Sumeet Pitkar1, Keyur Mahajan2, Shailesh Kanvinde3, Tarun Kumar1.
1Department of Pediatrics, Deenanath Mangeshkar Hospital and Research Centre, Pune, Maharashtra, India,
2Pediatric Infectious Diseases, Deenanath Mangeshkar Hospital and Research Centre, Pune, Maharashtra, India,
3Consultant Haemato-oncologist, Deenanath Mangeshkar Hospital and Research Centre, Pune, Maharashtra, India.
ADDRESS FOR CORRESPONDENCE
Dr Sumeet Pitkar, Department of Pediatrics, Deenanath Mangeshkar Hospital and Research Centre, Pune - 411004, Maharashtra, India.
Email: sumeetpitkar@gmail.com | | Abstract | Aim: The Primary aim of study was to assess the role of the immature platelets fraction in predicting severity of thrombocytopenia and occurrence of bleeding manifestation in dengue patients.
Material and Methods: Blood samples were collected in a K2EDTA bulb. Haemogram with IPF was done at first visit, 2nd IPF measurement was only done in patients with platelet count remaining below 50,000 and /or does not increase by more than 20,000 from baseline. Clinical parameters were assessed simultaneously.
Relevant data was collected and IPF values were analysed and matched with the platelet nadir, time to nadir and recovery of platelets. Correlation of IPF to incidence of bleeding manifestation was also studied.
Results: We compared IPF at baseline in two groups (<30000/cc mm and >30000/cc mm Platelet counts) to platelet nadir and time to nadir with normal and high IPF values. No statistically significant difference was noted in these two groups. We also compared the baseline IPF values to platelet recovery more than 1 lakh/cc mm or increased platelet count >20,000/cc mm. Correlation of baseline IPF values to bleeding manifestations was compared in the same two groups of patients with normal and high IPF values was done and results were not statistically significant.
Conclusion: Immature Platelet Fraction is not useful to predict either subsequent platelet nadir, time to reach platelet nadir or bleeding manifestations. From our study Platelet count at baseline can predict bleeding but Immature Platelet Fraction did not add any more information. | | | | Keywords | | Dengue, Immature Platelet Fraction, Thrombocytopenia, Pediatric Dengue. | | | | Introduction | Dengue, a mosquito-borne virus, can kill. It often has thrombocytopenia. Dengue is caused by one of the four Flaviviruses (DENV 1-4) spread by the Aedes aegypti mosquito. It is common in tropical and subtropical regions. Dengue causes symptomatic or asymptomatic seroconversion. Symptomatic dengue is dynamic and systemic. Its clinical spectrum encompasses severe and non-severe symptoms.
In moderate to severe cases, the illness begins quickly after incubation, followed by three phases: febrile, critical, and recovery. Since the condition is dynamic, its severity frequently becomes obvious during defervescence, the change from febrile to afebrile, which commonly corresponds with the critical period. Complex diseases can be managed easily, cheaply, and effectively to save lives if treated properly and promptly. Understanding and being aware of clinical issues that occur during the disease's distinct phases leads to reasonable case management and a positive clinical result.1
The primary haematological abnormalities in dengue are thrombocytopenia and leucopoenia.
IPF, a new biomarker that detects youthful, reticulated platelets, is utilised to understand cellular dynamics in mild to severe dengue infection. It implies a portion of bigger bone marrow-released platelets. Platelets containing more RNA are assessed by automated haematology analysers with reticulocyte detection channels and reported as %-IPF.2
Platelet production in bone marrow raises IPF. Thus, its peripheral blood sample measurement measures marrow platelet generation like a reticulocyte count measures red cell production.2
If IPF is serially monitored in dengue patients with thrombocytopenia, a rising trend may indicate active bone marrow and a platelet count recovery, avoiding transfusion and its complications like alloimmunisation, immunosuppression, graft versus host disease, and infection transmission.
Dengue fever patients' platelet counts can be predicted by IPF. Because there are no clear criteria for managing thrombocytopenia in dengue patients, the treating physician can use IPF% to forecast platelet recovery to minimise unnecessary platelet transfusion.3
The IPF is recognised by Sysmex XE2100 haematology analyser in the reticulocyte channel using a fluorescent dye and a precisely developed gating mechanism and counted by IPF master software. The Pathology laboratory of Deenanath Mangeshkar Hospital regarded IPF between 0.2 and 6.6% normal.
Role of immature platelet fraction
In 2007, Pons et al. examined the relationship between Reticulated Platelets (RP) and Immature Platelet Fraction (IPF) in thrombocytopenia and the diagnostic value of IPF. Healthy controls with normal platelets and thrombocytopenic patients with central, peripheral, and non-immune peripheral thrombocytopenia were studied. 66 cases and 14 controls were examined. In patients with peripheral platelet destruction and thrombocytopenia, RP and IPF correlated well.15
Reticulated platelets (RP) represent the newest platelets in circulation and have residual mRNA in their cytoplasm. They appear on blood films stained with fresh methylene blue. Thiazole orange or auramine O fluorescent dyes are used in RP flow cytometry. Thiazole orange and auramine O have different RP reference values. According to RP analysis in patients with thrombocytopenic disorders, RP measurement can estimate bone marrow thrombopoiesis, differential diagnose, and explain pathophysiology.16
A similar study by Monteagudo et al. found that flow cytometry measurement of RP from whole blood can screen for thrombocytopenia with high or low thrombopoietic activity. Activated RP over 11% has high sensitivity and good specificity for thrombocytopenia with increased thrombopoetic activity.17
Carol Briggs' 2004 extensive study developed an automated method to reliably quantify reticulated platelets, expressed as the immature platelet fraction (IPF). An IPF is identified by flow cytometry and a nucleic acid-specific dye in the reticulocyte/optical platelet channel. The flowcytometric IPF measurement uses a proprietary fluorescent dye with polymethine and oxazine. These two dyes stain red cell and platelet reticulocyte RNA through the cell membrane. Mature platelets are blue spots and immature ones are green dots, making up the IPF parameter.2
AIMS AND OBJECTIVES
AIM:
To assess the role of the immature platelet fraction in predicting severity of thrombocytopenia and occurrence of bleeding manifestation in dengue patients.
OBJECTIVES
1. Primary objectives:
Correlation of IPF at baseline
• With subsequent platelet count nadir.
• Occurrence of bleeding manifestation.
2. Secondary objectives:
• Predict time of platelet recovery to more than 1 lakh.
• Correlation of IPF at baseline with Increase of platelet count by >20,000 per cc mm.
• Define the range of baseline IPF value in Dengue patient with thrombocytopenia.
• Correlate change in IPF value in 48hr/72hr with baseline (if platelet count <50,000/cc mm)
| | | | Methods & Materials | Study Design: Prospective, Observational study.
Study Population: All the patients <18 years admitted/treated in OPD in Deenanath Mangeshkar Hospital with Dengue (Dengue NS1/Dengue IgM positive).
Study period: July 2018 to April 2020.
Inclusion Criteria: All of below
1. Dengue NS1 and /or IgM positive.
2. Age <18 years.
3. Thrombocytopenia (platelet count<100000 per cc mm)
Exclusion Criteria: any one of below
1. Patients with other platelet disorders.
2. Patients on any chemotherapy or any drug known to cause thrombocytopenia.
3. Marrow failure syndromes.
4. Liver diseases /Hypersplenism.
5. Any patient who received platelet transfusion
In these cases, thrombocytopenia has different causes, so it will confound the assessment findings.
METHODOLOGY:
• Patient registered in OPD/admitted in Deenanath Mangeshkar Hospital and Research Centre.
• Fulfilling inclusion criteria
• Baseline assessment including clinical examination and lab investigation.
Clinical examination
- Patient was assessed at baseline for bleeding.
- Other manifestation of dengue.
- Hypotension
- Oedema
- Ascites
- Pleural effusion
- Bleeding scores
- Lab investigation included.
Follow-up assessment including clinical examination and lab investigation.
• Haemogram with IPF was done at first visit, 2nd IPF was done in patients whose platelet count remains below 50,000 and /or does not increase by more than 20,000/cc mm from baseline.
• If platelet <50,000/cc mm Haemogram was done on daily basis in IPD patients till platelet increase to >50,000/cc mm and if platelet >50,000/cc mm haemogram was done on alternate day till platelet count> 1 lakhcc mm. For OPD patients irrespective of platelet count, haemogram was done on alternate day basis.
• Normal Reference range of IPF was considered from 0.2 to 6.6 %, which was the reference range of Pathology laboratory of DeenanathMangeshkar Hospital.
• Bleeding manifestation assessed in all patients as per Buchanan bleeding scores.31
| | | | Results and Observations | The present prospective observational study was conducted from July 2018 to April 2020. A total number of 105 patients of dengue fever, who presented in Deenanath Mangeshkar Hospital and met the inclusion criteria, were enrolled in the study after obtaining informed consent.
Out of 105 patients, 51 were male and 54 female. Male median age was 9 years, female 7 years.
Out of 105 patients, 86 got admitted on fay 2 of fever, 13 on day 3 and 6 on day 4 of fever. Most dengue fever patients (82% of the sample) were admitted on Day 2.
Figure 1. Column Chart Showing Serology of Patient Admitted.
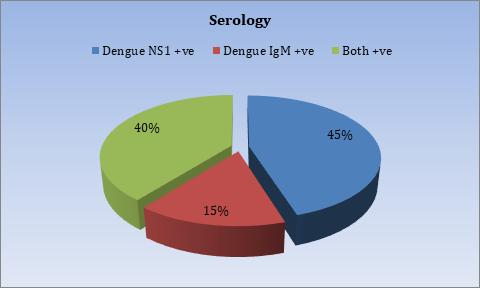
All 105 patients have NS1 antigen. 48 patients were NS1 antigen positive, 16 were IgM positive, and 41 were both. We did not find IgG-only positive instances.
Analysis of baseline IPF with respect to various parameters have been conducted in two groups of patients,
Group I - <30000 /cc mm platelet count
Group II - platelet count >30000/cc mm
In group I (platelet count <30000 /cc mm), 16 patients (94%) had bleeding manifestation, while in group II (platelet count >30000), only 9 patients (10%) had bleeding symptom.
Table 1. Correlation of baseline IPF with Platelet nadir in group I.
| BASELINE IPF |
PLT Nadir (Range) & Median (/cc mm) |
Time to Reach Nadir, (Range) & Median (days) |
| Normal |
(9000 -26000), 23000 |
(1-4), 1 |
| High |
(5000-30000), 22000 |
(1- 3), 1 |
| P value |
0.38 |
0.98 |
*.Normal IPF (0.2 to 6.6 %) high IPF (above 6.6%) platelet count in /cc mm
Remarks: In our study, IPF was associated with platelet nadir in group I for Normal IPF (9000-26000, Median 23000) and High IPF (5000-30000, Median 22000). Mean difference was not statistically significant (p >0.05). The link between baseline IPF and time to platelet nadir for normal and high IPF was not statistically significant (p >0.05).
Table 2. Correlation of baseline IPF with Platelet recovery in Group I.
| Baseline IPF |
Time to Reach Plt >1 Lakh (Range) & Median (days) |
Time to increase PLT >20,000 (Range) & Median (days) |
| Normal |
(3 - >5) >5 |
(1- >5) 2.5 |
| High |
(4 ->5) >5 |
(1- >5) 4 |
| P value |
0.4 |
0.6 |
Remarks: Our study found an association between IPF and time to reach platelet > 1lakh /cc mm in group I for Normal IPF Range 3-5, Median 5, and High IPF Range 4-5, Median 5.Mean difference was not statistically significant (p >0.05).IPF is associated with time to increase platelets by >20000 /cc mm from baseline in group I for Normal IPF Range 1-5, Median 2.5, and High IPF Range 1-5, Median 4. Mean difference was not statistically significant (P >0.05). Baseline IPF and platelet nadir, time to nadir were uncorrelated.
Table 3. Correlation of baseline IPF with Platelet nadir in group II.
| Baseline IPF |
Plat nadir (Range) & median (/cc mm) |
Time to Reach Nadir, (Range)& Median (days) |
| Normal |
(10000-107000) 77000 |
(1-5) 1 |
| High |
(15000- 82000) 71000 |
(1-3) 1 |
| P value |
0.62 |
0.86 |
*. Normal IPF (0.2 to 6.6 %) high IPF (above 6.6%) platelet count in /cc mm
Remarks: In our study correlation between IPF to platelet nadir it was found that for Normal IPF Range 10000-107000, Median 77000, whereas, High IPF Range 15000-82000, Median 71000. The mean difference was found statistically not significant as p value>0.05. Similarly, association between IPF and time to reach nadir for both normal and high IPF but for this also no statistically difference was observed as p value noted is >0.05.
Table 4. Correlation of baseline IPF with Platelet recovery in group II.
| Baseline IPF % |
Time to Reach Plt> 1 Lakh (Range)& Median (days) |
Time to Increase PLT>20,000 (Range)& Median (days) |
| Normal |
(1 - >5) 2 |
(1 - >5) 2 |
| High |
(2 ->5) 4.5 |
(1 ->5) 2 |
| P value |
0.08 |
0.15 |
Remarks: The above table shows that correlation between IPF to time to reach platelet > 1lakh it was found that for Normal IPF Range was 1-5, Median 2, whereas High IPF Range was2-5, Median 4.5. The mean difference was not found statistically significant as P value >0.05. Also, correlation between IPF to time to increase platelet > 20000 it was found that for Normal IPF Range was 1-5, Median 2 , whereas for High IPF Range was 1-5, Median 2 . The mean difference was not found statistically significant as P value >0.05.
Table 5. Distribution of Bleeding Manifestation Score wise (Buchanan bleeding scores).31
| Manifestation Score |
No. of Patients |
Percentage |
| 0 |
80 |
76.19 |
| 1 |
13 |
12.38 |
| 2 |
9 |
8.57 |
| 3 |
3 |
2.85 |
| 4 |
0 |
0 |
| 5 |
0 |
0 |
Remarks: 80 (76.19%) patients had bleeding score 0, 13 (12.38%) patients had score 1, 9(8.57%) patients had score 2 and remaining 3patients (2.85%) had score 3. Incidence of bleeding manifestations was observed in 25 (24%) out of 105 patients. Female patients having menstrual bleeding were not considered having bleeding manifestations. Patient with scores of 4 or 5 received platelet transfusion so ultimately excluded from our study.
Table 6. Correlation Between baseline IPF and number of patients having bleeding ingroup I.
| Baseline IPF |
Total no. of patients |
No. of patients having bleeding |
| Normal |
11 |
10 (90%) |
| High |
7 |
6 (85%) |
Table 7. Correlation Between baseline IPF and number of patients having bleeding in group II.
| Baseline IPF |
Total no. of patients |
No. of patients having bleeding |
| Normal |
84 |
8(9.5%) |
| High |
3 |
1(9%) |
Remarks: Tables 10 and 11 demonstrate that 16 of 19 patients in group I and 9 of 87 in group II had bleeding, regardless of IPF. Blood loss was more prevalent in patients with platelet counts <30,000/cc mm, regardless of IPF level. So, platelet count correlates more with bleeding than IPF.
Table 8. Change in IPF from baseline.
| Change in IPF |
No. of Patients |
Percentage |
| Decrease |
8 |
32% |
| Increase |
5 |
20% |
| Static |
6 |
24% |
# Increase/decrease was defined as an increase or decrease in IPF by more than 10% (CV of IPF)
| | | | Discussion | Dengue fever is an increasing health issue in tropical India. The world has 50-100 million dengue cases, including over 500,000 dengue haemorrhagic fever and dengue shock syndrome (DHF/DSS) cases.22 Many needless platelet transfusions expose patients to transfusion-related side effects. Many studies have found novel markers to predict platelet recovery.
This study examined whether platelet indices like IPF can predict dengue fever patients' thrombocytopenia severity and transfusion needs. In this 1.5-year prospective observational study at Deenanath Mangeshkar Hospital, 105 dengue fever patients under 18 were admitted.
Our study aimed to determine if baseline IPF predicts platelet nadir. We compared baseline IPF in two groups (<30000/cc mm and >30000/cc mm PLT counts) to eliminate the impact of lower baseline platelet counts on future nadir. Both groups (<30000/cc mm and >30000/cc mm PLT counts) showed no change in platelet nadir, regardless of IPF value. We found a correlation between baseline IPF and platelet recovery to >1 lakh or >20,000/cc mm or greater in two groups (<30000/cc mm and >30000/cc mm PLT counts) with normal and high IPF values. No meaningful difference was seen. No statistically significant difference was found between baseline IPF values and bleeding manifestations in patients with normal and high IPF values.
IPF has been used to predict platelet recovery in ITP, post-chemotherapy, and bone marrow transplant patients. However, few research have examined IPF and platelet recovery in dengue patients.
In dengue patients, Dadu et al. examined IPF and platelet recovery. Platelet counts were serially monitored until recovery and IPF values matched. IPF reference range was 0.7-4.3%.IPF that increased or decreased by more than 10% (CV of IPF) was considered rising/falling. IPF peak values, increasing trend, decreasing trend, and 10% crossing were associated. After peak IPF, 84.3% of patients recovered within 24 h and the rest within 24-48 h. Dengue patients' IPF rises even as platelets diminish. This is because peripheral damage lowers platelet count, stimulates the marrow to create more platelets, and increases IPF. After the IPF started climbing, 93.75% of patients recovered within 24-48 hours. After IPF peaks, platelets rise and IPF falls. If the patient is assessed at this point, when the initial value was the high, the second day's result will be lower. This drop in IPF predicts a platelet count rise.
1. Primary objective in our study was to assess relationship whether platelet nadir can be predicted by baseline IPF
Our study compared baseline IPF values (normal or high) to platelet nadir and time to achieve nadir in two groups (<30000 and >30000 platelet counts). Both groups (<30000 and >30000 platelet counts) showed no meaningful difference. IPF normal or high did not significantly affect platelet nadir in either group. We discovered no difference in platelet nadir time between normal and high IPF patients .Thus, our study did not identify platelet nadir or time to attain it with baseline IPF.
2. Second Primary objectives was to assess whether baseline IPF can subsequently predict bleeding manifestation in next few days
No association was seen between baseline IPF and bleeding in our study. We found that patients in group I (platelet count <30000/cc mm) had a higher bleeding rate than those in group II (platelet count >30000/cc mm), regardless of IPF levels. Our investigation found IPF unhelpful for bleeding prediction. IPF is not a good indicator/we cannot effectively compare because we had few patients with high baseline IPF values. We know of no research that correlated baseline IPF with bleeding.
The bleeding symptoms were more linked with low platelet counts than IPF values. Thus, patients with low platelet counts and high IPF should not be deemed bleeding-protective or at lesser risk, as in other conditions.
McDonnell et al. studied thrombocytopenia in various disorders (97 with ITP, 11 with BMF, 126 with malignancy, and 38 with other causes). This study found no significant difference in bleeding score with increased IPF.30
3. Correlation of baseline IPF with platelet recovery
No significant association was discovered between IPF and platelet recovery in our investigation. Dadu et al. showed a substantial association between IPF and platelet recovery. Renuka and Swasthik24 reported a strong connection between IPF values at admission and 24-48 hours of baseline in 105 confirmed dengue patients with platelet counts less than 1 lakh. 81.7 percent had high IPF (>4.3%) while the rest had low. High IPF group had considerably greater platelet count at 24–48 hours than normal IPF group.
In children post-chemotherapy, Larke et al. found that IPF increased before 24-48 hrs of platelet recovery. Platelet recovery took 2-3 days in dengue patients, according to Dadu et al. Another study by Po-tseng-Lee found that dengue fever patients' median platelet recovery time was 4 days.26
IPF in patients with increased platelet counts may not predict platelet recovery.25 We have fewer individuals in the lowest platelet risk category, therefore we cannot comment on the clinical implications of measuring IPF as a predictor of platelet recovery. We also learnt that baseline IPF values may not correspond and require serial monitoring. Platelet recovery time depends on presentation day and baseline platelet level. Platelet recovery can take over 5 days even with a high IPF.Baseline IPF from our study does not predict platelet recovery time.
4. Range of IPF values
Multiple factors can induce thrombocytopenia, from decreased platelet formation to increased destruction. IPF range reflects platelet synthesis separation in normal/elevated IPF patients. Elevated IPF implies normal platelet synthesis but likely peripheral platelet degradation, while normal IPF indicates reduced marrow production and enhanced platelet destruction.
Our investigation found 0.2-6.6% typical IPF. We found 95 patients with normal IPF and 10 with high IPF (above 6.6) at baseline. Only 19 patients repeated IPF, and 32% demonstrated a drop in IPF from baseline, 20% rose, and 24% remained unchanged from 48 to 72 hours.
In a study of 104 dengue fever patients, Renuka et al. defined normal IPF as <4.3 and high IPF as >4.3. At admission, the mean IPF value was 7.84±4.65%. 81% of patients had high IPF upon admission, whereas others had normal IPF. Two groups had very different platelet count increases. A high IPF value at admission was associated with a considerably larger platelet count rise at 24 to 48 hours than normal IPF.
In another study by Ahmad et al., 84% of 106 dengue fever patients had IPF >8% (high IPF) and 15% had normal IPF at baseline. Similar to Dadu et al.28, IPF was positively linked with platelet counts on days 2 and 3. Binvestigations used different IPF ranges and cutoffs. Both studies did not categorise patients by baseline platelet count, and the lowest platelet count group was unclear.
| | | | Conclusion | IPF is an economical and helpful criterion for thrombocytopenia diagnosis due to its repeatability and speed. IPF predicts platelet recovery.
In dengue patients with high Immature Platelet Fraction (IPF), platelet counts improve within 24–48 hours.
We found that IPF did not predict platelet nadir, time to nadir, or bleeding symptoms in the next five days.
Our study found that baseline platelet count predicted bleeding, whereas IPF did not.
Our study did not effectively represent the most vulnerable bleeding population due to a small number of individuals with lower platelet counts. Therefore, we could not anticipate IPF correlation for that population.
We cannot conclude from this study that baseline IPF can predict platelet recovery or bleeding. Other factors were likely involved.
Limitations
A larger multicentric study would be preferable than this urban single-center study. Dengue fever studies should include more patients and signs.
Recommendations
Larger population studies with longer follow-ups are needed to anticipate IPF's link with platelet recovery and bleeding.
Patients with lower baseline platelet counts have a higher risk of bleeding, hence serial monitoring of immature platelet fraction is indicated. IPF is an early sign of platelet recovery and can assist avoid prophylactic platelet transfusion.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Rajapakse S, Rodrigo C, Rajapakse A. Treatment of dengue fever. Infect Drug Resist. 2012;5:103-12. [CrossRef] [PubMed] [PMC free article]
- Briggs C, Kunka S, Hart D, Oguni S, Machin S. Assessment of animmature platelet fraction (IPF) in peripheral thrombocytopenia. British Journal of Haematology. 2004;126(1):93-99. [CrossRef] [PubMed]
- Dadu T, Sehgal K, Joshi M, Khodaiji S. Evaluation of the immature platelet fraction as an indicator of platelet recovery indengue patients. International Journal of Laboratory Hematology.2013;36(5):499-504. [CrossRef] [PubMed]
- Gubler DJ. Dengue, Urbanization and Globalization: The Unholy Trinity of the 21(st) Century. Trop Med Health. 2011 Dec;39(4 Suppl):3-11. [CrossRef] [PubMed] [PMC free article]
- Warkentien T. Dengue Fever: Historical Perspective and the Global Response. Journal of Infectious Diseases and Epidemiology.2016;2(2). [CrossRef]
- Murray NE, Quam MB, Wilder-Smith A. Epidemiology of dengue: past, present and future prospects. Clin Epidemiol. 2013;5:299-309. [CrossRef] [PubMed] [PMC free article]
- Gupta N, Shrivastava S, Jain A, Chaturvedi U. Dengue In India.Indian Journal of Medical Research. 2012;136(3):373-390.
- Martina BE, Koraka P, Osterhaus AD. Dengue virus pathogenesis: an integrated view. Clin Microbiol Rev. 2009 Oct;22(4):564-81. [CrossRef] [PubMed] [PMC free article]
- Srichaikul T. Disseminated intravascular coagulation in dengue haemorrhagic fever. Southeast Asian J Trop Med Public Health. 1987 Sep;18(3):303-11.
- Halstead S. Observations related to pathogenesis of dengue hemorrhagic fever. IV. Relation of disease severity to antibody response and virus recovered. Yale Journal of Biology and Medicine. 1970;42(5):311-328.
- Guzman M. Epidemiologic Studies on Dengue in Santiago de Cuba, 1997. American Journal of Epidemiology. 2000;152(9):793-799. [CrossRef] [PubMed]
- Takubo T. Reticulated platelet and its clinical significance. Rinshobyori. The Japanese journal of clinical pathology. 2002Aug;50(8):761-7.
- Thanachartwet V, Wattanathum A, Sahassananda D, Wacharasint P, Chamnanchanunt S, Khine Kyaw E, et al. Dynamic Measurement of Hemodynamic Parameters and Cardiac Preload in Adults with Dengue: A Prospective Observational Study. PLoS ONE. 2016;11(5):e0156135. [CrossRef] [PubMed] [PMC free article]
- Gubler DJ. Dengue and dengue hemorrhagic fever. Clin MicrobiolRev. 1998;11(3):480-496. [CrossRef] [PubMed] [PMC free article]
- Pons I, Monteagudo M, Lucchetti G, Muñoz L, Perea G, Colomina I, Guiu J, Obiols J. Correlation between immature platelet fraction and reticulated platelets. Usefulness in the etiology diagnosis of thrombocytopenia. European journal of haematology. 2010 Aug;85(2):158-63. [CrossRef] [PubMed]
- Takubo T. [Reticulated platelet and its clinical significance]. RinshoByori. 2002 Aug;50(8):761-7.
- Monteagudo M, Amengual MJ, Munoz L, Soler JA, RoigI,Tolosa C. Reticulated platelets as a screening test to identify thrombocytopenia aetiology. QJM: An International Journal of Medicine. 2008 Apr 8;101(7):549-55. [CrossRef] [PubMed]
- Sehgal KK, Tina D, Choksey U, Dalal RJ, Shanaz KJ. Reference range evaluation of complete blood count parameters with emphasis on newer research parameters on the complete blood count analyzer Sysmex XE-2100. Indian Journal of Pathology and Microbiology.2013 Apr 1;56(2):120. [CrossRef] [PubMed]
- Schoorl M, Schoorl M, Oomes J, van Pelt J. New fluorescent method (PLT-F) on Sysmex XN2000 hematologyanalyzer achieved higher accuracy in low platelet counting. American journal of clinical pathology. 2013 Oct 1;140(4):495-9. [CrossRef] [PubMed]
- Meintker L, Haimerl M, Ringwald J, Krause SW. Measurement of immature platelets with Abbott CD-Sapphire and Sysmex XE-5000 in haematology and oncology patients. Clinical chemistry and laboratory medicine. 2013 Nov 1;51(11):2125-31. [CrossRef] [PubMed]
- Dusse LM, Freitas LG. Clinical applicability of reticulated platelets. ClinicaChimica Acta. 2015 Jan 15;439:143-7. [CrossRef] [PubMed]
- Simmons CP, Farrar JJ, Chau NV, Wills B. Current concepts dengue. The New England Journal of Medicine. 2014;366:15. [CrossRef] [PubMed]
- Suharti C, Gorp E, Setiati TE, Dolmans W, Djokomoeljanto RJ, Hack CE, Cate HT, van der Meer JW. The role of cytokines in activation of coagulation and fibrinolysis in dengue shock syndrome. ThrombHaemost. 2002;87:42-6. [CrossRef]
- G. RB, Upadhya SP. Immature platelet fraction (IPF) as an indicator of platelet recovery in dengue fever. Int Jour of Biomed Res. 2019; 10(11):e5305.
- Have LW, Hasle H, Vestergaard EM, Kjaersgaard M. Absolute immature platelet count may predict imminent platelet recovery in thrombocytopenic children following chemotherapy. Pediatr Blood Cancer. 2013 Jul;60(7):1198-203. [CrossRef] [PubMed]
- Lee PT, Liu PY. TCTAP A-123 platelet activity recovery time is 48 hours slower than the platelet count recovery in hemorrhagic dengue fever subjects. Journal of the American College of Cardiology. 2016 Apr 26;67(16 Supplement):S56-7. [CrossRef]
- Jeon K, Kim M, Lee J, Lee JS, Kim HS, Kang HJ, et al. Immature platelet fraction: A useful marker for identifying the cause of thrombocytopenia and predicting platelet recovery. Medicine (Baltimore). 2020 Feb;99(7):e19096. [CrossRef] [PubMed] [PMC free article]
- Wayez A, Zafar L, Aijaz M, Afroz N. Study of platelet indices in dengue fever with thrombocytopenia and correlation of immature platelet fraction (IPF) with platelet recovery. Arch Hematol Case Rep Rev. 2020;5(1):001-5. [CrossRef]
- Bride KL, Lim D, Paessler M, Lambert MP. Can immature platelet fraction (IPF) be used to assess bleeding risk in pediatric immune thrombocytopenia (ITP) and to differentiate itp from bone marrow failure/aplastic anemia? A retrospective analysis. Blood. 2015;126:3474. [CrossRef]
- McDonnell A, Bride KL, Lim D, Paessler M, Witmer CM, Lambert MP. Utility of the immature platelet fraction in pediatric immune thrombocytopenia: Differentiating from bone marrow failure and predicting bleeding risk. Pediatric blood & cancer. 2018 Feb;65(2):e26812. [CrossRef] [PubMed]
- Buchanan GR, Adix L. Grading of hemorrhage in children with idiopathic thrombocytopenic purpura. J Pediatr. 2002 Nov;141(5):683-8. doi: 10.1067/mpd.2002.128547. PMID: 12410198. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2026.52
|
| Cite this article as: | | Pitkar S, Mahajan K, Kanvinde S, Kumar T. A Prospective Observational Study to Determine The Role of the immature platelet fraction in predicting severity of thrombocytopenia and occurrence of bleeding manifestation in patients of dengue. Pediatr Oncall J. 2025 Aug 05. doi: 10.7199/ped.oncall.2026.52 |
|