Sara Todo Bom Costa1, Graça Lopes2.
1Department of Pediatrics, Hospital Santa Maria, Central Hospital University of North Lisbon, Portugal,
2Department of Pediatric Orthopedics, Hospital Santa Maria, Central Hospital University of North Lisbon, Portugal.
ADDRESS FOR CORRESPONDENCE
Sara Todo Bom Ferreira da Costa, Department of Pediatrics, Hospital Santa Maria, Centro Hospitalar Universitário Lisboa Norte, Av. Prof. Egas Moniz MB, 1649-028 Lisboa.
Email: sara.tbferreiracosta@gmail.com | | Keywords | | Emergency Service, Hospital, Hip Dislocation, Congenital, Infant | | | A 3-month-old girl, with a history of breech presentation, was brought to the Emergency Department (ED) after she fell from her father’s lap. The fall caused traction of her left lower limb and resulted in pain and decreased mobility. At the ED she was observed by two specialties: pediatrics and orthopedics. Her lower left limb was flexed and in abduction, with normal passive movement and limited active movement. There was no limited abduction of the hip and the Ortolani reduction test was negative. Limb length discrepancy was absent. A hip radiograph was performed. There were no radiological signs of fracture or subluxation of the left hip. The child was admitted and remained in the observation room (OR) for 24 hours for close monitoring and pain relief. She was then discharged and referred to an Orthopedics consultation for follow up.
At the consultation, a more detailed observation detected a limb length discrepancy and limited abduction of the right hip. An ultrasound confirmed right hip dislocation. A careful review of the radiograph performed on the ED, confirmed pre-existing signs of DDH of the right hip, which were overlooked (Figure 1). The patient was then treated conservatively with an abduction orthosis and now shows a promising evolution.
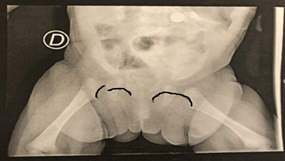
Figure 1. Bilateral Hip X-ray of the patient that shows a disrupted Shenton's line.
Developmental dysplasia of the hip (DDH) comprises a wide spectrum of pathologic conditions, that includes neonatal instability, acetabular dysplasia, hip subluxation and dislocation. It usually occurs due to abnormal growth of the hip.1 Clinical screening for DDH is done through the Ortolani reduction test and the Barlow test in newborns, while infants present other clinical signs.2 In infants, DDH should be suspected when limb length discrepancy, limited hip abduction (the most important sign after 3 months) and/or the Galeazzi sign are present.1,2,3 This screening is typically done at routine consultations. Children with positive findings and/or known risk factors require further investigation and referral to an Orthopedics consultation. Every observation, even during Emergency Department (ED) visits, should be considered an opportunity for screening, as an early detection can influence patient outcome. In Portugal, it has been defined by the Sociedade Portuguesa de Ortopedia e Traumatologia (SPOT) that radiological screening of DDH should be performed in the presence of hip instability (detected by clinical examination) or risk factors.3 Risk factors include a positive family history of DDH, breech presentation, history of oligohydramnios, congenital torticollis, congenital deformities of the foot, limb malformation and asymmetrical buttock creases.3 In our patient, the child had a risk factor, but no radiological screening was performed, which was a missed opportunity for diagnosis. If there is an early suspicion of dislocation or instability, an ultrasound (USG) of the hip is performed between the age of 4 to 6 weeks.3 After four to six months of life, the hip radiograph is the main method of evaluating the development of the hip.1 In our patient, we can see a disrupted Shenton´s line, a sign of DDH (Figure 1). If radiological findings confirm DDH, the child is then referred to an Orthopedics consultation. Treatment can be conservative or surgical. In the presence of a subluxated or dislocated hip, the objective is to obtain a concentric and stable reduction without forceful abduction.1 Abduction orthoses are used in the treatment of DHH in newborns and infants, while older children may require leg casting. Surgical management is considered when initial treatment has failed. The patient presented a favorable evolution with orthoses. An untreated hip dislocation can lead to poor function and early-onset osteoarthritis, which may require a total hip arthroplasty at a young age.2 Therefore, early diagnosis is of extreme importance.
Emergency healthcare systems worldwide are under intense pressure from ever-increasing demand.4 Emergency medicine (EM) is especially prone to diagnostic error. The high workload, time pressure, simultaneous events competing for attention and life-threatening consequences of misdiagnosis are all contributing factors.5 Mistakes in the assessment of radiographs are a known source of diagnostic error.6 This patient’s DDH could have been diagnosed if the physicians had had the time to look at the patient as a whole, instead of exclusively focusing on the complaint that brought the child to the ED and overlooking the changes of the right hip on the exam. Several unique factors influence diagnostic errors in pediatrics. These include patient/caregiver interaction, training of physicians and workflow.7 It is believed that close follow-up of patients and access to electronic medical records may help prevent error, and knowing the outcomes of the patients that are misdiagnosed can provide useful feedback.7 Referral to a consultation was important to identify the misdiagnosis, and helped track down the evolution of this patient, providing important feedback. It also revealed that an USG should have already been performed at 4 to 6 weeks of age, given the known risk factor.
Clinicians are not comfortable discussing diagnostic errors. These discussions should take place in a nonpunitive environment and physicians should accept accountability for what is within their control.8 The discussion of cases among peers might provide useful feedback that can potentially allow clinicians to improve their diagnostic methods. This case should be regarded as a learning opportunity. Missed diagnosis occur and should be demystified and reported to help the medical community improve diagnostic approaches. Hopefully this article will also bring attention to a common problem that affects ED physicians – the overcrowding of the ED and time pressure associated with it, that limits correct patient observation. This issue should be addressed with policy-makers and health system managers as it is vital to implement changes to the health system to ensure optimal work conditions and empower medical professionals.
Ethical statement/patient consent:
The subject (or their parents/guardians) has given their written informed consent to publish the case. There is no information that might reveal the subject’s identity.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Vaquero-Picado A, González-Morán G, Garay EG, Moraleda L. Developmental dysplasia of the hip: update of management. EFORT Open Rev. 2019;4:548-556. [CrossRef]
- Wenger D, Düppe H, Nilsson JÅ, Tiderius CJ. Incidence of Late-Diagnosed Hip Dislocation After Universal Clinical Screening in Sweden. JAMA Netw Open. 2019;2:e1914779 [CrossRef]
- Pereira C, Pinto M, Sant'Anna F. Displasia de desenvolvimento da anca: na perspetiva do pediatra. Nascer e Crescer. 2016;15:236-240.
- Cooper A, Davies F, Edwards M, Anderson P, Carson-Stevens A, Cooke MW, et al. The impact of general practitioners working in or alongside emergency departments: a rapid realist review. BMJ Open. 2019;9:e024501 [CrossRef]
- Hautz WE, Kämmer JE, Hautz SC, Sauter TC, Zwaan L, Exadaktylos AK, et al. Diagnostic error increases mortality and length of hospital stay in patients presenting through the emergency room. Scand J Trauma Resusc Emerg Med. 2019;27:54. [CrossRef]
- Mattsson B, Ertman D, Exadaktylos AK, Martinolli L, Hautz WE. Now you see me: a pragmatic cohort study comparing first and final radiological diagnoses in the emergency department. BMJ Open. 2018;8:e020230 [CrossRef]
- Singh H, Thomas EJ, Wilson L, Kelly PA, Pietz K, Elkeeb D, et al. Errors of diagnosis in pediatric practice: a multisite survey. Pediatrics. 2010;126:70‐79. [CrossRef]
- Grubenhoff JA, Ziniel SI, Cifra CL, Singhal G, McClead RE Jr, Singh H. Pediatric Clinician Comfort Discussing Diagnostic Errors for Improving Patient Safety: A Survey. Pediatr Qual Saf. 2020;5:e259. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2022.32
|
| Cite this article as: | | Costa S T B, Lopes G. Are Emergency Department Visits Missed Opportunities for Secondary Diagnosis?. Pediatr Oncall J. 2022;19: 97-98. doi: 10.7199/ped.oncall.2022.32 |
|