Jagdish Kathwate.
Department of Pediatrics, Motherhood Hospital, Pune, Maharashtra, India.
ADDRESS FOR CORRESPONDENCE
Dr Jagdish Kathwate, Department of Pediatrics, Motherhood Hospital, Mundhwa - Kharadi Rd, Kharadi, Pune, Maharashtra 411014, India.
Email: docjagdishkat@gmail.com | | Abstract | | Lymphadenitis is common in primary Tuberculosis (TB) in children and they may be asymptomatic during the non-suppurative lymphadenitis phase. Intrathoracic nodes may compress one of the bronchus leading to atelectasis, lung infection and bronchiectasis or thoracic duct leading to chylous effusion. Other intrathoracic complications include dysphagia, oesophago-mediastinal fistula, tracheo-oesophageal fistula, biliary obstruction and cardiac tamponade. Though mediastinal tubercular lymphadenitis (MTL) is common in developing countries, encasement of aorta by it is extremely rare. We report an eight-year-old girl who presented with non-healing right axillary lymphadenitis, later diagnosed to have MTL and found to have complete aortic encasement. | | | | Keywords | | Mediastinal tubercular lymphadenitis, Aorta encasement, children. | | | | Introduction | | Lymphadenitis is the most common extrapulmonary manifestation of tuberculosis (TB) accounting for 35% of cases.1 It is generally characterized by conglomerates, localized in multiple sites mostly in the right paratracheal, hilar and subcarinal areas, with an inhomogeneous CT enhancement pattern and associated with lung infiltrate in 90% of cases.2 Tuberculous involvement of the ascending aorta is rare, even in a country like India where the burden of TB is enormous, and here we have reported a case of complete encasement of aorta by enlarged MTL which is a first report of an ascending aortic encasement. | | | | Case Report | An 8-year-old girl presented with non-healing right axillary abscess with persistent discharging for 6 months. She was on anti-tuberculous therapy (ATT) for 10 months as she was detected to have primary complex on chest X-ray with positive tuberculin skin test (TST) and fever. After one month of ATT, she developed pericardial effusion with tamponade requiring pericardiocentesis. She also had bilateral pleural effusion and ascites. Pericardial fluid did not grow any organism on culture and TB culture was also negative. Her ATT had been continued and steroids were added. After 5 months of ATT, she developed a right axillary cold abscess. Incision and drainage were done and streptomycin and linezolid were added. The smear showed presence of acid-fast bacilli (AFB). streptomycin was stopped within a month and amikacin and levofloxacin was started which was given for 3 months. Echocardiography was repeated which was normal. On presentation to us, her weight was 16.6 kg, she had pallor and persistent discharging sinus in the right axilla. Blood pressure in upper limbs were 90/40 mm of Hg and that in lower limbs were 120/60 mm of Hg. On systemic examination, she had a systolic murmur at the apex. Other systems were normal. A repeat echocardiography showed solidified collection in the superior mediastinum completing encasing aorta and main pulmonary artery causing constriction with a peak gradient of 23 mm of Hg across it. CT chest showed patchy areas of consolidation in apical segment of right upper lobe and lower lobe and nodular opacities in adjacent lung with localized pleural effusion, pleural thickening on right side and calcified mediastinal and abdominal lymphnodes. (Figure 1) HIV Elisa was negative. On view of clinical suspicion of drug resistant TB, 2nd line ATT consisting of amikacin, moxifloxacin, ethionamide, pas, cycloserine were started along with prednisolone (1 mg/kg/day). Parents were asked to send the pus from the axilla for TB culture, but did not send the same. Child was given total 18 months of this ATT regime (amikacin was given for 6 months). There was no adverse effect to the ATT. Her lymphnodes completely regressed in 1 year and echocardiography was normal after 12 months of this ATT. Her ATT was stopped after 18 months (after CT chest showing complete resolution of the glands). She is on regular follow up and doing well.
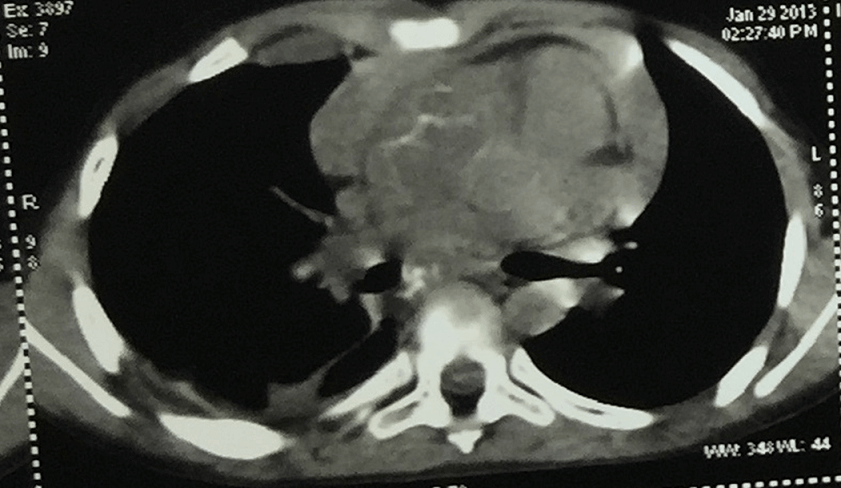
Figure 1. CT chest showing mediastinal nodes with right pleural effusion.
| | | | Discussion | | Intrathoracic nodes compression of one of the bronchus may lead to atelectasis, lung infection and bronchiectasis or thoracic duct leading to chylous effusion. Other intrathoracic complications include dysphagia3, esophago-mediastinal fistula4, tracheo-oesophageal fistula.5 Tuberculous mediastinal nodes encasing the aorta has never been reported before as was seen in our patient. However, Talwar et al. from India have suggested that it is not uncommon if suspected in appropriate clinical setting and they have reported 8 cases of tuberculous involvement in various parts of the aorta including 1 having a pseudo aneurysm of the ascending aorta.6 Initially, Haythorn described four types of tubercular involvement in the arterial system. This included miliary tuberculosis of the intima, tubercular polyps attached to the intima, tuberculosis involving several layers of the arterial wall, and aneurysm formation.7 The aorta may be involved in the tubercular process either through the hematogenous route or by way of direct extension of the disease from the neighboring organs.8 Encasement of aorta by tubercular lymphnodes can be fatal as it can cause aortic dissection and sudden death. Our patient improved after eighteen months of ATT signifies importance of accurate diagnosis of this unique and rare entity. Physician should remember this important complication of MTL and should remain vigilant while evaluating such patients. | | | | Conclusion | | We concluded that though encasement of aorta caused by MTL is extremely rare it does respond well to ATT. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Sharma SK, Mohan A. Extrapulmonary tuberculosis. Indian J Med Res. 2004;120:316-353.
- Mukund A, Khurana R, Bhalla AS, Gupta AK, Kabra SK. CT patterns of nodal diseases in pediatric chest tuberculosis. World J Radiol. 2011;3:17-23 [CrossRef]
- Singh B, Moodly M, Goga AD, Haffejee AA. Dysphagia secondary to tuberculous lymphadenitis. S Afr J Surg. 1996;34:197-199.
- Ohtake M, Saito H, Okuno M, Yamamoto S, Ohgimi T. Oesophagomediastinal fistula as a complication of tuberculous mediastinal lymphadenitis. Intern Med. 1996;35:984-986. [CrossRef]
- Macchiarini P, Delamare N, Beuzeboc P, Labussiere AS, Cerrina J, Chapelier A, et al. Tracheoesophageal fistula caused by mycobacterial tuberculous adenopathy. Ann Thorac Surg 1993;55:1561-1563. [CrossRef]
- Talwar S, Choudhary SK. Tuberculous aneurysms of the aorta. J Thorac Cardiovasc Surg. 2003;125:1184 [CrossRef]
- Haythorn SR. Tuberculosis of the large arteries. J Am Med Assoc. 1913; 60:1413-1416. [CrossRef]
- Bacourt F, Goeau-Brissonniere O, Lacombe P, Parlier H, Terestchenko MC. Surgical treatment of a tuberculous thoracoabdominal aneurysm. Ann Vasc Surg. 1986;1:378-381. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2022.33
|
| Cite this article as: | | Kathwate J. Mediastinal tubercular lymph nodes completely encasing aorta in a child- A rare complication. Pediatr Oncall J. 2022;19: 95-96. doi: 10.7199/ped.oncall.2022.33 |
|