Pancham Kumar, Rohit Vohra.
Department of Paediatrics, IGMC Shimla, Himachal Pradesh, India.
ADDRESS FOR CORRESPONDENCE
Dr Pancham Kumar, Department of Paediatrics, IGMC Shimla, Himachal Pradesh, India.
Email: panchamdr@gmail.com | | Abstract | | Eosinophilic enteritis (EE) is rare gastrointestinal disorder of unknown etiology which was first described by Kaijser in 1937. EE may affect any part of gut, but stomach and small intestine are most common area to be affected. EE has varied presentation which depends upon the site and extent of involvement. EE is diagnosed by demonstration of eosinophilic infiltration of gut wall and eosinophilia in the peripheral blood picture. We present a 13 years old boy with EE who had recurrent episodes of abdominal pain, vomiting and eosinophilic ascites. He was eventually diagnosed as EE based on histopathology. He responded to steroids and is doing well on follow-up. | | | | Introduction | | Eosinophilic gastroenteritis or eosinophilc enteritis (EE) is a rare and poorly understood entity which can affect both children and adults. Various allergic disorders are present in almost half of patients. (1) Proposed pathogenesis involves T cell paradigm imbalance which leads to increased cytokine production leading to IgE and eosinophil production. (1) Eosinophilic infiltration which is hallmark of EE can be patchy or diffuse which results in inflammation and ulcerations and eventually leading to various presentations of EE which depend upon the site and extent of involvement. (2) We present a 13 years old boy with EE who had recurrent episodes of abdominal pain, vomiting and eosinophilic ascites. | | | | Case Report | A 13 years old boy presented with recurrent episodes of abdominal pain, increasing abdominal distension and vomiting for three years. He had been to various physicians over this period and was treated for worm infestations, giardiasis & abdominal tuberculosis but had no relief. He had also received multiple courses of antibiotics. On presentation to us, his weight was 36 kg and height was 150 cms. General physical examination was normal except pallor was present. On abdominal examination, there was tense ascites. Other systems were normal. On investigations haemoglobin was 9.2 gm%, white cell count was 10500 cells/cumm with 64% eosinophils (absolute eosinophils count 6,720 cells/cumm), total protein was 7.2 gm% and albumin 3.6 gm%. Renal and liver function tests were normal. Chest X-ray, pulmonary function test, echocardiography, stool examination were also normal. Ascitic fluid had 780 cells/cumm (84% eosinophils) with absolute eosinophils count of 655 cells/cumm and albumin was 3.8 g/dl. On retrospective review of his previous records eosinophilia was persistent feature in his blood counts as shown in table 1. CT abdomen showed diffuse gut wall thickening of small intestine, parts of large intestine and stomach; ascites; mesentric lymphadenopathy and mesentric hypervascularity. Upper gastrointestinal (GI) scopy revealed edematous duodenal folds and duodenal biopsy showed ulceration of lining epithelium and increase in villi to crypt ratio with increased eosinophils in lamina propria and muscularis mucosa as shown in Fig 1. Diagnosis of eosinophilic enteritis was confirmed and patient was started on prednisolone (40mg/day) and montelukast (5mg/day). His symptoms resolved and he achieved normal blood counts in a span of two weeks. After eight weeks, steroids were tapered off and montelukast was tapered after 3 months. On follow-up child is asymptomatic for last 8 months.
Table1. Previous complete blood counts and percentage of eosinophils in peripheral smear
| Date |
White cell count (cells/cumm) |
Percentage of eosinophils |
Absolute eosinophil count (cells/cumm) |
| Feb 2013 |
8400 |
54% |
4536 |
| Sept 2013 |
11800 |
48% |
5564 |
| March 2013 |
9700 |
62% |
6040 |
Figure 1: Histopathology of duodenum - Lamina propria showed increased eosinophils (>50 eosinophils/hpf). Muscularis mucosa had scattered eosinophils and fibrosis.
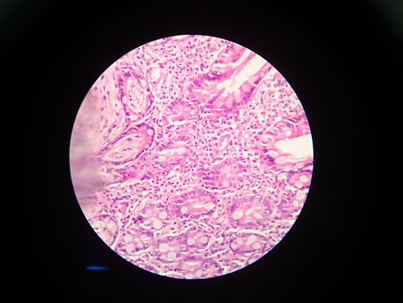
| | | | Discussion | | The exact incidence of EE is not known in India or world and only 280 cases have been reported in the medical literature till date. (3) Kim et al from Korea reported 31 new cases of eosinophilic gastroenteritis in his study over 33 years. (4) In India, 7 cases of eosinophilic gastroenteritis were reported by Venkataraman et al over a period of 10 years. (5) EE can affect present any age, peaking between third to fifth decade with slight male predominance. (3) Etiopathogenesis of EE is not well explored yet however presence of various allergic disorders and high IgE levels in EE patients suggest that hypersensitivity response plays a major role in pathogenesis. Eosinophils, cytokines (IL-3, IL-5and IL-13) and eotaxin play a crucial role in the pathogenesis of EE and which also support its intimate association with allergic disorders. (2) Inflammation of gut wall leads to various presentation of EE which depend upon the site and extent of involvement. Depending upon the area of gut involved, mucosal, muscularis, or serosal forms have been described. EE can present as diarrhea, abdominal, pain, cramping, malabsorption, and gastrointestinal loss of blood and protein. Definitive diagnosis requires eosinophilic infiltration (>20 eosinophils per high-power field) on biopsy which can be diffuse or patchy while excluding its other causes. (6) Other investigative work up shows peripheral blood eosinophilia, high eosinophil count in ascitic fluid and thickened gut wall and abdominal lymphadenopathy on imaging. (7) Active eosinophilic infiltration can also be demonstrated on white blood cell scintigraphy. Ulcers, hemorrhages or nodularity is seen on endoscopy. Differential diagnosis includes inflammatory polyp, intestinal parasite infestations, collagen disorder, hypereosinophilia syndrome, Churg-Strauss syndrome, Crohn's colitis, ulcerative colitis and lymphomas. Treatment modality depends on the severity of the clinical manifestations. Mild disease are treated symptomatically and small number of patients enter remission with dietary restriction alone. In patients with severe presentation or failure of dietary modifications or requiring surgical interventions, steroids arethe cornerstone of treatment. (1) Duration of steroid treatment depends upon the response to treatment. If patient requires long term steroids to maintain remission, alternate day steroids or other modalities like antihistamine and mast-cell stabilizing agents, selective leukotriene receptor antagonist can be used. A monoclonal eotaxin antibody (CAT-213) and agents to enhance eosinophil apoptosis are some upcoming modalities. (8) Intestinal perforation and/or obstruction may require surgery. (2) | | | | Conclusion | | EE should be suspected in patients having gastrointestinal symptoms with peripheral eosinophilia. Early diagnosis enables successful treatment, and decreases unnecessary use of medications, painful and costly interventions and morbidity. Histopathologic findings of eosinophilic infiltration are required to confirm the diagnosis due to the nonspecific clinical presentations. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Triantafillidis JK, Parasi P, Cherakakis P, Sklavaina M. Eosinophilic gastroenteritis: Current aspects on etiology, pathogenesis, diagnosis and treatment. Ann Gastroenterol.2002; 15: 106-115.
- Baig MA, Qadir A, Rasheed J. A Review of Eosinophilic Gastroenteritis. J Natl Med Assoc 2006, 98: 1116-1119.
- Nguyen MT. Eosinophilic Gastroenteritis. Available from: http://emedicine.medscape.com/article/174100-overview#showall. Accessed on 14 Dec 2014.
- Kim NI, Jo YJ, Song MH. Clinical features of eosinophilic gastroenteritis [in Korean]. Korean J Gastroenterol. 2004;44: 217-223. [PubMed]
- Venkataraman S, Ramakrishna BS, Mathan M. Eosinophilic gastroenteritis-an Indian experience. Indian J Gastroenterol. 1998; 17: 148-149. [PubMed]
- Macedo T, MacCarty RL. Eosinophiiic ileocolitis secondary to Enterobius vermicularis: case report. Abdom Imaging. 2000; 25: 530-532. [CrossRef]
- Marco-Domenech SF, Gil-Sanchez S, Jornet-Fayos J. Eosinophilic gastroenteritis: percutaneous biopsy under ultrasound guidance. Abdom Imaging. 1998; 23: 286-288. [CrossRef]
- Bochner BS. Verdict in the case of therapies versus eosinophils: the jury is still out. J Allergy Clin Immunol. 2004; 13:10. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2015.33
|
| Cite this article as: | | Kumar P, Vohra R. Eosinophilic Enteritis: A Rare Cause of Ascites in Children. Pediatr Oncall J. 2015;12: 44-45. doi: 10.7199/ped.oncall.2015.33 |
|