Tushar B Jagzape, Bhavana Lakhkar, Amol Lohakare, Sachin Damke, Sumeet Thakur.
Department of Pediatrics, J N Medical College,Sawangi -Meghe, Wardha, India.
ADDRESS FOR CORRESPONDENCE
Dr Tushar Jagzape, M2- 8 Meghdootam Apartment, JNMC campus, Sawangi (M), Wardha, Maharashtra.
Email: tusharjagzape@yahoo.com | | Keywords | | Menkes disease, neurodegeneration, developmental delay, low serum ceruloplasmin | | | A 6 months boy was referred by a pediatrician as a case of developmental delay for evaluation. As per the mother, he was normal upto 3 months of age. He was able to recognize his mother and had achieved partial neck holding. After that he not only did not achieve any further milestones but also lost the milestones already achieved. Development age at the time of presentation was that of a newborn. He was of consanguineous marriage born at term at home and did not cry immediately after birth. His birth weight was 2.3kg. Neonatal period was uneventful. There was no history of any previous hospitalization for any illness. Parents also did not give any history of convulsion. Family history was insignificant. He had received vaccines as per the National immunization schedule and there was no significant adverse reaction after vaccination. The baby was on exclusive breast feeding. On examination his vitals were stable. He had mild pallor. The child had hypopigmented wooly hair (Figure 1). No other specific dysmorphology was noted. On systemic examination, he had hypotonia, and reflexes were diminished. He had cortical thumb and neonatal reflexes like sucking, rooting reflex were present. His hearing was normal and baby turned his head to diffuse light. Fundus examination was showing early changes of optic atrophy. Other system examination was normal. Microscopic examination of the hair shaft showed pili torti, MRI revealed demyelination involving the optic radiation and occipital lobe. Serum ceruloplasmin and serum copper were low. Ultrasound of abdomen and pelvis was normal. Thus a diagnosis of Menkes disease was confirmed. Genetic study or plasma catecholamine levels were not done because of non availability of facility and high cost.
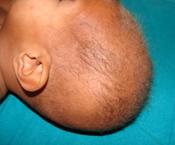
Figure 1- Typical sparse wooly hair of Menkes Kinky hair disease
Menkes disease (MD) is a genetic disease of X- linked recessive inheritance first described by Menkes et al in 1962. Menkes disease or trichopoliodystrophy is characterized by progressive degeneration of the central nervous system, treatment resistant convulsions, and hair abnormalities. (1) It is also called kinky hair disease because of the characteristic phenotype of boys with kinky, stubby, white hair. (2) MD is one of the four known disorders of copper metabolism. Together with occipital horn syndrome, it results from copper deficiency secondary to disturbances in copper transport. Wilson's disease and Indian childhood cirrhosis, on the other hand, result from the toxic effects of copper accumulation in the liver. (3) The clinical picture is caused by a defect in copper transporting ATPase (ATP7A), resulting in defects of key copper dependent enzymes, including Lysyl oxidase, Cytochrome C oxidase, dopamine β-hydroxylase, tyrosinase, and super oxide dismutase. Depigmentation of hair and skin pallor are due to tyrosinase deficiency, hypothermia is due to Cytochrome C oxidase deficiency and Lysyl oxidase deficiency causes tortuous arteries in brain, progressive vascular changes predispose to thrombosis and deficient blood supply to the developing brain. (4-6)
Infants with classic Menkes disease typically appear healthy until 2 to 3 months of age. Premature delivery is very frequent, as are neonatal hypothermia and hyperbilirubinemia. Hypothermia may also occur in older infants. Neonatal symptoms may resolve, and the babies may seem normal during next 2 or 3 months. At 3 months of age, they start to demonstrate developmental delay, hypotonia, intractable seizures and failure to thrive. Cerebral degeneration then dominates the clinical picture. (5,6). In our case the baby was born at term, but there was history of birth asphyxia. The child was apparently normal upto 3 months of age. The developmental delay, hypotonia and failure to thrive were noted by the mother after that. Our patient did not have convulsion till he presented to us. Hair abnormalities are the most striking signs in this syndrome. Several hair shaft abnormalities like pili torti, trichorrehexis nodosa, trichoclasis and trichoptilosis have been documented, with pili torti being the most common. (7,8) Our patient had hypopigmented hair with pili torti.
The clinical history and the appearance of the infant should suggest the diagnosis. Microscopic examination of the hair is very helpful even in a mild case. (9) In healthy children, concentrations of plasma copper and ceruloplasmin tend to be low during the first 3 weeks of life, may decrease even after the 6th week of life, and can sometimes be low even up to 6 months of age. In any case, plasma copper below 25% of normal range and low plasma ceruloplasmin concentrations can be diagnostic of MD after the 3rd week of life. (10) If doubt still exists, the diagnosis can be confirmed by demonstrating the intracellular accumulation of copper and decreased efflux of 64Cu from cultured fibroblasts. (11) Though lot of progress has been made in diagnostic work up not much is available as therapeutic options. copper histidine therapy has been tried but with variable results. It is important to recognize this disease and start treatment as early as possible to prevent neurological deficit. Early diagnosis may also be helpful in genetic counselling.
Financial disclosure - We state that we have not received any financial help or funding for this case. There is no financial interest.
Acknowledgements - The authors would like to thank Dr Amol Hazare, Consultant Pediatrician at Warora, district Chandrapur for referring this patient to us. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Giugliani R, Rotta N, Laser LFL, Costa AC, Wojciechowski M, Flores RZ, Drachler ML. Menkes Disease: Report of a case. Rev Brasil Genet. 1986; IX: 515-520.
- Bekiesinska-Figatowska M, Rokicki D, Walecki J, Gremida M. Menkes` disease with a Dandy-Walker variant: case report. Neuroradiology. 2001; 43: 948-950. [CrossRef] [PubMed]
- Petrukhin K, Gilliam TC. Genetic disorders of copper metabolism. Curr Opin Pediatr. 1994; 6: 698-701. [CrossRef] [PubMed]
- Danks DM, Campbel PE, Walker-Smith J et al. Menkes kinky-hair syndrome. Lancet. 1972; 1: 1100-1102. [CrossRef]
- Menkes JH. Kinky hair disease: twenty five years later. Brain Dev. 1998; 10: 77-79. [CrossRef]
- Menkes JH, Wilcox WR. Inherited metabolic disease of the nervous system. In: Menkes JH, Sarnat HB, Maria BL, editors. Child Neurology. 7th ed. Philadeiphia: Lippimcott Williams & Wilkins; 2006. pp:115-117. [PubMed]
- Smith VV, Anderson G, Malone M, et al. Light microscopic examination of scalp hair samples as an aid in the diagnosis of pediatric disorders: retrospective review of more than 300 cases from a single centre. J Clin Pathol. 2005; 58: 1294-1298. [CrossRef] [PubMed]
- Whiting DA. Structural abnormalities of the hair shaft. J Am Acad Dermatol. 1987; 16: 1-25. [CrossRef]
- Barzegar M, Fayyazie A, Gasemie B, Shoja MAM. Menkes Disease: Report of two cases. Iran J Pediatr. 2007; 17: 388-392.
- Itin P, Happle R, Schaub N, Schiller P, Izakovic J, Fistarol SK. Hereditary metabolic disorders. In Schachner LA, et al, editors. Pediatric Dermatology. 3rd ed. Edinburgh: Mosby; 2003. p. 350-364.
- Tumer Z, Horn N. Menkes disease: recent advances and new aspects. J Med Genet 1997; 34: 265-274. [CrossRef] [PubMed]
|
| Cite this article as: | | Jagzape T B, Lakhkar B, Lohakare A, Damke S, Thakur S. Menkes disease. Pediatr Oncall J. 2011;8: 23-24. |
|