Natalie Wing Tung HO, Mandy Hiu Ching LAM, Winnie Kwai Yu CHAN.
Department of Paediatrics, Queen Elizabeth Hospital, Hong Kong SAR.
ADDRESS FOR CORRESPONDENCE
Dr Natalie Wing Tung HO, Department of Paediatrics, Queen Elizabeth Hospital, 30 Gascoigne Road, Kowloon, Hong Kong SAR.
Email: mandylamhiuching@gmail.com | | Abstract | | Fibrodysplasia ossificans progressive (FOP) is an extremely rare non-inflammatory disease that involves heterotrophic bone formation after tissue injury. Diagnosis of FOP is based on clinical suspicion for children presenting with bilateral hallux valgus and acute soft tissue swelling after trauma. Genetic analysis for mutation of the ACVR1 gene is considered a confirmatory test. We present 2 children with FOP that were diagnosed at seven years and twenty months of age respectively. The first patient presented with acute tissue swelling over the back and an incidental finding of hallux valgus. Genetic study revealed heterozygous c617G>A mutation in exon 4 of the ACVR1 gene suggestive of FOP. She had several relapses, and management pitfalls are highlighted. This first case alerted early diagnosis of FOP in a twenty-month-old boy with bilateral hallux valgus. | | | | Keywords | | FOP, ACVR1 gene, trauma, bilateral hallux valgus. | | | | Introduction | Fibrodysplasia ossificans progressive is a rare non-inflammatory disease involving genetic mutation of the ACVR1 gene, characterised by heterotopic bone formation and recurrent episodes of painful soft tissue swelling that arises spontaneously or is triggered by minor trauma.1 As with almost all rare diseases, there are various scientific and medical challenges in FOP diagnosis and management. As trauma is a stimulant event, biopsy and surgical interventions can cause devastating results at the site of ossification. Thus, it is essential to recognise early features of FOP including bilateral hallux valgus and recurrent soft tissue swelling and avoid tissue biopsy in suspected cases. We present 2 children with FOP and the management issues.
Case 1
A 7-year-old girl presented with progressive left upper back swelling for three weeks after a minor contusion against the table corner. She had a history of mild bilateral conductive hearing impairment, otherwise unremarkable past health. Physical examination revealed mild scoliosis with diffuse swelling, erythema, and tenderness over the left paraspinal muscles. There was reduced movement over her back in all directions, especially over left lateral flexion, and reduced range of movement of both hips on internal and external rotation. Bilateral hallux valgus was noted. Autoimmune markers including anti-nuclear antibody, rheumatoid factor and anti-extractable nuclear antigen were negative. Magnetic resonance imaging (figure 1) revealed T2 hyper-intensity with soft tissue swelling around both scapulae, more severe over the left side. Bony structures appeared unremarkable. She was initially managed with regular physiotherapy for suspected muscle strain and treated with nonsteroidal anti-inflammatory drugs (NSAIDS) to control the inflammation. The treatment did not reduce the muscle discomfort, but stretching exercise aggravated the extent of muscle pain and subsequent “disease flared” over her right sternocleidomastoid muscle. The diagnosis of FOP was then considered. Genetic study revealed heterozygous c617G>A mutation in exon 4 of the ACVR1 gene. ACVR1 encodes for activin A receptor type I/ activin-like kinase 2, a bone morphogenetic protein type I receptor.2 Diagnosis of fibrodysplasia ossificans progressive was established. Since both parents did not have this mutation, it is likely a sporadic case. Subsequent disease flare-up involved the right thorax and right iliac crest, then left chest wall, followed by the left shoulder, then right arm, and her left thigh. Currently she is 17 years of age. During the flares, she had acute progressive swelling, tenderness, erythema with a limited range of movement over the affected site with or without a preceding trauma history. Short courses of high doses intravenous or oral corticosteroid were used for acute management of the flares. Despite that, progressive ossification could not be prevented. She currently has a marked fixation in the axial skeleton with severe kyphosis. Her spine is in 60-degree flexion, and her neck hyperextended at 10 degrees. She has severe micrognathia with receding chins. Her X-ray spine (figure 2a) revealed periosteal new bone over vertebral body L3-5. Her X-ray pelvis (figure 2b) showed bilateral acetabular dysplasia with multiple ossifications over the right hip joint and coxa magna. X-ray cervical spine (figure 2c) showed fusion of neural arches from C2 to C7.
The hyperextension of the neck and severe micrognathia resulted in swallowing difficulty. She is severely underweight with a weight-for-age of 18 kg at 17 years (below the 3rd centile), and she has a BMI of 13.8 kg/m2. She had obstructive sleep apnea with four clusters of desaturations associated with tachycardia, and the duration of SpO2 <90% lasted seventeen minutes. Continuous positive airway pressure was offered; she was, however, not keen on it. Pure tone audiometry confirmed bilateral mild low tone conductive hearing impairment with left Carhart's notch, and bilateral tympanogram was normal. She is currently studying in a special school with desk modification which can be elevated at varying angles. The fixation in the axial skeleton makes it difficult for her to sit, and thus she adopts a kneeling position when eating or attending lessons. She is managed with long term NSAIDs, montelukast and baclofen. Her nutritional status is supplemented with calcium carbonate, vitamin D and multivitamins drops.
Figure 1. T2-weighted coronal MRI thorax revealed hyper-intensity with soft tissue swelling around both scapula, more severe over the left side (white arrow). Bony structures appear unremarkable.
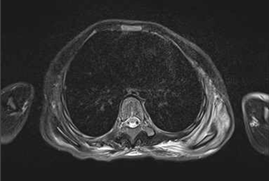
Figure 2a. AP X-ray lumbosacral spine showed periosteal new bone over vertebral body L3-5 (white arrow).
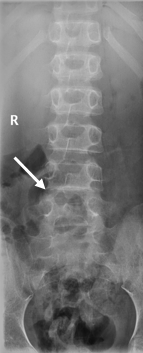
Figure 2b. AP X-ray pelvis showed bilateral acetabular dysplasia (white arrow) with multiple ossifications over the right hip joint and coxa magna.
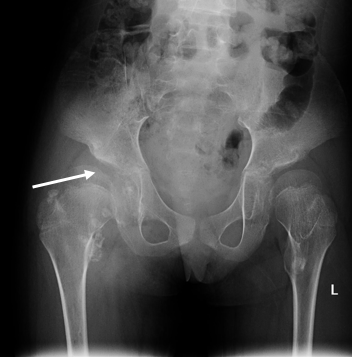
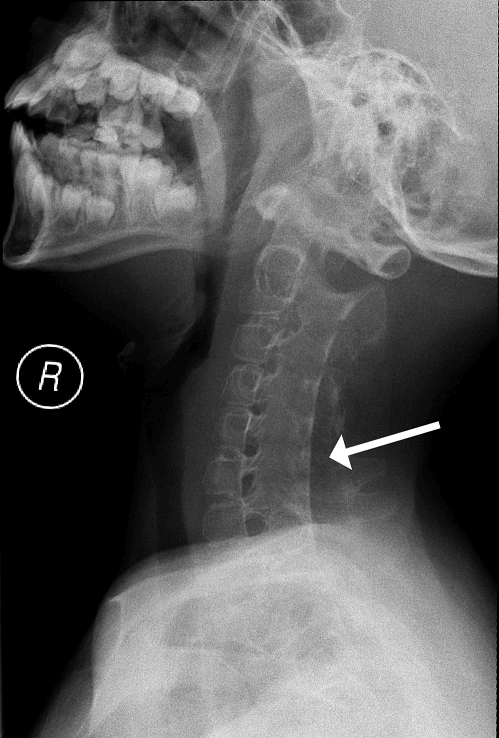
Figure 2c. Lateral X-ray of cervical spine showed fusion of neural arches from C2 to C7 (white arrow).
Case 2
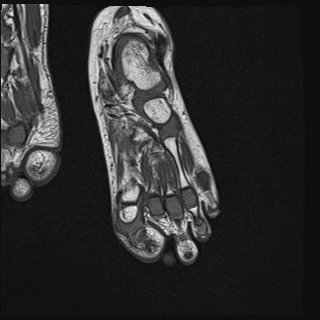
A Chinese boy born locally, was referred to us at 20 months old for bilateral hallux valgus at 40 degrees. He was managed with physiotherapy and splintage at the initial presentation. MRI right foot (figure 3) performed at 13-month-old showed fusion of metatarsal phalangeal joint and hallux valgus deformity at the interphalangeal joint. The proximal phalanx ossification centre was short, and the first metatarsal bone was borderline short. Genetic testing revealed ACVR1 mutation, which is a pathogenic variant. The diagnosis of FOP was substantiated. A detailed counseling was performed with the family on the importance of avoiding physical trauma, invasive procedures, dental care, and daily activity tips. On follow up, he suffered from one episode of acute flare over his right knee at the age of four, which was managed with oral corticosteroid therapy. He is managed with long term montelukast therapy. He was well when last assessed at five years old with no skeletal fixation and pending formal audiology assessment by otorhinolaryngologist.
Figure 3. T1-weighted MRI right foot of patient 2 showed fusion of metatarsal phalangeal joint and hallux valgus deformity at interphalangeal joint (white arrow). The proximal phalanx ossification centre was short, and the 1st metatarsal bone was borderline short.
| | | | Discussion | Fibrodysplasia ossificans progressive (FOP) is a non-inflammatory disease that involves heterotopic bone formation after injury to skeletal muscle, tendons, ligaments, and fascia. Guy Patin first described it in 1962.3 It is an extremely rare inherited disorder, which is severely disabling, characterised by recurrent episodes of painful soft tissue swelling. There is no ethnic, racial, gender, or geographic predilection to FOP.1 Up to date, approximately 800 FOP cases have been documented worldwide,4 but none have been reported in the Southern Chinese except these two patients.
Classically, the disease progresses from cranial to caudal, dorsal to ventral and proximal to distal. The diaphragm, tongue, extraocular muscles, cardiac muscles, and smooth muscles are spared.5 Many documented cases presented initially with paraspinal muscles involvement, which is also seen in our first patient.6 FOP typically presents with bilateral hallux valgus associated with absent or fused interphalangeal joint of the first toe at birth. It is followed by acute tissue swelling presenting from birth to the second decade of life.5 Suspicion of FOP is based on clinical presentation, and since most cases are sporadic, family history does not play an important role in diagnosis. In cases with clinical suspicion, genetic analysis for mutation of exon 4 in ACVR1 gene is considered a confirmatory test.5
Complications of FOP include hearing loss, kidney stone and thoracic insufficiency syndrome. A study performed in 1999 interviewed 54 patients with FOP and found that 52% suffer from hearing loss.7 Hearing impairment is a common feature amongst FOP patients. The onset is in childhood and may slowly progress. Hearing loss is usually conductive in nature and may be due to middle ear ossification.7 In the first case discussed, the patient was found to have a hearing problem since the age of six later confirmed on pure tone audiogram to have mild bilateral conductive hearing loss. Hearing aids or other assistive devices can also improve auditory monitoring of the environment and safety for FOP patients, especially for those with severely restricted ossification of the neck, limiting visual monitoring of the environment.7 FOP patients have a three times higher risk of suffering from kidney stones than the general population. It is postulated that immobilisation and increased bone turnover rate are a significant risk factor.8 High fibre diet with adequate fluid intake is therefore crucial in this group of patients. Thoracic insufficiency syndrome is a significant complication and leading mortality, accounting for 54% of deaths in FOP patients.9 The costovertebral malformations with ankylosis of costovertebral joints, ossification of intercostal muscle and progressive spinal deformity results in increased chest wall deformity and thoracic insufficiency syndrome. This leads to reduced vital capacity causing pulmonary hypertension and possible right congestive heart failure and mortality.10 Therefore, prophylactic measures to maximise pulmonary function and prevent chest infection help improve morbidity and mortality from thoracic insufficiency syndrome amongst FOP patients.5
Without a definitive treatment, the most promising management of FOP lies in the early diagnosis and prevention of tissue injury.11 Nearly 90% of patients with FOP were initially misdiagnosed and subjected to unnecessary interventions resulting in exacerbation of the disease.12 In case of clinical suspicion, tissue biopsy should be withheld until FOP is ruled out. Moreover, assiduous precautions are necessary for patients to prevent disease flare-up.5 Inappropriate stretching exercise may lead to stiffening of muscle and subsequent ossification. Therefore, any interventions with possible injury, including physiotherapy, should be cautiously evaluated before subjecting the patient to it.11 Patients should be reminded on avoidance of intramuscular and arterial puncture; moreover, a dental alert is necessary to prevent stretching of temporomandibular joint to avoid permanent ankylosis of jaw.5 A multidisciplinary team approach is crucial in managing patients with this rare disease. Physicians take part in managing acute and long term associated medical problems; dietician contributes by optimising nutritional intake and lowering the risk of renal stones. Otorhinolaryngologist provides biannual audiometry assessment; respirologist manages obstructive sleep apnea, the occupational therapist provides household modifications to reduce risk of falls and injuries; and clinical psychologist provides psychological counselling support to patient and family members.
| | | | Conclusion | | FOP is a severely debilitating disease with no definite cure. Recognising the early features of FOP and establishing the diagnosis early with detailed counselling may help to improve morbidity and quality of life in this group of patients. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Shah ZA, Rausch S, Arif U, El Yafawi B. Fibrodysplasia ossificans progressiva (stone man syndrome): a case report. J Med Case Reports. 2019;13:1-5. [CrossRef]
- Lin S, Svoboda KK, Feng JQ, Jiang X. The biological function of type I receptors of bone morphogenetic protein in bone. Bone Res. 2016;4:1-9. [CrossRef]
- Gupta N, Pruthi A, Kumar S, Verma R, Belho ES. Fibrodysplasia Ossificans Progressiva - A Rare Genetic Disorder and the Role of Technetium-99m Methylene Diphosphonate Bone Scan. Indian J Nucl Med. 2019;34:209-212. [CrossRef]
- Akyuz G, Gencer-Atalay K, Ata P. Fibrodysplasia ossificans progressiva: lessons learned from a rare disease. Curr Opin Pediatr. 2019;31:716-722. [CrossRef]
- Pignolo RJ, Shore EM, Kaplan FS. Fibrodysplasia ossificans progressiva: diagnosis, management, and therapeutic horizons. Pediatr Endocrinol Rev. 2013;10 Suppl 2(0 2):437-48.
- Bauer AH, Bonham J, Gutierrez L, Hsiao EC, Motamedi D. Fibrodysplasia ossificans progressiva: a current review of imaging findings. Skeletal Radiol. 2018;47:1043-1050. [CrossRef]
- Levy CE, Lash AT, Janoff HB, Kaplan FS. Conductive hearing loss in individuals with fibrodysplasia ossificans progressiva. Am J Audiol. 1999;8:29-33. [CrossRef]
- Gupta RR, Delai PL, Glaser DL, Rocke DM, Al Mukaddam M, Pignolo RJ, Kaplan FS. Prevalence and risk factors for kidney stones in fibrodysplasia ossificans progressiva. Bone. 2018;109:120-123. [CrossRef]
- Kaplan FS, Zasloff MA, Kitterman JA, Shore EM, Hong CC, Rocke DM. Early mortality and cardiorespiratory failure in patients with fibrodysplasia ossificans progressiva. J Bone Joint Surg Am. 2010;92:686-691. [CrossRef]
- Kaplan FS, Glaser DL. Thoracic insufficiency syndrome in patients with fibrodysplasia ossificans progressiva. Clin Rev Bone Miner Metab. 2005;3:213-216. [CrossRef]
- Gencer-Atalay K, Ozturk EC, Yagci I, Ata P, Delil K, Ozgen Z, Akyuz G. Challenges in the treatment of fibrodysplasia ossificans progressiva. Rheumatol Int. 2019;39:569-576. [CrossRef]
- Kitterman JA, Kantanie S, Rocke DM, Kaplan FS. Iatrogenic harm caused by diagnostic errors in fibrodysplasia ossificans progressiva. Pediatrics. 2005;116:e654-e661. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2022.11
|
| Cite this article as: | | HO N W T, LAM M H C, CHAN W K Y. Fibrodysplasia Ossificans Progressiva - Recognising the Early features and Avoid Doing Harm. Pediatr Oncall J. 2022;19: 15-18. doi: 10.7199/ped.oncall.2022.11 |
|