Jisha Mathew, Kishore Kumar R.
Department of Paediatrics and Neonatology, Cloudnine Hospital, Jayanagar, Bangalore, Karnataka, India.
ADDRESS FOR CORRESPONDENCE
Dr. Kishore Kumar R, Cloudnine Hospital, #1533, 9th Main, 3rd block, Jayanagar, Bangalore, 560011, India.
Email: drkishore@cloudninecare.com | | Abstract | Introduction: Apnoea of prematurity (AOP) is one of the most common causes of apnoea in preterm babies with lower gestational ages. There are many studied interventions to treat the same, namely, use of CPAP, Methylxanthine compounds, Tactile and Olfactory stimulation. We report an unconventional way to treat apnoea of prematurity.
Methods: We used a novel method of Glove ventilation to provide tactile stimulation to babies. The end delivery limb of the ventilator tubing was connected to a sterile glove and the ventilator was started with physiological settings. This glove was then kept in close contact with the baby’s chest to provide intermittent stimulation.
Conclusion: Glove ventilation could be used as an unconventional way to mechanically stimulate preterm babies with AOP. The added advantage of glove ventilation is that it could be used easily at peripheral centres without the need for expensive equipments and many babies could be extubated successfully.
| | | | Keywords | Respiratory, Mechanical stimulation, Critical newborn care.
Abbreviations:
AOP - Apnoea of prematurity, CPAP - Continuous Positive Airway Pressure, NIPPV- Non-invasive positive pressure ventilation, PIP - Peak inspiratory pressure, BPD - Bronchopulmonary dysplasia.
| | | | Introduction | Apnoea of prematurity (AOP) is defined as a pause of breathing for more than 15–20 s, or accompanied by oxygen desaturation (SpO2 ≤ 80% for ≥4 s) and bradycardia (heart rate < 2/3 of baseline for ≥4 s), in infants born less than 37 weeks of gestation.1
The pathogenesis of AOP is poorly understood. Immature pulmonary reflexes, immature respiratory center and breathing responses to hypoxia and hypercapnia due to prematurity may likely contribute to the occurrence or severity of AOP.2,3 Many other triggering factors have been associated with apnoea namely, Intraventricular hemorrhage, Anemia, Hemodynamically significant PDA, certain medications (like Opiates and sedatives), glucose and electrolyte imbalances.
AOP in itself may not be a major threat to infant’s health if addressed early, but frequent and recurrent episodes of severe apnoea, may lead to disturbances of cerebral hemodynamics. The short term consequences, could be cerebral hypoperfusion and hypoxic ischemic injury4 and long term could be poor neurodevelopmental outcomes.5
| | | | Methodology | The end delivery limb of the ventilator tubing was connected to a sterile glove as in Figure 1 and the ventilator (Drager, Babylog 8000 Plus) was started with physiological settings (Figure 2). The frequency of stimulation was set as the respiratory rate of ventilator. The impact was set by adjusting the Peak Inspiratory Pressure (PIP). This air-filled glove was kept under the baby’s nest, positioned below the chest and abdomen as seen in Figure 3 and it provided gentle vibratory tactile stimulation at frequent intervals.
Figure 1. The end delivery limb of the ventilator tubing.
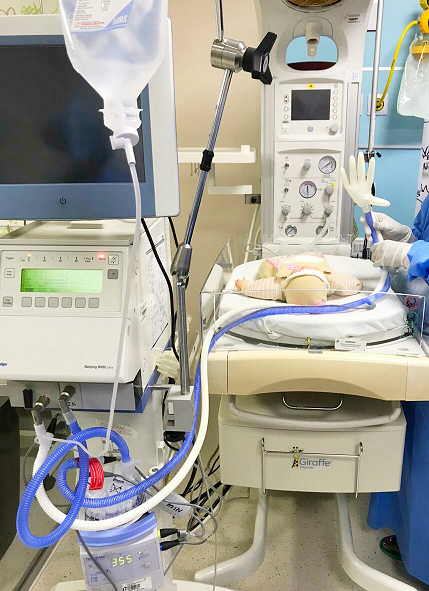
Figure 2. Ventilator (Drager, Babylog 8000 Plus).
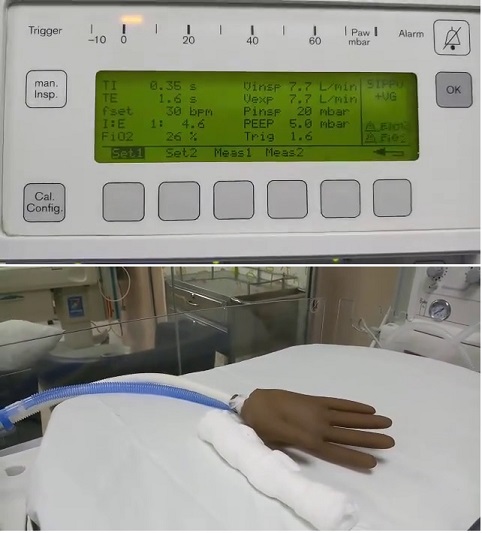
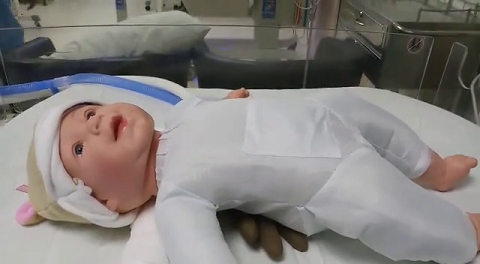
Figure 3. The air-filled glove was kept under the baby’s nest.
| | | | Case Report | We have managed a few cases of recurrent apnea in preterm infants by using this novel approach.
Case 1
A 25/40 week baby with birth weight of 770 gms, required to be ventilated for 7 days since birth. A trial of extubation was given on Day 7 of life, but he developed recurrent apnoea after a few hours, which improved briefly with tactile stimulation. He was also on medical management for a hemodynamically significant PDA at this point. We then put the baby on Glove ventilation as described above, along with IV caffeine and CPAP which the baby was already on, post extubation. The baby tolerated extubation and we continued glove ventilation for five days. This helped reduce the frequency of apneic episodes from 3-4 times an hour to 1-2 times for 24 hrs, self aborting and it soon subsided completely. All blood cultures were sterile till discharge.
Case 2
A 26/40 weeks baby with a birth weight of 690 gms, was ventilated for 5 days since birth and then extubated to CPAP. She required re-intubation for repeated apnoeas and suspected sepsis and was extubated again on day 16. Chest X Ray (CXR) showed good lung expansion and had early changes of BPD by now. On day 17 baby had recurrent apnoeas requiring tactile stimulation. Hence, instead of repeatedly stimulating the baby manually, she was put on glove ventilation which itself acted like stimulation and she improved and was weaned off glove ventilation by Day 21 of life.
Case 3
A 29/40 weeks baby born with a birth weight of 920 gms, had severe RDS requiring 2 doses of surfactant and ventilation for 5 days, following which the baby was on CPAP for 2 days and then on room air. Within 24 hours of baby being taken off CPAP, baby had recurrent apnoea requiring stimulation. Apnoea seemed to settle on CPAP. Though the baby had good lung expansion on CXR and didn’t require oxygen on CPAP, the baby continued to be dependent on CPAP for a few weeks. Hence the baby was taken off CPAP and a trial of glove ventilation was given and the baby seemed to cope very well. Baby remained on glove ventilation for 7 days after which it was discontinued.
| | | | Discussion | There are varied interventions for the treatment of AOP. Interventions for AOP include measures taken to reduce work of breathing and/or increase respiratory drive namely Prone positioning6, Continuous Positive Airway Pressure (CPAP) at 4-6 cmH2O7,8 and Methylxanthine compounds such as caffeine, theophylline and aminophylline which are powerful central nervous system stimulants.9 Kangaroo Mother Care, Sensory stimulation, namely tactile and olfactory stimulation, are all been studied too.
Tactile stimulation is a commonly used, simple intervention which likely works by generating excitatory, nonspecific neuronal activity in the brainstem centre which stimulates respiratory activity and causes arousal. It is shown to decrease the frequency of apnoea.10,11,12,13 However, it has the increased risk of cross-contamination and infections. It can cause sleep disturbances in baby which can be disadvantageous for the growth and development of the infant.12This intervention could also increase the workload of the nurses. Mechanical stimulation could reduce the risk of cross-contamination and enable a direct response, but data is scarce.14
This novel method of glove ventilation works by the principle of providing mechanical tactile stimulation. Our hypothesis is that, the intervention of using glove ventilation for preemies with recurrent apnoea, may reduce the frequency of apnoeic episodes and also the number of times the baby is handled for stimulation and in turn alleviating the burden on the nurse practitioner. We have used this method in 10-15 preterm babies (<30 weeks gestation), 3 of whom have been described above, immediately post extubation till about 48-120 hrs. We mostly used this method in preemies requiring prolonged ventilation, heading towards ventilator associated pneumonia/BPD. In these circumstances, where prematurity and its associated factors, more than atelectasis is the problem, extubating to CPAP and trying simultaneous glove ventilation instead of repeated tactile stimulation could be beneficial. Hence, the selection of babies is crucial for its success. Babies with good lung expansion, whose apnoea is not related to collapse of alveoli or central hypoventilation but require repeated stimulation to keep the desaturations to minimal, are the ones who do well on glove ventilation. | | | | Conclusion | | Glove ventilation could be used as an unconventional way to mechanically stimulate preterm babies with AOP. The added advantage of glove ventilation is that it could be used easily at peripheral centres without the need for expensive equipments and many babies could be extubated successfully. | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Moriette G, Lescure S, El Ayoubi M et al. Apnea of prematurity: what's new? Arch Pediatr. 2010;17(2):186-190 [CrossRef] [PubMed]
- Abu Shaweesh JM, Martin RJ. Neonatal apnea: what's new? Pediatr Pulmonol. 2008;43:937-44 [CrossRef] [PubMed]
- Darnall RA. The role of CO2 and central chemoreception in the control of breathing in the fetus and the neonate. Respir Physiol Neurobiol. 2010;173(3):201-212 [CrossRef] [PubMed] [PMC free article]
- Pilcher G, Urlesberger B, Muller W. Impact of bradycardia on cerebral oxygenation and cerebral blood volume during apnoea in preterm infants. Physiol Meas. 2003;24(3):671-680 [CrossRef] [PubMed]
- Janvier A, Khairy M, Kokkotis A, et al. Apnea is associated with neurodevelopmental impairment in very low birth weight infants. J Perinatol. 2004;24(12):763-768. [CrossRef] [PubMed]
- Bhat RY, Hannam S, Pressler R, et al. Effect of prone and supine position on sleep, apneas, and arousal in preterm infants. Pediatrics. 2006;118(1):101-107. [CrossRef] [PubMed]
- Paoli AG, Davis PG, Faber B, et al. Devices and pressure sources for administration of nasal continuous positive airway pressure (NCPAP) in preterm neonates. Cochrane Database Syst Rev. 2008;23(1).
- Pantalitschka T, Sievers J, Urschitz MS, et al. Randomized crossover trial of four nasal respiratory support systems on apnoea of prematurity in very low birth weight infants. Arch Dis Child Fetal Neonatal Ed. 2009;94(4):245-248. [CrossRef] [PubMed]
- Henderson-Smart DJ, Steer PA. Caffeine versus theophylline for apnea in preterm infants. Cochrane Database Syst Rev. 2010;20(1):CD000273. [CrossRef] [PubMed]
- Kattwinkel J, Nearman HS, Fanaroff AA, et al. Apnea of prematurity. Comparative therapeutic effects of cutaneous stimulation and nasal continuous positive airway pressure. J Pediatr. 1975;86(4):588-592. [CrossRef]
- Bloch-Salisbury E, Indic P, Bednarek F, et al. Stabilizing immature breathing patterns of preterm infants using stochastic mechanosensory stimulation. J Appl Physiol. 2009;107(4):1017-1027. [CrossRef] [PubMed] [PMC free article]
- Camargo VC, Honorato da Silva S, Freitas de Amorim M, Nohama P. Instrumentation for the detection and interruption of apnea episodes for premature newborn. Conference of the IEEE Engineering in Medicine and Biology Society Chicago, IL: IEEE (2014). p. 2127-30.10.1109/EMBC.2014.6944037. [CrossRef] [PubMed]
- Pichardo R, Adam JS, Rosow E, et al. Vibrotactile stimulation system to treat apnea of prematurity. Biomed Instrum Technol (2003) 37(1):34-40. [CrossRef]
- S J E Cramer, J Dekker, J Dankelman et al. Effect of Tactile Stimulation on Termination and Prevention of Apnea of Prematurity: A Systematic Review. Front Pediatr. 2018 Mar 2;6:45. [CrossRef] [PubMed] [PMC free article]
DOI: https://doi.org/10.7199/ped.oncall.2023.8
|
| Cite this article as: | | Mathew J, R K K. A novel treatment for Apnoea of Prematurity. Pediatr Oncall J. 2023;20: 14-16. doi: 10.7199/ped.oncall.2023.8 |
|