Ajay Garg1, Raman Wadhera1, S P Gulati1, Jagjit Singh2, Rohit Goyal3.
1Department of Otorhinolaryngology, PGIMS, Rohtak,
2Department of Pediatrics, PGIMS, Rohtak,
3Deen Dayal Upadhyay Hospital, New Delhi.
ADDRESS FOR CORRESPONDENCE
Dr. Jagjit Singh, H.No.44, Street No.11, Jawahar Nagar, Hisar, Haryana-125001, India.
Email: drjagjitsingh@hotmail.com | | Abstract | | Nasopharyngeal carcinoma (NPC) is well known for its marked invasive & metastatic potential and manifests in a variety of forms. Cranial nerve(s) involvement is seen in 20% cases of NPC. But clinically evident facial nerve paresis/palsy is a rare presentation. Authors describe a case of NPC in an 11 years female child who presented with right sided cervical mass with facial nerve paresis. | | | | Keywords | | Nasopharyngeal carcinoma (NPC), Facial nerve paresis. | | | | Introduction | | Nasopharyngeal carcinoma (NPC) pragmatically refers to a specific category of carcinoma, arising from nasopharyngeal epithelium is found with highest frequency in southern China in the central Guangdong province and Guangxi Autonomous region. NPC is relatively rare neoplasm in Caucasian populations including Indians (age standardized rate is less than 1/100000). Characteristic bimodal pattern of age distribution is seen, with a small peak in late childhood and second peak in 50-60 years of age and male to female ratio being 2:3 (1). Although etiology of NPC remains obscure, but a susceptible genetic constitution clearly plays a part and some environmental co-factors are equally important. (1) The WHO (World Health Organization) has categorized NPC as: TYPE- I Squamous cell carcinoma, TYPE- II Non- keratinizing carcinoma (Transitional cell carcinoma), TYPE-III Undifferentiated carcinoma (Lymphoepithelioma, anaplastic, clear cell and spindle cell variants) (2). Facial nerve involvement by NPC is rarely reported in the literature making present case an interesting one. | | | | Case Report | An 11 years old female child presented with 8 months history of right sided cervical mass gradually increasing in size with occasional history of nasal obstruction. There was no history of epistaxis, fever, weight loss or any other audiological symptoms. She had been taking anti-tubercular drugs for the last 6 months on prescription of a general practitioner, who diagnosed her to be a case of tuberculous lymphadenitis. She had no significant relief which prompted her parents to consult an otorhinolaryngologist. Examination revealed a single, non-tender, hard, cervical mass of size 3 x 4cm in size, fixed to the underlying structures in right jugulodigastric area. Anterior rhinoscopy revealed totally obliterated bilateral choanae. Slight weakness of right orbicularis oculi muscle was also noticed when she was asked to close the eye along with deviation of angle of mouth to left suggesting right facial nerve involvement. Her further neurological, audiological, ophthalmological and laryngeal examination was normal. Fine needle aspiration cytology of the cervical mass showed features of undifferentiated carcinoma. Subsequently Non Contrast Computed tomography scan of nose & nasopharynx demonstrated mass filling the nasopharynx (Figure 1). Patient underwent nasoendoscopic biopsy, which confirmed the diagnosis of undifferentiated nasopharyngeal carcinoma (Type III). Patient was referred for radiotherapy. External beam radiation in the dosage of 66GY in 33 divided fractions were delivered to the nasopharynx with concurrent chemoradiation (carboplatin, 5 -FU).
Figure 1- Coronal CT image showing bone erosion & extension of tumor to infratemporal fossa.
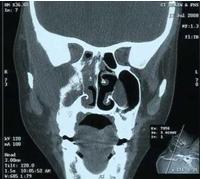
| | | | Discussion | Malignant lesions of the nasopharynx are perhaps the most commonly misdiagnosed, most poorly understood, and most pessimistically regarded of all tumors of the upper respiratory tract. (3) Early diagnosis of NPC is usually difficult attributed to its insidious onset and non-specific features in initial stages. The symptomatology of NPC varies depending on the stage of the disease at the time of presentation. Commonest presenting symptom includes painless cervical lymphadenopathy (75%), epistaxis and nasorespiratory symptoms (30%), audiological symptoms (tinnitus, otalgia, deafness) (20%), neurological symptoms (headache, cranial nerve palsies, and Horner's syndrome) (20%), and metastases which can be locoregional (paranasal sinus, parapharyngeal space, infratemporal fossa, orbit, parotid and cervical lymphadenopathy) or distant (bone, lung and liver). (1)
One fifth of patients have symptoms of cranial nerve involvement at the time of diagnosis. Proximity of fossa of Rosenmuller to foramen lacerum and middle cranial fossa floor allows direct tumor extension into the cranium and involvement of the adjacent nerves. Trigeminal nerve involvement is found most frequently followed by abducent nerve producing facial pain & paresthesia and diplopia respectively. (4) Facial nerve palsy caused by NPC is uncommon; its incidence is less than 1%. Among all cases of facial nerve paralysis, 5% have been reported to be involved by tumors. After emerging from the brainstem, the facial nerve enters the cerebellopontine angle (CPA), the temporal bone (internal auditory canal, middle ear and mastoid) and the parotid before branching out to supply the facial muscles. Tumor involvement any where along the course can cause facial palsy.(5) Swaski et al in a series of patients of NPC studied that 4.6% cases had clinically evident facial nerve palsy. (6) Facial nerve involvement at CPA is by metastasis (via hematogenous, CSF, or leptomeningeal), while in middle ear it is either direct spread (via Eustachian tube or direct invasion from parapharyngeal space) or by metastasis. Facial nerve involvement at parotid attributes to lymphatic dissemination of tumor to the parotid lymph nodes via retropharyngeal group of lymph nodes as seen in our case. (5) Various syndromes involving multiple cranial nerves in association of NPC have also been described in the literature. Gradenigo's syndrome is defined by triad of sixth nerve palsy, pain and parasthesia in the distribution of fifth nerve and otitis media. Involvement of cranial nerves III & IV indicates more advanced disease along cavernous sinus called as cavernous sinus syndrome. Rarely, NPC may affect IX, X, & XI cranial nerves in parapharyngeal space, causing jugular foramen syndrome.(4) NPC involving nine cranial nerves in a patient has also been reported in the literature.(7)
NPC is extremely radiosensitive tumor and the mainstay of treatment for primary local and regional disease is invariably radiotherapy, almost irrespective of the stage of the disease. Additional chemotherapy is advocated in patients with advanced disease to improve overall results. Local & regional failures are controlled by surgical salvage. (1) | | | | Conclusion | | Early diagnosis of NPC is difficult attributes to the hidden location of the disease & wide spectrum of nonspecific and sparse symptoms. So an otolaryngologist should be well acquainted with this situation; if a patient presents with isolated or multiple cranial nerve palsies. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Woo JKS, Hasselt CAV. Nasopharyngeal carcinoma. In: Glesson M ed. Scott's-Brown Otorhinolaryngology, Head and surgery, 7th ed., Hodder Arnold, London, 2008 Vol.2 : 2448-2474. [CrossRef]
- Shanmugaratnam K, Jobin LH. Histological typing of upper respiratory tract tumors, No. 19. Geneva, World Health Organisation, 1978: 32-33.
- Scanlon PW, Devine KD, Woolner LB. Malignant lesions of the nasopharynx. Ann Otol Rhinol Laryngol. 1958; 67: 1005-1021. [CrossRef] [PubMed]
- Peters LG, Rischin D, Corry J, Harari PM. Cancer of the nasopharynx. In: Harrison LB, Sessions RB, Hong WK eds. Head & Neck cancer- a multidisciplinary approach, 2nd ed. Lippincott Williams, Williams & Wilkins, Philadelphia. 2004: 529-559.
- Wong-Kein Low "Facial palsy from metastatic nasopharyngeal carcinoma at various sites: Three reports _ Original Article - Brief Article". Ear, Nose & Throat Journal. FindArticles.com. 01 Sep.2008. http://findarticles.com/p/articles/mi_mOBUM/is_2_81/ai_83516035.
- Swaski S, Sugano H, Hirayama T. Analytical aspects of symptoms of nasopharyngeal malignancies. In: de-The G, Ito Y, eds. Nasopharyngeal carcinoma: etiology and control. IARC Sci Pub 1978; 20: 147-163.
- Kaushik ML, Pandey D, Sood BR, Thakur S. Nasopharyngeal carcinoma presenting as multiple cranial involvement. JIACM 2003; 4: 61-63.
|
| Cite this article as: | | Garg A, Wadhera R, Gulati S P, Singh J, Goyal R. Nasopharyngeal Carcinoma Presenting as Facial Nerve Paralysis. Pediatr Oncall J. 2010;7: 43-44. |
|