Mridula Arabu Manjunath, Pushpalatha Kariyappa, Sujatha Ramabhatta, Pavan Anilkumar Kittagaly, Kavya Shankar.
Department of Pediatrics, ESIC Medical College & Post Graduate Institute of Medical Sciences and Research, Bangalore, India.
ADDRESS FOR CORRESPONDENCE
Dr.Pushpalatha Kariyappa, #20, Sri Sai Mansion, 5th cross, Athmananda colony, RT Nagar, Bangalore 560032, India.
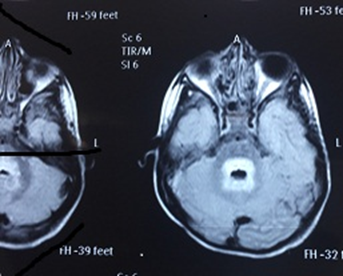
Email: dr.pushpalathaanil@yahoo.in | | Abstract | | Encephalitis is a common neuroinfection resulting in high mortality and morbidity in children. Bickerstaff Brainstem Encephalitis (BBE) is a rare immune mediated disorder considered to be one among the anti Gq1b syndromes. It is essentially a self-limiting disorder though intravenous immunoglobulin and plasmapheresis are known to hasten recovery. We report a case of BBE in a 3-year-old girl who presented with altered sensorium, ataxia, ophthalmoplegia, hypertonia and remained comatose for 15 days. MRI Brain showed typical findings of BBE. Child was treated with supportive measures and intravenous immunoglobulin. Child improved and recovered over a period of 5 months. | | | | Keywords | | BBE, ophthalmoplegia, ataxia | | | | Introduction | | Brainstem encephalitis is a rare condition seen in children due to varied etiologies such as infections, immune mediated and paraneoplastic disorders. Bickerstaff Brainstem Encephalitis (BBE) was first described by Bickerstaff and Cloake in 1950 when they presented 3 cases with a constellation of symptoms of acute ophthalmoplegia, ataxia and altered sensorium.1 The diagnostic criteria proposed for BBE were: (a) progressive, relatively symmetric ophthalmoplegia and ataxia by 4 weeks; (b) either consciousness disturbance or pyramidal signs; (c) limb strength of 5 or 4 on the Medical Research Council scale.2 BBE is an essentially self-limiting condition and undergoes spontaneous recovery, though sometimes there can be a grave presentation with varying degrees of altered sensorium. Review of literature show few cases of BBE in paediatric age group, from India.3 We present a 3 years old child with BBE who recovered after being comatose for 15 days. | | | | Case Report | A 3 years-old-girl was hospitalised with high grade continuous fever of 4 days associated with few episodes of non-projectile vomiting. On day 2 of hospitalization, she developed multiple episodes of decerebrate posturing with decreasing level of consciousness (Glasgow Coma Scale of 3/15) and hemodynamic instability requiring vasopressor support and mechanical ventilation. Neurological examination revealed bilateral pin point pupils, generalised hypertonia, hyperreflexia and extensor plantar response without signs of meningeal irritation. A differential diagnosis of bacterial meningitis/ viral encephalitis was made. Child was started on intravenous (IV) ceftriaxone and acyclovir. Investigations revealed anemia (hemoglobin 8.2 g/dl), leukopenia (total white cell count 2700 cells/cumm) and platelets of 1,60,000 cells/cumm. Cerebrospinal fluid (CSF) analysis was normal with cell count 0, sugar 55 mg/dl and protein 40 mg/dl. CSF PCR for Japanese Encephalitis, Herpes simplex, enterovirus and dengue were negative. No seizures were observed during the course of illness and child continued to have a GCS of 3-4 /15 for around 10 days. MRI brain done at 1 week showed signal changes around pons and mid-brain. In T2 weighted images, there were hyperintensities around medulla, posterior cerebellar peduncles and the walls of third and lateral ventricles, suggestive of brainstem encephalitis. (Figure 1). Considering possibility of BBE, serum for Anti Gq1B antibodies was done which was found to be negative. Child was treated with intravenous immunoglobulin (IVIG) 2 g/kg on day 7 of hospitalisation. She developed dystonia with vertical nystagmus on day 12 of hospitalisation. Sensorium gradually improved and she was weaned off ventilator after 15 days. A detailed neurological examination after extubation, revealed, bilateral ophthalmoplegia and ataxia, which fulfilled the criteria for diagnosis of BBE. She was discharged after 25 days of hospitalisation. At discharge child had mild ataxia and bilateral ophthalmoplegia. Dystonia had subsided and she was active and feeding well. Follow up at 5 months showed mild vertical nystagmus and ophthalmoplegia with no ataxia or dystonia.
Figure 1. MRI brain shows hyperintensities around medulla, posterior cerebellar peduncles and walls on T2 image.
| | | | Discussion | BBE is an immune mediated disorder. Antecedent illness is seen in almost 94% of cases with upper respiratory infection being most common.4 Campylobacter and Haemophilus Influenza seropositivity was also found in certain case control studies.5 Clinically, BBE is characterised by the presence of ataxia, bilateral ophthalmoplegia and altered sensorium. Absence of one of the above signs does not preclude the diagnosis of BBE.4 BBE is considered to be an illness at one end of the spectrum of conditions called AntiGq1B syndromes like Guillian Barre Syndrome (GBS) and Miller Fischer Syndrome (MFS).4 Altered sensorium is the main differentiating feature between BBE and MFS. The altered sensorium occurs in nearly 20% of cases.6 BBE is differentiated from GBS by the absence of peripheral neuropathy and the presence of pyramidal signs.6 Though BBE has a central pathology, in about 60% of cases it is found to be associated with absent or decreased reflexes.6 Albumino-cytological dissociation in the CSF is seen in 25% of cases of BBE.6 Other differential diagnosis for BBE include Wernicke’s encephalopathy, vascular disease involving the brainstem, multiple sclerosis, botulism and brainstem tumour.4 Typical MRI findings in BBE include high T2 signals with little enhancement in brainstem and basal ganglia as was seen in our patient. Typically these regions demonstrate minor restricted diffusion.4 Different studies have shown that anti Gq1B antibodies are present in BBE in 66 to 68% cases.6,7,8,9,10 In our patient, anti Gq1B antibodies were absent. However, the clinical criteria for BBE were fulfilled.
No specific guidelines are available for the treatment of BBE. Plasmapheresis, ivig therapy has been found to hasten the recovery.11 rituximab was found to bring about resolution in a resistant case of BBE.11 Patients with BBE often recover spontaneously, regaining the baseline functional status within 6 months of diagnosis in majority of cases as was seen in our patient.
| | | | Conclusion | | BBE needs to be considered as a differential diagnosis in cases presenting with altered sensorium with ataxia and ophthalmoplegia. Despite grave presentation and involvement of brainstem, complete spontaneous recovery is the norm. Hence supportive measures should be continued and possible therapeutic interventions tried in all cases. | | | | Contributor Statement | | MAM compiled the case report, PK and SR reviewed and edited the report, PAK and KS collected the data. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Bickerstaff ER. Brainstem Encephalitis: further observation on a grave syndrome with benign prognosis. Br Med J. 1957;1:1384-7 [CrossRef] [PubMed] [PMC free article]
- Bickerstaff ER. Brain stem encephalitis (Bickerstaff's encephalitis). In: Vinken PJ, Bruyn GW (eds). Handbook of clinical neurology. Vol. 34. Amsterdam: North-Holland. 1978; 605-609
- Kamate M, Chetal V, Patil P, Reddy L S, Hattehdi V. Bickerstaff Brainstem Encephalitis. Paediatr Oncall J. 2011; 8:100-101
- Odaka M, Yuki N, Hirata K. Anti-Gq1b IgG antibody syndrome. Clinical and immunological range. J Neurol Neurosurg Psychiatry. 2001;70:50-55. [CrossRef] [PubMed] [PMC free article]
- Shahrizailla N, Yuki N. Bickerstaff brainstem encephalitis and Fisher syndrome: anti-GQ1b antibody syndrome. J Neurol Neurosurg Psychiatry. 2013; 84:576–83. [CrossRef] [PubMed]
- Ito M, Kuwabara S, Odaka M, Misawa S, Koga M, Hirata K, et al. Bickerstaff's brainstem encephalitis and Fisher syndrome form a continuous spectrum: clinical analysis of 581 cases. J Neurol. 2008;255:674–682. [CrossRef] [PubMed]
- Bulakbasi N, Kocaoglu M. Central nervous system infections of virus family. Neuroimaging. Clin N Am.2008;18:53-84 [CrossRef] [PubMed]
- Koga M, Kusunoki S, Kaida K, Uehara R, Nakamura Y, Kohriyama T, et al. Nationwide survey of patients in Japan with Bickerstaff brainstem encephalitis: epidemiological and clinical characteristics. J Neurol Neurosurg Psychiatry. 2012;83:1210–1215. [CrossRef] [PubMed]
- Ju Yi Park, Kyong Og Ko, Jae Woo Lim, Eun Jung Cheon et al. A pediatric case of Bickerstaff's brainstem encephalitis. Korean J Pediatr. 2014; 57: 542–545. [CrossRef] [PubMed] [PMC free article]
- Shameem R, Sonpal N, Hamid M, Orsher S, Bhatia N, David M et al. Expert Opinion. Bickerstaff's Brainstem Encephalitis: A Rare Variant of the Anti-Gq1b Antibody Syndrome. Practical Neurology. 2013; Sept: 28-31
- TA Hardy. Severe Bickerstaff's encephalitis treated with Rituximab: serum and CSF GQ1b antibodies. J Neuroimmunol. 2012;251:107-9. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2019.46
|
| Cite this article as: | | Manjunath M A, Kariyappa P, Ramabhatta S, Kittagaly P A, Shankar K. Bickerstaff Brainstem Encephalitis - A Serious Disease with a Favourable Outcome. Pediatr Oncall J. 2019;16: 86-87. doi: 10.7199/ped.oncall.2019.46 |
|