Patient Education
Insulin
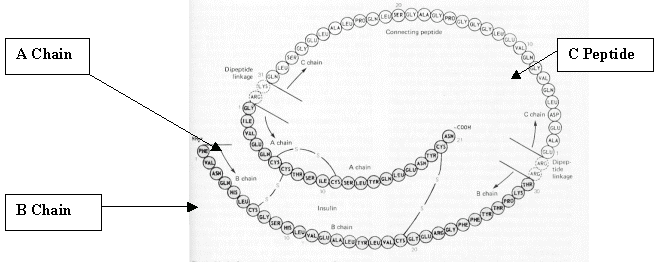
Insulin is a hormone produced by the beta-cells of the pancreas. It is a protein with a molecular weight of approximately 5700 kDa. It is formed from proinsulin after cleavage into insulin and C-peptide (Fig 1). The normal insulin secretion is 0.5-0.7 units/kg per day.Insulin has two chains A and B and during its production. A third chain of peptides called C Peptide links these. C peptide is removed before Insulin is secreted into the blood.
Physiological Functions of Insulin
- Stimulates entry of glucose into cells for utilization as energy source.
- Stimulates entry of amino acids into cells, enhancing protein synthesis
- Enhances fat storage and prevents mobilization of fat for energy (lipolysis)
- Promotes storage of glucose as glycogen in muscle and liver cells (glycogenesis)
- Inhibits formation of glucose from non carbohydrates (gluconeogenesis)
The body's homeostatic system maintains a uniform blood glucose level between meal times and fasting periods. Basal insulin secretion maintains a balance against high blood sugar during the resting state.
Indications For Insulin Therapy
Absolute
- All individuals with Type 1 diabetes
- Type 2 diabetes not adequately controlled by other forms of therapy (drugs, diet and exercise)
- Malnutrition related diabetes mellitus
Intermittent
- Gestational diabetes
- Individuals with Type 2 diabetes during periods of physiological stress (major surgery, infection)
- Diabetic ketoacidosis (DKA)
- Hyperosmolar hyperglycemic nonketotic syndrome (HHNS)
- Diabetics with tuberculosis often do better with insulin.
- Secondary diabetes (pancreatitis, corticosteroids)
Insulin Sources
The insulins available for routine clinical use are derived from three sources beef, pork, and human (recombinant).
Types of Insulin
The insulins available now are the "pure" varieties and contain negligible risks of immunogenicity. These are of four types - beef, porcine, mixed and human insulin
- Beef insulin differs from human insulin in three amino acids, namely A8, A 10, and B 30.
- Porcine insulin differs from human insulin in only one amino acid i.e. B30 position. Thus, porcine insulin is less immunogenic than beef insulin.
- Mixed insulin contains a mixture of bovine and porcine insulin and it is more antigenic than single species
- Human insulin is pure and has the same amino acid structure as that of native insulin. They are made by genetic engineering or by the transformation from porcine insulin by substituting alanine with threonine in the B30 position.
Classification of Insulin
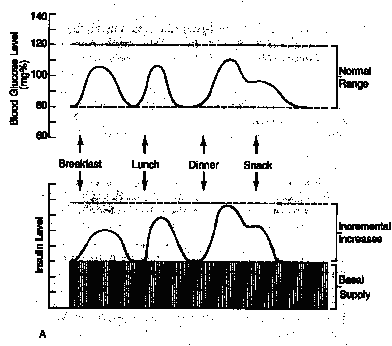
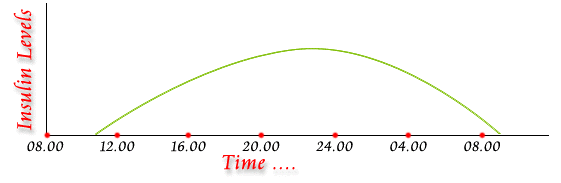
In a normal person without diabetes, insulin is secreted throughout the day and thus there is a basal level and peaks of insulin secretion are seen following meals when the blood glucose rises (Fig 2). Physiological Secretion of Insulin
Insulin Administration and Storage
Insulin vials should be preferably stored at 4-8°C. If possible they should be kept in the refrigerator, but not in the freezer compartment. The insulin vial should be brought down to body temperature by gently rubbing it between the palms before withdrawing the insulin into the syringes.
If refrigeration facilities are unavailable, then the currently used vial can be stored at room temperature away from heat and direct sunlight. If vials have to be stored for longer periods, a simple method is for the unopened vials to be stored in the earthen pots, which contain drinking water and are found in most homes where a refrigerator is not present.
Insulin Initiation
Initiation of Insulin
There are no precise formulae by which the initial dose can be calculated. The usual total dose of insulin is between 0.5 and 1 unit/kg/day although it is usual to start with a starting dose of 0.25 unit/kg/day. The usual regimen is to start with a small dose of intermediate-acting insulin about 8-12 units S.C. before breakfast or with a mixture of short-acting insulin and Intermediate-acting insulin in small doses. When stabilized most patients require about 60% of total insulin in the morning and 40% in the evening. However insulin-dosing regimen is highly individualized and it has to be tailor-made depending upon the patient's age, weight, sugar levels, and presence of any other condition, which may affect the status of blood sugars. Often overweight patients may need more insulin due to insulin resistance.
Most of the short-acting and the intermediate/long-acting insulins available here may be mixed in the same syringe except Lantus. Insulin InitiationInsulins are presently available in strengths of U-40, and U-100. The patient must ensure that the syringes used by him/her are compatible with the strength of insulin used.
The various methods of insulin delivery are by injections, insulin pens, and insulin pumps, and lately by inhalation (EXUBERA). The inhaled insulin is in the last phase of a clinical trial in the USA and is expected to be available in the market by next year.
Insulin Delivery
The various methods of insulin delivery are by injections, insulin pens, and insulin pumps and lately by inhalation (EXUBERA). The inhaled insulin is in the last phase of clinical trial in the USA and is expected to be available in the market by next year.
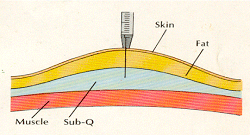
Insulin Delivery Methods Injection: The needle and syringe are the commonest of the four insulin delivery systems. Today's needles are much improved from years ago. They are sharper, finer, and coated with Teflon to make injections much less painful than they used to be. Injections should be given preferably 20-30 minutes before the meal to achieve the proper peak of insulin action corresponding to elevated sugar levels after a meal except for Lantus which can be given just before the meals. The needle is to be inserted in the pinched up skin at a 90o angle so that the injection is in the subcutaneous tissue. It is advisable to use disposable syringes, which are now easily available.
The cost of the syringe is often a limiting factor to the routine use of these syringes. Patients can reuse the same disposable syringe and decrease costs. Insulin syringes may be reused 2-3 times if the needle is not blunt. The same syringe can be used for different sites but it should never be used on different patients.
Insulin pens: An insulin pen is a compact, portable device that serves exactly the same function as a needle and syringe, but is handier and more convenient to use. A wide variety of disposable and reusable insulin pens that come pre-loaded with their insulins are available in the market. One of the great advantages of insulin pens is that they are more suitable for patients who are frequent travelers.

Insulin pump: An insulin pump is a computer-controlled device, which comes in the size and shape of a pager. It painlessly and accurately delivers insulin all day long through a tiny tube inserted just under the skin.
An insulin pump is a best and most intensive way that currently exists to control diabetes. The pump is not entirely pain-free. The location of the infusion set has to be changed after every second or third day to prevent infection at the site.
Insulin Therapy Regimens
To optimize glycemic control, an individual would need to receive small amounts of insulin continuously (basal), with boluses of insulin before meals and snacks. Adjust the dose based on self-monitoring of glucose levels, HbA1C, weight, lifestyle, and other concurrent conditions.
Insulin Therapy for Type 1 diabetes
Successful insulin therapy for type 1 diabetes requires the co-ordination of the following factors:
- Properly titrated insulin dose
- Diet
- Physical activity
- Blood glucose monitoring
- Patient education
- Readily accessible medical support
There are 2 main insulin regimens
- Twice-daily injections of mixed intermediate (cloudy isophane) or long-acting insulin with a short-acting (clear soluble) insulin.
- The basal-bolus regimen: This is particularly suitable for patients with irregular meal times or hectic lifestyles. This consists of intermediate-acting insulin at bedtime (to provide the basal insulin requirement) with short-acting insulin before each meal.
- Multiple Dose Insulin (MDI) regimen: Here a combination of short and long-acting insulin (Mixtard 30:70 0r 50:50) is given prior to breakfast and dinner, while short-acting insulin is given at lunch. This regime can be modified in numerous ways to suit the patient's needs, e.g. long-acting insulin may be added at bedtime.
Nowadays an entirely new dimension has been added with the availability of ultra short-acting Lispro/Aspart insulin and the very long-acting Glargine (Lantus) insulins. Glargine insulin is given at bedtime, with the ultra-short insulins being administered prior to each major meal.
Self-monitoring of blood glucose (SMBG) with or with a glucometer is recommended at least once daily. Testing time should be changed frequently with the majority of the readings being pre-meal or at bedtime.
Insulin therapy for Type 2 diabetes
Insulin therapy for type 2 diabetes can be supplementary or absolute depending upon the indication. Intermediate-acting isophane insulin works well on its own in these patients but a soluble component is often needed to achieve good glycemic control. Soluble insulin can be added if postprandial hyperglycemia 2 hours after a meal is excessive (>180 mg/dl). A few elderly patients can be managed on once-daily Lente insulin. Lente insulin is regular insulin complexed with zinc to form a long-acting suspension and cannot be mixed with soluble insulin.
Mixing of Insulin
When mixing two different types of insulin are required in a single syringe then mutual contamination of the two vials must be avoided. What is equally important is that you must always load the rapid-acting insulin first and then the intermediate or long-acting insulin. If you do the reverse then you are likely to change the time action profile of the short or rapid-acting insulin. Once the injection is prepared inject immediately and definitely not after 5 minutes.
Sites of Insulin Injection
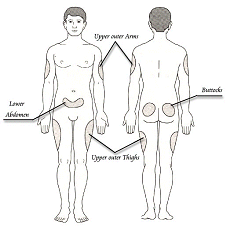
The sites where the injections can be given are shown in Fig 8. These include the abdomen, outer upper arms, the thighs, the buttocks, and hip areas. Do not inject insulin in bony areas or near any of your joints. Efforts must be made to rotate the site of the injection throughout the permissible areas and not inject only into one region. Fig 8: Sites of insulin Injections
Complications of Insulin Therapy
Hypoglycemia (Low blood sugar):
This is a major side effect and the patient should be educated about it before initiation of insulin and he should be taught about the emergency measures to be taken in such a condition.
Resistance:
The impurities present in the older insulins gave rise to antibodies, which interfere with normal insulin action. However, newer insulins are purer and the chances of insulin resistance minimal.
Edema:
Insulin has salt retaining properties and may cause fluid retention in some patients.
Lipodystrophy (Abnormal fat accumulation):
This may present as lipoatrophy (decreased fat) or lipohypertrophy (increased fat). Lipoatrophy was seen with the use of older insulins and it is rare with the newer insulins. Lipohypertrophy can be seen with the use of insulin. The best way to avoid this condition is to frequently change the site of injections.
Local or systemic hypersensitivity reactions
Caution:
- Never be in haste. Always start with a low dose, go slow. There is no rush to achieve adequate control since this may take several weeks. Start with 8-10 units twice daily. Increase by 2-4 units every 2-3 days according to capillary blood glucose values and your physical condition.
- You should always consult your physician about any healthcare questions you may have, especially before trying a new medication, diet, fitness program, or approach to health care issues.
Types Of Insulin
The insulins available for clinical use can be classified according to peak effect and duration of action.
Rapid acting Insulins:
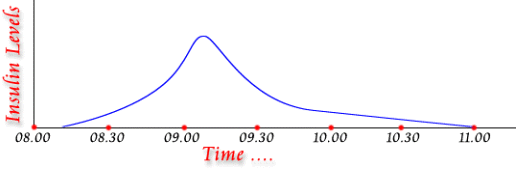
The only insulin analog available in India is the rapid-acting Lispro. It reaches the blood within 15 minutes after injection. It peaks 30 to 90 minutes later and may last as long as 4-5 hours (Fig 3). It is injected just before meals. Fig 3: Peak and Duration of Action of Rapid Acting Insulins
Short acting (Regular):
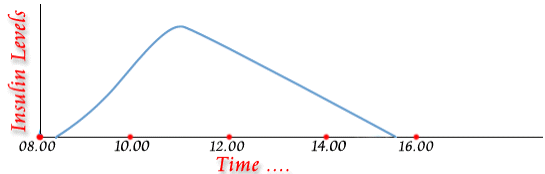
Short-acting (regular) insulin usually reaches the blood within 30 minutes after injection. It peaks 2 to 4 hours later and stays in the blood for about 4 to 8 hours (Fig.4). Fig 4: Peak and Duration of Action of Short Acting Insulins
Intermediate acting:
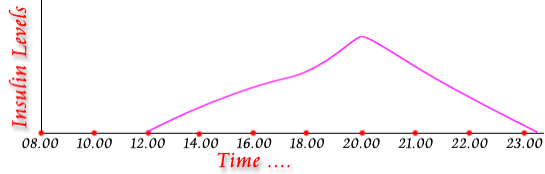
NPH and Lente (Fig.5): Intermediate-acting (NPH and Lente) insulins reach the blood 2 to 6 hours after injection. The peak of 4 to 14 hours later and stay in the blood for about 14 to 20 hours. Intermediate-acting insulins include Lente and NPH. Insulin preparations with a predetermined proportion of NPH mixed with regular, such as 70% NPH to 30% regular, or a 50/50 mix are called intermediate-acting insulin. Fig 5: Peak and Duration of Action of Intermediate Acting Insulins
Long Acting
: Ultralente (Fig.6): Long-acting (ultralente) insulin takes 6 to 14 hours to start working. It has no peak or a very small peak of 10 to 16 hours after injection. It stays in the blood between 20 and 24 hours.Fig 6: Peak and Duration of Action of Long Acting Insulins
Very long acting
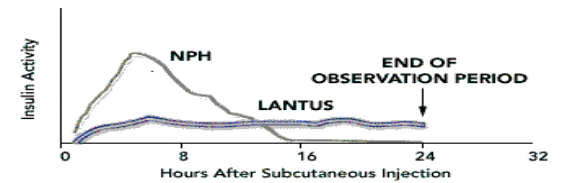
: Lantus (Fig.7): Lantus is newer insulin, which works for 24 hrs. The chemical structure of Lantus makes it to be released steadily and continuously in the body, mimicking almost the basal physiological secretion of Insulin. It is the only long-acting insulin that is clear and cannot be mixed up with any other insulin.
Regular insulin, Lispro, and Aspart are only clear insulins or solution of insulin. Regular insulin modified with the addition of protamine and zinc (NPH) or zinc alone (Lente, Ultralente) to prolong the duration of action of insulin is cloudy white suspensions. Lispro is an insulin analog identical to human insulin except for the reversal of two amino acids, lysine and proline, on the B chain. Fig 7: Peak and Duration of Action of Very Long Acting Insulins
1. Shah SC, Malone JI, Simpson NE. A randomized trial of intensive insulin therapy in newly diagnosed insulin dependent diabetes mellitus. N Eng J Med 1989; 320-4.
2. The Diabetes Control and Complication Trial research group. The effect of intensive treatment of diabetes on the development of progression of long-term complications in insulin dependent diabetes mellitus. N Eng J Med 1993; 329; 977-86.
3. Ohkubo Y, Kishikawa H, Araki E et al. Intensive insulin therapy prevents progression of diabetic microvascular complications in Japanese patients with non-insulin dependent diabetes mellitus: a randomized prospective six year study. Diabetes Res Clin Pract 1995; 28; 103-17.
4. Turner R, Cull C, Holman R. United Kingdom Prospective Diabetes Study 17: A nine year update of a randomized control trial on the effect of improved metabolic control on complication in non insulin dependent diabetes mellitus. Ann Intern Med 1996; 33; 438-43.
5. The DCCT research group. Epidemiology of severe hypoglycemia in the diabetes control and complications trial. Am J Med 1991; 90; 450-9.
6. Amiel SA, Tamborlane WV, Simonson DC et al. Defective glucose counter regulation after strict glycemic control of insulin dependent diabetes mellitus. N Eng J Med 1987; 316; 1376-83.
7. The DCCT research group. Weight gain associated with intensive therapy in diabetes control and complication trial. Diabetes Care 1988; 11; 567-73.
8. Mecklenberg RS. Acute complications associated with the use of insulin infusion pumps. Endocrinologist 1991; 1; 19-24.
9. Chandalia H. B. Insulin therapy in Diabetes Mellitus. Bombay Hosp. Jour. 18 : 39, 1976.
10. Chandalia H. B.: Insulin Delivery Systems In Current concepts in Diabetes Mellitus. Ed : Sainani G. S., Indian College of Physicians, Bombay, 1993, p. 131-142.
11. Gale EAM, Tattersall RV. Unrecognized nocturnal hypoglycemia in insulin treated diabetics. Lancet 1979; 1; 1049-52.
12. Owens DR, Barnett A. Designer insulins: have they revolutionized insulin therapy? In Batterdge JD ed. Diabetes-current perspectives. London; Martin Dunilitz 1999.
13. Heinemann L, Linkeschova R, Rave K et al. Time action profile of the long acting analogue insulin Glargine (HOE 901) in comparison with those of NPH insulin and placebo. Diabetes Care 2000; 23; 644-9.
14. Dashora U, Dashora V. insulin Glargine. Int J Diabetes Developing Countries 2000; 20; 140-4.
15. Herold KC, Polonsky KS, Cohen RM et al. Variable deterioration in cortical function during insulin-induced hypoglycemia. Diabetes 1985; 34; 677-85.
16. Howey DC, Bowsher RR, Brunelle RL et al. [Lys (B28)Pro(B29)] Human insulin. A rapidly absorbed analogue of human insulin. Diabetes 1994; 43; 396-402.
17. Fineberg SE, Fineberg NS, Anderson JH et al. Insulin immune response to LYSPRO human insulin therapy in insulin native type 1 and type 2 patients. Diabetologia 1995; 38(Suppl 1): A78.
18. Uwe B, Ebraham S, Hirschberger S et al. Effect of rapid acting insulin analogue, insulin Aspart on quality of life and treatment satisfaction in type 1 diabetic patients. Diabetes 1999; 48 (Suppl 1); Abs 0481; A112.
19. Weiss SR, Berger S, Cheng S-L et al. Adjunctive therapy with inhaled human insulin in type 2 diabetic patients failing oral agents. A multicentric phase II trial. Diabetes 1999; 48 (Suppl 1) A 12.
20. Mudaliar SR, Strange P. Lindberg FA et al. Insulin Aspart : a fast acting analogue of human insulin. Diabetes Care 1999; 22; 1501-6.