D.T.N. Paul, Tania Chakraborty, Debashish Bandyopadhyay.
Department of Pediatrics, B R Singh Hospital & Centre for Medical Education and Research, Kolkata, India.
ADDRESS FOR CORRESPONDENCE
Tania Chakraborty, Senior Resident, Department of Pediatrics, B.R.Singh Railway Hospital, Parikshit Roy Lane, Sealdah, Kolkata 700014.
Email: taniachakraborty@ymail.com | | Abstract | | A 4-month-old male infant presented with a severe desquamating rash involving the face, extremities, perianal and perioral region which was followed by persistent lower respiratory tract infection. Investigations revealed a low serum zinc level and a positive sweat chloride test. In this case, we aim to emphasize that although cystic fibrosis in children usually presents with respiratory and gastrointestinal manifestations, mucocutaneous involvement could be a rare feature of this multisystemic disorder. | | | | Keywords | | Cystic fibrosis, acrodermatitis enteropathica, zinc, malabsorption | | | | Introduction | Acrodermatitis enteropathica is classically a rare autosomal recessive disorder caused by malabsorption of zinc, usually manifesting as a cutaneous eruption of eczematous, dry, scaly lesions in perioral, acral, perineal areas, knees and elbows.1 Acquired zinc deficiency can result from low nutritional intake, malabsorption, excessive loss of zinc, or a combination of these factors.2 Transient deficiency can occur in preterm infants due to their greater demand and low body stores. Also, in full-term breast-fed infants, deficiency may result from low maternal serum, zinc levels or defective mammary zinc secretion.2 Rapid response is seen on starting zinc supplementation, especially in acquired cases.2
Cystic fibrosis is an inherited multisystem disorder of children and adults. It usually presents with pulmonary and gastrointestinal manifestations.3 There are case reports with cutaneous manifestations mostly in European and American population.4,5
We present a 4-month-old child who presented initially with acrodermatitis enteropathica and later with pulmonary manifestations and was finally diagnosed as cystic fibrosis. | | | | Case Report | A 4-month-old male child, born to non-consanguineous parents, presented with 8-10 episodes of loose stools and rash for 3 days. There was no fever. Child was exclusively breastfed and was delivered by normal vaginal delivery at 38 weeks of gestation and had a birth weight of 2.8 kg. Milestones were normal and immunization was complete as per age as per the universal immunization programme (UIP) schedule. On admission, weight was 4.9 kg (<3rd centile as per Indian Academy of Pediatrics (IAP) growth charts), length 62 cm (3rd–50th centile, IAP growth charts), head circumference 38cm (<3rd centile, IAP growth charts). On examination, dry desquamating, erythematous rash was present periorally, over the neck, upper and lower limbs, and perianal region (figure 1). Child was normothermic, irritable and had sunken anterior fontanelle with normal skin turgor suggestive of some dehydration. Pulse was feeble with a rate of 110/min, blood pressure was 90/60 mm of Hg and respiratory rate was 56/min. On systemic examination, he had hepatomegaly. Investigations showed hemoglobin 10.9 g/dl, white cell count 11,500 cells/cumm (polymorphs 60%, lymphocytes 34%, eosinophils 3%, monocytes 2%, basophils 1%) and platelets 2,10,000 cells/cumm. Serum zinc was 32 mcg/dl (Normal 66-110 mcg/dl). TORCH IgM & IgG were negative. Dehydration was corrected with intravenous fluids and replacement of ongoing losses was done by oral fluids. Oral zinc supplementation was given at 1 mg/kg/day. After 5 days, rash and loose stools subsided, and child was discharged from the hospital on oral zinc supplementation. Child was readmitted after 10 days with a cough and respiratory distress for 4 days. There was no fever. On examination, child was tachypneic with lower chest retractions, the upper respiratory tract was normal. Chest x-ray showed bilateral hazy opacities with hyperinflation. CT chest showed diffuse ground glass opacity in both lungs (Figure 2). Arterial blood gas (ABG) showed pH 7.37, pCO2 41, pO2 62, bicarbonate 23.7 mmol/L and oxygen saturation of 83% in room air. Serum sodium was 127 mEq/L and potassium was 3.7 mEq/L. Blood culture did not grow any organism. Mantoux test with 2TU was negative and gastric aspirate was negative for Mycobacterium tuberculosis. Initial diagnosis of viral bronchiolitis was made, and child was given oxygen and nebulization with 3% hypertonic saline and levo-salbutamol. He responded initially and worsened later with a waxing and waning course for 14 days. An underlying immunodeficiency was suspected. HIV Elisa of parents was negative. Serum immunoglobulins were normal. Sweat chloride was 87 mEq/l and 91 mEq/l done on two separate days (sweat chloride > 60mEq/L is suggestive of cystic fibrosis). Specific mutational analysis for delta F508 was negative. Further screening for other mutations for cystic fibrosis could not be done due to financial constraints. He was treated with oral azithromycin, nebulization with 3% hypertonic saline, budesonide, levo-salbutamol, and 10% acetylcysteine solution along with chest physiotherapy and fat-soluble vitamins and pancreatic enzymes supplementation to which he responded. On follow-up after 6 months the child was gaining weight (7.6 kg) head circumference (41 cm) and length (67 cm).
Figure 1. Acrodermatitis enteropathica.
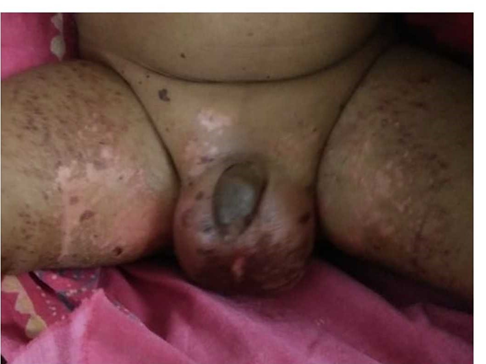
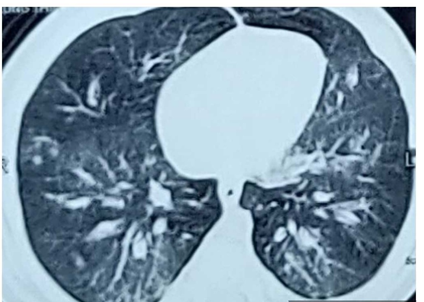
Figure 2. CT Thorax showed diffuse ground glass opacity in both lungs.
| | | | Discussion | The clinical manifestations of cystic fibrosis are variable. The usual manifestations are meconium ileus in the neonatal period, recurrent bronchiolitis in infancy and early childhood, recurrent lower respiratory tract infections, chronic lung disease, bronchiectasis, failure to thrive, steatorrhea and rectal prolapse.6 Older patients may present with pancreatic insufficiency and male infertility due to azoospermia.6 Pancreatic insufficiency is usually more severe in Indian scenario, may be due to delayed diagnosis6. The gene for cystic fibrosis has been identified in chromosome 7.7 Among the Caucasian population, Delta F508 mutation is the commonest and found in 70% of the population.7 The exact incidence of various mutations in Indian population is lacking.7 However, a study conducted by Kabra et al at AIIMS, Delhi has shown that the frequency of delta F508 mutation in the Indian population was 19%, which is much lower than the Caucasian population.7 Around 1000 mutations have been identified till date and the frequency of mutations varies according to geographic regions.7 Conventionally, the diagnosis of cystic fibrosis is confirmed by the presence of typical phenotype and abnormal sweat chloride values on more than one occasion. Values of sweat chloride >60 mEq/L are considered abnormal and values between 40-60 mEq/L are considered equivocal and repeat testing is recommended in presence of supportive clinical features. Average sweat chloride values in cystic fibrosis children is 100 mEq/L and in Indian children, around 90 mEq/L.6 Similar values of sweat chlorides were seen in our patient. Blood biochemistry work-up in cystic fibrosis children usually shows a low or low normal sodium, metabolic alkalosis and hypochloremia. Anemia and hypoalbuminemia, even ascites may occur due to vitamin E deficiency and protein malabsorption.6
Acrodermatitis enteropathica is a rare autosomal recessive disorder due to decreased absorption of zinc from the diet.1 The inherited variety results from defect in zinc-specific transporter gene SLC39A4.1 Usually manifestation develops after weaning from breast milk to cow’s milk.1 Acquired zinc deficiency is more prevalent and may present with similar clinical manifestations.2 Signs and symptoms in infancy include periorificial and acral dermatitis, diarrhea, behavioral changes and neurologic disturbances. Older children may present with failure to thrive, anorexia, alopecia, nail dystrophy and repeated infections.2
Maternal milk has got protective action as it has zinc ligands which increase zinc absorption and hence masks the clinical features due to inherited deficiency of the transport protein. However, in children who are fed with breast-milk poor in zinc, may present with transient deficiency of this micronutrient. Hence mothers who breastfeed their babies must be kept on zinc supplementation until weaning.8 We did not assess maternal serum zinc level and as the clinical manifestations improved with zinc supplementation, the deficiency was considered secondary to malabsorptive process due to cystic fibrosis. Recently Yarmuch et al9 and Patrizi et al10 have described acrodermatitis enteropathica as initial manifestation of cystic fibrosis.
In conclusion children with cystic fibrosis can present with dermatological manifestations, which is a part malabsorptive process of the disease10 that may lead to hypoproteinemia, zinc and essential fatty acid deficiency. Cystic fibrosis should be considered as a differential diagnosis in children presenting with cutaneous exanthema and malnutrition. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Joyce JC. Nutritional Dermatoses In: Kliegman RM, Stanton BF, Geme JWS, Schor NF (eds.) Nelson Textbook of Pediatrics. 20th ed. Philadelphia. Elsevier. 2016: 3238-9
- Subramanian KNS. Pediatric acrodermatitis enteropathica. Available at URL: https://emedicine.medscape.com/article/912075-overview. Accessed on 19th September 2019.
- Egan ME. Cystic fibrosis. In: Kliegman RM, Stanton BF, Geme JWS, Schor NF. (eds.) Nelson Textbook of Paediatrics. 20th ed. Philadelphia. Elsevier. 2016: 2098-2112
- Crone J, Huber WD, Eichler I, Granditsch G. Acrodermatitis enteropathica-like eruption as the presenting sign of cystic fibrosis--case report and review of the literature. Eur J Pediatr. 2002;161:475-478. [CrossRef] [PubMed]
- Massie J. Re: acrodermatitis enteropathica -like eruption and failure to thrive as presenting signs of cystic fibrosis. J Am Acad Dermatol. 2008;59:720-1. [CrossRef] [PubMed]
- Ahuja AS, Kabra SK. Cystic fibrosis: Indian experience. Indian Pediatr. 2002;39:813-818
- Kabra SK, Kabra M, Lodha R, Shastri S, Ghosh M, Pandey RM et al. Clinical profile and frequency of delta f508 mutation in Indian children with cystic fibrosis. Indian Pediatr. 2003;40:612-619.
- Ciampo IRLD, Sawamura R, Ciampo LAD, Fernandes MIM. Acrodermatitis enteropathica: clinical manifestations and pediatric diagnosis. Rev Paul Pediatr. 2018;36:238-241. [CrossRef] [PubMed] [PMC free article]
- Yarmuch GP, Chaparro RX, Fischer SC. [Cutaneous manifestations of cystic fibrosis in an infant: acrodermatitis enteropathica and gray hair]. Rev Chil Pediatr. 2015;86:52-55. [CrossRef] [PubMed]
- Patrizi A, Bianchi F, Neri I, Specchia F. Acrodermatitis enteropathica-like eruption: a sign of malabsorption in cystic fibrosis. Pediatr Dermatol. 2003;20:187-188. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2020.35
|
| Cite this article as: | | Paul D, Chakraborty T, Bandyopadhyay D. Cystic fibrosis presenting with Atypical skin rash in an infant. Pediatr Oncall J. 2020;17: 85-87. doi: 10.7199/ped.oncall.2020.35 |
|