Shinas K Nellicka, Vivin Abraham.
Department of Pediatrics, Medical Trust Hospital, Kochi 682016, India.
ADDRESS FOR CORRESPONDENCE
Shinas K Nellicka, Senior Resident, Medical Trust Hospital, Kochi 682016, India.
Email: shinas_156@hotmail.com | | Abstract | | Arteriopathies are the leading cause of stroke which causes lifelong morbidity in children. Stroke associated with hypertension should lead to a suspicion of fibromuscular dysplasia. A 2 years 8 month old boy presented with left hemiparesis with left sided lower motor neuron facial palsy and accelerated hypertension. On MR angiography, there was non-visualization of right internal carotid artery (ICA). CT renal aortography showed string of beads sign. He was diagnosed with fibromuscular dysplasia. He was started on anti-hypertensives along with physiotherapy. | | | | Keywords | | arteriopathy, hypertension, hemiplegia | | | | Introduction | | Stroke causes lifelong neurological morbidity in children. Arteriopathies are the leading cause of stroke but mechanisms are poorly understood.1,2 The result is that treatment and prevention strategies are limited with poor outcome in most survivors.3 Fibromuscular dysplasias are a group of idiopathic, non-inflammatory arteriopathies with distinct pathological and angiographic findings.4 The most commonly described form of fibromuscular dysplasia is medial subtype, typically affecting young adult females with renal and cerebral vessel involvement, distinct ‘string of beads’ appearance on angiography, refractory hypertension and stroke.5 Here we present a 2 years 8 month old male presenting with all the above classical features associated with fibromuscular dysplasia. | | | | Case Report | A 2 years 8 month old male presented with sudden onset weakness of left side involving lower limb more than the upper limb along with left lower motor neuron (LMN) facial palsy. He was treated with oral steroids at local hospital. He had a similar episode at 9 months of age and was on oral anticonvulsants since then. There was no residual deficit after the first episode and child was walking normally. There were no similar complaints in the family. On admission, he was afebrile, conscious and alert with a pulse rate 116 beats/ min and blood pressure of 230/140 mm of Hg in right upper limb in supine position. All peripheral pulses were well felt. Neurological examination showed left sided LMN facial palsy with left hemiparesis. Deep tendon reflexes were exaggerated and plantars were extensor bilaterally. On investigation, hemogram, coagulation parameters, lipid profile, electrolytes, ESR, CRP, ANA, Anti ds-DNA, serum C3, C4 and urine vanillylmandelic acid (VMA) levels were normal. MRI brain showed hypointensity along the right middle cerebral artery territory and left occipital lobe and diffusion restriction along the right MCA territory and left occipital lobe (Figure 1,2). MR angiography showed marked luminal narrowing at the right common carotid artery bifurcation and along the entire length of external carotid artery and internal carotid artery (Figure 3). CT aortography showed bilateral renal artery stenosis with characteristic string of beads appearance (Figure 4). Echocardiography showed severe concentric left ventricular hypertrophy with left ventricular outflow tract turbulence with a gradient 35 mm of Hg. He was treated with multiple anti-hypertensives including intravenous labetalol, nitroglycerine and oral nifedipine. Blood pressure was gradually controlled over 72 hours and physical rehabilitation was initiated. Left sided hemiparesis gradually improved and blood pressure was well controlled on oral anti-hypertensives. He was discharged and advised bilateral renal artery stenting.
Figure 1: MRI brain showing hypointensity along the right middle cerebral artery territory and left occipital lobe.
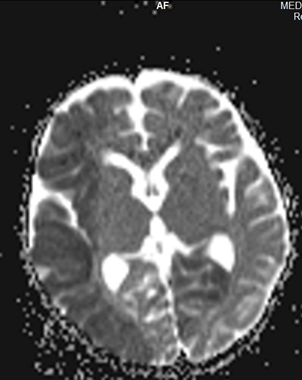 | Figure 2: Diffusion- weighted MRI shows diffusion restriction along the right MCA territory and left occipital lobe.
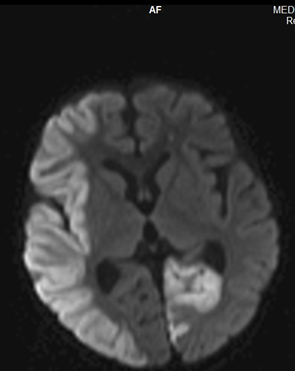 | Figure 3: CT angiography shows string of beads appearance with marked narrowing of mid segment of bilateral renal arteries.
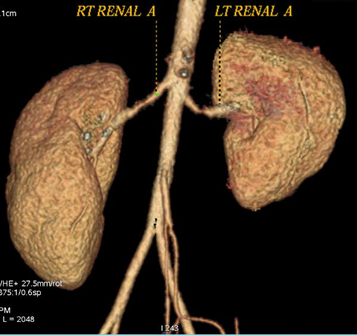 | Figure 4: Carotid angiography shows marked luminal narrowing at the right common carotid artery bifurcation and along the entire length on external carotid artery and internal carotid artery.
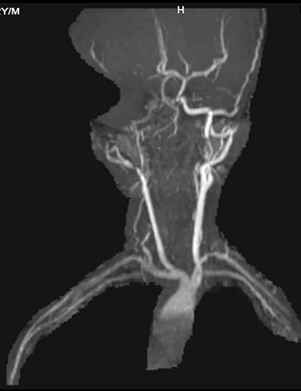 |
| | | | Discussion | Fibromuscular dysplasia (FMD) a systemic arteriopathy that has a predilection for renal arteries followed by cervicocranial vessels. The etiology of the disease is still unknown. Three main types of FMD have been identified as intimal, medial and perimedial6 and these types have also been described in extrarenal arteries.7 Medial dysplasia is the most common histologic type. It is reported in association with connective tissue disorders like Ehler-Danlos syndrome and alpha-1 antitrypsin deficiency.8,9 Familial cases have also been reported leading to a suspicion of a genetic disorder. In our patient, there was no family history of FMD and no other findings suggestive of connective tissue disorder. Although we did not measure the activity of alpha-1 antitrypsin, the patient showed no signs of cirrhosis or emphysema that are typically associated with this condition. Atherosclerosis as a cause of stroke in children is rare as compared to adults. In children, lipoprotein abnormality may lead to occlusive cerebrovascular atherosclerosis leading to ischaemic stroke. Lipid profile done in our patient was normal.
Among the brain vessels, the most commonly involved vessels are extracranial carotid arteries followed by vertebro-basilar and intracranial carotid arteries. The involvement is often bilateral.10 Our patient had extensive unilateral involvement of intracranial carotid artery, MCA and a portion of posterior cerebral artery. On the other hand, the most common presentation of FMD is renovascular hypertension secondary to renal artery involvement. Hypertension is rarely associated with childhood stroke11 and its presence should prompt consideration of renal arteriopathy and possible fibromuscular dysplasia as seen in our patient. MR angiography is an important diagnostic tool for FMD, but the exact diagnosis is established with conventional angiography. The “string of beads” appearance is characteristic for FMD12 which was seen in our patient.
The treatment options include anti-platelet agents, anti-coagulant agents and surgical treatment. Our case was treated with anti-hypertensives, physiotherapy and is planned for bilateral renal artery stenting.
In conclusion, increasing awareness of stroke in children has improved our knowledge about the etiology, diagnostic methods and treatment options for such cases. FMD as a cause of stroke is rarely encountered in children and this report adds a new childhood case of FMD with extensive unilateral intracranial vessel involvement. FMD should be considered as a differential diagnosis in cases of childhood stroke. | | | | Contributor Statement | | All authors contributed to case management and manuscript | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Fullerton HJ, Wu YW, Sidney S, Johnston SC. Risk of recurrent childhood arterial ischaemic stroke in population-based cohort: the importance of cerebrovascular imaging. Pediatrics 2007;119:495-501. [CrossRef] [PubMed]
- Amelie-Lefond C, Bernard TJ, Sebire G, Friedman NR, Heyer GL, Lerner NB, et al. Predictors of cerebral arteriopathy in children with arterial ischaemic stroke: results of International pediatric stroke study. Circulation. 2009;119: 1417-23. [CrossRef] [PubMed] [PMC free article]
- deVeber GA, MacGregor D, Curtis R, Mayank S. neurologic outcome in survivors of childhood arterial ischaemic stroke and sinovenous thrombosis. J Child Neurol. 2000;15: 316-24. [CrossRef] [PubMed]
- Slovut DP, Olin JW. Fibromuscular dysplasia. N Engl J Med. 2004;350:1862-71. [CrossRef] [PubMed]
- Touze E, Oppenheim C, Trystram D, Nokam G, Pasquini M, Alamowitch S, et al. Fibromuscular dysplasia of cervical and intracranial arteries. Int J Stroke. 2010;5:296–305. [CrossRef] [PubMed]
- Stanley JC. Renal artery fibrodysplasia. In: Novick AC, Scable J, Hamilton G (eds). Renal Vascular Disease. WB Saunders. London. 1996:21-23. [PubMed]
- Luscher TF, Lie JT, Stanson AW, Houser OW, Hollier LH, Sheps SG. Arterial fibromuscular dysplasia. Mayo Clin Proc. 1987;62: 931-952. [CrossRef]
- Schievink WI, Meyer FB, Parisi JE, Wijdicks EF. Fibromuscular dysplasia of the internal carotid artery associated with alpha-1 antitrypsin deficiency. Neurosurg. 1998;43:229-33. [CrossRef]
- Niccolaides P, Appleton R. Stroke in children. Dev Med Child Neurol. 1996; 38: 172-80. [CrossRef]
- Healton BH, Mohr JP. Fibromuscular dysplasia. In: Barnett HJ, Stein BM, Mohr JP, Yatsu FM (eds). Stroke: Pathophysiology, Diagnosis and Management (3rd ed). New York. Churchill Livingstone. 1998: 833–44.
- Kirkham FJ, Prengler M, Hewes DK, Ganesan V. Risk factors for arterial ischemic stroke in children. J Child Neurol. 2000;15:299-307. [CrossRef] [PubMed]
- Lassiter F D. The string-of-beads sign. Radiology.1998;206:437–438. [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2019.43
|
| Cite this article as: | | Nellicka S K, Abraham V. Fibromuscular Dysplasia in a child with Hypertension and Stroke. Pediatr Oncall J. 2019;16: 88-90. doi: 10.7199/ped.oncall.2019.43 |
|