When an arthritis persists for more than six weeks, especially in the absence of trauma or sepsis, juvenile idiopathic arthritis (JIA) should be considered.
1,2 In this clinical case, the disease started around 6 years of age. However, it was not possible to determine exactly the number of joints affected in the first six months, thus it was not able to differentiate between oligoarticular and polyarticular arthritis. The patient also had an inconsistent history of fever, markedly increased acute phase reactants and no autoantibodies, but no other characteristics of systemic-onset JIA. However, it is not possible to guarantee that it is not a systemic arthritis with a later evolution to polyarticular. The patient also did not have characteristics of psoriatic or enthesitis-related arthritis.
3 The hypothesis of being an infectious arthritis was also considered unlikely, due to the time of the disease's evolution and negative viral serologies and TB IGRA test. Thus, diagnostic hypothesis of polyarticular JIA (polyJIA) RF(-) ANA(-) with the following scores: JADAS 37, articular JADI 26 and extra articular JADI 2 was considered in our patient.
The therapy of polyJIA should be based on an early diagnosis and allocation to specialists in pediatrics rheumatology and a rapid and effective anti-inflammatory treatment with appropriate pain and disease control.
4 None of these principles were possible to apply in our patient. Recent therapy algorithms support the initial treatment of patients with high risk polyJIA with methotrexate, non-steroidal anti-inflammatory drugs, oral prednisolone, intra-articular glucocorticoids and even biological treatment.
4,5 Concerning biologics, there are currently six approved for use in JIA patients with different modes of action: three tumor necrosis factor inhibitors (adalimumab, etanercept and golimumab), one interleukin (IL)-1 inhibitor (canakinumab), one IL-6 inhibitor (tocilizumab) and one T-cell co-stimulation clocker (abatacept).
6 In our patient, the initial therapy was prednisolone (starting 1 mg/kg/day and decreasing until ~0.25 mg/kg/day in ~4 weeks), parenteral methotrexate (starting with ~10 mg/m
2/week and increasing until ~17.5 mg/m
2/week in ~4 weeks) and ibuprofen, with cholecalciferol, calcium and folic acid supplementation. The wrists, elbows, knees and tibiotarsal joints were injected with triamcinolone hexacetonide. During hospitalization, there was a significant improvement in disease control and functional capacity, with less active joints, besides the extensive irreversible structural damages. The patient was then referred to an inpatient urgent rehabilitation program, maintaining the treatment with subcutaneous methotrexate in increasing doses (up to ~20 mg/m
2/week), with a consequent reduction in the prednisolone dose. Despite the improvement in inflammatory analytical parameters (Table 2), she always presented with pain and disturbance of joint functionality. Six months later, therapy with tocilizumab (8 mg/kg/4 weeks) was started. A tocilizumab therapeutic failure was considered after 4 months (Figure 2A) and therapy was replaced by etanercept (0.8 mg/kg/week). There was an improvement in the number of painful and swollen joints (Figure 2B), and it was possible to suspend therapy with prednisolone (after one year). However, she still had increased inflammatory analytical parameters (Table 2). MRI of the knees showed moderate effusion and extensive synovitis on the right side after 4 months of etanercept, so a synovectomy was performed. After 8 months, ultrasounds still presented significant alteration of the wrists and ankles architecture, mild to moderate intra-articular effusion bilaterally in the elbows and tibiotarsic synovitis. Synovectomy was again planned for the knees and elbows. Currently, under etanercept for 10 months (~1 mg/kg/week) and methotrexate (~16 mg/m
2/week), she is able to walk, although limping, and run, despite irreversible joint structural damage.
Table 2. Serial direct and indirect inflammatory parameters.
| Parameter |
Months after hospital discharge without therapy with biologicals |
| 1 |
2.5 |
4 |
| Leukocytes (x10^9/L) |
14500 |
12540 |
16410 |
| Neutrophils (% / x10^9/L) |
11380 |
9960 |
13030 |
| Eosinophils (% / x10^9/L) |
70 |
30 |
50 |
| Basophils (% / x10^9/L) |
10 |
0 |
20 |
| Lymphocytes (% / x10^9/L) |
2640 |
2280 |
2920 |
| Monocytes (% / x10^9/L) |
390 |
280 |
390 |
| Platelets (x10^9/L) |
380000 |
624000 |
567000 |
| C reactive protein (mg/dL) |
|
3.82 |
4.02 |
| Erythrocyte sedimentation rate (mm/hour) |
77 |
77 |
87 |
| Parameter |
Months after hospital discharge, under tocilizumab |
| 6 |
7.5 |
8 |
8.5 |
9 |
| Leukocytes (x10^9/L) |
|
|
|
7860 |
|
| Neutrophils (% / x10^9/L) |
|
|
|
2990 |
|
| Eosinophils (% / x10^9/L) |
|
|
|
540 |
|
| Basophils (% / x10^9/L) |
|
|
|
20 |
|
| Lymphocytes (% / x10^9/L) |
|
|
|
3600 |
|
| Monocytes (% / x10^9/L) |
|
|
|
700 |
|
| Platelets (x10^9/L) |
|
|
|
254000 |
|
| C reactive protein (mg/dL) |
3.4 |
0.1 |
0.1 |
0.03 |
0.1 |
| Erythrocyte sedimentation rate (mm/hour) |
28.7 |
4 |
3 |
2 |
4 |
| Parameter |
Months after hospital discharge, under etanercept |
| 10 |
11 |
12 |
14 |
18 |
20 |
| Leukocytes (x10^9/L) |
|
|
6240 |
|
6130 |
7590 |
| Neutrophils (% / x10^9/L) |
|
|
3730 |
|
3680 |
4010 |
| Eosinophils (% / x10^9/L) |
|
|
170 |
|
200 |
270 |
| Basophils (% / x10^9/L) |
|
|
10 |
|
10 |
20 |
| Lymphocytes (% / x10^9/L) |
|
|
1820 |
|
1820 |
2690 |
| Monocytes (% / x10^9/L) |
|
|
510 |
|
420 |
610 |
| Platelets (x10^9/L) |
|
|
483000 |
|
419000 |
365000 |
| C reactive protein (mg/dL) |
0.1 |
1 |
3.65 |
5.18 |
2.54 |
1.58 |
| Erythrocyte sedimentation rate (mm/hour) |
3 |
13 |
47 |
|
52 |
40 |
Figure 2. Evolution under tocilizumab (A) and under etanercept (B)
A)
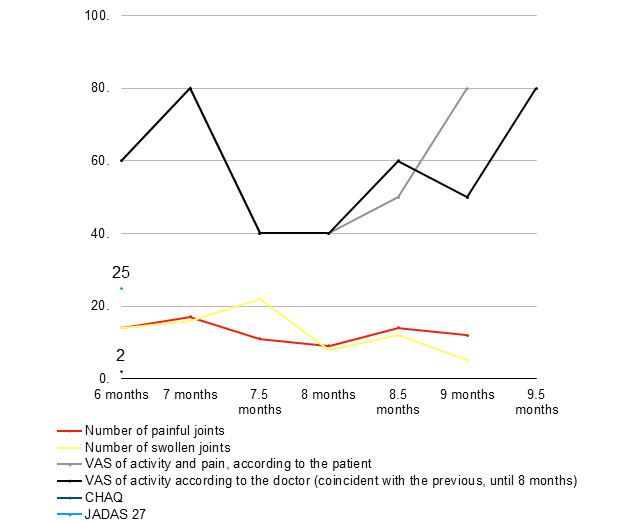 Note: x axis:
Note: x axis: months after hospital discharge
Abbreviations: VAS - visual analogue scale; CHAQ - The Child Health Assessment Questionnaire; JADAS: Juvenile Arthritis Disease Activity Score
B)
 Note:
Note: x axis: months after hospitalar discharge
Abbreviations: VAS - visual analogue scale; JADAS: Juvenile Arthritis Disease Activity Score
What we intend to alert with this case is that JIA is the most frequent cause of inflammatory arthritis in children and an early diagnosis and appropriate therapy are decisive for prognosis.
2,3,8 This clinical case is special not because of the disease itself, but for the fact that it was diagnosed at a very advanced stage, rarely seen nowadays, having exceeded all possible therapeutic windows. We will probably never be able to achieve clinical remission, but the fact that low to moderate disease activity has been achieved is very positive for the patient.
| References : |
- Eisenstein EM, Berkun Y. Diagnosis and classification of juvenile idiopathic arthritis. J Autoimmun. 2014;48-49:31-33.
- Aoust L, Rossi-Semerano L, Koné-Paut I, Dusser P. Time to diagnosis in juvenile idiopathic arthritis: a french perspective. Orphanet J Rare Dis. 2017;12(43). doi: 10.1186/s13023-017-0586-4
- Prakken B, Albani S, Martini A. Juvenile idiopathic arthritis. Lancet [Internet]. 2011;377:2138-2149.
- Horneff G, Klein A, Ganser G, Sailer-Höck M, Günther A, Foeldvari I, et al. Protocols on classification, monitoring and therapy in children's rheumatology (PRO-KIND): results of the working group Polyarticular juvenile idiopathic arthritis. Pediatr Rheumatol. 2017;15(78). doi: 10.1186/s12969-017-0206-9
- Ringold S, Angeleshan ST, Beukelman T, Lovell D, Cuello CA, Becker ML, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Treatment of Juvenile Idiopathic Arthritis: Therapeutic Approaches for Non-Systemic Polyarthritis, Sacroiliitis, and Enthesitis. Am Coll Rheumatol. 2019;71:717-734.
- Santos M, Conde M, Mourão A, Ramos FO, Cabral M, Brito I, et al. 2016 update of the Portuguese recommendations for the use of biological therapies in children and adolescents with Juvenile Idiopathic Arthritis. Acta Reumatol Port. 2016;41:194-212.
- Weiss PF. Polyarticular juvenile idiopathic arthritis: Clinical manifestations, diagnosis, and complications [retrieved October 2019] Available at: https://www.uptodate.com/contents/ polyarticular-juvenile-idiopathic-arthritis-clinical-manifestations-diagnosis-and-complications? search=polyarticularjuvenileidiopathicarthritis& source=search_result&selectedTitle=1~38& usage_type=default&display_rank=1. Accessed on 22nd April 2021
- Marcdante KJ, Kliegman RM. Juvenile Idiopathic Arthritis. In: Marcdante KJ, Kliegman RM. eds. Nelson Essentials of Pediatrics. Elsevier. Philadelphia. 7th ed. 2015:305-308.
|