Shantanu Gupta, Sumant Patil, Rashmi Gapchup.
Department of Pediatrics, Deenanath Mangeshkar Hospital, Pune 411004, India.
ADDRESS FOR CORRESPONDENCE
Sumant Patil, MD, MRCPCH(UK), DCH(UK), In-Charge Pediatric Intensivist, Department of Pediatrics, Deenanath Mangeshkar Hospital, Pune 411004, India.
Email: sumantsp22@gmail.com | | Abstract | | Squirrels are common rodents in rural and urban areas of India. They may seem adorable and even friendly but are not completely harmless. Though mostly squirrel bites are associated with insignificant clinical course, we present a 14-year-old male with a history of provoked squirrel bite leading to necrotizing fasciitis and compartment syndrome of lower limb requiring fasciotomy, treatment with intravenous antibiotics and finally local wound debridement. | | | | Keywords | | Squirrel bite, necrotizing fasciitis, antirabies prophylaxis, fasciotomy | | | | Introduction | | Squirrel bite is amongst the uncommon animal bites seen in medical practice. Mostly these are provoked bites while trying to feed or handle them. While most of these bites do not lead to complicated course1, some case reports had been published notifying association of squirrel bite with tularemia2, typhus3 and syndrome resembling rat bite fever.4 To our knowledge, necrotizing fasciitis as a presentation of squirrel bite has not been documented before. | | | | Case Report | A 14-year-old male was referred to our hospital with history of provoked squirrel bite over dorsum of left foot while trying to dress the injured leg of squirrel. Child developed intense swelling of affected limb and received emergency treatment at local hospital in the form of intramuscular (IM) adrenaline and intravenous (IV) hydrocortisone for suspected anaphylaxis. On admission to pediatric intensive care unit (PICU), he had severe pain and swelling over left lower limb. On examination he was febrile, pulse was 112/min, respiratory rate was 22/min and blood pressure was 118/70 mm Hg. Systemic examination was normal. On local examination of left lower limb, there was a bite mark over dorsum of left foot surrounded by intense erythema, swelling, severe tenderness and raised local temperature. Swelling extended till mid-thigh. Dorsalis pedis and posterior tibial artery pulsations were present but feeble. Investigations revealed neutrophilic leukocytosis (white cell count -14,700 cells/cumm with 90% polymorphs) with thrombocytopenia (platelets 99,000 cells/cumm), negative C- reactive protein (CRP), normal liver and renal functions tests and deranged coagulation with prothrombin time (PT) >180 sec, activated partial thromboplastin time (APTT) 39.6 sec (control 26.1 sec) and hypofibrinogenemia (fibrinogen - 122 mg/dl) . Twenty mins whole blood clotting test was negative. Emergency doppler of the left lower limb revealed normal flow in arterial tree with patchy flow in left sapheno-femoral junction, left popliteal and posterior tibial veins. Child was started on IV antibiotics (ceftriaxone and amikacin) after taking blood culture. On admission, IV hydrocortisone (100 mg), IM adrenaline (0.5 ml of 1:1000 dilution) and IV chlorpheniramine was given. He received anti rabies prophylaxis (post exposure prophylaxis with Inj. Rabipur - 1 ml IM on day 0, 3, 7 and 14) and tetanus toxoid (0.5 ml IM). Fresh frozen plasma (FFP) transfusion was given in view of deranged coagulation. Within 24 hours of admission, swelling and tenderness increased significantly with restriction of movements (Figure 1). IV clindamycin was added for worsening local inflammatory reaction. An urgent surgical intervention in the form of fasciotomy (Figure 2) was performed for evolving compartment syndrome, under cover of ffp and cryoprecipitate transfusions. Tissue culture sent from affected limb grew staphylococcus equorum. Within 2 days after fasciotomy, child improved symptomatically. Movements of affected limb improved with physiotherapy. Subsequently he developed necrotic wound around the bite mark extending deep upto muscles which required local wound debridement. Child was discharged after 10 days of hospitalization.
Figure 1. Local inflammatory reaction on admission
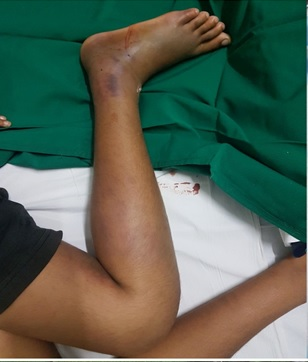
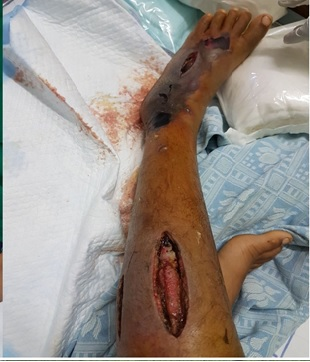
Figure 2. Fasciotomy site with evolving necrosis on left foot.
| | | | Discussion | | The most common variety of squirrel seen in India is Palm or Striped squirrel belonging to genus Funambulus. Giant squirrels belonging to genus Ratufa are also common in India. Ratufa indica (endemic species) are also known as Malabar giant squirrel because of their common occurrence in Western Ghats.5 Few case reports had been published in the past on squirrel bite and transmission of human infections. In India, a case of 7-year-old boy presenting with rabies after 2 months of squirrel bite was reported.6 In United States, grey squirrels (Scirus cardinensis) had been implicated in transmission of tularemia2 and flying squirrels (Glaucomys volans) in transmission of typhus.3 A syndrome resembling rat bite fever caused by Streptobacillus moniliformis and Spirillium minus had been reported following bite by red-legged ground squirrel (Xerus erythropus) in Nigeria.4 A recent short report of 35 incidences of squirrel bites over 5-year period in Thailand showed no serious systemic or local complications where all patients received routine wound care and anti-rabies prophylaxis.7 Squirrel involved in the bite of our patient could not be identified. Tissue culture from the affected part grew staphylococcus equorum, a coagulase negative staphylococcus which is not seen as a skin commensal in humans and rarely isolated in human clinical specimens. Therefore, this case report demonstrates an unusual presentation of squirrel bite and clinicians should be aware of exaggerated local inflammatory response to a squirrel bite apart from risk of rabies. | | | | Conclusion | | Necrotizing fasciitis is a serious complication of squirrel bite which can lead to severe local reactions and must be kept in mind while treating it promptly to avoid further complications. | | | | Acknowledgement | | SP identified and conceptualized the topic. SG drafted the first draft of the manuscript. SP and RG contributed substantially to its revision. SP takes responsibility for the paper as a whole. The final copy of the manuscript has been approved by all the authors. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Wyatt JP. Squirrel bites [letter]. BMJ.1994;309:1694. [CrossRef] [PubMed] [PMC free article]
- Magee JS, Steele RW, Kelly NR, Jacobs RF. Tularemia transmitted by a squirrel bite. Pediatr Infect Dis J. 1989;8:123-5
- McDade JE. Flying squirrels and their ectoparasites: disseminators of epidemic typhus. Parasitol Today. 1987;3:85-7 [CrossRef]
- Gray HH. Squirrel bite fever. Trans R Soc Trop Med Hyg. 1967;61:857. [CrossRef]
- Mehta P. Is the giant squirrel really of least concerns? WWF - India Newsletter July - September 2012 Page 14. Available at URL: https://www.rufford.org/files/WWF%20-%20INDIA%20NEWSLETTER%20JULY-%20SEPTEMBER%202012.pdf. Accessed on 24th November 2019
- Kumari PL, Mohanan KR, Kailas L, Chacko KP. A case of rabies after squirrel bite. Indian J Pediatr. 2014;81:198 [CrossRef] [PubMed]
- Sriwiijittalai W, Wiwanitkit V. Squirrel bite: Analysis of 35 case. Ann Trop Med Public Health. 2017; 10:478 [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2020.11
|
| Cite this article as: | | Gupta S, Patil S, Gapchup R. Squirrel bite leading to Necrotizing Fasciitis. Pediatr Oncall J. 2020;17: 19-20. doi: 10.7199/ped.oncall.2020.11 |
|