A Gaffar Billoo, Saira Waqar Ahmed.
Department of Pediatrics, Aga Khan University Karachi, Pakistan.
ADDRESS FOR CORRESPONDENCE
Professor A Gaffar Billoo, Department of Pediatrics, Aga Khan University Karachi, Pakistan.
Email: gaffar.billoo@aku.edu | Introduction
Diarrhea is the second among the most common causes of death in children. Death is usually due to loss of fluid and electrolytes. It is an important factor in development of malnutrition. It is one of the principal causes of morbidity and mortality among children in the developing world. About 4 billion episodes of diarrhea / year cause 1.5 million deaths mostly in children <5 yrs.
For children under 5 years of age in developing areas and countries, there is a median of 3.2 episodes of diarrhea/child/year. This mortality study revealed that 4.9 children per 1000 per year in these areas and countries died as a result of diarrheal illness in the first 5 years of life, a decline from the previous estimates of 13.6 and 5.6 per 1000 per year. The decrease was most pronounced in children aged less than 1 year. Despite improving trends in mortality rates, diarrhea continues to account for a median of 15% of all deaths of children aged less than 5 years in these areas and countries, being responsible for 1.5 million deaths per year. (fig.1)
The major cause of concern is that there has not been a concurrent decrease in morbidity rates attributable to diarrhea. As population growth is focused in the poorest areas, the total morbidity component of the disease burden is greater than previously.(1)
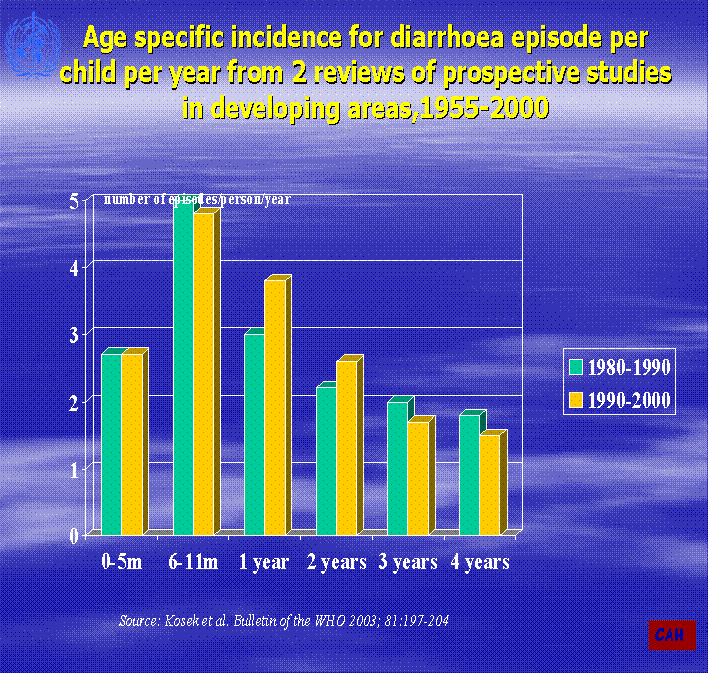
In 1982, on the basis of a review of active surveillance data from studies conducted in the 1950s, 1960s and 1970s, it was estimated that 4.6 million children died annually from diarrhea. In 1992, a review of studies conducted in the 1980s suggested that diarrheal mortality had declined to approximately 3.3 million annually. Both reviews estimated that children in the developing world experienced a median of 3 episodes of diarrhea every year.
Most interventions for diarrheal disease, e.g. increased breastfeeding, better weaning practices, clean water, improved sanitation and higher rates of measles immunization, would be expected to affect mortality as well as morbidity simultaneously. Nutritional status is another factor that may help to explain the de-linking of diarrheal mortality and morbidity rates. The use of oral rehydration therapy is an exception, its increased use over the past two decades probably having been responsible for some of the decrease in case-fatality rates, especially from acute dehydrating diarrhea (2).
In order to achieve further declines in mortality it may be necessary to adopt a more complex approach that would include distinguishing acute watery diarrhea, dysentery and persistent diarrhea, and ensuring appropriate case management for each syndrome. These issues are specifically addressed in the WHO/UNICEF initiative for the improved management of childhood illness (3).
Diarrhea thus still accounts for 1.5 million deaths annually, and each child in the developing world experiences an average of three episode of diarrhea per year. (fig.2)
STEPS FOR PREVENTION OF DIARRHOEA
Proper case management, consisting of oral rehydration therapy and feeding, can reduce the adverse effects of diarrhea, which include dehydration, nutritional damage, and risk of death.
A number of interventions have been proposed for preventing diarrhea in young children, most of which involve measures related to infant feeding practices, personal hygiene, cleanliness of food, provision of safe water, safe disposal of faeces, and immunization. An analysis of the effectiveness, feasibility, and cost of each proposed intervention has shown that some are particularly effective and affordable.
Efforts to prevent diarrhea should focus on a few interventions of proven efficacy. The seven practices identified as targets for promotion are:
Breast-feeding
Improved weaning practices
Use of plenty of water for hygiene and use of clean water for drinking
Hand-washing
Use of latrines and safe disposal of the stools of young children
Measles immunization
Zinc supplementation
Continued feeding the child during diarrhea
Provision of Water supply at community and national level
BREAST-FEEDING
Although breast milk is the best and safest food for young infants, the incidence of breast feeding is declining in most developing countries. Some of the reasons for this decline include the following:-Belief that bottle-feeding is "modern"; the aggressive promotion and marketing of infant formulas; the need for mothers to work away from their children; the lack of facilities for breast-feeding at places of work; fear of not being able to breast-feed adequately and lack of medical and nursing support for mothers who want to breast-feed.
Some major benefits are that breast-fed babies have fewer episodes of diarrhea, less severe episode and a lower risk of dying from diarrhea than babies who are not breast-fed.
Important advantages of breast-feeding are:
Exclusive breast feeding during the first 4-6 months greatly reduces the risk of severe or fatal diarrhea.
Breast-feeding is clean; it does not require the use of bottles, nipples, water, and formula which are easily contaminated with bacteria that may cause diarrhea.
Breast milk has immunological properties (especially antibodies) that protect the infant from infection, and especially from diarrhea; these are not present in animal milk or formula.
The composition of breast milk is always ideal for the infant; formula or cow's milk may be made too dilute (which reduces its nutritional value) or too concentrated (so that it does not provide sufficient water) and may provide too much salt and sugar.
Breast milk is a complete food; it provides all the nutrients and water needed by a healthy infant during the first 4-6 months of life.
Breast-feeding is economical. One of the expenses associated with feeding breast milk substitutes are the cost of fuel, utensils, and special formulas, and of the mother's time and knowledge required in formula preparation.
Breast-feeding immediately after delivery encourages the 'bonding' of the mother to her infant; this has important emotional benefits for both and helps to secure the child's place within the family.
Exclusive breast feeding protects against infectious morbidity and mortality during the early months of life (7). In Peru, for example young infants who received on-nutritive liquids, artificial milks, or solid foods in addition to breastfeeding had 2-5 times greater prevalence of diarrhea than their exclusively breastfed counterparts. (8) Similar results have been reported from the Philippines. (9) Thus, if complementary foods are introduced earlier than necessary, they are likely to cause increased rates of otherwise preventable childhood diarrhoea. (10) Nevertheless, the optimal age for introduction of non-breast milk foods has been debated because excessively delayed initiation of these foods could result in low energy and nutrient intakes and consequent malnutrition. The World Health Organization currently recommends exclusive breast feeding for four to six months, whereas UNICEF states that complementary feeding should be initiated at about six months. Because of the considerably increased risk of diarrhea associated with introduction of these foods, a two-month difference in their timing of introduction of theses foods could have important implications for global burden of diarrhea.
If possible, infants should be exclusively breast-fed during the first 6 months of life. At 6 months of age, infants should start to receive cereals and other foods to meet their increased nutritional requirements, but breast-feeding should be continued at least until one year of age and preferably till age of two years. Breast milk given after the age of 6 months is an important source of nutrients and it continues to help protect the child from repeated episodes of severe diarrhea.
IMPROVED WEANING PRACTICES
Weaning is the process by which an infant gradually becomes accustomed to an adult diet. During weaning, supplementary foods other than milk are introduced in order to meet the child's increased nutritional demands. However, beast milk remains an important part of the diet.
Weaning is a hazardous period for many infants. This is because the child may not receive food of adequate nutritional value and the food and drinks provided may be contaminated with pathogenic microbes, including those that cause diarrhea. The danger is that the child will become undernourished due to an inadequate diet and repeated episodes of diarrhea, or will succumb to dehydration caused by an acute episode of diarrhea. Unfortunately, these processes are inter-related: under-nutrition leads to frequent and more severe episodes of diarrhea and diarrhea accelerates the development of under-nutrition.
Some specific problems associated with weaning that can lead to diarrhea are:
- Preparing and storing weaning foods in unhygienic way that leads to bacterial contamination and
- Giving milk or other drink prepared with contaminated water or in a contaminated feeding bottle.
Mothers should be taught ways of preparing, giving, and storing weaning foods that minimize the risk of bacterial contamination. These include:
Washing her hands before preparing weaning foods and before feeding the baby.
Preparing the food in a clean place
Cooking or boiling the food well when preparing it.
If possible, preparing the food immediately before it is eaten.
Keeping food in a cool place; refrigerating it if possible. Covering food that is being kept.
Protect food from insects and animals as they carry pathogenic organisms and are potential sources of contamination of food.
Feeding the baby with a clean spoon, from a cup, or with a special feeding spoon.
Feeding bottles should never be used.
What health care providers should do?
Make the assessment of weaning diets and weaning education a routine element of well-baby programmes. This should be coordinated with the use of growth charts to identify children with growth faltering, for whom improved feeding is especially important.
Evaluate the nutritional status of children with diarrhea, by measuring mid upper arm circumference, weight for age, or weight for height: refer all children with severe undernutrition to a treatment centre where nutritional rehabilitation is possible.
For moderately undernourished children, ask about the child's weaning diet and feeding practices. Advise the mother on ways of increasing the child's intake of safely prepared, energy-rich foods. If possible, follow up the child after diarrhea stops until the weight or rate of growth has become normal.(4)
PROPER USE OF WATER FOR HYGIENE AND DRINKING
Most infectious agents that cause diarrhea are transmitted by the fecal-oral route. This includes transmission by contaminated drinking water or contaminated food, and person-to-person spread. A plentiful supply of clean water helps to encourage hygienic practices, such as hand washing, cleaning of eating utensils. Theses practices can interrupt the spread of infectious agents that cause diarrhea. Clean water is essential, however, for drinking and for preparing food.
HAND WASHING
Parents can help to protect young children against diarrhea by adopting certain hygiene practices. One very important practice is hand-washing. Hands should be washed carefully after defecation before handling food and before feeding. Good hand washing requires the use of soap (or a local substitute), plenty of water (5).
USE OF LATRINES
Human faeces should be disposed of in a way that prevents them form coming into contact with hands or contaminating a water source. This is best a achieved through regular use of a well-maintained latrine. The proper use of latrines can reduce the risk of diarrhea to almost the same extent as improved water supplies, but the greatest benefit occurs when improvement in sanitation and water supply are combined and education is given on hygienic practices.
MEASLES IMMUNIZATION
Children who have measles., or have had the disease in the previous four weeks, have a substantially increased risk of developing severe or fatal diarrhea or dysentery (there is some evidence that the increased risk lasts up to six months after measles). Because of the strong relationship between measles and serious diarrhea, and the effectiveness of measles vaccines, measles immunization is a very cost-effective measure for reducing diarrhea morbidity and deaths. Measles vaccine given at 9 months of age can prevent up to 25% of diarrhea-associated deaths in children under 5 years of age.
What healthcare providers should do?
providers Include screening and referral for Immunization, including measles immunization, as a routine in well-baby visits.
providers Ask mothers always to bring the child's immunization card when they come to the clinic for any reason. Check the immunization status of every patient and make sure that those who need it are immunized during the visit, unless there is a valid reason against it.
ZINC SUPPLEMENTATION
Zinc is an important micronutrient for a child's overall health and development. Zinc is lost in greater quantities during diarrhea; replacing the lost zinc is important to help the child recover and to keep the child healthy in the coming months. It has been shown that zinc supplements given during an episode of diarrhea reduce the duration and severity of the episode, and lower the incidence of diarrhea in the following 2-3 months. Therefore, all patients with diarrhea should be given zinc supplements as soon as possible after diarrhea has started (6).
CONTINUE TO FEED THE CHILD
The child should be offered small amounts of nutritious and easily digestible foods frequently. If the child is breast fed, try to increase the frequency and duration of feed. Feeding during the diarrhea episode provides the nutrients the child needs for the growth and prevents weight loss. After diarrhea has stopped an extra meal each day for a week will help the child regain weight lost during diarrhea.
TALKING WITH MOTHERS ABOUT PREVENTING DIARRHOEA
Most activities that help to prevent diarrhea must take place in the home. However, mothers and other family members cannot practice diarrhea prevention until they have learned what this involves and understand how best to carry out each preventive activity. Information on the prevention of diarrhea can be provided in a variety of ways, e.g., at community meetings, through schools, during home visits and visits to a health centre.
Provision of water supply at community and national level
Last but not the least, important is the provision of safe drinking water supply to all the communities at the national level in all the developing countries, where diarrhea continues to be major cause if morbidity and a leading cause of death. This needs the commitment of policy and decision makers and politicians of poor countries to allocate adequate resources for basic needs of life, like water and sanitation. It is only then that sizable reduction in diarrhea morbidity will be achieved.
Figure 1
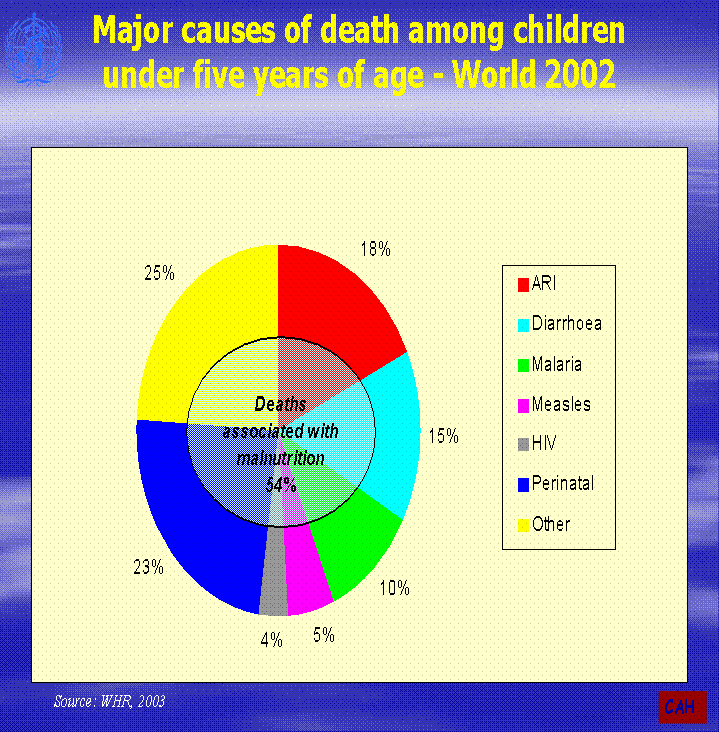
Figure 2
 | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Snyder JD, Merson MH. The magnitude of the global problem of acute diarrheal disease: review of active surveillance data. Bulletin of the World Health Organization 1982; 60:604-13.
- World Health Organization. The World health report 1999: making a difference. Geneva : World Health Organization; 1999.
- World Health Organization. The world health report 2000-health system: improving performance: Geneva World Health Organization; 2000.
- The treatment of diarrhea. A manual for physicians and other senior health workers, WHO/CAH/03.7, World Health Organization, Geneva.
- Excerpted from: WHO 1996. Basic Principles for the preparation of safe food for infants and young children. Geneva WHO.
- Gahl, R. et al., "Effect of zinc supplementation on clinical course of acute diarrhea. Report of a Meeting, New Delhi May 2001. Journal of health, population and nutrition, vol. 19, no. 4 Dec 2001, pp.338-346.
- Butte , NF Energy requirements of infants. Europ J Clin Nutr 1995; 50: S24-S36.
- Brown KH, Black RE, Lopez de Romana G, Creed de Kanashiro H. Infant feeding practices and their relationship with diarrheal and other diseases. Pediatrics 1989; 83: 31-40. [PubMed]
- Popkin BM, Adair L, Akin JS, Black R, Briscoe J, Flieger W. Breastfeeding and diarrheal morbidity. Paediatrics 1990;86: 874-82.
- Adair l, Popkin BM, VanDerslice J, Akin J, Guilkey D, Black R, Briscoe J, Flieger W Growth dynamics during the first two years of life: a prospective study in the Philippines. Eur J Clin Nutr 1993; 47: 42-51. [PubMed]
|
| Cite this article as: | | Billoo A G, Ahmed S W. Prevention of Diarrhea. Pediatr Oncall J. 2007;4: 19-22. |
|