Pseudohypoaldosteronism Secondary to Urinary Tract Infection in a Premature Newborn Baby
|
|
Pseudohypoaldosteronism Secondary to Urinary Tract Infection in a Premature Newborn Baby
03/01/2023
03/01/2023
https://www.pediatriconcall.com/Journal/images/journal_cover.jpg
Samet Benli, Erdal Taşkın, Mustafa Aydın.
Department of Neonatology, Firat University School of Medicine, Elazig, Turkey.
ADDRESS FOR CORRESPONDENCE
Samet Benli, Department of Neonatology, Firat University School of Medicine, 23200, Elazig / Turkey.
Email: drbenli@gmail.com
Pseudohypoaldosteronism Secondary, Urinary Tract Infection, Newborn
|
Clinical Problem
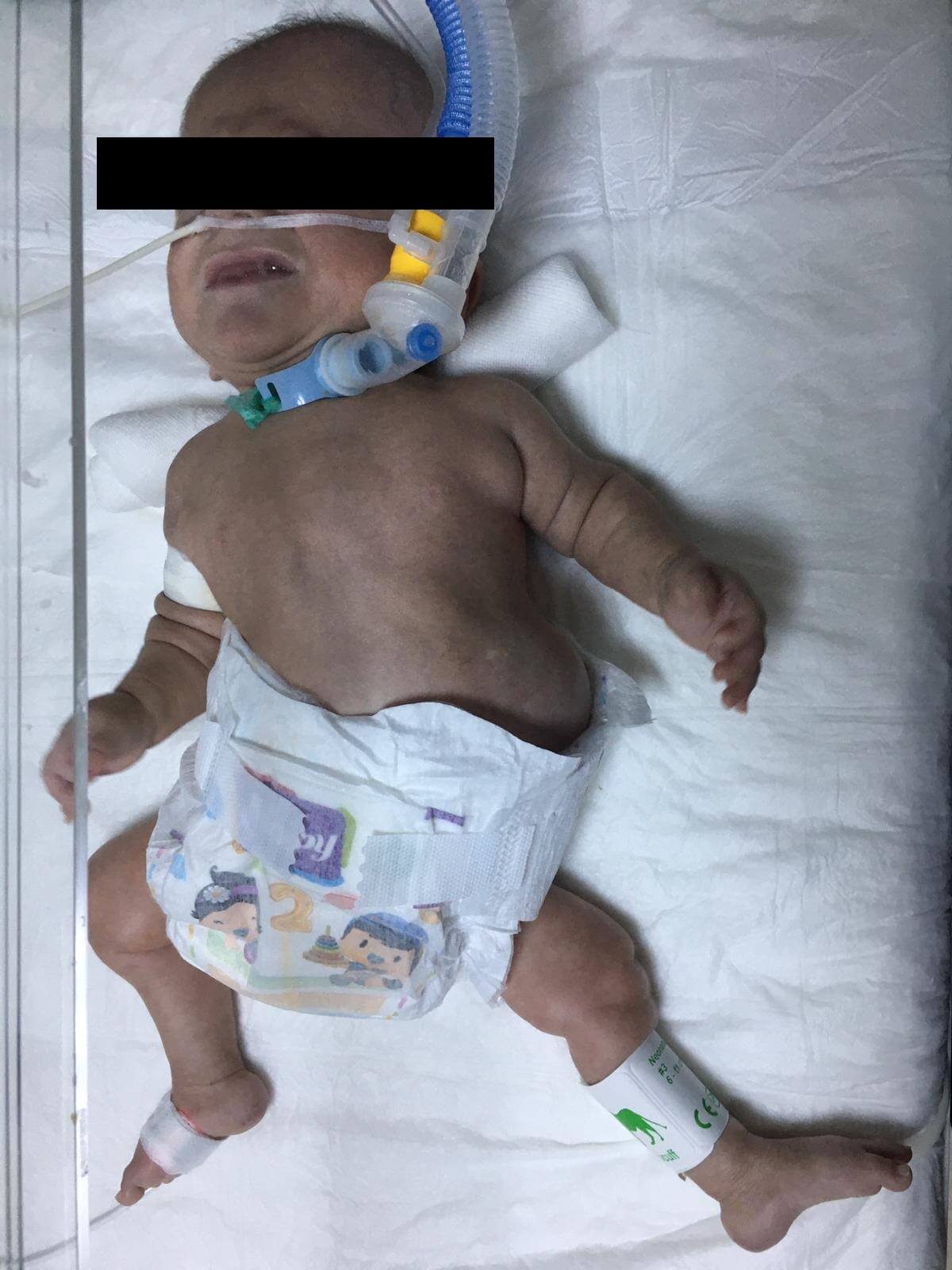
Upon the detection of sodium 120 mmol/L and potassium 8.8 mmol/L in the routine examinations taken on the 93th day of hospitalization of a premature baby born at the 24th gestational week, weighing 700 g (Figure 1), further investigations for the etiology were performed.
The patient has been fed full enteral (8x70 cc) with an orogastric tube. The patient who was operated on postnatal 14th day for intestinal perforation had ileostomy. Tracheostomy was performed on the postnatal 78th day of the patient who developed posthemorrhagic hydrocephalus during the clinical follow-up and could not be extubated. The patient is still on mechanical ventilation (PIP 23, PEEP 6, IT 0.40 and FiO2 30%). Of the vital signs, body temperature was 36.3 degrees Celsius, heart rate 126 beats/min (range 120-160), oxygen saturation 93% (range 90-94) and blood pressure 87/46 (mean 62) mmHg. There was no any central catheter other than the previously inserted umbilical venous catheter.
His previous sodium and potassium levels were within normal limits. Capillary blood gas analysis was consistent with metabolic acidosis (pH 7.28, pCO2 26.1, HCO3 16.2). The patient’s other laboratory parameters were normal as follows: hemoglobin 10.3 g/dL (range 14-23.7 g/dL), hematocrit 32% (range 47-75%), white blood cells 16.2x103 cells/µL (range 9-30 cells/µL), platelets 608x103 cells/µL (range 150-400 cells/µL) , Cl 90 mmol/L (range 98-110 mmol/L), BUN 30 mg/dl (range 10-50 mg/dL), creatinine 0.5 mg/dl (range 0.2-0.9 mg/dL), eGFR 24 ml/min (range ~20 ml/min per 1.73 m2) and C-reactive protein 62 mg/L (range 0-5). In spot urine, sodium was <10 mEq/L (range 54-150 mEq/L), potassium 13.3 mEq/L (range 20-80 mEq/L), calcium <1 mg/dL (range 6.7-21.3) and protein 37.4 mg/dL (range 1-14 mg/dL). Urinalysis was consistent with urinary tract infection (leukocyte esterase +3, nitrite positive, protein trace; leukocyte 217/HPF (range <5/HPF), erythrocyte 20/HPF (range <3/HPF) and bacteria 5/HPF). On further laboratory analysis, 17-hydroxyprogesterone was 5.1 nmol/L (range 0.3-5.2), renin 100 ng/mL (range 2.4-37) and aldosterone >1000 ng/dL (range 7-99). 105 colonies of Klebsiella pneumonia were isolated in the urine culture and after that ceftazidime/avibactam treatment was started according to the antibiogram. Urinary ultrasonography showed signs of urinary tract infection. Insulin-glucose infusion and sodium bicarbonate treatment was given for hyperkalemia. Replacement was given for hyponatremia and then 2 g/day of salt was added to his diet. The urinary tract infection resolved after antibiotic treatment and sodium and potassium levels returned within normal limits on the 10th day of treatment. Afterwards, the patient’s salt support was gradually reduced and discontinued.
In this context, what should we consider in the etiology for hyponatremia, hyperkalemia and metabolic acidosis that occurred during follow-up in this patient?
Figure 1. General appearance of the patient.
|
| |
What should we consider in the etiology that occurred during follow-up?
|
|
|
Discussion
Pseudohypoaldosteronism (PHA) is a salt-losing disease caused by peripheral resistance to aldosterone. It may be primary as a result of mutation in the mineralocorticoid receptor or epithelial sodium channel, or it may develop secondary to urinary infection, uropathy and drugs. Clinical experience shows that secondary PHA is more common than primary.1 Three types of PHA are seen as type 1 and type 3 salt-losing and type 2 salt-retaining forms.1,2
PHA 1 manifests with salt loss, growth retardation, dehydration and circulatory collapse in the neonatal period. According to clinical and genetic findings, it has two different forms as systemic and limited to the kidney. In PHA 2, by contrast, potassium is retained and hypertension is seen. In this disease, first described by Gordon, plasma aldosterone levels are highly variable and plasma renin activity is suppressed; varying degrees of hyperchloremia and metabolic acidosis are seen. Renal and adrenal functions are normal. PHA 2 is inherited in an autosomal dominant trait. The “with no lysine kinase” (WNK) gene, which encodes the protein that causes the disease, belongs to the serine-threonine kinase (WNK1 and WNK4) family. The typical feature of Gordon’s syndrome is that it can be treated with thiazide diuretics.3,4,5
The third clinical form of PHA is the secondary or transient form. The most common causes of secondary / transient PHA are urinary tract infections and obstructive uropathies. The mechanism of transient mineralocorticoid resistance has not been fully elucidated.6 Congenital urinary tract obstruction such as ureterohydronephrosis, ureterocele, ureteropelvic junction obstruction, posterior urethral valve, systemic lupus erythematosus, sickle cell nephropathy, acute renal allograft rejection and chronic allograft nephropathy cause secondary PHA.7 Accordingly, based on the current clinical and laboratory findings, it was thought that secondary/transient PHA occurred in our case due to urinary system infection. After antibiotic therapy and salt supplementation, the patient's hyponatremia, hyperkalemia and metabolic acidosis improved.
If hyponatremia, hyperkalemia and metabolic acidosis occur during the clinical follow-up of a patient without any previous metabolic and electrolyte disturbance, secondary / transient PHA should be considered in the differential diagnosis. Congenital adrenal hyperplasia (CAH) is the most important disease in its differential diagnosis. On the other hand, PHA should be considered in these newborn infants who do not have signs of CAH on physical examination. These both conditions are fatal if late diagnosed and left untreated.
|
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
- Belot A, Ranchin B, Fichtner C, et al. Pseudohypoaldosteronisms, report on a 10-patient series. Nephrol Dial Transplant 2008; 23(5): 1636-41. [CrossRef] [PubMed]
- Bonny O, Rossier BC. Disturbances of Na/K balance: pseudohypoaldosteronism revisited. J Am Soc Nephrol 2002; 13(9): 2399-414. [CrossRef] [PubMed]
- Gordon RD. Syndrome of hypertension and hyperkalemia with normal glomerular filtration rate. Hypertension 1986; 8(2): 93-102. [CrossRef] [PubMed]
- Wilson FH, Disse-Nicodème S, Choate KA, et al. Human hypertension caused by mutations in WNK kinases. Science 2001; 293(5532): 1107-12. [CrossRef] [PubMed]
- Disse-Nicodème S, Achard JM, Desitter I, et al. A new locus on chromosome 12p13.3 for pseudohypoaldosteronism type II, an autosomal dominant form of hypertension. Am J Hum Genet 2000; 67(2): 302-10. [CrossRef] [PubMed] [PMC free article]
- Watanabe T. Reversible secondary pseudohypoaldosteronism. Pediatr Nephrol 2003; 18(5): 486. [CrossRef] [PubMed]
- Proctor G, Linas S. Type 2 pseudohypoaldosteronism: new insights into renal potassium, sodium, and chloride handling. Am J Kidney Dis 2006; 48(4): 674-93. [CrossRef] [PubMed]
|
|
| |
Cite this article as:
Benli S, Taşkın E, Aydın M. Pseudohypoaldosteronism Secondary to Urinary Tract Infection in a Premature Newborn Baby. Pediatr Oncall J. 2023;20: 34-35. doi: 10.7199/ped.oncall.2023.11
|