Inês Silva Costa, João Sousa Marques, Ana Rita Rodrigues Matos, Gisela Oliveira, Sandra Oliveira, Paula Pinto Ferreira, Lígia M. Ferreira, Cristina Baptista.
Pediatrics Department, Centro Hospitalar Tondela-Viseu, Portugal.
ADDRESS FOR CORRESPONDENCE
Inês Silva Costa, Av. Rei Dom Duarte, 3504-509 Viseu.
Email: c-ines@hotmail.com. | | Abstract | Background and Aim: The Manchester Triage System (MTS) is a clinical risk management tool used to attribute priority in emergency departments. In pediatric acute care, triage systems are associated with more subjective evaluations as they often depend on caregivers’ perceptions. This study aims to study the relationship between MTS and clinical outcomes.
Methods: We analyzed every visit to the Pediatric Emergency Department (PED) between august 2018 and February 2021. The exposure group was defined as a red or orange priority and a compound outcome of hospitalization, transfer to tertiary care hospital or death was assessed.
Results: We obtained 63.897 admissions, of which 52,5% corresponded to male patients and 80,6% were admitted by the parents´ initiative. Green priority (49,9%) was the most frequent, followed by yellow (42,0%), orange (7,6%), blue (0,4%) and red (0,1%).
The incidence rate of the studied outcome was 17,8% in the exposure group and 3,1% in the other patients, with an attributable risk of 14,7%. 7 patients must be triaged with red or orange priority so that one additional case of the outcome is verified. The main used flowchart was “Child that doesn´t feel well” (20,3%).
Conclusion: The priority attributed by the MTS has some association with the patient´s outcome. The low number needed to harm can be due to a useful application of the system and may reflect the deleterious effect that a bad clinical first impression may pose in the prognosis. | | | | Keywords | Manchester Triage System, Pediatric Emergency, Pediatric Nursing.
Abbreviations: MTS - Manchester Triage System, PED - Pediatric Emergency Department. | | | | Introduction | The use of Triage Systems to guide health workers when determining the priority of medical assessment and treatment has been adopted to classify risks and enable a safe patient flow in the Emergency Departments. Triage systems are developed by expert opinion and most flowcharts are in line with adult patient care. Several Triage Systems are available but Manchester Triage System is the most applied in Europe. This system stratifies the patients into 5 categories of needed readiness of care: red (immediate), orange (very urgent), yellow (urgent), green (standard) and blue (non-urgent). Although it determines the maximum recommended time for the first medical observation, it doesn’t make assumptions about the underlying diagnosis. The MTS algorithm has 52 flowcharts with key signs or symptoms and each has additional discriminators that are consecutively evaluated. When a discriminator applies to the patient, the triage stops and that priority is attributed. A determined discriminator may appear in more than one flowchart, but it leads to the same priority level regardless which decreases inner observation differences. Forty-nine flowcharts are suitable for children.1,2,3
The validity of MTS is still uncertain, as some age groups or medical conditions lack sensitivity and specificity. In particular, pediatric patients are of more subjective evaluation as the information provided by caregivers is often not adequate and based on personal biased perceptions. Furthermore, the pediatric population includes a very heterogeneous group of patients since newborns, schoolers and teens are very different in clinical findings for the same pathology but also their age affects greatly the range of normal vital signs. Some flowcharts were created as an adaptation to the pediatric emergency care setting such as “Worried Parents”, “Child that doesn´t feel well” or “Baby that Cries”.4,5,6,7,8,9
This study aims to determine the performance of the MTS for the pediatric population attending the emergency hospital as a predictor of poor outcomes.
| | | | Methods & Materials | This is an observational, retrospective, cohort study of patients presenting to a level II European hospital between the 1st of august 2018 and the 28th of February 2021. This hospital provides acute emergency care, 24 hours, 7 days per week. The medical staff includes pediatricians, pediatric or general surgeons and orthopedists. The center provides general emergency and trauma care, except neuro-surgery. Patients can be admitted either by their parents’ initiative or after referral: by SNS 24 (a national telephonic line to whom sick citizens can call 24 hours/7 days a week), by National Emergency Institute (pre-hospital care) or after medical observation (in primary care or ambulatory hospital appointments).
Before the studied period, the hospital had 7 years of experience with MTS and the system is applied through a computerized application by nurses, with a minimum experience of 6 months in the emergency department and whom a certificate of accreditation with the MTS course provided by the national organization MTS network was awarded.
The computation of the sample size took into account that it should enable inferential analysis between the studied groups (exposure vs non-exposure group). All consecutive patients, aged [0; 18] years, attending the emergency department, who underwent risk classification were included in the study.
The exposure group was defined as patients with red or orange priority, determined at the admission in our unit, as every patient undergoes this process even when they were transferred from another prior institution. Yellow, green and blue priorities were gathered in the comparison group. The inclusion of green and blue priority patients, who should seek acute care in primary health care services, was chosen because in our setting these patients are not derived to other outpatient services after classification.
The outcome was defined as a compound measure of hospitalization, transfer to a level III hospital (more differentiated healthcare) or death.
Data collection was performed automatically through the electronic hospital system (Alert®) and variables that were consulted manually were imported into the database with a code series to blind identification, triage priority and outcome.
Analysis was performed using Statistical Package for Social Sciences software (version 26.0).
| | | | Results | During the 30-month study period, 65081 patients were admitted to the PED. We excluded 1184 patients from the final analysis due to the lack of attributed triage. This group includes children and adolescents admitted by medical order for revaluation of their clinical condition or to repeat urine samples through an aseptic method.
The final cohort included 63897 admissions, with a mean age of 6,1±5,4 years and of which 52,5% were males. The major portion of patients was admitted by the parents´ initiative (52166; 81,6%), followed by primary care (4748; 7,5%), after triage from the national telephonic line SNS24 (4324; 6,8%), national emergency institute (2629; 4,2%) and outpatient medical appointments (30; <0,1%). The division of patients by triage groups is represented in Figure 1.
Figure 1. Patients priority according to Manchester Triage System.
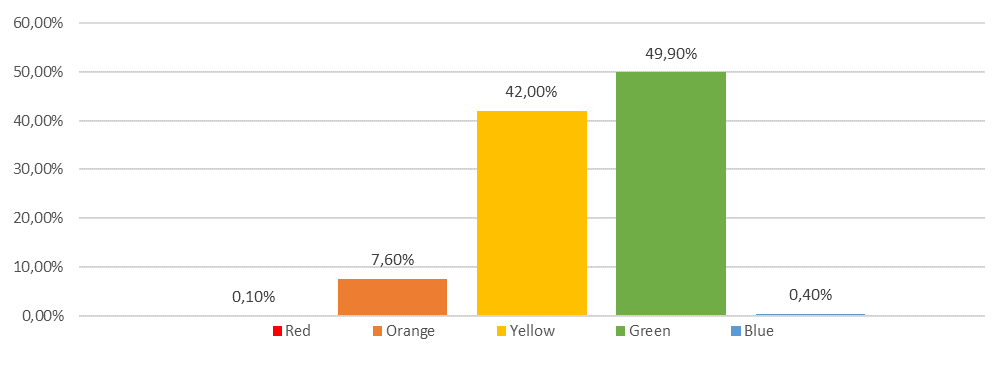
After allocation, the final exposure group included 4956 (7,8%) patients and the comparison group 58941 (92,2%). No association was found between sex and triage subgroups. On the other hand, patients in the exposure group were significantly younger (4,5±5,6 years vs 6,3±5,4 years; p<0,01 t-student test for independent samples). An association was also found between the group and type of provenience (p<0,01 in the Chi-Squared test), as fewer patients were admitted by parents´ initiative in the exposure group (71,4% vs 82,3%) and more brought by the national emergency institute (11,8% vs 3,5%).
The studied outcome happened in 2688 (4,2%) patients: 2433 (3,8%) were admitted to an inpatient facility, 253 (0,4%) were transferred to a level III hospital and 2 (<0,01%) deaths. The distribution of patients with the defined outcome, per group of triage, is represented in Figure 2.
Figure 2. Outcome of the patients according to the exposure group.
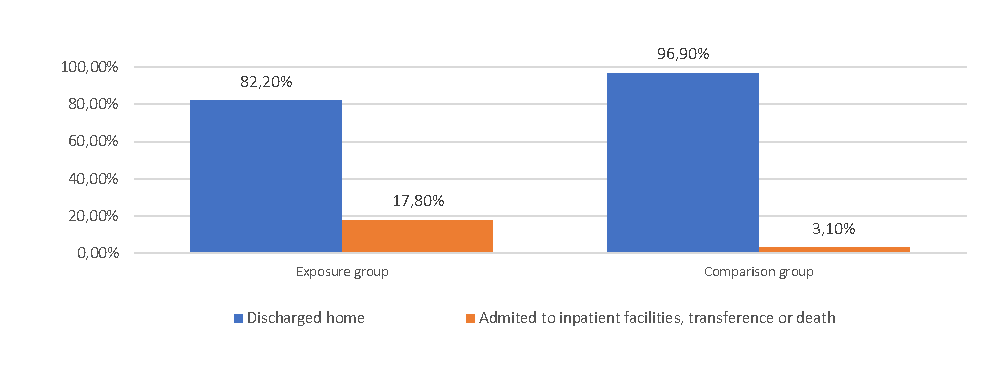
The cumulative incidence rate of the compound outcome in the exposure group was 17,8% and 3,1% in the comparison group, which leads to an attributable risk of 14,7% and a number needed to harm of 7.
The main used flowcharts were “Child that doesn´t feel well” (12970; 20,3%), “Limb Problems” (6607; 10,3%) and “Diarrhea or vomiting” (5810; 9,1%). Specific pediatric flowcharts used also included: “Abdominal Pain in Children” (2622; 4,1%), “Irritable Child” (771; 1,2%), “Worried Parents” (528; 0,8%) and “Crying Baby” (374; 0,6%).
No association was found between the initially chosen flowchart at the admission and the studied outcome, except in flowcharts “Dyspnea in the child” (p=0,02), “Seizures” (p<0,01) and “Overdosage and Poisoning” (p<0,01).
| | | | Discussion | Our study reports a major portion of patients is admitted by self-referral. Although this finding is similar in more countries worldwide, the percentual value is higher than most reported studies.10,11 More equivalent values are found in European settings, with a self-referral of 88% in the UK.12 This translates to easy access to pediatric healthcare but it also traduces a problem of health management and literacy, converging in low rates of patients with the actual need for emergent/urgent care. More than half of the admitted patients had standard or non-urgent priority which differs from other publications´ rates, as standard priority represents 34,0% of admissions.6,13
The difference in median age between the exposure and comparison groups may translate to the higher prevalence of need for urgent care in this age group because of respiratory and infectious pathologies. The high frequency of patients transported by the National Emergency Institute, to whom a more urgent priority was attributed, may be because these types of patients often need differentiated transportation to hospital facilities or a first medical approach outside the emergency department.
The global incidence of the studied outcome in our cohort (4,2%) highlights the low morbimortality in children in our country and the seek for urgent pediatric care to find “resolutivity” as stated in previous studies.13,14 The higher incidence of the outcome in the exposure group is of no surprise, as children presenting with severity signs that require a more urgent medical evaluation are the ones who, more probably, will require inpatient admission for therapeutics or clinical surveillance. Nevertheless, an attributable risk of 14,7% for the MTS at admission is of note since it requires only a very brief evaluation focused on warning signs. Other studies report hospitalization rates of 53,5% in emergent and 28,6% in very urgent priorities, which is higher than what was found in our context.12,15 In our PED, it is a local protocol that in children under 30 days of age, unless a previous discriminator is applied, triage stops at Severe Pain, so that orange priority is attributed. This may pose a bias since most of these patients do get discharged home. This fact, associated with the absence of low-predictability discriminators like the degree of fever in red priority, may contribute greatly to the difference in the number needed to harm between exposure and comparison group vs orange and red priority.
Two of the three most used flowcharts were based on objective complaints (“Limb Problems” and “Diarrhea or vomiting”). It is the author´s opinion that this may translate two different scenarios: the high prevalence of trauma and infection in pediatric emergency departments and therefore, these are the items that are more suitable in those scenarios but it also can be because nurses are more likely to try to find objective complaints as the triage must be performed quickly and what concerns the caregivers may not be what concerns the health staff.
In similar studies, “worried parents” was one of the most used flowcharts (22,4%), but not in our cohort (0,8%).6,8,16 This may happen because “Child that doesn´t feel well”, which was the most used, is very interoperable in most of the discriminators and can be applied to a very large proportion of emergent/urgent situations.
The fact that most flowcharts don´t associate with the outcome is a positive finding since the choice of the flowchart should not indicate the priority of the patient, but rather the discriminator that applies in that scenario. The association between the use of the flowcharts “Seizures” and “Overdosage and Poisoning” is of no surprise since most of these patients must stay under medical surveillance for a non-neglectable period, even if the diagnosis is not confirmed during anamnesis.
The MTS is a dynamic system and improvement or worsening of the clinical condition is taken into account. This may be a bias since only the first attributed priority was assessed. Other limitations must be addressed as this study does not take into account the underlying medical condition of the child or their age group.
MTS aims to ensure priority treatment for patients requiring urgent care. The ideal triage system would bring reliable and standardized information regardless of differences between clinical presentation in age or pathological phenotype subgroups. Its application in pediatric patients can correlate to poor outcomes or the need for inpatient care.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Mackway‐Jones K. Emergency triage: Manchester Triage Group. London: BMJ Publishing Group, 1997.
- Zachariasse JM, van der Hagen V, Seiger N, et al. Performance of triage systems in emergency care: a systematic review and meta-analysis. BMJ Open. 2019;9(5):e026471. [CrossRef] [PubMed] [PMC free article]
- Jesus APS, Okuno MFP, Campanharo CRV, et al. Manchester Triage System: assessment in an emergency hospital service. Rev Bras Enferm. 2021;74(3):e20201361. [CrossRef] [PubMed]
- Magalhães-Barbosa MC, Robaina JR, Prata-Barbosa A, et al. Validity of triage systems for paediatric emergency care: a systematic review. Emerg Med J. 2017;34(11);711-719. [CrossRef] [PubMed]
- Costa JP, Nicolaidis R, Gonçalves AVF, et al. The accuracy of the Manchester Triage System in an emergency service. Rev Gaucha Enferm. 2020;41:e20190327. [CrossRef] [PubMed]
- Amthauer C, Cunha MLC. Manchester Triage System: main flowcharts, discriminators and outcomes of pediatric emergency care.Rev Lat Am Enfermagem. 2016;24:e2779. [CrossRef] [PubMed] [PMC free article]
- Seiger N, Van Veen M, Steyerberg EW, et al. Undertriage in the Manchester triage system: an assessment of severity and options for improvement. Arch Dis Child. 2011;96:653-657. [CrossRef] [PubMed]
- Van Ierland Y, Seiger N, Van Veen M, et al. Alarming signs in the Manchester Triage System: a tool to identify febrile children at risk of hospitalization. J Pediatr. 2013;162(4):862:6-862:6. [CrossRef] [PubMed]
- Van Veen M, Steyerberg EW, Lettinga L, et l. Safety of the Manchester Triage System to identify less urgent patients in pediatric emergency care: a prospective observational study. Arch Dis Child. 2011;96:513-518. [CrossRef] [PubMed]
- Thiongane A, Ndongo AA, Sow A, et al. Epidemiology of Admissions in a pediatric emergency department in Albert Royer Hospital Dakar. Open Journ Pediatrics. 2022;12:188-195. [CrossRef]
- Rothschild M, Gilboa S, Sagi H, et al. Referral, admission and discharge patterns in a pediatric emergency department in Israel. Pediatr Emerg Care. 1994;9(2):72-6. [CrossRef] [PubMed]
- Seiger N, van Veen M, Almeida H, et al. Improving the Manchester Triage System for Pediatric Emergency Care: an International Multicenter Study. PLoS One. 2014;9(1):e83267. [CrossRef] [PubMed] [PMC free article]
- Rati RMS, Goulart LMHF, Alvim CG, et al. "Criança não pode esperar": a busca de serviço de urgência e emergência por mães e suas crianças em condições não urgentes. Ciênc Saúde Coletiva. 2013;18(12):3663-3672. [CrossRef] [PubMed]
- Lima LMB, Almeida NMGS. Procura da emergência pediátrica pelas mães: implicações para a superlotação. Saúde Debate. 2013;37(93):51-61. [CrossRef]
- Roukema J, Steyerber EW, van Meurs A, et al. Validity of the Manchester Triage System in paediatric emergency care. Emerg Med J. 2006;23(12):906-910. [CrossRef] [PubMed] [PMC free article]
- Van Veen M, Steyerberg EW, Van't Klooster M, et al. The Manchester triage system: improvements for paediatric emergency care. Emerg Med J. 2012:1-6. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2024.20
|
| Cite this article as: | | Costa I S, Marques J S, Matos A R R, Oliveira G, Oliveira S, Ferreira P P, Ferreira L M, Baptista C. Manchester Triage and its outcome in a pediatric cohort: what relationship?. Pediatr Oncall J. 2024;21: 56-59. doi: 10.7199/ped.oncall.2024.20 |
|