Bader Al-Khabbaz, Mustafa Abbas, Mahmoud Abdulmenam, Nasser Al-Dalal.
Department of surgery, Farwania Hospital, Kuwait.
ADDRESS FOR CORRESPONDENCE
Bader Al-khabbaz, P.O. Box 401, Surrah, Kuwait.
Email: baker_110@hotmail.com | | Keywords | | Enteritis Cystica Profunda, Intussusception | | | | Abstract | | Enteritis Cystica Profunda (ECP) is a very rare benign disease entity of the small intestine. It is defined as mucin-filled cystic spaces, partially lined by non-neoplastic columnar to cuboidal or flattened epithelium found predominantly in the submucosa of the small bowel. We report a case of 12 year-old boy with small bowel intussusception caused by Enteritis Cystica Profunda. The patient had symptoms mimicking acute appendicitis except the passage of "red-currant jelly-like" diarrhea which drew attention to the possibility of intussusception which was confirmed by ultrasonography. Diagnostic laparoscopy was followed by laparoscopic assisted resection anastomosis of affected bowel which precipitated the intussusception. It contained a 2x2 cm mass intraluminally presenting the leading point of the intussusception, and proved histologically as Enteritis Cystica Profunda. A review of the English medical literature revealed only four cases in children with similar symptoms in the last 32 years. Conclusion: Enteritis Cystica Profunda is a very rare benign condition of the small intestine. We are reporting the 5th case worldwide in pediatric population. Small-bowel intussusception is often over-looked due to nonspecific clinical presentation. Ultrasound is very reliable method of diagnosis of intestinal intussusception. Laparoscopy can safely be used in this matter diagnostically as well as therapeutically. | | | | Case Report | A previously healthy 12 year old boy presented complaining of acute onset of lower abdominal pain for 2 days duration; the pain was colicky in nature associated with anorexia & vomiting. After obtaining a detailed history from the mother, she reported that the child passed one episode of bloody diarrhea, which raised the suspicion of intussusception. His past medical history was negative for any previous diseases as well as for family history. On examination his vital signs were normal, abdominal examination revealed lower abdominal tenderness mainly located at right iliac fossa with positive Rebound tenderness; digital rectal examination revealed no bleeding or masses; his white blood count = 12,600/cu mm; there were dilated small bowel loops seen on abdominal X-ray at the right iliac fossa. The provisional diagnosis was between Intussusception, Acute Appendicitis and Meckel's diverticulum. An ultrasound abdomen was requested to differentiate between acute appendicitis and intussusception and showed thickened multiple small bowel loops in lower abdomen and wall thickening up to 5 mm & diameter up to 2-6 cm; intussuscepting ileal loop seen in the pelvic cavity measuring 9x5 cm; there was free fluid in the pelvis surrounding bowel loops. The impression was intussusception of ileal loops.
Fig 1a and 1b: Longitudinal and axial image showing wall within wall appearance and concentric sign appearance respectively typical of intussusception.
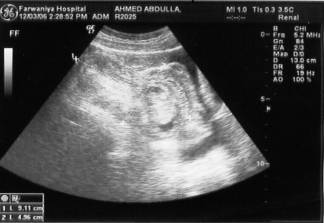
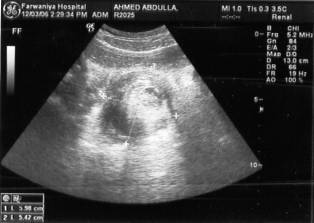
The patient underwent emergency diagnostic laparoscopy which revealed significant amount of free serous fluid, small bowel intussusception located 30 cm from ileocaecal valve, and a subserosal mass 2x2 cm, and multiple mesenteric lymph nodes. Laparoscopic assisted resection anastomosis of a 10 cm small bowel segment was done. On table examination of specimen, it showed 2x2 cm submucosal mass. Histologically, the section show mucus-containing cyst in the wall of small intestine with entrapped inflammatory cells and congested vascular spaces. The diagnosis was cystica profunda (Figure 2). The patient had uneventful recovery and he was discharged on the 6th post-operative day.
Figure 2: Lakes of mucin with nests of epithelial cells and acute inflammatory cells in the wall (10x10)
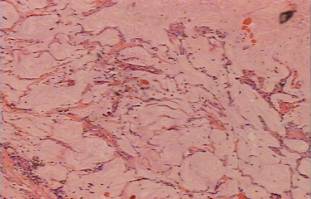 | | | | Discussion | Colonic Submucosal Cyst is a benign epithelial cyst that develops in the mucosa and submucosa of the colon which was first described by Stark in cases associated with chronic dysentery in 1766. Virchow, 1863 reported similar case producing multiple polypoid lesions in the colon and introduced the term Colitis Cystica Profunda (CCP) (1; 2). Goodall and Sinclair provided an elaborate description of CCP in 1957 (3). This type of benign cysts can develop in any part of the gastrointestinal tract but mainly in the colon as more than 144 cases were reported in the English literature (2, 4). In adults, it is often mistaken for mucinous carcinoma and invasive carcinoma or can represent premalignant change or the initial pathological feature of malignancy, but nuclear morphology of the epithelium in CCP is not neoplastic. (1, 5, 6)
Macroscopically and histologically similar disorder has been discovered in the esophagus, gallbladder, stomach and small intestine. Cysts develop in the small intestine are called Enteritis Cystica Profunda (ECP) however they are the small intestinal analogue of CCP with similar histological features: mucin-filled cystic spaces, partially lined by non-neoplastic columnar to cuboidal or flattened epithelium in the submucosa of the small bowel (5). It is much less common than the CCP with only 13 cases reported; four of these cases were among the pediatric population (12-22). There is controversy regarding the etiology of the CCP and ECP. Most investigators favor acquired pathogenesis, it has a high incidence of concurrence with diseases that tend to irritate the bowel due to mucosal ulceration or inflammatory damage to submucosa, such as Ulcerative Colitis, Dysentery, Crohn's Disease, Adenomatous Polyposis, Peutz-Jeghers Syndrome, spastic colitis, other causes can be calcifications, fibrosis and ossified deposits within the mucin lakes. Ectopic submucosal glands or cysts have been observed after gastrointestinal surgery, radiation therapy and exteriorization of the small intestine in experiments on rats (2, 7). Others believe it is congenital; this hypothesis is supported by the following findings: embryological studies demonstrated submucosal cyst in various locations of the gastrointestinal tract. The fact that this conditions occurs mainly in young adults and pediatric age groups.
In our case the benefit of history taking especially in children, can get additional information, and the use of ultrasound were helpful in diagnosing the case, of small-bowel intussusception which is often over-looked in this age group due to nonspecific clinical presentation. Ultrasound is extremely beneficial in the evaluation of acute pediatric abdominal disease, such as hypertrophic pyloric stenosis, intussusception, and acute appendicitis. (10) In the four cases reported, only two cases including our case used the ultrasound for diagnosing intussusception. The accuracy in detecting appendicitis and intussusception are respectively close to 95% and 100% with experienced radiologist (11).
Laparoscopy is used for diagnosing these cases in case of doubt and also in the management adding a good outcome. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Levine DS: Solitary rectal ulcer syndrome. Are solitary rectal ulcer syndrome and localized colitis cystica profunda analogous syndromes caused by rectal prolapse-Gastroenterology 1987,92:243-253.
- Guest CB, Reznick RK: Colitis cystica profunda. Review of the literature. Dis Colon Rectum 1989, 32:983-988. [CrossRef] [PubMed]
- Goodall HB, Sinclair ISR: Colitis cystica profunda. J Pathol Bact 1957, 73:33-42. [CrossRef]
- Epstein SE, Ascari WQ, Ablow RC, et al: Colitis cystica profunda: Am J Clin Pathol 1966, 45:186-201. [CrossRef] [PubMed]
- Saul SH, Wong LK, Zinsser KR: Enteritis cystica profunda: Association with Crohn's disease. Hum Pathol 1986, 17:600-603. [CrossRef]
- Sakuria Y, Kobayashi H, Imazu H, Hasegawa S, Matsubara T, Ochiai M, et al. the development of an elevated lesion associated with colitis cystica profunda in the transverse colonic mucosa during the ulcerative colitis: report of case. Surg. Today 2000; 30:69-73. [CrossRef] [PubMed]
- Kyriakos M, Condon SC: Enteritis cystica profunda. Am J Clin Pathol 1978, 69:77-85. [CrossRef] [PubMed]
- O'Donnell N. Enteritis cystica profunda revisited, Hum Pathol 1987; 18:1300-1. [CrossRef]
- Johnson RL, Antonius JI: Colitis cystica profunda. Am Surg 1979, 45:743-747. [PubMed]
- Radiol clin North Am. 2004 Mar; 42(2):445-56. Review. [PubMed]
- J Radiol. 2001 Jun: 82(6 pt 2):764-78; discussion 779-80. Review. Frensh.
- Baillie EE, Abell MR. Enteritis cystica polyposa. Am J Clin Pathol 1970; 54:643-9. [CrossRef]
- Karnak I, Gogus S, Senocak ME, Akcoren Z, Hicsonmez A. Enteritis cystica profunda causing ileoileal intussusception in a child. J Pediatr Surg 1997; 32:1356-9. [CrossRef]
- Salman AB, Gogus S, Taynel FC, akcoren Z, Hicsonmz A. Enteritis cystica profunda mimicking acute abdominal picture in a twelve-years-old boy. Eur J Pediatr Surg 1998; 8:168-9. [CrossRef] [PubMed]
- H. Sunagawa et al.: ECP Causing Ilioileal Intussusception. Surg today 2005; 35:164-167. [CrossRef] [PubMed]
- Aftalion B, Lipper S: Enteritis cystica profunda associated with Crohn's disease. Arch Pathol Lab Med 1984 (letter), 108:532-533.
- Anderson NJ, Rivera ES, Flores DJ: Peutz-Jeghers syndrome with cervical adenocarcinoma and enteritis cystica profunda. West J Med 1984, 141:242-244. [PubMed] [PMC free article]
- Dippolito AD, Aburano A, Bezouska CA, et al: Enteritis cystica profunda in Peutz-Jeghers syndrome. Report of a case and review of the literature. Dis Colon Rectum 1987, 30: 192-198. [CrossRef] [PubMed]
- Pirozynski WJ: Cystica malformation of the bowel. Hum Pathol 1987, 18:310-311. [CrossRef]
- Spjut HJ, Helgason AH, Trabanino II JG: Jejunitis cystica profunda in a hamartomatous polyp. Am J Surg Pathol1987, 11: 328-332. [CrossRef] [PubMed]
- Alexis J, Lubin J, Wallack M: Enteritis cystica profunda in a patient with Crohn's disease. Arch Pathol Lab Med 1989, 113:947-949. [PubMed]
- Zidi SH, Marteau P, Piard F, et al: Enterocolitis cystica profunda lesion in a patient with unclassified ulcerative enterocolitis. Digest Dis Science 1994, 39: 426-432. [CrossRef] [PubMed]
|
| Cite this article as: | | Al-Khabbaz B, Abbas M, Abdulmenam M, Al-Dalal N. Enteritis Cystica Profunda Causing Intussusception. Pediatr Oncall J. 2007;4: 35. |
|