [9] studied 107 adult patients with SVTs. In a retrospective survey 67% fulfilled the criteria for panic disorders and SVT was not recognized after initial medical evaluation in 55%.
A SVT can be detected with a careful clinical assessment at various stages of physical activity, keeping in mind the age dependant normal heart rate values [5]. A 12 lead ECG will confirm the diagnosis but sometimes repeated 24h Holter ECG monitoring or an event recorder is necessary to record and verify the tachycardia. Early detection and therapy of permanent tachycardias is mandatory to prevent left ventricular dysfunction and tachycardia induced cardiomyopathy [6].
Since the development of radiofrequency catheter ablation (RFA) as a new treatment option in the early 1990s, a definitive cure of the tachycardia can often be achieved [7]. With an overall, initial success rate of 91% and a low complication rate of 2.9% [6] this approach has become an accepted standard method in the management of pediatric patients suffering from SVT and fulfilling the following criteria [8]: signs of cardiomyopathy or cardiac impairment (as in our case), existence of a fast conducting pathway or frequent and bothersome episodes.
In conclusion, diagnosis of a SVT is often possible by the means of a clinical examination and an ECG. The prognosis of SVTs is good, in most of the patients it can be cured by RFA even in the presence of a tachycardia related cardiomyopathy. Nevertheless symptoms of a SVT can be unspecific and difficult to interpret, especially in children, and may be misinterpreted as neuro-psychiatric disorders. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Nair J, Ehimare U, Beitman BD, Nair SS, Lavin A. Clinical review: evidence-based diagnosis and treatment of ADHD in children. Missouri Medicine 2006; 103: 617-621. [PubMed]
- Katragadda S, Schubiner H. ADHD in children, adolescents and adults. Prim Care Clin Office Pract 2007; 34: 317-314. [CrossRef] [PubMed]
- Bauersfeld U, Pfammater J-P. Arrhythmien im Kindesalter. Ther Umsch 2004; 61: 245-249. [CrossRef] [PubMed]
- Vos P, Pulles-Heintzberger CFM, Delhaas T. Supraventricular tachycardia: an incidental diagnosis in infants and difficult to prove in children. Acta paediatr 2003; 92: 1058-1061. [CrossRef] [PubMed]
- Davignon A, Rautaharju P, Boisselle E, Soumis F, Megelas M, Choguette A. Normal ECG standards for infants and children. Pediatr Cardiol 1979/80; 1: 123-31. [CrossRef]
- Dubin AM, Van Hare GF. Radiofrequency catheter ablation: Indications and Complications. Pediatr Cardio 2000;21: 51-556. [CrossRef] [PubMed]
- Dick M, O-Connor BK, Serwer GA, LeRoy S, Armstrong B. Use of radiofrequency current to ablate accessory connections in children. Circulation 1991; 84: 2318-24. [CrossRef] [PubMed]
- Pfammatter J-P, Pavlovic M, Bauersfeld U. Impact of curative ablation on pharmacologic management in children with reentrant supraventricular tachycardias. International Journal of Cardiology 2004; 94: 279-282. [CrossRef] [PubMed]
- Lessmeier TJ, Gamperling D, Johnson-Liddon V, Fromm BS, Steinman RT, Meissner MD, Lehmann MH. Unrecognized paroxysmal supraventricular tachycardia. Potential for misdiagnosis as panic disorder. Arch Intern Med 1997; 157(5): 537-43. [CrossRef] [PubMed]
|
| Cite this article as: | | Anna C, Urs B, Guenter W, Christian B. Attention Deficit Hyperactivity Disorder- Would You Think of a Supraventricular Tachycardia. Pediatr Oncall J. 2008;5: 115-116. |
|