Ana Luisa Correia, Carolina Castro, Joana Machado Morais, Ana Lurdes Aguiar
Department of Pediatrics, Hospital Pedro Hispano, Unidade Local de Saúde de Matosinhos, Matosinhos, Portugal
Address for Correspondence: Miss. Ana Luisa Correia, Avenida Padre Sá Pereira nº27, lote 8, RC direito, Esposende, 4740-206, Portugal.
Email: analuisacorreia57@gmail.com
|
Question :A previously healthy 17-year-old girl presented at the emergency department with acute pain in the left popliteal fossa with 4 hours of evolution, which woke her from sleep. She also mentioned paresthesias in the painful area. Fever, recent injuries, strenuous exercise, consumption of any medication or tobacco use were denied.
On presentation, she was hemodynamically stable and afebrile, walking with a limp. Palpation of the left popliteal fossa revealed tenderness and movement maneuvers showed pain with knee extension and flexion; the remaining physical examination did not reveal any significant abnormality, namely, any cutaneous findings.
A complementary study showed normal blood count, normal renal and liver function, negative C-reactive protein, normal lactate dehydrogenase and normal erythrocyte sedimentation rate (9 mm/h). The coagulation profile and D-dimer test were within the reference range.
A vascular surgeon performed a doppler ultra-sound and ruled out vascular pathology. She was observed by an orthopedist, who prescribed a left leg X-ray. This exam revealed a radiotransparent multiloculated bone lesion with a sclerotic rim located in the distal femur, without associated periosteal reaction, cortical breach or associated soft tissue mass (Figures 1 and 2).
This lesion was diagnosed as a small non-ossifying fibroma, which was considered an imaging finding, not related to the patient’s complaints. Since the physical examination was normal and the complementary study did not reveal abnormal findings, the patient was discharged with symptomatic treatment. To follow the evolution of the non-ossifying fibroma, she was referred to an orthopedic consultation.
Figure 1. Conventional X-ray, anterior view of the left leg. 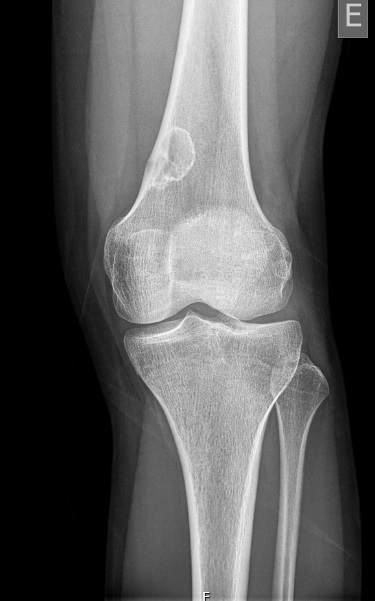 Figure 2.
Figure 2. Lateral view of the left leg. 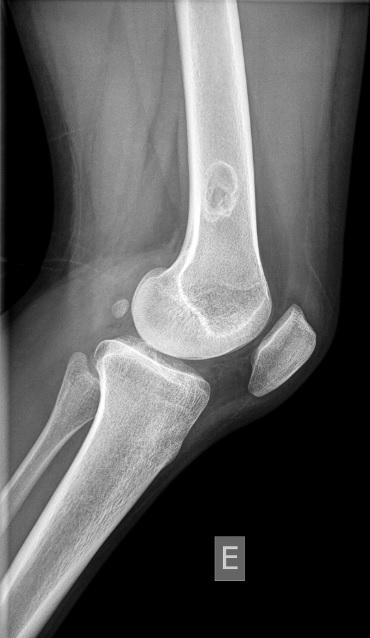 What is the diagnosis?
|
Discussion :
Benign bone tumors are frequently discovered incidentally. It’s fundamental to recognize the characteristic radiographic features of these lesions, avoiding unnecessary advanced imaging and invasive diagnostic studies. 1,2,3,4,5,6 A careful anamnesis can lead us to the correct diagnosis: nonaggressive, nonmalignant bone lesions usually are asymptomatic, but may cause pain in association with pathologic fracture or neurovascular compression. 1,2,3,4,5,6 On the other hand, malignant bone tumors may be associated with pain that awakens the child from sleep and is more rapidly progressive. Our patient presented with potential warning signs and an abnormal leg X-ray. However, the fibroma was small and was not considered the cause for the patient’s complaints; hence the importance of correctly identifying these benign lesions, that do not require treatment.
Non-ossifying fibromas are very common in pediatric age (30% of estimated prevalence). 1,2 Most of these are asymptomatic and heal spontaneously with time. Larger lesions may be painful and weaken the bone, predisposing to pathological fractures. 1,2,3,4,5,6 According to Ritschl classification, which distinguishes the four different stages of a non-ossifying fibroma 5, this lesion was a stage B: a lesion with a thin sclerotic border, near the metaphysis; this stage has the highest risk for pathologic fracture 5, thus the need for follow up in this patient.
We intend to familiarize clinicians with this condition and its radiographic features, since it can raise a suspicion of malignancy, especially in the presence of confounding symptoms. | References : | - Emori, M., Tsuchie H., Teramoto A., Shimizu J., Mizushima E., Murahashi Y., et al. "Non-Ossifying Fibromas and Fibrous Cortical Defects around the Knee - an Epidemiologic Survey in a Japanese Pediatric Population." BMC Musculoskeletal Disorders 2022;volume(23):378-383. https://doi.org/10.1186/s12891-022-05330-9.
- Sakamoto A., Arai R., Okamoto T., and Matsuda S.. "Non-Ossifying Fibromas: Case Series, Including in Uncommon Upper Extremity Sites." World Journal of Orthopedics 2017;Volume(8), no.7:561-566. https://doi.org/10.5312/wjo.v8.i7.561
- Bovée, J., Pancras, H. "Non‐Ossifying Fibroma: A Ras‐Mapk Driven Benign Bone Neoplasm." The Journal of Pathology 2019;volume(248):127-30. https://doi.org/10.1002/path.5259.
- Bowers, L., Cohen D., Bhattacharyya I., Pettigrew J., and Stavropoulos M. "The Non-Ossifying Fibroma: A Case Report and Review of the Literature." Head and Neck Pathology 2013;volume(7):203-210. https://doi.org/10.1007/s12105-012-0399-7.
- Herget, G., Mauer D., Krauß T., Tayeh A., Uhl M., et al. "Non-Ossifying Fibroma: Natural History with an Emphasis on a Stage-Related Growth, Fracture Risk and the Need for Follow-Up." BMC Musculoskeletal Disorders 2016;Volume(17):147-153. https://doi.org/10.1186/s12891-016-1004-0.
- Jashmitha R., Zhang C., Thahir A., and Krkovic M. "Imaging of Non-Ossifying Fibromas: A Case Series." Cureus, 2021;13(3):e14102 https://doi.org/10.7759/cureus.14102.
|
|
| Correct Answers : |  100% 100% |
Last Shown : Feb 2026
|