Banuprritaa Veejeyahshegarun, John Emmanuel, Pavin Bal Baldev Singh, Muhammad Firdaus Bin Madzlan, Nurdaliza Binti Mohd Badarudin.
Department of Surgery, Paediatric Surgical Unit, Hospital Raja Permaisuri Bainun, Ipoh, Malaysia.
ADDRESS FOR CORRESPONDENCE
Dr. Banuprritaa Veejeyahshegarun, Lot 240 Kampung Baru Dengkil, Dengkil, 43800, Malaysia
Email: prritaa90@gmail.com | | Abstract | | Hybrid lung lesions are a rare entity which consists of congenital lung malformations with both cystic and solid components also with vascular supply consistent with bronchopulmonary sequestration. In view of the peculiar behavior of this lesions, there is no clear cut gold standard guideline on its investigation nor management techniques. We reported case of a 6 year old boy with a hybrid lesion consisting of an intralobar pulmonary sequestration associated with a type II Congenital Pulmonary Airway Malformation (CPAM) who presented as a case of complicated pneumonia. The lesion was diagnosed via a Contrast Enhanced Computerized Tomography (CECT). Child underwent a thoracotomy and left lower lobe lobectomy and histopathology examination confirmed our diagnosis. A literature review showed our case to be the first case of a hybrid lesion in a child reported in Malaysia. | | | | Keywords | | Hybrid lung lesions, Type II Congenital Pulmonary Airway Malformation. | | | | Introduction | Pulmonary sequestrations and congenital pulmonary airway malformations are a spectrum of lung anomalies that are well known, yet uncommon. When congenital pulmonary airway malformation is associated with a systemic blood supply it is termed as a “Hybrid” lesion. This term was coined by Children’s Hospital of Philadelphia (CHOP) in 1998. This abnormal mass of
non-functioning lung tissue may be further categorized as extralobar or intralobar. While the extralobar hybrid lesions are well described, literature on the intralobar lesion is scarce.1
We describe a 6 year old boy with a hybrid lesion consisting of an intralobar pulmonary sequestration associated with a type II Congenital Pulmonary Airway Malformation (CPAM). This is the first case of a hybrid lesion in a child reported in Malaysia. | | | | Case Report | A 6 years old boy presented to our district hospital with chief complains of fever and cough for the past 4-5 days. Child was admitted and treated for an upper respiratory tract infection. However, in view of persistent temperature spikes, a chest x-ray was performed which revealed a left sided pleural effusion (a total whiteout). Child developed intermittent grunting, became increasingly tachypnoeic with suprasternal and subcostal recessions and appeared more lethargic. Trachea appeared to be deviated to the right side, there was dullness on percussion and reduced breath sounds over the left middle and lower zone. Child was intubated and transferred to our Paediatric Intensive Care Unit for further management. On arrival to our center, child appeared to be in a decompensated septic shock requiring inotropic support. An ultrasound thorax done revealed a large heterogeneous highly vascular lesion in the left lower hemithorax with blood supply arising from the abdominal aorta, superolateral to origin of the coeliac artery. A Contrast Enhanced Computerized Tomography (CECT) thorax was done which revealed a heterogeneously enhancing mass seen at the left hemithorax measuring 10.8x11.9x13.1 cm, with numerous fluid-filled cyst within, arterial supply noted to be arising from the abdominal aorta at the level of the coeliac trunk and venous return into the left pulmonary vein. There was a mediastinal shift with a left sided pleural effusion noted as well. A rounded hyper-density was also noted at the lateral aspect of the mass suggestive of an arterial aneurysm. An ultrasound guided biopsy was performed to rule out pleuropulmonary blastoma which revealed no malignant cells. We then proceeded with a thoracotomy. The left lower lobe was filled with pus and adhered to the diaphragm, a feeding vessel was noted from a branch above the coeliac artery piercing through the diaphragmatic tissue. A left lower lobectomy was performed and a chest drain inserted intraoperatively. Post-operative period was complicated with a haemothorax and recurrent pneumonias with parapneumonic effusions requiring prolonged ventilation. Child subsequently recovered and was discharged well. Child has been doing well since then and follow up visits have been uneventful. HPE showed various dilated cystic spaces lined by cuboidal to ciliated pseudostratified columnar epithelium with minimal foci of cartilaginous tissue in intervening area suggestive of CPAM most probably type II with associated inflammatory changes and fibrosis.
Figure 1. Shows erect chest radiograph during his presentation which shows left massive pleural effusion.
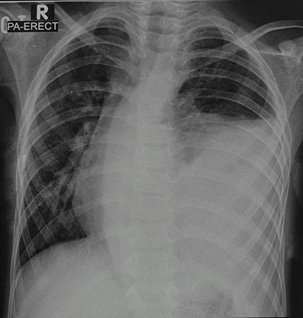
Figure 2 A, B Shows CT images of the hybrid lung lesion with the feeding vessel.
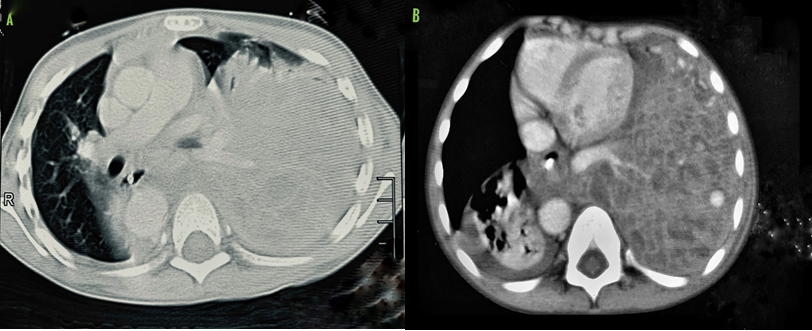
Figure 3A. Shows the affected lung.
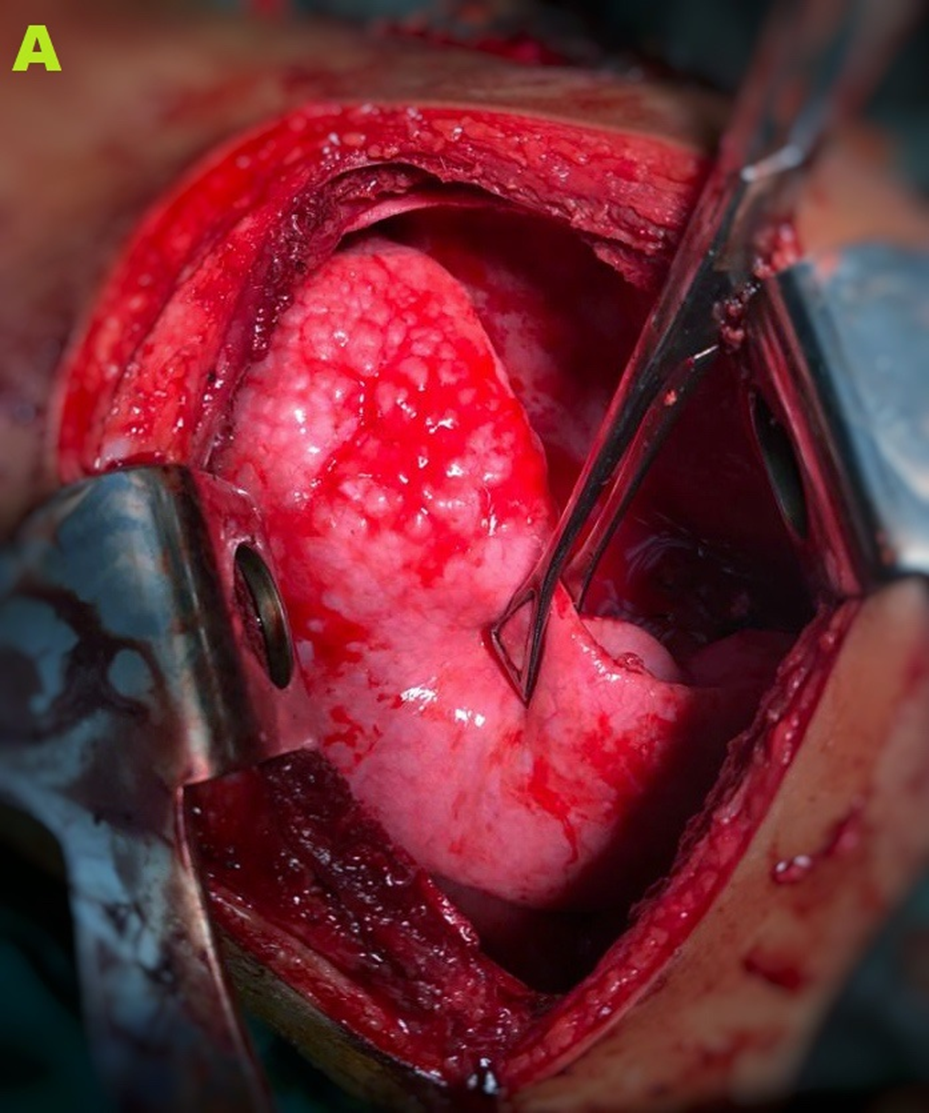
Figure 3B. Arrow shows the feeding vessel to the hybrid lesion.
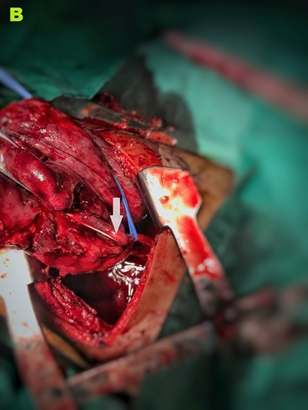
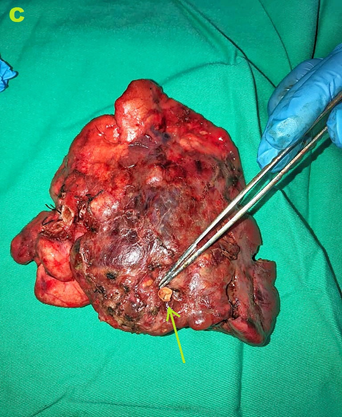
Figure 3C. Shows the gross sample of the excised hybrid lesion with the arrow showing the feeding vessel.
 | | | | Discussion | The intralobar pulmonary sequestration associated with type II CPAM is a congenital lung malformation which is described as a non-functioning lung tissue invested within the same pleura as normal lung, with an aberrant arterial supply from the systemic vasculature and drainage into the pulmonary or systemic veins. The non-functioning lung tissue displays features of type II CPAM with multi cystic areas of over proliferation and dilatation of terminal respiratory bronchioles, lacking normal alveoli.2,3
From the literature review performed, these lesions usually tend to be symptomatic during the neonatal or infancy period and rarely present during childhood.4,5,6,7,8,9 However Pierre Goussard et al10 and Fatima Naumeri et al11, reported hybrid lesions in older children, who presented with lung infection, similar to our case. Therefore, a hybrid lung lesion should be kept in mind as a differential diagnosis in children presenting with recurrent pneumonia. These hybrid lesions are commonly seen in the left lower lobe, as seen in our patient. In an extensive review by Savic et al from 1862-1978, 86% of patients presented with a lesion in the left lower lobe.12
Common modalities in investigation of hybrid lung lesion in children are chest x-ray, ultrasound and CECT Thorax. We however performed an ultrasound guided biopsy to rule out pleuropulmonary blastoma in view of the age of presentation and the vascularity of the lesion as seen in the ultrasound. However, retrospectively, we think that this could have been avoided, as the systemic arterial supply, pulmonary venous drainage and multicystic appearance on the CECT thorax was suggestive of a hybrid lesion.
Involution of hybrid lesions with significant systemic arterial supply is highly unlikely. The potential risk of recurrent pneumonias, haemoptysis, malignant transformations suggest that surgical resections should be performed when child stabilizes or as an elective surgery to reduce the morbidity. Performing early surgical resection, also helps reduce parental anxiety.7 In accordance to type of surgery, the argument between thoracotomy and thoracoscopic surgery has been widely controversial. A meta-analysis by A.Nasi,j.bass14 showed no difference with regards to complications and duration of surgery. Only variable noted was the reduced in hospital stay, better cosmesis and reduce post-operative pain for patients post thoracoscopic resection. As for our patient we proceeded with thoracotomy in view of lack of expertise in the thoracoscopic approach. The left posterolateral thoracotomy confirmed the CECT findings of a systemic arterial supply from the abdominal aorta. The HPE report suggestive of a type II CPAM and CECT as well as the intra operative findings of systemic arterial supply confirmed the diagnosis of a hybrid lesion in our patient.
| | | | Conclusion | | The diagnosis of a hybrid lesions should be in the list of differentials when treating children with recurrent episodes of pneumonia. Radiological features of these hybrid early surgical resection is advised to reduce the risk of morbidity and parental anxiety. | | | | Acknowledgement | I would like to thank and give my warmest thanks to my Surgeons under Paediatric Surgical Unit from Hospital Raja Permaisuri Bainun, Ipoh, Perak, Malaysia for regularly cultivating their support in my case report and made this work possible. Their guidance and advice carried me through all the stages in writing my case report.
I would also like it give special thanks to Dr John Emmanuel and Dr Pavin Bal Baldev Singh as a whole for their continuous support and understanding when undertaking my research and writing my case report. Your assistance was what sustained me this far. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- The Children's Hospital of Philadelphia. (2019, July 12). Hybrid lesions. Children's Hospital of Philadelphia. Retrieved February 20, 2022, from https://www.chop.edu/conditions-diseases/hybrid-lesions
- Jonathan Durell, Kokila Lakhoo,Congenital cystic lesions of the lung,Early Human Development,Volume 90, Issue 12,2014,Pages 935-939,ISSN 0378-3782, https://doi.org/10.1016/j.earlhumdev.2014.09.014. (https://www.sciencedirect.com/science/ article/pii/S0378378214002394) [CrossRef] [PubMed]
- Darren J. Fowler, Steve J. Gould, The pathology of congenital lung lesions,Seminars in Pediatric Surgery,Volume 24, Issue 4,2015,Pages 176-182,ISSN 1055-8586, https://doi.org/10.1053/j.sempedsurg.2015.02.002. (https://www.sciencedirect.com/science/ article/pii/S1055858615000281) [CrossRef] [PubMed]
- Herman, T., Siegel, M. Congenital intralobar pulmonary sequestration with cystic adenomatoid malformation. J Perinatol 29, 175-177 (2009). https://doi.org/10.1038/ jp.2008.90 [CrossRef] [PubMed]
- Orpen, N., Goodman, R., Bowker, C. et al. Intralobar pulmonary sequestration with congenital cystic adematous malformation and rhabdomyomatous dysplasia. Ped Surgery Int 19, 610-611 (2003). https://doi.org/10.1007/s00383-003-1040-3 [CrossRef] [PubMed]
- Darrell L Cass, Timothy M Crombleholme, Lori J Howell, Perry W Stafford, Eduardo D Ruchelli, N.Scott Adzick, Cystic lung lesions with systemic arterial blood supply: A hybrid of congenital cystic adenomatoid malformation and bronchopulmonary sequestration,Journal of Pediatric Surgery, Volume 32, Issue 7,1997,Pages 986-990, ISSN 0022-3468, https://doi.org/10.1016/S0022-3468(97)90383-3. (https://www.sciencedirect.com/science/article/pii/S0022346897903833) [CrossRef]
- Samuel M, Burge DM. Management of antenatally diagnosed pulmonary sequestration associated with congenital cystic adenomatoid malformation. Thorax. 1999;54(8):701-706. doi:10.1136/thx.54.8.701 [CrossRef] [PubMed] [PMC free article]
- Zeidan, S., Hery, G., Lacroix, F. et al. Intralobar sequestration associated with cystic adenomatoid malformation: diagnostic and thoracoscopic pitfalls. Surg Endosc 23, 1750- 1753 (2009). https://doi.org/10.1007/s00464-008-0183-7 [CrossRef] [PubMed]
- Schuster B, Holland-Cunz SG, Zimmermann PIntradiaphragmatic hybrid lesion: surgical decision-making and value of minimal invasive surgeryCase Reports 2017;2017:bcr-2016-218527. [CrossRef] [PubMed] [PMC free article]
- Goussard P, Andronikou S, Mfingwana L, et alHybrid lesion in a child presenting with cough, fever and haemoptysisBMJ Case Reports CP 2020;13:e238796. [CrossRef] [PubMed]
- Naumeri, Fatima & Sajjad, Muhammad. (2018). Hybrid Lesion: Extralobar Sequestration With Cystic Adenomatoid Malformation - Misdiagnosed As Pulmonary Tuberculosis. Journal of the College of Physicians and Surgeons Pakistan. 28. S204-S206. 10.29271/jcpsp.2018.09.S204. [CrossRef] [PubMed]
- Savić B, Birtel FJ, Knoche R, Tholen W, Schild H. Pulmonary sequestration. Ergeb Inn Med Kinderheilkd. 1979;43:57-92. doi: 10.1007/978-3-642-67379-5_2. PMID: 394961. [CrossRef] [PubMed]
- Oliver, Edward & DeBari, Suzanne & Giannone, Mariann & Pogoriler, Jennifer & Johnson, Ann & Horii, Steven & Gebb, Juliana & Howell, Lori & Adzick, N. & Coleman, Beverly. (2017). Going With the Flow: An Aid in Detecting and Differentiating Bronchopulmonary Sequestrations and Hybrid Lesions: Prenatal Diagnosis of Intralobar and Extralobar Lung Lesions. Journal of Ultrasound in Medicine. 37. 10.1002/jum.14346. [CrossRef] [PubMed]
- Nasr A, Bass J. Thoracoscopic vs open resection of congenital lung lesions: a meta- analysis.JPediatr Surg. 2012 May;47(5):857-61. doi: 10.1016/j.jpedsurg.2012.01.036. PMID: 22595561. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2023.40
|
| Cite this article as: | | Veejeyahshegarun B, Emmanuel J, Singh P B B, Madzlan M F B, Badarudin N B M. Hybrid Lung lesion: An Accidental Finding. Pediatr Oncall J. 2023;20: 156-160. doi: 10.7199/ped.oncall.2023.40 |
|