Karuna Thapar, Naresh Jindal, Gaurav Dhawan.
Department of Pediatrics, Government Medical College, Amritsar.
ADDRESS FOR CORRESPONDENCE
Dr Karuna Thapar, Department of Pediatrics, Government Medical College, Amritsar, India.
Email: kthapar2000@yahoo.com | | Abstract | | Cutaneous tuberculosis is rare and constitutes only about 0.15% of all dermatological outpatients in our country however a combination of abdominal tuberculosis with cutaneous tuberculosis is extremely rare. We present a 13 year old male with fever, multiple discharging non-healing cutaneous ulcers and progressive ascites for the last 6 months. Ascitic tap and skin biopsy were suggestive of tuberculosis. | | | | Introduction | | The prevalence of tuberculosis is around 30 million globally and approximately 1/3 rd of cases are in India. Cutaneous tuberculosis is rare and constitutes only about 0.15% of all dermatological outpatients in our country however a combination of abdominal tuberculosis with cutaneous tuberculosis is extremely rare and authors could not find any such presented case in the Indian literature so far. We report this case due to its rarity. | | | | Case Report | A 13 year old male child was admitted with fever, multiple discharging non-healing cutaneous ulcers and progressive ascites, for the last 6 months. There was history of previous hospital admissions with various antibiotics given in last 6 months. On physical examination, child was having microcephaly (head circumference - 42 cms), multiple non-healing ulcers, tense ascites with dilated veins and enlarged liver-palpable 5 cms below the costal margin. Multiple ulcers in different stages of healing were evident in groin, behind the knee, over the feet and ankle regions. Some ulcers were also showing changes of healing with disfiguring scars and contractures (figure 1) probably due to prior antibiotic therapy (quinolones & aminoglycosides). The floor of ulcers showed dirty-yellow slough and the base was composed of subcutaneous and underlying tissue, ulcer edges were inflamed, edematous, tender, and undermined in some areas.
Laboratory testing revealed that the child was anemic with hemoglobin 7.0 mg/dl. Total count was 5800/cmm and erythrocyte sedimentation rate (ESR) 110 mm at 1 hour. Liver functions were deranged with normal serum proteins and renal functions. Chest X- ray was normal. VDRL test and ELISA for HIV were negative. Ultrasonography abdomen did not reveal any abnormality except for fluid collection seen in peritoneal cavity. A standard tuberculin test was positive with 12 mm induration. Ascitic tap revealed straw colored fluid with total cell count of 2700/ µl, 78% lymphocytes and protein content 3.4 g/dl favoring tuberculosis. Sputum-smear examination for acid-fast bacilli (AFB) on 3-consecutive days was negative. A skin biopsy was taken from the ulcer edge and patient started on broad spectrum antibiotics but no improvement seen in 7 days. Report of skin biopsy revealed granulation tissue with areas of necrosis, epitheloid and langerhans giant cells as in tuberculosis. All antibiotics were stopped.
4 drugs anti tubercular therapy (ATT) with isoniazid: 5 mg/kg/day, Rifampin: 10-20 mg/kg/day, Pyrazinamide: 15-30 mg/kg/day and Streptomycin: 20-40 mg/kg/day for two months were started along with steroids. isoniazid tablets were powdered and sprinkled over all the ulcers. Patient showed remarkable improvement within first 7 days of therapy. Ascites subsided and ulcer healing was seen. On follow up child had complete recovery after two months and was asked to continue on ATT.
Figure1
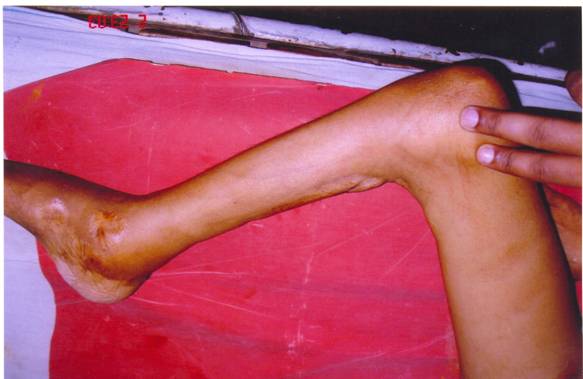 | | | | Discussion | The recent resurgence of tuberculosis is worldwide probably due to increase spread of HIV infection. Tuberculosis can involve any organ system in the body. While pulmonary tuberculosis is the most common presentation, extrapulmonary tuberculosis (EPTB) is also an important clinical problem (1-3). EPTB is more difficult to diagnose it than its pulmonary counterpart and constitutes about 10 percent of all cases of tuberculosis.
Tuberculosis can involve any part of the gastrointestinal tract. The major pathogen is Mycobacterium tuberculosis but from some parts of the world cases caused by M. bovis, an organism found in dairy products, are still reported (4). The most frequent sites of involvement in gastrointestinal tract are caecum, ileocecal region and terminal ileum. Other parts of the gastrointestinal system are rarely exposed to tuberculous involvement. The patient of abdominal tuberculosis may be asymptomatic initially but in advanced cases abdominal pain and swelling, unexplained fever, weakness, anorexia and weight loss predominate in the clinical picture. In this case the child had progressively increasing abdominal swelling as the presenting feature and ascitic fluid biochemistry pointing towards abdominal tubercular infection.
Cutaneous tuberculosis is essentially an invasion of the skin by Mycobacterium tuberculosis. Cutaneous tuberculosis represents 1.5 percent of all cases of EPTB (5). Incidence of childhood cutaneous tuberculosis is more in girls (6). The incidence of childhood cutaneous tuberculosis in an Indian series conducted over 25 years was estimated at 18.7 percent (7). Because it is a paucibacillary form of tuberculous infection, culture is often negative and the diagnosis is mainly based on the Mantoux test, the histopathologic picture, and the response to multi drug therapy as seen in this case. Where facilities permit, the polymerase chain reaction can improve diagnostic accuracy.
Treatment is based on triple or quadruple anti-tubercular therapy for minimum 6 months (8). After treatment, disfiguring scars are frequent in children. Misdiagnosis, neglect, or late diagnosis of cutaneous tuberculosis in children may result in extensive disease.
Detailed clinical scrutiny, non-response to broad spectrum antibiotics, high ESR, a negative ELISA test for HIV were suggestive of tuberculosis in this case. Positive tuberculin test, ascitic tap biochemistry in favor of tuberculosis further strengthened our suspicion and the diagnosis was confirmed histopathologically from skin biopsy. Finally, the excellent response to multi-drug anti-tubercular therapy clinched the diagnosis in this case. Case was thus named as of Abdomino-cutaneous tuberculosis. Occurrence of cutaneous tuberculosis in combination with abdominal tuberculosis is extremely rare.
Despite prevention programs, tuberculosis is still progressing endemically in developing countries and authors would like to stress upon the need for careful evaluation, accurate diagnosis & complete treatment of the patients with tuberculosis. | | | | Acknowledgement | Authors would like to thank Ms. Raj for her help in the preparation of the case report.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Fanning A. Tuberculosis: 6 Extrapulmonary disease. CMAJ 1999; 160: 1597-1603. [PubMed] [PMC free article]
- Iscman MD. Tuberculosis in relation to human immunodeficiency virus and acquired immunodeficiency syndrome. In: Iseman MD, editor. A clinician's guide to tuberculosis. Philadelphia: Lippincott Williams and Wilkins; 2000: 199-252.
- Dutt AK, Stead WW. Epidemiology In: Schlossberg D, editor. Tuberculosis and nontuberculous mycobacterial infection. Philadelphia: W.B. Saunders Company; 1999: 3-16.
- Gorbach SL. Tuberculous of the gastrointestinal tract. In: Sleisenger MH, Fordtran JS, eds. Gastrointestinal Disease Pathophysiology, Diagnosis, Management. Philadelphia: WB Saunders1993; 2: 1158- 1161.
- Kumar B, Muralidhar S. Cutaneous tuberculosis: A-twenty-year prospective study. Int J Tuberc Lung Dis 1999; 3: 494-500. [PubMed]
- Ramesh V, Misra RS, Beena KR, Mukherjee A. A study of cutaneous tuberculosis in children. Pediatr Dermatol 1999; 16 (4): 264-269. [CrossRef] [PubMed]
- Kumar B, Rai R, Kaur I, Sahoo B, Muralidhar S, Radotra BD. Childhood cutaneous tuberculosis: a study over 25 years from northern India. Int J Dermatol 2001; 40: 26-32. [CrossRef] [PubMed]
- Morand JJ, Cuguilliere A, Sayag J. Tuberculose cutanee. Encycl Med Chir (Elsevier, Paris), Dermatologie, 98-360-A-10, 1999, p12.
|
| Cite this article as: | | Thapar K, Jindal N, Dhawan G. Abdomino-Cutaneous Tuberculosis: A Rare Case Report. Pediatr Oncall J. 2007;4. |
|