Carolina Freitas Fernandes1, Carolina Gouveia1, Pedro Gouveia2, Bernardo Camacho1, Maria João Borges1.
1Pediatrics, Hospital Central do Funchal, Funchal, Portugal,
2Endocrinology, Hospital Central do Funchal, Funchal, Portugal.
ADDRESS FOR CORRESPONDENCE
Carolina Freitas Fernandes, Avenida Luís de Camões, nº 57 – 9004-514 Funchal, Madeira, Portugal.
Email: acff@campus.ul.pt | | Abstract | Polydipsia is characterized by the voluntary and excessive intake of liquids. Primary polydipsia usually occurs in adolescents or adults with a psychiatric disorder. Other pathologies, such as diabetes mellitus and diabetes insipid, also manifest with these symptoms.
We present a case of a 15-month-old male infant who suddenly started with polyuria and polydipsia. Ingestion of about 3 L/day of water and urinary output of 12.9 ml/Kg/h. Analytically, hyponatremia, low plasma and urinary osmolarity. A fluid restriction test was performed, that resulted in an increased urinary concentration. The diagnosis of primary polydipsia was assumed. A progressive reduction in daily water intake was carried out, with good response.
Primary polydipsia is a differential diagnosis of polyuria and polydipsia, but infrequent in younger children. The authors intend to emphasize the need for a high index of suspicion and the challenge of etiological investigation because of the atypical age for the occurrence of this diagnosis. | | | | Keywords | | Potomania, Polydipsia, Polyuria. | | | | Introduction | Polydipsia is characterized by the voluntary and excessive intake of water or other liquids. Primary polydipsia usually occurs in adolescents or adults with a psychiatric disorder (potomania) Despite of being generally associated with an increased intake of beer, potomania is characterised by excessive drinking of liquids, such as water (polydipsia) or alcoholic beverages (dipsomania).1 Despite being a well-known entity in adulthood, this situation is uncommon in younger children and there are few cases described in the literature.
Polyuria is accompanied by hypo-osmolarity of the urine, but a concentrated urine may be formed when avoiding the ingestion of water. Polydipsia precedes polyuria and it’s the cause of it in this scenario.2
The worst complication of this pathology is water intoxication. Excessive oral fluid intake over a short period of time can lead to clinically significant hyponatremia. Water intoxication syndrome is characterized by lethargy, confusion and coma.3
Other pathologies, such as diabetes mellitus and diabetes insipidus, also manifest with polydipsia and polyuria.
We report a case of a 15-month-old male who developed a sudden onset of polyuria and polydipsia. | | | | Case Report | A previously healthy 15-month-old male infant was referred to Pediatric Department because of sudden onset of polyuria and polydipsia within 2 weeks. He presented hand-foot-and-mouth disease, about 2 weeks before the current clinical condition.
His father has renal agenesis and chronic kidney disease of unknown etiology, diagnosed 3 years before.
In the clinical examination no remarkable data was found, normal psychomotor, height and weight development.
He had an ingestion of about 6L/m2/day of water, with reference to nighttime awakenings for drinking water and high urinary output.
The child was admitted and to confirm polydipsia and polyuria, fluid intake and diuresis were measured in 24 hours, obtaining intake values of 4950 ml (9.8 L/m2) and diuresis of 3785 ml equivalent to 13.7 ml/Kg/hour (7.6 L/m2)
Analytically, he had hyponatremia (130mmol/L) and low plasma osmolarity (267.6 mosm/Kg). The urinalysis showed a low density of 1003 and a low osmolarity (183 mosm/Kg). The hemogram and the general biochemistry, including blood glucose, urea and creatinine, were normal. No evidence of glycosuria.
Given the rarity of primary polydipsia in children, secondary causes were excluded.
A water deprivation test was performed. Before starting the test, patient was weighed, catheterize, serum osmolarity and serum sodium was measured as well as urinary volume and urine osmolarity. During the test patient was submitted to dry diet. Vital signs, weight and urinary osmolarity were monitored every hour. Serum osmolarity and serum sodium were measured every 2 hours.
Before beginning the trial, patient weight was 11.495 Kg, after 2 hours of test weight was 11.385 Kg. Plasma osmolarity was 275 mosm/Kg and urinary osmolarity 212 mosm/Kg, after 1 hour of the trial child presents urinary osmolarity of 603 mosm/Kg. Two hours after the beginning of the test plasma osmolarity was 281 mosm/Kg and urinary osmolarity was 725 mosm/Kg.
Water deprivation test showed, already in the second hour after fluid restriction, that the patient perfectly concentrates the urine (urinary osmolarity >500 mosm/Kg), while remaining well hydrated throughout the test. With these results the diagnosis of diabetes insipidus was excluded and primary polydipsia was assumed. As a treatment, a progressive reduction of water intake was established, with good response.
The child had no more episodes and remains stable under follow-up at the Pediatrics consultation.
| | | | Discussion | Primary polydipsia is a differential diagnosis of polyuria and polydipsia, but infrequent in young children. Etiology is not yet well known, however it can be associated with disorders of the hypothalamus and hippocampus and can originate the water intoxication syndrome.2
With this case report, the authors intend to emphasize the need for a high index of suspicion and the challenge of etiological investigation because of the atypical age for the occurrence of this diagnosis.
A careful stepwise approach in polyuria–polydipsia syndrome is recommended. The assessment of the medical history should include timing and onset of symptoms, their severity and possible triggering factors. In addition, a history of head trauma, headaches, vision disturbances and signs for anterior pituitary dysfunction should be enquired. The medical history should include questions about psychiatric disorders and a thorough drug history. Family history is important for possible hereditary causes.4
In our patient there was no relevant personal or family history, except the father with a single kidney and chronic kidney disease.
Diabetes insipidus is a rare disease that can manifest at any age and the prevalence is similar amongst males and females. Diabetes insipidus is a form of polyuria–polydipsia syndrome and is characterized by excessive hypotonic polyuria (>50 mL/Kg/day) and polydipsia (>2 L/m2/day), observed in our patient.5
After exclusion of disorders of osmotic diuresis, such as uncontrolled diabetes mellitus (in our patient blood glucose was normal and there was no evidence of glycosuria), the differential diagnosis of diabetes insipidus involves distinguishing between primary forms (central or renal) and secondary forms (resulting from primary polydipsia) – Chart 1. The presence of hyponatremia (plasma sodium <135 mmol/L) or low plasma osmolarity (<280 mosm/Kg) is highly suspicious for primary polydipsia, both reported in our clinical case.6
Central diabetes insipidus is a rare disease in children, where the most important etiologies include intracranial tumours or malformations of the central nervous system. In this pathology the secretion of adh is diminished. In part, the action of adh depends on the functional integrity of renal V2 receptors and adequate tonicity of the renal medullary interstitial tissue and various nephropathies and drugs can interfere with the ability of urinary concentration.7,8
Chart 1. Differential diagnosis of polyuria–polydipsia syndrome.
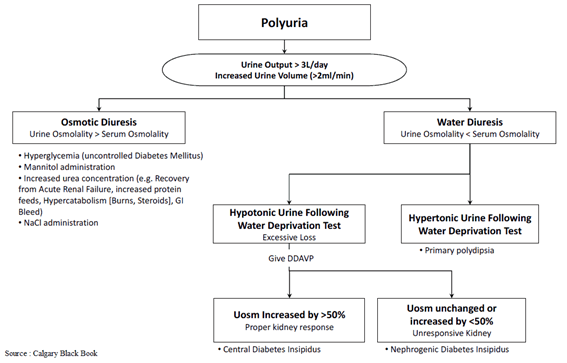
It’s necessary to make a differential diagnosis between primary polydipsia, central diabetes insipidus and nephrogenic diabetes insipidus. Therefore, a water deprivation test was performed in our patient, in which a clear increase in the osmolarity of urine in the second hour of the test, reaching normal values, allow us to rule out the diagnosis of diabetes insipidus, both central and nephrogenic. Consequently, the authors decided not to submit the child to an MRI to rule out central pathology. If a central pathology were present, the water deprivation test would show failure to maximally concentrate urine.
In our patient, the fluid restriction test was planned to have the duration of 6 hours or finish in the presence of one of the following situations listed in Table 1.
Table 1. Criteria to end the water deprivation test.
| Water deprivation test finishes after 6 hours or in the presence of one of the following situations: |
| 1. Urinary density=1020 |
| 2. Urinary osmolarity=500 mosm/kg |
| 3. Urinary density/urinary osmolarity reaches plateau in 2-3 consecutive samples (density variations <1, or urinary osmolarity vary less than 30 mosm/kg). |
| 4. Plasma osmolarity >305 mosm/kg |
| 5. Serum sodium=145 mmol/L |
| 6. Weight loss >5% or signs of volume depletion or intolerable thirst |
If the trial ends up by non-laboratory criteria, serum osmolarity, urinary osmolarity and serum sodium should be measured at that point. If fluid restriction test was positive, a desmopressin test should be performed to exclude secondary polydipsia - Table 2. To exclude central diabetes insipidus a central nervous system imaging study should be feasible. In the present case, we did not consider it necessary, as explained above.
When symptoms and laboratory tests are mild, the only treatment for psychogenic polydipsia is water restriction, in moderate cases treatment may include intravenous saline administration in addition to water restriction,and in severe cases, the provision of a hypertonic saline solution, diuretics and anticonvulsants.2
Table 2. Desmopressin test.
| Desmopressin Test: |
| 1. Start after completion of the water deprivation test (if positive) |
| 2. Administer 1 mcg of DDAVP IV over 20 minutes |
| 3. Urinary osmolarity collection at 30, 60 and 120 minutes |
| 4. During 10-12 hours after administration of desmopressin, the liquids administered should not exceed diuresis to avoid water intoxication, and the child can eat. Allow the child to drink up to 1.5 to 2 times the volume of urine passed during the restriction phase if thirst is intolerable |
In primary polydipsia, a chronic intake of excess fluids associated with psychogenic polydipsia can suppress the axis hypothalamic-pituitary and consequently produce an unregulated release of adh. This entity it’s described in the literature at such early ages, as in the case we present, but in a very limited way.9
In our patient the treatment with a progressive reduction of water intake was established, with good response. A closer watch should be maintained, undergoing frequent serum electrolyte checks. We recommend observing their behaviour because the possible correlation between psychogenic and hyperactive disorders in children.2 | | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Domínguez R.O, Laguarde N, Pinkala E, et al. Potomania and osmotic imbalance: Permanent cortical visual impairment due to extrapontine myelinolysis. Neurología 2013; Vol. 28. Issue 7: 449-450 [CrossRef]
- Méndez Pérez P, Núñez Estévez M.b, Arias Castro S, et al. Polidipsia Primaria en el Niño: Caso Clínico. Vox Paediatrica 2010; 17(2): 59-62
- Hiramatsu R, Takeshita A, Taguchi M, et al. Symptomatic Hyponatremia after Voluntary Excessive Water Ingestion in a Patient without Psychiatric Problems. Endocrine Journal. 2007; 54: 643-45 [CrossRef] [PubMed]
- Christ-Crain M, Winzeler B, Refardt J, et al. Diagnosis and management of diabetes insipidus for the internist: an update (Review). J Intern Med 2021; 290: 73-87 [CrossRef] [PubMed]
- Fenske W, Allolio B. Clinical review: current state and future perspectives in the diagnosis of diabetes insipidus: a clinical review. J Clin Endocrinol Metab. 2012; 97: 3426-37 [CrossRef] [PubMed]
- Verbalis JG, Goldsmith SR, Greenberg A, et al. Hyponatremia treatment guidelines 2007: expert panel recommendations. Am J Med. 2007; 120: S1-21. [CrossRef] [PubMed]
- Christ-Crain M, Bichet DG, Fenske WK, et al. Diabetes insipidus. Nat Rev Dis Primers. 2019; 5: 54 [CrossRef] [PubMed]
- Bichet DG. Genetics in endocrinology pathophysiology, diagnosis and treatment of familial nephrogenic diabetes insipidus. Eur J Endocrinol. 2020; 183: R29-R40. [CrossRef] [PubMed]
- Sailer CO, Winzeler B, Nigro N, et al. Characteristics and outcomes of patients with profound hyponatraemia due to primary polydipsia. Clin Endocrinol (Oxf). 2017; 87: 492 [CrossRef] [PubMed]
DOI: https://doi.org/10.7199/ped.oncall.2024.30
|
| Cite this article as: | | Fernandes C F, Gouveia C, Gouveia P, Camacho B, Borges M J. Potomania in pediatric age? The diagnostic challenge. Pediatr Oncall J. 2024;21: 118-120. doi: 10.7199/ped.oncall.2024.30 |
|