Right Lung Opacification – What is the diagnosis?
|
|
Right Lung Opacification – What is the diagnosis?
07/03/2018
07/03/2018
Ilechukwu GC, Kollannoor B, Abdulaziz M.
https://www.pediatriconcall.com/Journal/images/journal_cover.jpg
Ilechukwu GC, Kollannoor B, Abdulaziz M..
Department of Paediatrics, Whiston Hospital, Prescot, UK.
ADDRESS FOR CORRESPONDENCE
Dr Maysara Abdelaziz, Consultant Paediatrician, St Helens & Knowsley NHS trust, Warrington Road, Prescot, Liverpool L35 5DR, UK.
Email: Maysara.Aziz@sthk.nhs.uk |
Clinical Problem
A previously well, 7 week old baby presented to the paediatrics accident and emergency unit with a history of cough and fast breathing of one week duration associated with reduced oral intake of <50%. There was no fever. He was born in good condition at term by normal vaginal delivery with a birth weight of 2.77kg. He was unwell at 3 weeks of age and was admitted and treated with intravenous antibiotics. At that time his abdominal ultrasound (USG) was normal. On this presentation he was afebrile but in moderate respiratory distress (respiratory rate 60/min) with tracheal tug, intercostal retractions and head bobbing. Air entry was initially good on both sides but on later review was reduced on the right inframammary region. He was clinically suspected to have bronchiolitis and was started on intravenous fluids and chest x-ray was requested. Chest x-ray report showed extensive opacification of the right hemithorax with a small right pleural effusion. The right hemidiaphragm was not seen. There was suggestion of a subcarinal mass, splaying the carina with some atelectasis in the right upper lobe. The left hemithorax left hemidiaphragm were normal (Figure1). In view of the recent ultrasound scan showing normal right hemidiaphragm, congenital diaphragmatic hernia was excluded and a congenital cystic adenoid malformation was considered a likely diagnosis. A CT scan of the chest was advised (Figure 2).
Figure 1
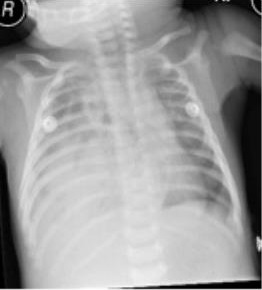
Figure 2
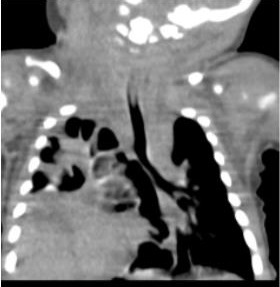
|
| |
What is the diagnosis? How to treat this patient?
|
|
|
Discussion
The CT chest (Figure 2) showed right diaphragmatic hernia with herniation of small bowel loops and part of the liver above the diaphragm, compressing the right lung anteriorly and further displacing the heart to the left. The left lung appeared normal.
Congenital diaphragmatic hernia (CDH) is defined as the presence of an orifice in the diaphragm, more commonly on the left than the right that allows the passage of intra-abdominal contents into the thorax. CDH occurs in less than 1-5:10,000 birth. (1) It seems to be slightly more frequent in males. (2,3) The commonest defect is the posterolateral (Bochdalek) type. More than 90% of the patients will be diagnosed during the antenatal period or will present with respiratory distress in the first few hours of life. In these cases diagnosis does not seem to pose any problems. However about 5-30% of CDH presents beyond the neonatal period. (4,5) CDH with mediastinal shift by hernia contents beyond the neonatal period is a rare but potentially a life threatening emergency. (6-8) In delayed presenting CDH the extent of herniation of the abdominal contents into the thorax may vary, leading to acute or intermittent symptoms. It is presumed that right-sided lesions present late as the liver offers some resistance to displacement of abdominal content into the thorax. A previously normal chest investigations has been reported in number of cases suggesting that in such cases the defects are confined by the hernia sac or obstructed by a solid organ. It is common for a misdiagnosis of primary lung disease to be made in cases of late diaphragmatic hernia. (6,9,10)
In our patient the initial diagnosis was bronchiolitis because of the clinical symptoms. The previous ultrasound, which showed intact diaphragm misled the clinical team who considered primary lung pathology, supported by the x-ray finding of extensive opacification of the right hemithorax. However non- resolution of symptoms raised the suspicion of CDH for which a CT chest was requested which clinched the diagnosis.
|
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
- Gallot D, Boda C, Ughetto S, Perthus I, Robert-Gnansia E, Francannet C, et al. Prenatal detection and outcome of congenital diaphragmatic hernia: a French registry-based study. Ultrasound Obstet Gynecol 2007; 29:276-283 [CrossRef] [PubMed]
- Torfs CP, Curry CJ, Bateson TF, Honore LH. A population-based study of congenital diaphragmatic hernia. Teratology 1992; 46:555-565 [CrossRef] [PubMed]
- Yang W, Carmichael SL, Harris JA, Shaw GM. Epidemiologic characteristics of congenital diaphragmatic hernia among 2.5 million California births, 1989-1997. Birth Defects Res A Clin Mol Teratol; 2006, 76:170-174 [CrossRef] [PubMed]
- Davenport M, Holmes K. Current management of congenital diaphragmatic hernia. Br J Hosp Med 1995;53:95–101 [PubMed]
- Elhalaby EA, Abo Sikeena MH. Delayed presentation of congenital diaphragmatic hernia. Pediatr Surg Int 2002;18:480-485 [CrossRef] [PubMed]
- Berman L, Stringer D, Ein SH, Shandling B. The late-presenting pediatric Bochdalek hernia: a 20-year review. J Pediatr Surg 1988;23:735-739 [CrossRef]
- Baglaj M. Late-presenting congenital diaphragmatic hernia in children: a clinical spectrum. Pediatr Surg Int 2004;20:658-669 [CrossRef] [PubMed]
- Baglaj M, Dorobisz U. Late-presenting congenital diaphragmatic hernia in children: a literature review. Pediatr Radiol 2005;35:478-488 [CrossRef] [PubMed]
- Fein JA, Loiselle J, Eberlein S, et al. Diaphragmatic hernia masquerading as pneumothorax in two toddlers. Ann Emerg Med 1993;22:1221–4. [CrossRef]
- Snyder HS, Salo DF, Kelly PH. Congenital diaphragmatic hernia presenting as massive gastrothorax. Ann Emerg Med 1990;19:562–4. [CrossRef]
|
|
| |
Cite this article as:
GC I, B K, M. A. Right Lung Opacification – What is the diagnosis?. Pediatr Oncall J. 2018;15: 121-122. doi: 10.7199/ped.oncall.2018.45
|