Shyam Sundar Meena1, Deepika Meena2.
1Department of Pediatrics, Kalawati Saran Childrens Hospital, Lady Harding Medical College, New Delhi, India,
2Department of Obstetrics and Gynecology, Maulana Azad Medical College, New Delhi, India.
ADDRESS FOR CORRESPONDENCE
Dr. Shyam Sundar Meena, Consultant Paediatrician, Room no-118, Department of Pediatric Medicine, Kalawati Saran Children Hospital, Lady Hardinge Medical College, New Delhi 110001, India.
Email: dr.shyamsnmc2000@gmail.com | | Keywords | | Cutaneous myiasis, Vulvar myiasis, Poor hygiene | | | We present 2 children with myiasis including one scalp myiasis in a 6 year old male street child and other one with vulvar myiasis in an 18 year old unmarried girl suffering from of insulin- dependent diabetes mellitus and psychiatric illness.
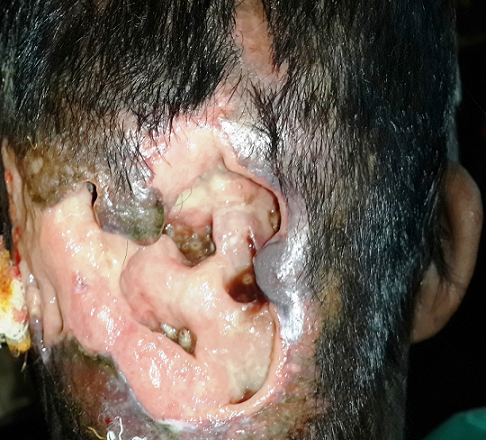
A 6 year old male child living on the streets presented with the social worker in pediatric emergency department with blood stained pus discharge from a scalp wound for 4 weeks. On examination, there were numerous live, larval forms in scalp wound (Figure 1). Initially about 10 maggots were removed using the non-toothed forceps, and the wound was cleaned with betadine. He was then treated with chloroform and turpentine oil in the ratio 1:4 which was followed by manual removal of the maggots (n=20) and wound was maggot free in 2–3 days. He was put on cefuroxime empirically from the 1st day. He was also given tetanus toxoid on admission.
Second child was an 18-years old unmarried girl who presented with vaginal discharge and vulval irritation for 2 week. She had also noted some worms at vulva. Her hygiene was poor and she was wearing dirty clothes. She was suffering from insulin- dependent diabetes mellitus (IDDM) and was poorly compliant to her medications. She was also on antidepressant drugs. She was living with her relatives because her mother had died. She had regular menstrual cycle prior to the onset of this genital discharge. She did not use sanitary napkins during the menstrual periods; instead, she used dirty ragged clothes during menstrual cycles. On examination, there was edema and inflammation of the labia minora. Few maggots were found on the perineum. Examination under local anesthesia revealed an ulcer on the inner surface of the left labium minus involving the hymen ring as well. The ulcer was infested by a large number of maggots. No maggots were found in the vagina or rectum. Initially about 31 maggots were removed with help of non-toothed forceps and the wound was cleaned with betadine. She was treated with ceftriaxone, metronidazole and doxycycline and also received tetanus toxoid on admission. From 2nd day onwards, turpentine oil was applied on the ulcer. By the 4th day, the maggots had completely disappeared and the ulcer was healing. Patient was followed up for 4 weeks and was found to be completely cured. She was given advice on personal hygiene to avoid re-infestation.
In both cases, larvae were preserved in a laboratory for development of adult fly which was confirmed to be house fly.
Figure 1: Scalp wound showing maggots
Myiasis is defined as a disease caused by the infiltration of body tissues by larvae of several fly species of veterinary and medical interest. Risk factors for human myiasis is poor hygiene, low education level and immunocompromised state. (1) Human myiasis can be classified as cutaneous myiasis, ocular myiasis, urogenital myiasis and intestinal myiasis based on clinical presentation. (2) It occurs predominantly in rural areas and is common in children. (1,3) Maggots can enter through intact skin or through a wound. Vulvar myiasis constitutes only 0.7% of human infestation. (4) The most common species that infest wounds in USA is found to be Phaenicia sericata. (4) The fly species that infest healthy tissue are called Biontophages and responsible for the cutaneous forms of this condition (furunculoid myiasis). (1) Complications include secondary infections and tetanus. Treatment is removal of larvae and thorough cleaning of the affected area. Applying turpentine oil makes the respiration impossible for the larvae and is one modality of treatment. (1) A small surgical procedure may be required to remove larvae and after removal the area should be cleaned and covered with an antibiotic ointment. (4) Treatment of secondary infection and administering tetanus toxoid is mandatory. As poor hygiene is known to be associated with vulvar myiasis (5), washing and keeping the genital area clean may prevent to a great extent the occurrence of this condition. It is important to exclude sexually transmitted diseases as a high proportion of cases had sexually transmitted diseases including HIV. (1,2) Sherman et al recommend maggots to be submitted for species identification. (4) Species identification is important for determining pathogenesis, its potential invasiveness, in determining the exact timing and circumstances of infestation.
We re-emphasize that pediatricians should be aware of myiasis causing larvae and take microbiologists advice in laboratory identification and initiate appropriate supportive treatment wherever necessary to minimize the morbidity.
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Passos MRL, Varella RQ, Tavares RR, Barreto NA, Santos CCC, Pinheiro VMS, et al. Vulvar myiasis during pregnancy. Infect Dis Obstetr Gynecol. 2002; 10(3): 153-8. [CrossRef] [PMC free article]
- Zumpt F. Myiasis in man and animals in the Old World. Butterworths, London, United Kingdom. 1965. [PubMed]
- Predy G, Angus M, Honish L, Burnett CE, Stagg A. Myiasis in an urban setting: A case report. Canadian J Infect Dis. 2004; 15(1): 51-2. [CrossRef]
- Sherman RA. Wound myiasis in urban and suburban United States. Arch Int Med 2000; 60: 2004-14. [CrossRef]
- Nunzi E, Rongioletti F, Rebora A. Removal of Dermatobia hominis larvae. Arch Dermatol 1986; 122(2): 140. [CrossRef]
DOI: https://doi.org/10.7199/ped.oncall.2015.64
|
| Cite this article as: | | Meena S S, Meena D. Myiasis in Children: Fly Larval Infestation. Pediatr Oncall J. 2015;12: 114-115. doi: 10.7199/ped.oncall.2015.64 |
|