Inês Silva Costa, João Sousa Marques, Sandra Soares Cardoso, Margarida Tojal, Margarida Montenegro, Lígia M. Ferreira, Joana Pimenta, Cristina Faria.
Pediatrics Department, Centro Hospitalar Tondela-Viseu, Portugal.
ADDRESS FOR CORRESPONDENCE
Inês Silva Costa, Av. Rei Dom Duarte, 3504-509 Viseu, Portugal.
Email: c-ines@hotmail.com | | Abstract | Introduction: The evaluation of an organization's Safety Culture is an essential task to optimize behaviors and processes, improving the provided care and reducing risks and errors.
Materials and Methods: To assess a Pediatric ward, the Hospital Survey on Patient Safety Culture questionnaire, on 12 dimensions of patient safety culture, was applied.
Results: 49 professionals answered the questionnaire, corresponding to 75% of the population. Most participants were female (81.6%), belonged to the medical team (51.1%), were over 45 years old (48.9%) and had more than 13 years of work experience in the evaluated service (51.0%). The dimension with the highest positive perception was teamwork (66.9%), while the one with the lowest positive perception was the non-punitive response to error (18.7%).
Less positive perceptions were more frequent among doctors and younger professionals or those with less work experience.
Conclusions: The results obtained are in line with what is available in the literature, namely the dimensions with the most positive perception which are, across the board, the most frequent in national studies. Overall, there was a low positive perception in various areas, leaving it unclear whether the changes caused by the COVID-19 pandemic had any impact on the perception of professionals.
| | | | Keywords | Safety Culture, Pediatrics, Health Professionals
Abbreviations: HSPSC - Hospital Survey on Patient Safety Culture | | | | Introduction | The World Health Organization defines the concept of patient safety as the method of minimizing the acceptable risk of unnecessary harm associated with healthcare. This issue constitutes one of the main current challenges in healthcare, both in terms of medical practice and legal aspects, with developments in the 21st century. The objective of its study is to create measures that promote safe care, as well as the formation of teams capable of preventing and managing risks.1
Historically, the increasing complexity of healthcare observed in the last century, along with increasingly invasive diagnostic and therapeutic procedures, has enhanced the effectiveness of care but has also exposed it to errors. The production of collateral damage is greater as the effectiveness of modern medicine increases in relation to the associated risk. On the other hand, teamwork is increasingly recognized and implemented in healthcare, so that care is rarely performed by a single person. Thus, the effective and safe management of patients depends not only on individual knowledge but also on how professionals cooperate and interact with each other.2
Safety culture is then defined as the product of individual and group values, as well as competencies and patterns of behavior that determine the commitment to the management and safety of an organization. The perception of healthcare professionals regarding patient safety culture and their self-assessment, both of their own performance and that of the group they belong to, is an essential instrument for establishing improvement measures for safety and quality.3
The assessment of the Patient Safety Culture within an organization is the fundamental pillar for establishing strategies to improve the quality of care and bring about positive changes for patients, professionals and the community. The evaluation process aims to identify areas with opportunities for intervention and improvement, create an environment of active awareness on the subject, enable the evaluation of interventions applied in the medium and long term and comply with the regulations of healthcare regulatory and auditing entities.4,5
Healthcare organizations are constantly influenced by the surrounding physical environment, the community that utilizes them and the professionals who work within them, making these interactions complex and errors inevitable. Errors should be seen as opportunities for positive change, making processes more effective and safer. Healthcare professionals, on the other hand, are the basic and moldable functional units of organizations, which is why addressing their perceptions is considered essential in the evaluation of the culture.2,5
The first phase in developing a stable and robust culture is to identify the culture of the healthcare organization and produce indicators to identify opportunities for improvement. In this way, tools can be created to make organizations more competitive, safe and of high quality.1,6,7
For this reason, the aim was to assess the baseline safety culture of a Pediatric inpatient ward, producing initial indicators on the subject, with the objective of establishing improvement processes and enabling future comparative analysis, paving the way for long-term monitoring of patient safety culture within the organization.
| | | | Methods & Materials | This is a cross-sectional and correlational study conducted in the year 2021 in the Pediatric Ward of a level II hospital, where all children and adolescents between 30 days and 17 years and 364 days of age are admitted for both medical and surgical conditions. The ward consists of 40 beds and had a total of 1272 admissions in 2020. The healthcare team in the ward comprises 65 professionals.
The chosen assessment instrument was the Hospital Survey on Patient Safety Culture (HSPSC) questionnaire8, in its validated Portuguese version. It consists of 42 questions on 12 dimensions of patient safety culture, using a Likert scale with five levels: "strongly disagree" / "never" to "strongly agree" / "always." Additionally, it includes a set of socio-professional questions and two ordinal numerical response questions (Patient Safety Grade and Number of Events Reported in the last 12 months). The applied questions include positively formulated statements (example: “There is good collaboration between the services/units of the hospital that need to work together”) and negatively formulated ones (example: “It is often unpleasant to work with professionals from other services/units of the hospital”). The Likert scale scoring for the latter is reversed in the final analysis. According to recommendations, the five response levels of the Likert scale were recoded into three categories: Negative ("never/rarely" or "strongly disagree/disagree"), Neutral ("neither agree nor disagree" or "sometimes") and Positive ("agree/strongly agree" or "most of the time/always").
From the obtained results, the final score of each dimension falls into either of two groups: Strengths or Areas for Improvement. To classify a particular dimension as a Strength, the criterion of more than 75% positive responses is used, while Areas for Improvement are defined as less than 50% positive responses.
Regarding the last question of HSPSC, responders were asked to attribute a level of perceived Patient Safety Culture in the Service, classifying it into 5 categories (very weak, weak, acceptable, very good or excellent).
Data collection took place from June to August of 2021, ensuring the confidentiality of participants. The paper-based format was used for nurses, assistants and technical staff, while the medical team utilized a digital format. All professionals who worked in the Pediatric Ward during a complete civil year, corresponding to 2020, were eligible to participate. Healthcare professionals whose original service was not Pediatrics or Pediatric Surgery were excluded from the sample due to their limited and gradual exposure to ward procedures.
The collected data underwent frequency analysis and subsequent hypothesis testing for subgroup comparisons. The interpretation of hypothesis tests was based on a significance level of α = 0.05. Data processing was conducted using IBM - SPSS® version 26.0.
The development of this study was formalized with the request for authorization from the Hospital Ethics Committee and subsequent authorization was obtained from the author of the validation for the Portuguese population, Margarida Eiras, both of which were granted. | | | | Results | We obtained 49 responses (75.4%), with a breakdown of 10 (21.3%) from operational assistants, 24 (51.1%) from physicians, 12 (25.6%) from nurses and 1 (2.1%) from technical assistants. Two surveys were missing regarding the professional group. The sample consisted of 40 (81.6%) female professionals, 24 (48.9%) aged over 45 years and 25 (51.0%) with service experience exceeding 13 years.
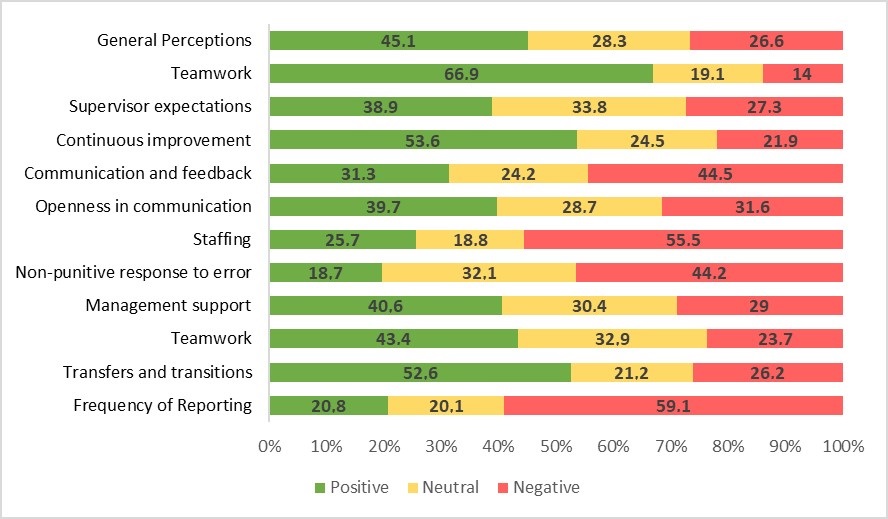
After grouping the questions into the 12 dimensions of Patient Safety (Figure 1), the following were identified as Areas for Improvement: General Perceptions, Supervisor Expectations, Communication and Feedback, Openness in Communication, Staffing, Non-punitive Response to Error, Management Support, Teamwork and Frequency of Reporting. No dimensions were identified as Strengths in terms of Patient Safety.
Figure 1. Relative percentage of perception, per dimension of patient safety culture.
In hypothesis testing, aiming to identify variations in perception among professional groups, years of experience and age groups for each of the 42 patient safety questions, the Kruskal-Wallis test was applied for independent samples with non-normal distribution. Significant differences were found in the subgroup of years of experience for the items "We are actively working to improve patient safety" (p=0.04), "We evaluate the effectiveness of changes we make to improve patient safety" (p<0.01), "We are informed about errors that occur in this Service/unit" (p=0.04), "When an error is made but is caught and corrected before it affects the patient, how often is it reported?" (p=0.03) and "The hospital administration provides a work environment that promotes patient safety" (p=0.03). In all these questions, the perception was more positive among professionals with more years of service experience.
Regarding the age subgroup of healthcare professionals, significant differences in perception were found in the following questions: "There is enough staff to handle the workload" (p=0.04), "Staff members work longer hours, which compromises patient safety" (p<0.01), "It is only by chance that more serious mistakes don't happen in this Service/unit" (p=0.01) and "Patient safety is never sacrificed, even when there is a lot of work" (p=0,04), all of which had a less positive perception among younger individuals.
Among the professional groups, there were differences in two questions: "When an error is made but is caught and corrected before it affects the patient, how often is it reported?" (p=0.02) and "The actions of the hospital administration show that patient safety is a priority" (p=0.02), both of which had a less positive perception among the group of physicians.
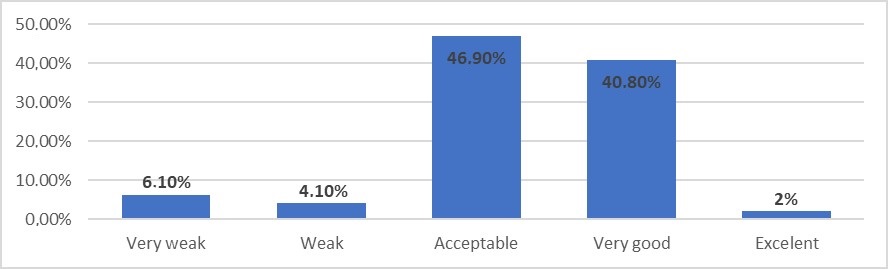
Regarding the perceived level of Patient Safety in the Service (Figure 2), the majority of responses were positive. In the subgroup analysis, a higher positive perception was found among professionals with more years of service (p=0.02).
Regarding the reporting of incidents in the last 12 months, 91.5% of professionals had not reported any incidents. We recorded one professional (2.1%) who had filled out at least 3 incident reports.
Figure 2. Relative percentage of global patient safety perception.
| | | | Discussion | The dimension of General Perceptions on safety culture achieved a positive rate in 45.1% of professionals, slightly lower than that found in other studies. However, there are also few publications, even those related to reassessment after the implementation of targeted measures, in which this dimension is considered a Security Strength. The literature defines strengths as dimensions that achieve at least 75% positive perceptions and therefore are considered to be the best areas in the patient safety culture of the studied organization.2
Teamwork was the most positive dimension (66.9%), close to studies conducted in Portugal (67-76%), but far from the references of international studies, where it is generally considered a Security Strength.9,10,11,12
The dimensions of Continuous Improvement and Transfers and Transitions were relatively positive, with the former being lower and the latter higher than other studies.13,14 It is the authors opinion that Continuous Improvement is a dimension with great potential to achieve better results in reassessments, as the necessary processes for raising awareness and increasing the literacy of nursing professionals in Quality and Safety are now being initiated.
Transitions may be more positive due to the particularity of Pediatric Nursing, where transfers and transitions mostly occur within the Service team, unlike in adult healthcare where various specialties and services, with distinct dynamics and physical hospital locations, participate in patient care.
The Staffing, Frequency of Reporting and Non-Punitive Response to Error were the least positive dimensions. The Staffing dimension shows results similar to Portuguese studies but contrasting with its counterparts in the United States of America, where this dimension reaches 50%.8,12 This reflects the national reality of Portuguese public hospitals, which are increasingly struggling to attract professionals, as indicated in the Annual Health Bulletin of the National Institute of Statistics.15
The Non-Punitive Response to Error was the dimension with the lowest rating (18.7%), consistent with the majority of national and international studies where it has never been considered a Security Strength.9,11,14 On the other hand, it was also one of the dimensions with the highest neutral responses (32.1%). Therefore, it is imperative to ensure confidentiality in event reporting and the existence of an environment where errors are seen as causes rather than consequences. Improving the non-punitive response may potentially also contribute to increasing the frequency of reporting.
The majority of individuals did not report any incidents in the last 12 months (91.5%), possibly because reporting is not seen as a valuable tool for improving safety or, on the other hand, due to the fear that errors will be perceived as a guarantee of punishment.16 Consequently, the Frequency of Reporting dimension was also not very positive (20.8%) and underreporting is a pervasive reality in quality studies similar to ours.13,14 This finding requires targeted measures since analyzing the frequency of errors within each organization allows for specific interventions and focuses on the error mechanism rather than the healthcare professional who committed it.17
The degree of patient safety in the organization was rated positively by a significant number of professionals: 40.8% as very good and 2.0% as excellent. These results are similar to those found in the literature for an initial analysis of the organization's safety culture and it is expected that after measures specifically addressing the identified problems, this value will improve significantly in subsequent reassessments.13,14
Perceptions of safety differences among age subgroups, experience and professional groups should be carefully analyzed. Most physicians in the organization do not exclusively work in Pediatric Nursing but are also involved in Outpatient Clinics and the Emergency Department. Exposure to different contexts and dynamics may, on one hand, hinder integration into the established safety norms and processes in pediatric nursing, but there may also be a comparative factor to other services with lower error risk and where the potential for serious adverse events is rare. On the other hand, nurses, operational assistants and technicians dedicate their activity exclusively to the Pediatric Nursing unit. Older individuals and those with more experience may feel more confident in their actions as healthcare professionals and therefore have a more positive perception of the organization's safety culture.
The authors believe that the dimensions rated more negatively should also be understood within the context of the pandemic period during which data collection took place. Service restructuring, new hygiene and safety standards, circuits, changes in team dynamics and work and increased overtime activity have profoundly altered how professionals perform their duties, particularly in terms of changing processes and procedures that were already well-structured in clinical practice.
This study has some limitations regarding the interpretation and generalization of results, both due to the scarcity of similar studies in the pediatric scope and the number of elements in the organization.
| | | | Conclusion | The perceived Patient Safety Culture among the professionals in our Nursing unit presents several areas for improvement. The Strengths identified are Teamwork, Continuous Improvement and Transfers and Transitions.
On the other hand, the negative aspects highlighted are the Non-Punitive Response to Errors, Frequency of Reporting and Staffing. This underscores the need to create a more conducive environment for learning and process improvement, shifting the burden of error from the healthcare professional to the underlying causes.
This study provides initial indicators for our organization and reveals areas that require deep reflection and the implementation of targeted measures. The use of a validated questionnaire will enable more effective measurement of the impact that Patient Safety Improvement measures may have on our reality. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Kohn LT, Corrigan JM, Donaldson MS. To err is human: building a safer health system: a report of the Committee on Quality of Health Care in America. 2000. Institute of Medicine. Washington, DC: National Academy.
- Eiras, M. Avaliação da Cultura de Segurança do Doente em meio hospitalar: investigação ação numa Unidade de Radioterapia. [PhD dissertation]. Universidade Nova de Lisboa, Lisboa; 2011.
- Fragata, J. Segurança dos doentes: Uma abordagem prática. Lisboa, Portugal: Lide; 2011.
- Nieva NF, Sorra J. Safety culture assessment: a tool for improving patient safety in healthcare organizations. Qual Saf Health Care. 2003;12(Suppl II):ii17-ii23. [CrossRef] [PubMed] [PMC free article]
- Pimenta LC. Avaliação da cultura de segurança do doente e propostas de melhoria. [Masters Degree dissertation]. Escola Superior de tecnologia da saúde de Lisboa, Lisboa;2013.
- Carneiro AV. O erro clínico, os efeitos adversos terapêuticos e a segurança dos doentes: uma análise baseada na evidência científica. Rev Port Saúde Pública. 2010;10:3-10.
- Colla JB, Bracken AC, Kinney LM, Weeks W. Measuring patient safety climate: a review of surveys. Qual Saf Health Care. 2005;14:5;364-366. [CrossRef] [PubMed] [PMC free article]
- Sorra J, Nieva VF. Hospital survey on patient safety culture. Rockville, MD: Agency for Healthcare Research and Quality. 2004. (AHRQ Publication; 04-0041).
- Fernandes A., Queirós P. Cultura de segurança do doente percecionada por enfermeiros em hospitais distritais portugueses. Revista de Enfermagem Referência. 2011;3(4):37- 48. [CrossRef]
- Gomes MJ. Cultura de segurança do doente no bloco operatório [Masters Degree Dissertation]. Escola Superior de Enfermagem de Coimbra. Coimbra, Portugal; 2012.
- Mardon RE, Khanna K, Sorra J, Dyer N, Famolaro T. Exploring relationships between hospital patient safety culture and adverse events. J Patient Saf. 2010;6(4), 226-232. [CrossRef] [PubMed]
- Sorra J, Khanna K, Dyer N, Mardon R, Famolaro T. Exploring relationships between patient safety culture and patients' assessments of hospital care. J Patient Saf. 2012;8(3):131-9. [CrossRef] [PubMed]
- Peralta TJ. Segurança do doente: Perspetivas dos profissionais de um hospital da região centro [Masters Degree Dissertation]. Escola Superior de Enfermagem de Coimbra. Coimbra, Portugal; 2012.
- Sousa AM. Avaliação da cultura de segurança do doente num centro hospitalar da região centro [Masters Degree Dissertation]. Universidade de Coimbra. Coimbra, Portugal; 2013.
- Instituto Nacional de Estatística. Boletim de Estatísticas da Saúde 2015-2021. Lisboa.
- Sorra J, Dyer N. Multilevel psychometric properties of the AHRQ hospital survey on patient safety culture. BMC Health Services Research. 2010; 10(199):1-13. [CrossRef] [PubMed] [PMC free article]
- Direção Geral de Saúde. (2018). Avaliação da Cultura de Segurança do Doente nos Hospitais. Norma de Orientação 005/2018.
DOI: https://doi.org/10.7199/ped.oncall.2024.46
|
| Cite this article as: | | Costa I S, Marques J S, Cardoso S S, Tojal M, Montenegro M, Ferreira L M, Pimenta J, Faria C. Assessing Patient Safety Culture in a Pediatric Ward. Pediatr Oncall J. 2024;21: 146-150. doi: 10.7199/ped.oncall.2024.46 |
|