Pink Hematuria in an Infant
|
|
Pink Hematuria in an Infant
22/12/2020
22/12/2020
https://www.pediatriconcall.com/Journal/images/journal_cover.jpg
Mohammed Azar, Aryn Jaitley.
Department of Paediatrics, Altnagelvin Area Hospital, Londonderry, United Kingdom.
ADDRESS FOR CORRESPONDENCE
Mohammed Azar, MBBS, MD (Paediatrics), MRCPCH, Fellowship (Paeds Nephrology), CCT/CESR (UK), Consultant Paediatric Nephrologist, Department of Pediatrics, Altnagelvin Area Hospital, Londonderry, United Kingdom.
Email: shammemazar@gmail.com
Hemorrhagic cystitis, Adenovirus, Hematuria
|
Clinical Problem
An 8 months old girl born of non-consanguineous marriage presented with two weeks history of bright blood spotting in her nappy. These episodes were intermittent with 3-4 episodes per week with multiple episodes in a day (Figure 1). There was no fever, excessive crying on micturition or drug intake. Family history was non-contributory. She had diarrhea one week prior to the onset of these symptoms. There was no trauma or history of bleeding from other sites. On examination, her growth was appropriate, blood pressure and systemic examination were normal. An examination of the genitalia showed no evidence of laceration or injury to the labia majora, minora or hymen respectively and no anal-fissures were visible. Urinalysis showed red blood cells (RBC) +++ and few pus cells. Urine culture did not grow any organism. Urine calcium/creatinine ratio was normal (0.09 mmol/mmol). There was no proteinuria. Her full blood counts, blood film, creatinine kinase, renal function, electrolytes, liver function and coagulation profile were normal. A renal ultrasound showed no evidence of any renal or bladder mass. She was managed conservatively and her haematuria completely subsided after three weeks.
|
Figure 1. Blood spot on the nappy
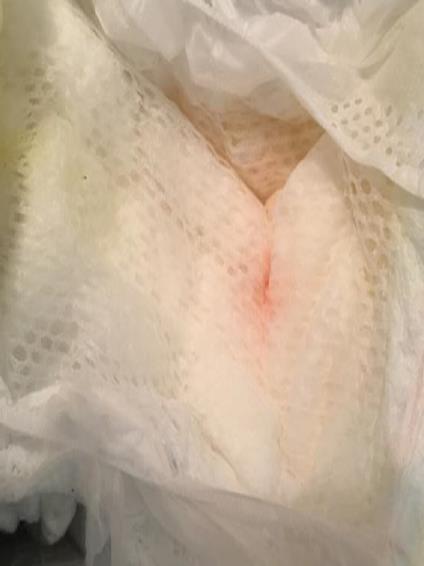
|
| |
What is the cause of her haematuria?
|
|
|
Discussion
Her pink haematuria was thought to be likely due to virus induced haemorrhagic cystitis. Urine and blood viral PCR (polymerase chain reaction) picked up adenovirus. Urine for cytomegalovirus and polyoma viruses were negative. Other blood viral PCR (cytomegalovirus, Epstein-Barr, parvovirus, rhino, parainfluenza, respiratory syncytial, influenza, Boca, metapneumo were negative. Haemorrhagic cystitis is coined by the presence of bright pink haematuria and lower urinary tract symptoms, such as dysuria, frequency, or urgency. It is most commonly caused by viruses. The most common encountered viruses are adenovirus, cytomegalovirus, and polyomaviruses.1 Adenovirus, particularly serotypes 11 and 21 of subgroup B are the common among children.1,2 Drugs also play an important etiological factor namely cyclophosphamide, ifosfamide and radiation therapy. Moreover, children on immunosuppressive drugs are prone to have haemorrhagic cystitis.3 Usually diagnosis is confirmed by PCR sequencing of urine.4 The differential diagnosis of pink haematuria could be urinary tract infection, kidney stones, bladder, urethral injury, and sexual abuse. Moreover, history of preceding diarrhoea may give clue to virus induced cystitis. The treatment of virus induced haemorrhagic cystitis is conservative as it generally spontaneously resolves within few days, However if it is persistent or is causing bladder outlet obstruction, then referral to urologist for cystoscopy and bladder irrigation may be required.5
|
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
- Gorczynska E, Turkiewicz D, Rybka K, Kalwak K, Dyla A, Szczyra Z, et al. Incidence, clinical outcome, and management of virus-induced haemorrhagic cystitis in children and adolescents after allogeneic hematopoietic cell transplantation. Biol. Blood Marrow Transplant. 2005;11:797-804 [CrossRef] [PubMed]
- Decker DB, Karam JA, Wilcox DT. Pediatric haemorrhagic cystitis. J Pediatr Urol. 2009; 5: 254-264 [CrossRef] [PubMed]
- Saito Y, Kumamoto T, Makino Y, Tamai I, Ogawa C, Terakado H. A retrospective study of treatment and prophylaxis of ifosfamide-induced hemorrhagic cystitis in pediatric and adolescent and young adult (AYA) patients with solid tumors. Jpn J Clin Oncol. 2016;46(9):856-861. [CrossRef] [PubMed]
- Hemorrhagic Cystitis. Available from URL: https://en.wikipedia.org/wiki/Hemorrhagic_cystitis. Accessed on 2nd Sept 2020
- Hemorrhagic Cystitis. Available from URL: https://emedicine.medscape.com/article/2056130-overview. Accessed on 2nd Sept 2020
|
|
| |
Cite this article as:
Azar M, Jaitley A. Pink Hematuria in an Infant. Pediatr Oncall J. 2020;17: 143-144. doi: 10.7199/ped.oncall.2020.52
|